Analysis of influencing factors on the recent neurological prognosis of AIS patients receiving pre-hospital RIC combined with intra hospital thrombolysis therapy
-
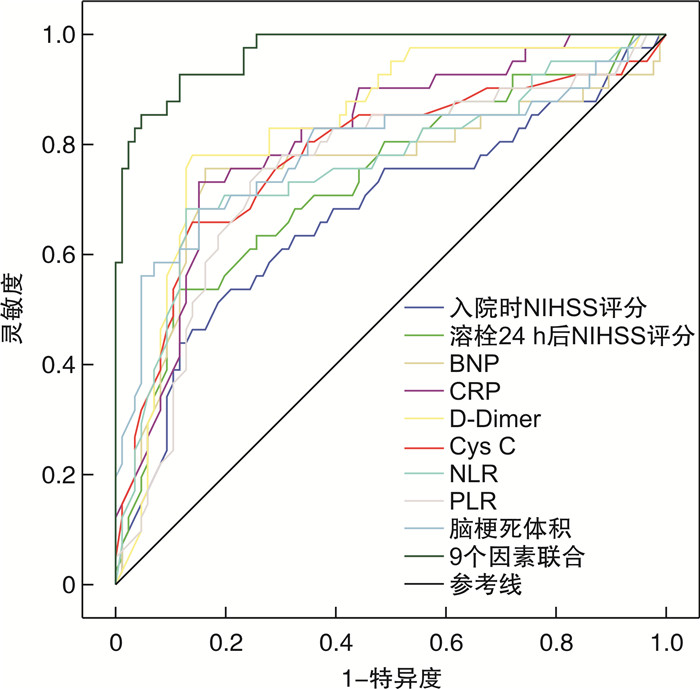
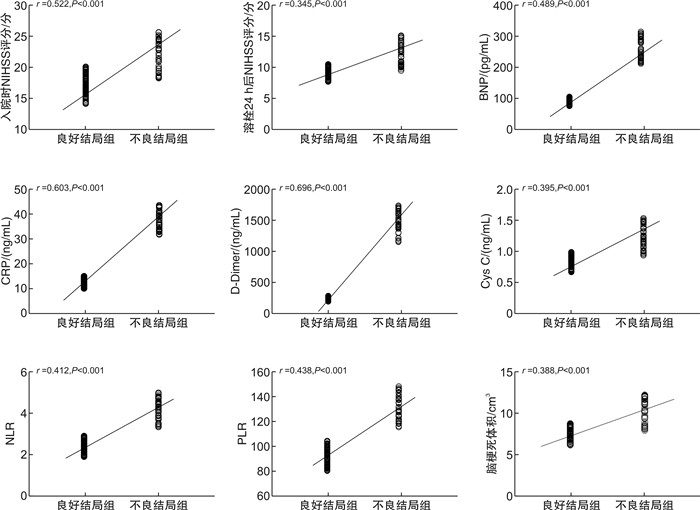
摘要: 目的 探讨急性缺血性脑卒中(acute ischemic stroke,AIS)患者接受院前远隔缺血适应(remote ischemic conditioning,RIC)联合院内溶栓治疗后近期神经功能预后的影响因素。方法 回顾性选择2020年1月—2023年1月我院行院前RIC+院内溶栓的127例AIS患者为观察组,将同期在我院行溶栓而未进行RIC治疗的AIS患者50例纳至对照组,比较分析两组治疗效果与预后情况。根据127例AIS患者近期神经功能预后情况,将其分为良好结局组与不良结局组,比较两组临床资料及实验室指标,分析AIS近期神经功能预后的危险因素,分析各因素/指标与AIS近期神经功能预后的相关性,评价各因素/指标对AIS近期神经功能预后的预测效能。结果 观察组治疗总有效率显著高于对照组,差异有统计学意义(P < 0.05);不良结局率显著低于对照组,差异有统计学意义(P < 0.05)。与良好结局组比较,不良结局组年龄、糖尿病史占比、冠心病史占比、入院时美国国立卫生研究院卒中量表(national institute of health stroke scale,NIHSS)评分、溶栓24 h后NIHSS评分、脑钠肽(brain natriuretic peptide,BNP)、C-反应蛋白(C-reactive protein,CRP)、D-二聚体(D-Dimer)、胱抑素C(Cystatin C,Cys C)、中性粒细胞/淋巴细胞比值(neutrophil-to-lymphocyte ratio,NLR)、血小板/淋巴细胞比值(platelet-to-lymphocyte ratio,PLR)、脑梗死体积明显升高,差异有统计学意义(P < 0.05)。logistic回归模型显示,入院时NIHSS评分、溶栓24 h后NIHSS评分、BNP、CRP、D-Dimer、Cys C、NLR、PLR、脑梗死体积为AIS患者近期神经功能预后的危险因素(P < 0.05)。Spearman检验提示,AIS患者近期神经功能预后与入院时NIHSS评分、溶栓24 h后NIHSS评分、BNP、CRP、D-Dimer、Cys C、NLR、PLR、脑梗死体积呈正相关(P < 0.05)。绘制ROC曲线发现,9个因素(入院时NIHSS评分、溶栓24 h后NIHSS评分、BNP、CRP、D-Dimer、Cys C、NLR、PLR、脑梗死体积)联合预测AIS近期神经功能预后的AUC值、灵敏度、特异度为0.948、80.50、94.23,其效能明显优于单一指标,差异有统计学意义(P < 0.05)。结论 入院时NIHSS评分、溶栓24 h后NIHSS评分、脑梗死体积、BNP、CRP、D-Dimer、Cys C、NLR、PLR升高为AIS患者近期神经功能预后的危险因素,并对预后不良有较好的预测价值。Abstract: Objective To explore the influencing factors of recent neurological prognosis in patients with acute ischemic stroke(AIS) after receiving pre hospital remote ischemic adaptation(RIC) combined with intra hospital thrombolysis therapy.Methods Retrospectively selection of 127 AIS patients who underwent pre-hospital RIC and intra-hospital thrombolysis in our hospital from January 2020 to January 2023 were retrospectively selected as the observation group, 50 AIS patients who underwent thrombolysis in our hospital during the same period but did not receive RIC treatment were selected as the control group.The treatment efficacy and prognosis of the two groups were compared and analyzed. Based on the recent neurological prognosis of 127 AIS patients, they were divided into a good outcome group and adverse outcome group. Clinical data and laboratory indicators were compared between the two groups, and the risk factors for recent neurological prognosis of AIS were analyzed. The correlation between each factor/indicator and recent neurological prognosis of AIS was analyzed, and the predictive efficacy of each factor/indicator on recent neurological prognosis of AIS was evaluated.Results The total effective rate of the observation group was significantly higher than that of the control group(P < 0.05), and the adverse outcome rate was significantly lower than that of the control group(P < 0.05). Compared with the good outcome group, the age, the proportion of diabetes history, the proportion of coronary heart disease history, the national institute of health stroke scale(NIHSS) score at admission, the NIHSS score 24 hours after thrombolysis, brain natriuretic peptide(BNP), C-reactive protein(CRP), D-Dimer, cystatin C(Cys C), neutrophil/lymphocyte ratio(NLR), platelet/lymphocyte ratio(PLR), and cerebral infarction volume in the adverse outcome group increased significantly(P < 0.05). The logistic regression model showed that NIHSS score at admission, NIHSS score 24 hours after thrombolysis, BNP, CRP, D-Dimer, Cys C, NLR, PLR, and cerebral infarction volume were risk factors for the recent neurological prognosis of AIS patients(P < 0.05). Spearman test showed that the recent neurological prognosis of AIS patients was positively correlated with NIHSS score at admission, NIHSS score 24 hours after thrombolysis, BNP, CRP, D-Dimer, Cys C, NLR, PLR and cerebral infarction volume(P < 0.05). Drawing the ROC curve, it was found that the AUC value, sensitivity and specificity of combining nine factors (NIHSS score at admission, NIHSS score 24 hours after thrombolysis, BNP, CRP, D-Dimer, Cys C, NLR, PLR, and cerebral infarction volume) for predicting the recent neurological prognosis in AIS were 0.948, 80.50 and 94.23, respectively. And their efficacy was significantly better than any single indicator (P < 0.05).Conclusion The NIHSS score at admission, the NIHSS score 24 hours after thrombolysis, cerebral infarction volume, BNP, CRP, D-Dimer, Cys C, NLR, and PLR elevation are risk factors for the recent neurological prognosis of AIS patients, and have good predictive value for poor prognosis.
-

-
表 1 两组疗效及预后情况比较
例(%) 分组 例数 显效 有效 无效 总有效 不良结局 对照组 50 27 8 15 35(70.00) 26(52.00) 观察组 127 95 21 11 116(91.34) 41(32.28) χ2 13.035 5.928 P < 0.001 0.015 表 2 AIS患者近期神经功能预后的单因素分析
X±S 资料 良好结局组(86例) 不良结局组(41例) χ2/t P 年龄/岁 65.46±5.62 68.37±5.04 2.818 0.006 入院时NIHSS评分/分 17.26±3.11 21.63±4.12 6.022 < 0.001 溶栓24 h后NIHSS评分/分 9.16±1.43 12.28±2.94 6.441 < 0.001 脑梗死体积/cm3 7.12±1.26 9.83±2.24 7.221 < 0.001 BMI/(kg/m2) 22.61±2.23 22.20±2.47 0.935 0.351 性别/例 0.196 0.657 男 51 26 女 35 15 吸烟史/例 0.336 0.562 有 25 14 无 61 27 饮酒史/例 1.242 0.265 有 27 17 无 59 24 高血脂史/例 0.194 0.659 有 24 13 无 62 28 高血压史/例 0.773 0.379 有 54 29 无 32 12 糖尿病史/例 4.817 0.028 有 23 19 无 63 22 冠心病史/例 7.537 0.006 有 21 20 无 65 21 脑动脉闭塞部位/例 0.552 0.457 颅内动脉 48 20 颈内动脉 38 21 BNP/(pg/mL) 91.12±15.33 264.19±52.56 20.669 < 0.001 CRP/(mg/L) 12.45±2.54 37.69±6.12 25.385 < 0.001 D-Dimer/(ng/mL) 240.49±45.72 1449.70±293.06 26.268 < 0.001 Cys C/(mg/L) 0.83±0.16 1.24±0.30 8.211 < 0.001 NLR 2.41±0.51 3.53±0.84 7.873 < 0.001 PLR 92.27±12.46 131.88±17.30 13.127 < 0.001 WBC/(×109/L) 9.92±2.03 10.37±2.17 1.142 0.256 TG/(mmol/L) 1.48±0.35 1.57±0.37 1.330 0.186 TC/(mmol/L) 4.59±1.12 4.68±1.14 0.421 0.675 LDL-C/(mmol/l) 2.46±0.56 2.38±0.57 0.748 0.456 HDL-C/(mmol/L) 1.37±0.32 1.44±0.33 1.141 0.256 表 3 AIS患者近期神经功能预后的多因素分析
变量 赋值 β SE Wald P OR 95%CI 年龄 原值带入 0.112 0.176 0.400 0.538 1.118 0.731~1.459 入院时NIHSS评分 原值带入 0.423 0.176 5.771 0.016 1.527 1.243~2.480 溶栓24 h后NIHSS评分 原值带入 0.562 0.196 8.180 0.004 1.754 1.312~2.834 脑梗死体积 原值带入 0.465 0.174 7.168 0.007 1.592 1.267~2.503 糖尿病史 有=1;无=0 0.267 0.263 1.034 0.314 1.306 0.673~1.884 冠心病史 有=1;无=0 0.198 0.163 1.480 0.226 1.219 0.830~1.571 BNP 原值带入 0.958 0.258 13.784 < 0.001 2.606 1.531~4.209 CRP 原值带入 0.925 0.243 14.495 < 0.001 2.523 1.482~3.843 D-Dimer 原值带入 1.082 0.261 17.209 < 0.001 2.950 1.859~5.167 Cys C 原值带入 1.152 0.375 9.455 0.002 3.165 2.366~10.278 NLR 原值带入 0.828 0.216 14.620 < 0.001 2.288 1.481~3.460 PLR 原值带入 1.011 0.239 17.884 < 0.001 2.749 1.728~4.412 表 4 各因素预测AIS近期神经功能预后的效能
变量 截断值 AUC 灵敏度/% 特异度/% P 入院时NIHSS评分 19.63分 0.674 53.71 79.11 0.002 溶栓24 h后NIHSS评分 10.66分 0.734 53.72 88.40 < 0.001 BNP 159.20 pg/mL 0.755 75.60 83.70 < 0.001 CRP 23.38 mg/L 0.810 73.23 84.92 < 0.001 D-Dimer 721.76 ng/mL 0.834 78.02 86.01 < 0.001 Cys C 0.98 mg/L 0.780 65.91 86.02 < 0.001 NLR 3.14 0.762 68.31 87.21 < 0.001 PLR 109.59 0.752 75.62 73.30 < 0.001 脑梗死体积 8.09 cm3 0.790 68.31 84.90 < 0.001 9个因素联合 - 0.969 92.72 88.50 < 0.001 -
[1] 赵嵩, 伊德日, 钱永刚, 等. 内蒙古自治区脑卒中高危人群筛查及主要危险因素流行病学分布[J]. 现代预防医学, 2023, 50(4): 6-9.
[2] 陈俊培, 黄昌志, 蒙定程. 凝血因子ⅩⅢ水平与急性脑卒中患者溶栓治疗后出血转化风险的相关性[J]. 临床急诊杂志, 2023, 24(2): 68-72. https://lcjz.whuhzzs.com/article/doi/10.13201/j.issn.1009-5918.2023.02.004
[3] 胡汉国, 邓小斌, 陈韧刚. 血清Lp-PLA2, 炎症因子预测AIS静脉溶栓治疗近期预后的价值[J]. 现代科学仪器, 2022, 39(4): 55-56.
[4] Amorim S, Felício AC, Aagaard P, et al. Effects of remote ischemic conditioning on cognitive performance: A systematic review[J]. Physiol Behav, 2022, 254: 113893.
[5] 赵文博, 李思颉, 吉训明. 《远隔缺血适应防治缺血性脑血管病中国专家共识》解读[J]. 中国脑血管病杂志, 2021, 18(9): 5-11.
[6] 孙维明, 王桂华, 张颖, 等. 急性缺血性卒中患者静脉溶栓前应用远隔缺血前适应的随机对照研究[J]. 北京医学, 2022, 44(12): 69-71.
[7] 中华医学会神经病学分会, 中华医学会神经病学分会脑血管病学组. 中国急性缺血性脑卒中诊治指南2018[J]. 中华神经科杂志, 2018, 51(9): 17-20.
[8] 武磊. 阿加曲班丁苯酞在治疗急性缺血性脑卒中的临床疗效[J]. 中国药物与临床, 2021, 6(8): 40-44.
[9] 王萍, 孟令杰, 吕婷, 等. 优质护理服务在老年性脑梗塞护理中应用对患者NIHSS评分的影响[J]. 现代消化及介入诊疗, 2022, 2(1): 256-259.
[10] 庞文冲, 陈志强, 张志辉, 等. 发病4.5 h内急性大血管闭塞性缺血性脑卒中患者直接取栓及桥接治疗的效果及安全性观察[J]. 齐齐哈尔医学院学报, 2022, 8(1): 43-46.
[11] 刘爱芹, 岳冬雪, 张津溶, 等. 不同mRS评分的急性缺血性脑卒中患者血清PTX3, GAL3, Npt水平[J]. 中国老年学杂志, 2021, 41(21): 34-37.
[12] 贾丽娇, 王雨, 孙炎, 等. 吲哚布芬与阿司匹林对急性轻型缺血性脑卒中的临床疗效对比研究[J]. 临床急诊杂志, 2022, 23(5): 332-336. https://lcjz.whuhzzs.com/article/doi/10.13201/j.issn.1009-5918.2022.05.007
[13] 张雷, 孔祥丽, 李军朝, 等. 远隔缺血适应联合静脉溶栓对急性脑梗死患者临床预后及氧化应激表达的影响[J]. 中国脑血管病杂志, 2022, 19(9): 7-9.
[14] 齐爽. 远隔缺血处理对脑卒中静脉溶栓患者脑血流自动调节改善作用的研究[D]. 吉林大学, 2022.
[15] 苏俊, 李鑫海. 肢体缺血预适应联合超早期静脉溶栓减轻急性脑梗死患者神经功能缺损并改善预后[J]. 内科急危重症杂志, 2021, 27(6): 4-12.
[16] 张雷, 孔祥丽, 李军朝, 等. 远隔缺血适应联合静脉溶栓对急性脑梗死患者临床预后及氧化应激表达的影响[J]. 中国脑血管病杂志, 2022, 19(9): 7-8.
[17] 崔艳萍, 杨源瑞, 林秀, 等. 血浆BNP和D-二聚体与老年脑梗死患者神经功能缺损评分及预后的关系[J]. 西部医学, 2023, 35(6): 858-862.
[18] 朱来运, 刘静, 肖成华. 全身免疫炎症指数及D-二聚体与青年急性脑梗死患者的病情严重程度及预后的关系[J]. 神经疾病与精神卫生, 2022, 22(5): 363-368.
[19] 王联军, 李世芳. 房颤, 血清CysC, Hcy水平对rt-PA静脉溶栓治疗急性脑梗死患者预后结局的影响[J]. 临床医学研究与实践, 2022, 7(4): 17-20.
[20] 夏瑜, 康艳飞, 曹敬然, 等. RDW联合血清CRP、PCT、sTLT-1与急性脑梗死患者脑梗死体积、神经功能受损程度和预后的关系研究[J]. 现代生物医学进展, 2022, 22(12): 2356-2360.
[21] 杨晓丽, 邵祥忠, 黄晓勇. 血清Lp-PLA2、pro-BNP、NSE及CRP水平与行急诊静脉溶栓治疗脑梗死患者预后关系[J]. 湖南师范大学学报(医学版), 2021, 18(6): 157-161.
[22] 李茂新, 乐灵丹, 赵宏宇. 中性粒细胞与淋巴细胞比值和血小板与淋巴细胞比值对急性脑梗死患者预后的预测价值研究[J]. 中国实用内科杂志, 2021, 8(2): 25-28.
[23] 阿加尔·木合大, 玛依拉·吐尔逊, 罗东辉. 中性粒细胞与淋巴细胞比值和血小板与淋巴细胞比值对急性脑梗死患者预后的预测价值研究[J]. 临床和实验医学杂志, 2023, 22(1): 12-15.
-




 下载:
下载: