Factors influencing the prognosis of patients with acute cerebral infarction complicated by upper gastrointestinal bleeding
-
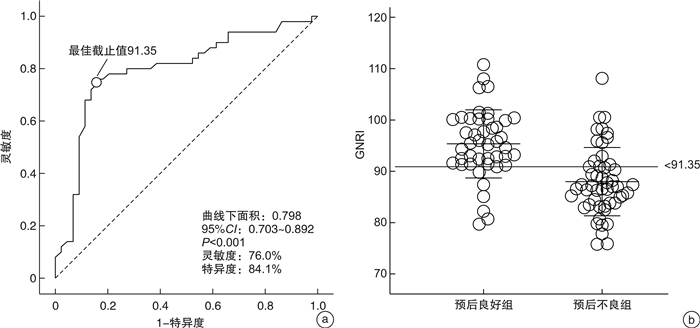
摘要: 目的 分析急性脑梗死并发上消化道出血患者预后的影响因素。方法 选取2015年3月-2022年10月在徐州医科大学附属医院住院且符合纳入及排除标准的住院期间并发上消化道出血的急性脑梗死患者94例为研究对象。采用改良Rankin量表(mRS)评分通过电话随访以评价发病90 d预后情况,按照发病90 d mRS评分是否≤2分,分为预后良好组(44例)和预后不良组(50例)。收集患者的临床资料和实验室检查资料,并计算患者的老年人营养风险指数(geriatric nutritional risk index, GNRI)评分。采用多因素logistic回归分析影响急性脑梗死并发上消化道出血患者预后的影响因素;采用受试者工作特征(ROC)曲线分析GNRI对急性脑梗死并发上消化道出血患者的预测价值。结果 预后不良组既往饮酒、丘脑或脑干梗死、大面积脑梗死、出血量≥800 mL、入住ICU等占比、入院美国国立卫生研究院卒中量表(National Institute of Health stroke scale,NIHSS)评分、出院NIHSS评分明显高于预后良好组,血红蛋白、白蛋白、GNRI明显低于预后良好组,差异有统计学意义(P < 0.05)。多因素logistic回归分析显示,饮酒(OR:7.169,95%CI:1.677~30.645,P=0.008)、丘脑或脑干梗死(OR:99.255,95%CI:14.190~694.273,P < 0.001)是急性脑梗死并发上消化道出血患者预后的独立危险因素;GNRI(OR:0.823,95%CI:0.741~0.914,P < 0.001)是急性脑梗死并发上消化道出血患者预后的保护因素。GNRI评估急性脑梗死并发上消化道出血患者预后不良的曲线下面积为0.798(P < 0.05)。结论 饮酒、丘脑或脑干梗死、GNRI是急性脑梗死并发上消化道出血患者预后不良的独立危险因素。急性脑梗死并发上消化道出血患者营养不良与预后风险增加有关。GNRI有助于评估急性脑梗死并发上消化道出血患者预后。Abstract: Objective To analyze the factors influencing the prognosis of patients with acute cerebral infarction complicated by gastrointestinal bleeding.Methods Ninety-four patients with acute cerebral infarction complicated by gastrointestinal bleeding during hospitalization who met the inclusion and exclusion criteria and were admitted to the Affiliated Hospital of Xuzhou Medical University from March 2015 to October 2022 were selected for the study. The prognosis at 90 days of onset was evaluated by telephone follow-up using the modified Rankin scale(mRS) score, and the patients were divided into a good prognosis group(44 cases) and a poor prognosis group(50 cases) according to whether the mRS score was ≤2 at 90 days of onset. The patients' clinical data and laboratory tests were collected, and the patients' geriatric nutritional risk index(GNRI) scores for the elderly were calculated. Multi-factor logistic regression was used to analyze the factors influencing the prognosis of patients with acute cerebral infarction complicated by gastrointestinal bleeding; the subject work characteristic(ROC) curve was used to analyze the predictive value of the GNRI for patients with acute cerebral infarction complicated by gastrointestinal bleeding.Results The proportion of previous alcohol consumption, thalamic or brainstem infarction, large cerebral infarction, bleeding ≥800 mL, ICU admission, admission National Institutes of Health Stroke scale(NIHSS) score, and discharge NIHSS score were significantly higher in the poor prognosis group than in the good prognosis group, and hemoglobin, albumin, and GNRI were significantly lower than in the good prognosis group, with statistically significant differences(P < 0.05). Multi-factor logistic regression analysis showed that Alcohol consumption, thalamic or brainstem infarction, and GNRI in the elderly were independent risk factors for the prognosis of patients with acute cerebral infarction complicated by gastrointestinal bleeding(P < 0.05).The area under the curve of GNRI to assess the poor prognosis of patients with acute cerebral infarction complicated by gastrointestinal bleeding was 0.798(P < 0.05).Conclusion Alcohol consumption, thalamic or brainstem infarction, and GNRI in the elderly are independent risk factors for poor prognosis in patients with acute cerebral infarction complicated by gastrointestinal bleeding. Malnutrition in patients with acute cerebral infarction complicated by gastrointestinal hemorrhage was associated with increased prognostic fractional risk. The GNRI is useful for assessing the prognosis of patients with acute cerebral infarction complicated by gastrointestinal hemorrhage.
-

-
表 1 预后良好组与预后不良组一般临床资料和营养指标比较
项目 预后良好组(44例) 预后不良组(50例) χ2/t/Z P 男性/例(%) 30(68.2) 34(68.0) 0.001 0.985 年龄/岁 73.82±8.9 70.24±10.78 1.740 0.085 BMI/(kg/m2) 23.96±4.07 23.10±3.39 1.121 0.069 高血压/例(%) 26(59.1) 32(64.0) 0.239 0.625 糖尿病/例(%) 19(43.2) 16(32.0) 1.252 0.263 冠心病/例(%) 8(18.2) 9(18.0) 0.001 0.982 房颤/例(%) 4(9.1) 3(6.0) 0.031 0.860 高脂血症/例(%) 6(13.6) 3(6.0) 0.818 0.366 脑血管病史/例(%) 21(47.7) 18(36.0) 1.326 0.250 吸烟/例(%) 11(25.0) 15(30.0) 0.292 0.589 饮酒/例(%) 10(22.7) 21(42.0) 3.933 0.047 卒中发生至上消化道出血时间/d 5(2,10.75) 5(2,12.00) 0.279 0.780 丘脑或脑干梗死/例(%) 3(6.8) 34(68.0) 36.704 < 0.05 大面积脑梗死/例(%) 9(20.5) 24(48.0) 7.795 < 0.05 出血量≥800 mL/例(%) 3(6.8) 24(48.0) 19.388 < 0.05 入住ICU/例(%) 8(18.2) 39(78.0) 33.498 < 0.05 既往口服抗栓药物/例(%) 27(61.4) 26(52.0) 0.497 0.481 溶栓/例(%) 6(13.6) 8(16.0) 0.001 0.975 取栓/例(%) 0(0) 2(4.0) 0.497 住院天数/d 10(7,20.75) 12(5,19.5) 0.152 0.879 入院GCS评分/分 15(13,15) 11(7.75,13) 28.504 < 0.05 入院NIHSS评分/分 5(3.0,8.0) 14.5(10.0,18.0) 5.226 < 0.05 出院NIHSS评分/分 7(4.0,13.75) 22(16.0,35.0) 5.588 < 0.05 血红蛋白/(g/L) 101.43±27.47 89.80±22.12 2.272 0.025 血清白蛋白/(g/L) 37.21±3.34 32.31±4.29 6.121 < 0.05 NRS2002/分 3.57±1.17 3.66±1.14 0.386 0.809 GNRI/分 95.35±6.64 87.99±6.66 5.349 < 0.05 注:GNRI=14.89×白蛋白(g/dL)+ 41.7×(体重/理想体重)。 表 2 AIS并发上消化道出血患者预后影响因素的多因素logistic回归分析
项目 B Wald OR 95%CI P 饮酒 1.970 7.062 7.169 1.677~30.645 0.008 丘脑或脑干梗死 4.598 21.461 99.255 14.190~694.273 < 0.001 GNRI -0.195 13.170 0.823 0.741~0.914 < 0.001 -
[1] 刘鸣, 贺茂林. 中国急性缺血性脑卒中诊治指南2014[J]. 中华神经科杂志, 2015, 48(4): 246-257. doi: 10.3760/cma.j.issn.1006-7876.2015.04.002
[2] 李艳, 王丽丽, 曹雪芳, 等. 主动监测胃残留对早期卒中患者应激性消化性溃疡的研究进展[J]. 临床医药文献电子杂志, 2017, 4(68): 13447. doi: 10.3877/j.issn.2095-8242.2017.68.129
[3] O'Donnell MJ, Kapral MK, Fang J, et al. Gastrointestinal bleeding after acute ischemic stroke[J]. Neurology, 2008, 71(9): 650-655. doi: 10.1212/01.wnl.0000319689.48946.25
[4] 李映彩, 冷军, 孟祥志, 等. 近5年脑卒中吞咽障碍研究进展的可视化分析[J]. 中国康复理论与实践, 2022, 28(9): 1049-1059. https://www.cnki.com.cn/Article/CJFDTOTAL-ZKLS202209007.htm
[5] Kang Y, Shuanggen Z, Huaiming W, et al. Association between malnutrition and long-term mortality in older adults with ischemic stroke[J]. Clinical Nutrition, 2021, 40(5): 2535-2542. doi: 10.1016/j.clnu.2021.04.018
[6] 王拥军, 赵性泉, 王少石, 等. 中国卒中营养标准化管理专家共识[J]. 中国卒中杂志, 2020, 15(6): 681-689. doi: 10.3969/j.issn.1673-5765.2020.06.019
[7] Chen Y, Yang XG, Zhu YY, et al. Malnutrition Defined by Geriatric Nutritional Risk Index Predicts Outcomes in Severe Stroke Patients: A Propensity Score-Matched Analysis[J]. Nutrients, 2022, 14(22): 4786. doi: 10.3390/nu14224786
[8] 彭斌, 吴波. 中国急性缺血性脑卒中诊治指南(2018)[J]. 中华神经科杂志, 2018, 51(9): 666-682. doi: 10.3760/cma.j.issn.1006-7876.2018.09.004
[9] 柏愚, 李延青, 任旭, 等. 应激性溃疡防治专家建议(2018版)[J]. 中华医学杂志, 2018, 98(42): 3392-3395. doi: 10.3760/cma.j.issn.0376-2491.2018.42.003
[10] 《中华内科杂志》编辑委员会, 《中华医学杂志》编辑委员会, 《中华消化杂志》编辑委员会, 等. 急性非静脉曲张性上消化道出血诊治指南(2018年, 杭州)[J]. 中华内科杂志, 2019, 58(3): 173-180. doi: 10.3760/cma.j.issn.0578-1426.2019.03.005
[11] 许铁, 张劲松, 燕宪亮. 急救医学[M]. 南京: 东南大学出版社, 2019: 618.
[12] 焦延军, 王永霞, 陈勇. 消化道出血失血程度的判断及参考指标[J]. 中国社区医师(医学专业), 2010, 12(26): 158. doi: 10.3969/j.issn.1007-614x.2010.26.176
[13] Kondrup J, Rasmussen HH, Hamberg O, et al. Nutrition risk screening(NRS 2002): a controlled clinical trials[J]. Clin Nutr, 2003, 22(3): 321-336. doi: 10.1016/S0261-5614(02)00214-5
[14] Derya Y, Ozgur CM. The comparison of GNRI and other nutritional indexes on short-term survival in geriatric patients treated for respiratory failure[J]. Ag Clin Experim Res, 2021, 33(3): 611-617. doi: 10.1007/s40520-020-01740-8
[15] Kenichiro Y, Yuichiro I, Makoto N, et al. Reliability of the Modified Rankin scale Assessment Using a Simplified Questionnaire in Japanese[J]. J Stroke Cerebrovascular Dis, 2021, 30(2): 105517. doi: 10.1016/j.jstrokecerebrovasdis.2020.105517
[16] Hsu HL, Lin YH, Huang YC, et al. Gastrointestinal hemorrhage after acute ischemic stroke and its risk factors in Asians[J]. Eur Neurol, 2009, 62(4): 212-218. doi: 10.1159/000229018
[17] 刘佳, 吴建维. 急性缺血性卒中患者发生院内消化道出血的危险因素分析[J]. 中国卒中杂志, 2020, 15(10): 1083-1087. doi: 10.3969/j.issn.1673-5765.2020.10.010
[18] Ogata T, Kamouchi M, Matsuo R. Gastrointestinal Bleeding in Acute Ischemic Stroke: Recent Trends from the Fukuoka Stroke Registry[J]. Cerebrovascular Dis Extra, 2014, 4(2): 156-164. doi: 10.1159/000365245
[19] 翁山山, 聂虎. 创伤性脑损伤相关神经特异性血清生物学标记物的研究进展[J]. 临床急诊杂志, 2020, 21(3): 249-256. https://www.cnki.com.cn/Article/CJFDTOTAL-ZZLC202003018.htm
[20] 颜雪琴, 陈勇. 急性脑梗死并发上消化道出血相关因素的临床分析[J]. 标记免疫分析与临床, 2017, 24(7): 770-773, 811. https://www.cnki.com.cn/Article/CJFDTOTAL-BJMY201707012.htm
[21] Cui P, McCullough LD, Hao JW. Brain to periphery in acute ischemic stroke: mechanisms and clinical significance[J]. Frontiers Neuroendocrinol, 2021, 63: 100932. doi: 10.1016/j.yfrne.2021.100932
[22] 许颖玲. 重症脑卒中患者肠内营养支持期间发生上消化道出血的影响因素分析[J]. 现代诊断与治疗, 2021, 32(11): 1781-1782. https://www.cnki.com.cn/Article/CJFDTOTAL-XDZD202111050.htm
[23] Wu D, Shen L, Yang R, et al. Dynamic Change of Acute Infarct Volume in Patients with Acute Ischemic Stroke[J]. Stroke, 2017, 48(9): 2454-2460.
[24] Maier B, Desilles JP, Labreuche J, et al. Evolution of cerebral infarct volume assessed by magnetic resonance imaging in acute stroke patients treated with mechanical thrombectomy[J]. J Neuroradiol, 2018, 45(4): 232-237.
[25] 王欢欢, 刘霖, 高莹卉, 等. 老年阻塞性睡眠呼吸暂停低通气相关高血压患者颈动脉粥样硬化的影响因素[J]. 中华老年多器官疾病杂志, 2022, 21(6): 413-419. https://www.cnki.com.cn/Article/CJFDTOTAL-ZLQG202206003.htm
[26] 张欣玉, 毛森林, 张本平, 等. 丘脑梗死的特点及对认知功能的影响[J]. 中华老年心脑血管病杂志, 2019, 21(9): 1006-1008. https://www.cnki.com.cn/Article/CJFDTOTAL-LNXG201909032.htm
[27] 孙鹏慧, 李莹莹, 刘鑫, 等. 卒中相关性肺炎患者神经功能恶化的影像指标及其预测价值分析[J]. 首都医科大学学报, 2022, 43(1): 74-81. https://www.cnki.com.cn/Article/CJFDTOTAL-SDYD202201014.htm
[28] Cook DJ, Fuller HD, Guyatt GH, et al. Risk factors for gastrointestinal bleeding in critically ill patients. Canadian Critical Care Trials Group[J]. N Engl J Med, 1994, 330(6): 377-81.
[29] Du WL, Zhao XQ, Wang YL, et al. Gastrointestinal bleeding during acute ischaemic stroke hospitalisation increases the risk of stroke recurrence[J]. Stroke Vascul Neurol, 2020, 5(2): 116-120.
[30] Kim Y, Kim CK, Jung S, et al. Prognostic importance of weight change on short-term functional outcome in acute ischemic stroke[J]. Int J Stroke, 2015, 10(SA100): 62-68.
[31] Mao SY, Hu YH, Zheng XW, et al. Correlation Analysis of Neutrophil/Albumin Ratio and Leukocyte Count/Albumin Ratio with Ischemic Stroke Severity[J]. Cardiol Cardiovascular Med, 2023, 7(1): 32-38.
[32] Park H, Hong M, Gil-Ja Jhon GJ, et al. Repeated Oral Administration of Human Serum Albumin Protects from the Cerebral Ischemia in Rat Brain Following MCAO[J]. Exp Neurobiol, 2017, 26(3): 151-157.
[33] Wang CY, Deng LH, Qiu S, et al. Serum Albumin Is Negatively Associated with Hemorrhagic Transformation in Acute Ischemic Stroke Patients[J]. Cerebrovasc Dis(Basel, Switzerland), 2019, 47(1-2): 88-94.
[34] 杨田军, 费明明, 叶文, 等. 血浆白蛋白及血红蛋白水平对单纯严重脑外伤患者预后影响的回顾性队列研究[J]. 中华危重病急救医学, 2013, 25(5): 301-305.
[35] Minwoo L, Jaesung L, Yerim K, et al. Association between Geriatric Nutritional Risk Index and Post-Stroke Cognitive Outcomes[J]. Nutrients, 2021, 13(6): 1776.
[36] Shoji T, Yuta M, Yasuhiro K, et al. Association between geriatric nutritional risk index and stroke risk in hemodialysis patients: 10-Years outcome of the Q-Cohort study[J]. Atherosclerosis, 2021, 323: 30-36.
[37] 李文静, 李树仁, 孙明超, 等. 老年人营养风险指数预测住院慢性心力衰竭患者的预后研究[J]. 中国全科医学, 2021, 24(23): 2955-2961. https://www.cnki.com.cn/Article/CJFDTOTAL-QKYX202123028.htm
[38] Hu J, Chen T, Wang Z, et al. Geriatric Nutritional Risk Index and the Prognosis of Patients with Stroke: A Meta-Analysis[J]. Horm metab res, 2022, 54(11): 736-746.
[39] 李喆楠, 王军民, 王毅兰. 急性上消化道出血的急诊处理与内镜下诊疗进展[J]. 临床急诊杂志, 2023, 24(6): 326-330. https://lcjz.whuhzzs.com/article/doi/10.13201/j.issn.1009-5918.2023.06.010
-




 下载:
下载: