Clinical study of serum EPA/AA ratio combined with sTWEAK in the evaluation of hemorrhagic transformation and prognosis after thrombolysis in patients with acute cerebral infarction with leukoaraiosis
-
摘要: 目的 探究血清二十碳五烯酸(eicosapentaenoic acid,EPA)/花生四烯酸(arachidonic acid,AA)比值联合可溶性肿瘤坏死因子样弱凋亡诱导剂(soluble tumor necrosis factor-like weak apoptosis inducer,sTWEAK)在合并脑白质疏松(leukoaraiosis,LA)的急性脑梗死患者溶栓后出血转化和预后评估中的临床价值。方法 选择2021年2月—2023年2月收治的149例急性脑梗死合并LA患者,均接受静脉溶栓治疗,根据其溶栓后出血转化情况分为非出血转化组与出血转化组,检测并比较两组血清EPA/AA比值、sTWEAK水平。分析血清EPA/AA比值联合sTWEAK预测急性脑梗死合并LA患者溶栓后出血转化的效能。随访3个月,采用改良Rankin量表(mRS)评估急性脑梗死合并LA患者的预后情况,根据预后将其分为预后良好组与预后不良组,比较两组临床资料、实验室指标及血清EPA/AA比值、sTWEAK水平。多因素回归分析急性脑梗死合并LA患者预后不良的影响因素;ROC曲线分析血清EPA/AA比值联合sTWEAK预测患者预后不良的价值。结果 与非出血转化组比较,出血转化组血清EPA、EPA/AA比值显著降低,sTWEAK显著升高,均差异有统计学意义(P<0.05)。当EPA/AA比值<0.37、sTWEAK>279.6 pg/mL时,两者联合预测急性脑梗死合并LA患者溶栓后出血转化的曲线下面积(area under the curve,AUC)、灵敏度、特异度依次为0.861、82.12%、90.14%,显著优于单项指标检测,差异有统计学意义(P<0.05)。多因素分析结果显示,年龄增大、sTWEAK升高、合并高血压、出血转化、溶栓24 h后NIHSS评分升高是急性脑梗死合并LA患者预后不良的危险因素(P<0.05),而EPA、EPA/AA比值升高为其保护因素(P<0.05)。血清EPA/AA比值联合sTWEAK检测预测急性脑梗死合并LA患者预后不良的AUC、灵敏度、特异度依次为0.899、83.32%、98.11%,显著优于单项指标检测,差异有统计学意义(P<0.05)。结论 血清EPA/AA比值下降、sTWEAK水平升高与合并LA的急性脑梗死患者溶栓后出血转化和预后不良的发生有关,二者联合检测对于溶栓后出血转化及预后不良均有较高的预测价值。
-
关键词:
- 二十碳五烯酸/花生四烯酸比值 /
- 可溶性肿瘤坏死因子样弱凋亡诱导剂 /
- 急性脑梗死 /
- 脑白质疏松症 /
- 静脉溶栓 /
- 出血转化 /
- 预后
Abstract: Objective To explore the clinical value of serum eicosapentaenoic acid(EPA)/arachidonic acid(AA) ratio combined with soluble tumor necrosis factor-like weak apoptosis inducer(sTWEAK) in assessing post thrombolytic hemorrhage transformation and prognosis in patients with acute cerebral infarction complicated with cerebral leukoaraiosis (LA).Methods One hundred and forty nine patients with acute cerebral infarction with LA who were admitted from February 2021 to February 2023 were selected, and all patients treated with intravenous thrombolysis, the patients were divided into non-hemorrhagic transformation group and hemorrhagic transformation group according to the hemorrhagic transformation after thrombolysis. Serum EPA/AA ratio and sTWEAK level were detected and compared between the two groups. The efficacy of serum EPA/AA ratio combined with sTWEAK in predicting hemorrhagic transformation after thrombolysis in patients with acute cerebral infarction complicated with LA were analyzed. After 3 months of follow-up, the prognosis of patients with acute cerebral infarction with LA were evaluated by mRS, patients were divided into good prognosis group and poor prognosis group according to the prognosis, the clinical data, laboratory indexes, serum EPA/AA ratio and sTWEAK level were compared between two groups. The influencing factors of poor prognosis in patients with acute cerebral infarction with LA were analyzed by multivariate regression. The value of serum EPA/AA ratio combined with sTWEAK in predicting poor prognosis of patients were analyzed by ROC curve.Results Compared with the non-hemorrhagic transformation group, the hemorrhagic transformation group showed a significant decrease in serum EPA and EPA/AA ratio(P<0.05), and a significant increase in sTWEAK(P<0.05). When the EPA/AA ratio was less than 0.37 and sTWEAK was greater than 279.6 pg/mL, the combined prediction of the area under the curve(AUC), sensitivity, and specificity of thrombolytic transformation in patients with acute cerebral infarction complicated with LA were 0.861, 82.12%, and 90.14%, which were respectively, significantly better than these of single indicator detection(P<0.05). Multivariate analysis showed that, increased age, elevated sTWEAK, hypertension, hemorrhagic transformation and increased NIHSS score after 24 hours of thrombolysis were risk factors for poor prognosis in patients with acute cerebral infarction with LA(P<0.05), while elevated EPA and EPA/AA ratio were protective factors(P<0.05). The AUC, sensitivity and specificity of serum EPA/AA ratio combined with sTWEAK detection in predicting poor prognosis of patients with acute cerebral infarction with LA were 0.899, 83.32% and 98.11% respectively, which were significantly better than those of single index detection(P<0.05).Conclusion The decrease of serum EPA/AA ratio and sTWEAK level are relate to the occurrence of hemorrhagic transformation and poor prognosis after thrombolysis in patients with acute cerebral infarction with LA, the combine detection has a high predictive value for hemorrhagic transformation and poor prognosis after thrombolysis. -

-
表 1 出血转化组和非出血转化组血清EPA/AA比值和sTWEAK水平比较
X±S 组别 EPA/(μg/mL) AA/(μg/mL) EPA/AA比值 sTWEAK/(pg/mL) 非出血转化组(121例) 75.53±13.68 181.30±32.26 0.41±0.09 125.11±19.59 出血转化组(28例) 58.16±10.64 180.87±31.47 0.32±0.06 305.91±24.45 t 6.287 0.064 5.032 -41.915 P <0.001 0.949 <0.001 <0.001 表 2 血清EPA/AA比值联合sTWEAK对溶栓后出血转化的预测价值
指标 灵敏度/% 特异度/% 截断值 AUC 95%CI 约登指数 EPA/AA比值 46.41 88.43 0.38 0.700 0.579~0.821 0.349 sTWEAK 75.00 77.72 213.68 pg/mL 0.789 0.701~0.876 0.527 两项联合 82.12 90.14 - 0.861 0.763~0.960 0.723 表 3 预后良好组与不良组临床资料、实验室指标及血清EPA/AA比值、sTWEAK水平比较
X±S 指标 预后良好组(107例) 预后不良组(42例) t/χ2 P 年龄/岁 65.78±5.69 69.43±6.11 3.450 0.001 溶栓24 h后NIHSS评分/分 9.83±0.54 14.62±2.08 -22.099 <0.001 溶栓时间/h 3.64±0.62 3.80±0.51 1.486 0.139 BMI/(kg/m2) 22.36±2.17 22.20±2.41 0.392 0.695 糖化血红蛋白/% 6.23±1.51 6.12±1.49 0.401 0.689 EPA/(μg/mL) 81.16±14.97 49.62±11.42 12.311 <0.001 AA/(μg/mL) 180.57±29.84 182.88±30.13 -0.424 0.672 EPA/AA比值 0.45±0.10 0.26±0.06 11.513 <0.001 sTWEAK/(pg/mL) 119.99±18.59 258.69±23.47 -37.952 <0.001 性别/例(%) 0.127 0.721 女 39(36.45) 14(33.33) 男 68(63.55) 28(66.67) 高血压/例(%) 6.350 0.012 无 70(65.42) 18(42.86) 有 37(34.58) 24(57.14) 心房颤动/例(%) 0.4711 0.492 无 75(70.09) 27(64.29) 有 32(29.91) 15(35.71) 糖尿病/例(%) 0.800 0.371 无 72(67.29) 25(59.52) 有 35(32.71) 17(40.48) 高血脂/例(%) 0.554 0.457 无 85(79.44) 31(73.81) 有 22(20.56) 11(26.19) 吸烟史/例(%) 0.346 0.556 无 79(73.83) 29(69.05) 有 28(26.17) 13(30.95) 饮酒史/例(%) 0.642 0.423 无 76(71.03) 27(64.29) 有 31(28.97) 15(35.71) 梗死部位/例(%) 0.887 0.829 基底节 45(42.06) 18(42.86) 脑叶 36(33.64) 15(35.71) 脑干 16(14.95) 7(16.67) 丘脑 10(9.35) 2(4.76) 出血转化/例(%) 10.974 0.001 无 94(87.85) 27(64.29) 有 13(12.15) 15(35.71) 表 4 多因素回归分析急性脑梗死合并LA患者预后不良的影响因素
变量 赋值 β SE Wald χ2 P OR 95%CI 高血压 有=1;无=0 0.743 0.209 12.633 <0.001 2.102 1.316~2.986 年龄 原值输入 0.619 0.174 12.599 <0.001 1.857 1.313~2.601 出血转化 有=1;无=0 0.565 0.200 7.964 0.005 1.759 1.208~2.647 溶栓24 h后NIHSS评分 原值输入 0.907 0.200 20.530 <0.001 2.477 1.543~3.382 EPA 原值输入 -0.367 0.056 42.256 <0.001 0.693 0.602~0.751 EPA/AA比值 原值输入 -0.319 0.054 34.264 <0.001 0.727 0.647~0.801 sTWEAK 原值输入 0.663 0.208 10.142 0.001 1.940 1.254~2.835 表 5 血清EPA/AA比值联合sTWEAK对急性脑梗死合并LA患者预后不良的预测价值
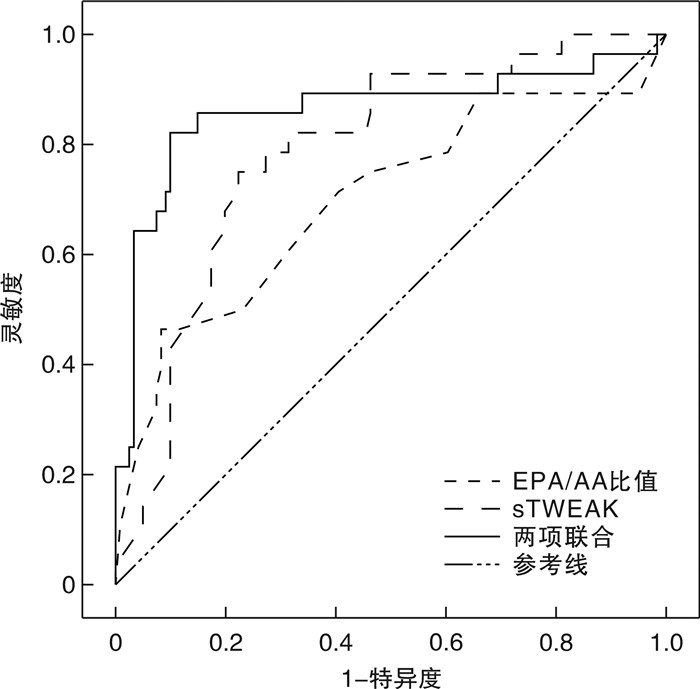
指标 灵敏度/% 特异度/% 截断值 AUC 95%CI 约登指数 EPA/AA比值 76.23 68.20 0.37 0.762 0.674~0.851 0.444 sTWEAK 78.64 70.12 279.6 pg/mL 0.741 0.657~0.826 0.487 两项联合 83.32 98.11 - 0.899 0.822~0.976 0.814 -
[1] 《中国脑卒中防治报告2020》编写组, 王陇德. 《中国脑卒中防治报告2020》概要[J]. 中国脑血管病杂志, 2022, 19(2): 136-144.
[2] 乔小利, 王厚清, 燕宪亮, 等. 急性脑梗死并发上消化道出血患者预后的影响因素[J]. 临床急诊杂志, 2023, 24(8): 387-393. https://lcjz.whuhzzs.com/article/doi/10.13201/j.issn.1009-5918.2023.08.001
[3] 徐瑶, 王从凯, 王富元, 等. 西洛他唑在急性脑梗死患者rt-PA溶栓治疗后的作用及对血清CD62p、CD63、PAF的作用分析[J]. 现代生物医学进展, 2022, 22(20): 3982-3986.
[4] 王岩, 倪耀辉, 李爱红. 脑白质疏松与急性脑梗死溶栓后出血转化及临床预后的相关性[J]. 脑与神经疾病杂志, 2023, 31(1): 52-57.
[5] 陈宏权, 陈云森, 王磊, 等. 缺血性脑小血管病与血生物标志物相关研究[J]. 中华老年心脑血管病杂志, 2020, 22(12): 1251-1254. doi: 10.3969/j.issn.1009-0126.2020.12.006
[6] 吕书悦, 李松涛, 吴凡, 等. 老年患者血管源性脑白质病变与血游离脂肪酸的相关性研究[J]. 中国实验诊断学, 2022, 26(8): 1194-1198. doi: 10.3969/j.issn.1007-4287.2022.08.028
[7] Nelson JR, Raskin S. The eicosapentaenoic acid: arachidonic acid ratio and its clinical utility in cardiovascular disease[J]. Postgrad Med, 2019, 131(4): 268-277. doi: 10.1080/00325481.2019.1607414
[8] 卜一, 窦志杰, 张硕, 等. 急性脑梗死患者早期血清可溶性肿瘤坏死因子样弱凋亡诱导剂水平与脑白质病变的相关性[J]. 临床和实验医学杂志, 2022, 21(22): 2368-2370. doi: 10.3969/j.issn.1671-4695.2022.22.005
[9] 中华医学会神经病学分会, 中华医学会神经病学分会脑血管病学组. 中国急性缺血性脑卒中诊治指南2018[J]. 中华神经科杂志, 2018, 51(9): 666-682. doi: 10.3760/cma.j.issn.1006-7876.2018.09.004
[10] 廖丹, 许丽. 血浆同型半胱氨酸与脑微出血及脑白质疏松分级的相关性研究[J]. 中国实验诊断学, 2020, 24(5): 777-780.
[11] Suh CH, Jung SC, Cho SJ, et al. MRI for prediction of hemorrhagic transformation in acute ischemic stroke: a systematic review and meta-analysis[J]. Acta Radiol, 2020, 61(7): 964-972. doi: 10.1177/0284185119887593
[12] York SN. Modified Rankin Scale[J]. Encyclopedia of Clinical Neuropsychology, 2011, 40(3): 438-445.
[13] 杨京东, 宋焱. 脑白质疏松与缺血性卒中及颅内外动脉硬化关系的研究进展[J]. 国际医学放射学杂志, 2019, 42(6): 673-677, 683.
[14] 陈俊培, 黄昌志, 蒙定程. 凝血因子ⅩⅢ水平与急性脑卒中患者溶栓治疗后出血转化风险的相关性[J]. 临床急诊杂志, 2023, 24(2): 68-72. https://lcjz.whuhzzs.com/article/doi/10.13201/j.issn.1009-5918.2023.02.004
[15] 李佳润, 范琰, 刘梅林. 二十碳五烯酸防治心血管疾病的进展[J]. 中国临床研究, 2021, 34(10): 1423-1426.
[16] 李春, 赵高峰, 薛文华, 等. 二十碳五烯酸对急性脑梗死大鼠梗死体积, 神经功能及氧化应激-炎症反应的影响[J]. 郑州大学学报(医学版), 2021, 56(4): 475-479.
[17] 陈义明, 易兴阳, 余泽珍, 等. 花生四烯酸代谢产物20-HETE、EETs、DHETs与脑梗死相关性研究[J]. 浙江医学, 2018, 40(9): 968-969.
[18] 宁珑, 孙航, 冯晋, 等. 花生四烯酸诱导建立大鼠弥漫性脑血栓模型[J]. 实验动物与比较医学, 2022, 42(2): 141-145.
[19] Fukuda S, Fujioka S, Hosaka S, et al. Relationship between arteriosclerosis obliterans and the ratio of serum eicosapentaenoic acid to arachidonic acid[J]. Ann Thorac Cardiovasc Surg, 2014, 20(1): 44-47. doi: 10.5761/atcs.oa.12.02063
[20] Shojima Y, Ueno Y, Tanaka R, et al. Eicosapentaenoic-to-Arachidonic Acid Ratio Predicts Mortality and Recurrent Vascular Events in Ischemic Stroke Patients[J]. J Atheroscler Thromb, 2020, 27(9): 969-977. doi: 10.5551/jat.52373
[21] 吴月, 殷梅. 炎症反应与急性缺血性脑卒中静脉溶栓后出血转化的研究进展[J]. 神经疾病与精神卫生, 2020, 20(12): 890-894.
[22] 段秋艳, 宋文玲, 徐萍. sTWEAK, MMP-9与急性ST段抬高型心肌梗死关系的临床研究进展[J]. 心脏杂志, 2019, 31(5): 602-605.
[23] Méndez-Barbero N, Gutiérrez-Muñoz C, Blázquez-Serra R, et al. Tumor Necrosis Factor-Like Weak Inducer of Apoptosis(TWEAK)/Fibroblast Growth Factor-Inducible 14(Fn14) Axis in Cardiovascular Diseases: Progress and Challenges[J]. Cells, 2020, 9(2): 405.
[24] Stephan D, Roger A, Aghzadi J, et al. TWEAK and TNFα, Both TNF Ligand Family Members and Multiple Sclerosis-Related Cytokines, Induce Distinct Gene Response in Human Brain Microvascular Endothelial Cells[J]. Genes(Basel), 2022, 13(10): 1714.
-




 下载:
下载:
