The predictive value of RDW combined with plasma albumin and blood amylase ratio for infection in acute pancreatitis patients
-
摘要: 目的 探究红细胞分布宽度(red blood cell distribution width,RDW)联合血浆白蛋白和血淀粉酶比值对急性胰腺炎(acute pancreatitis,AP)患者合并感染的预测价值。 方法 选取2020年1月—2023年1月新疆维吾尔自治区人民医院诊治的130例AP患者进行回顾性研究,根据感染发生情况分为感染组(35例)和非感染组(95例)。收集入组患者的一般资料、RDW、血浆白蛋白及血淀粉酶比值等临床信息并进行组间分析比较,分别绘制RDW、血浆白蛋白、血淀粉酶比值及联合指标的受试者工作曲线,完成各指标的预测价值评估。 结果 两组基线资料均衡可比;相较于非感染组,感染组患者RDW和血淀粉酶比值显著升高,而血浆白蛋白水平显著降低,差异有统计学意义(P<0.05)。联合指标预测AP合并感染的预测价值高于RDW、血淀粉酶比和血浆白蛋白单独作为预测指标的价值。 结论 RDW显著升高、血浆白蛋白显著降低和血淀粉酶比值≥0.3可作为预测AP患者合并感染的重要指标,且三项指标联合可提高预测价值,具有较好的临床应用前景。Abstract: Objective To investigate the predictive value of red blood cell distribution width(RDW) combined with the ratio of plasma albumin to serum amylase for infection in acute pancreatitis(AP) patients. Methods A retrospective study was conducted on 130 AP patients who were diagnosed and treated in our hospital from January 2020 to January 2023. The patients were divided into infection group(n=35) and non-infection group(n=95) according to the presence or absence of infection. The general data, RDW, plasma albumin and serum amylase ratio of the enrolled patients were collected and compared between the two groups. The receiver operating characteristic(ROC) curves of RDW, plasma albumin, serum amylase ratio and combined indexes were made respectively, and the predictive value of each index was evaluated. Results The baseline data of the two groups were balanced and comparable. Compared with that of the non-infection group, the ratio of RDW and blood amylase in the infection group was significantly increased, while the plasma albumin level was significantly decreased(P < 0.05). The predictive value of the combined index in predicting AP infection was higher than that of RDW, serum amylase ratio, and plasma albumin alone. Conclusion A significant increase in RDW, a significant decrease in plasma albumin, and serum amylase ratio greater than or equal to 0.3 can be used as important indicators to predict infection in AP patients. The combination of the three indicators can improve the predictive value and has a good clinical application prospect.
-
Key words:
- red blood cell distribution width /
- albumin /
- blood amylase /
- acute pancreatitis /
- infection
-

-
表 1 两组患者基线资料比较
项目 感染组(35例) 非感染组(95例) 统计量 P 年龄/岁 45.84±8.74 46.03±11.09 0.040 0.968 性别/例(%) 0.977 0.322 男 20(57.1) 45(47.4) 女 15(42.9) 50(52.6) BMI/(kg/m2) 24.60±2.22 24.57±2.20 0.573 0.568 高血压/例(%) 1.882 0.170 是 11(31.4) 19(20.0) 否 24(68.6) 76(80.0) 糖尿病/例(%) 0.195 0.659 是 14(40.0) 34(35.8) 否 21(60.0) 61(64.2) 高血脂/例(%) 1.813 0.178 是 19(54.3) 39(41.1) 否 16(45.7) 56(58.9) 饮酒史/例(%) 0.112 0.738 是 11(31.4) 27(28.4) 否 24(68.6) 68(71.6) 吸烟史/例(%) 0.195 0.659 是 10(28.6) 31(32.6) 否 25(71.4) 64(67.4) 病因/例(%) 0.835 0.361 胆源性 16(45.7) 52(54.7) 非胆源性 19(54.3) 43(45.3) 胰腺外伤史/例(%) 0.188 0.665 是 9(25.7) 21(22.1) 否 26(74.3) 74(77.9) Ranson评分/分 3.63±1.25 2.99±1.17 1.376 0.171 Marshall评分/分 1.84±1.08 1.66±0.59 1.295 0.198 MCTSI评分/分 5.95±1.38 5.71±1.53 1.096 0.275 表 2 两组患者研究指标比较
项目 感染组(35例) 非感染组(95例) 统计量 P RDW 13.58±0.49 13.1±0.32 4.537 <0.001 血浆白蛋白/(g/L) 26.85±4.02 30.17±3.70 3.243 0.002 血淀粉酶比值≥0.3/例(%) 13.540 <0.001 是 24(68.6) 31(32.6) 否 11(31.4) 64(67.4) 表 3 独立和联合研究指标的预测价值
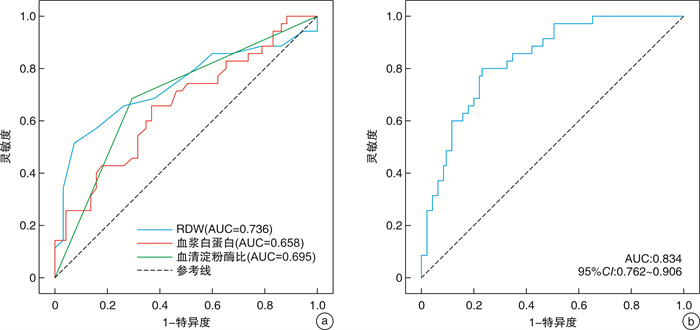
预测指标 AUC cut-off值 灵敏度 特异度 RDW 0.736 13.55 0.514 0.926 血浆白蛋白/(g/L) 0.658 29.15 0.657 0.632 血淀粉酶比值≥0.3 0.695 - 0.686 0.705 联合指标 0.834 - 0.800 0.768 -
[1] Hong W, Lillemoe KD, Pan S, et al. Development and validation of a risk prediction score for severe acute pancreatitis[J]. J Transl Med, 2019, 17(1): 146. doi: 10.1186/s12967-019-1903-6
[2] 刘丹希, 孙备. 重症急性胰腺炎治疗的热点问题[J]. 临床外科杂志, 2022, 30(7): 617-620. doi: 10.3969/j.issn.1005-6483.2022.07.005
[3] 中华医学会外科学分会胰腺外科学组. 中国急性胰腺炎诊治指南(2021)[J]. 浙江实用医学, 2021, 26(6): 511-519. https://www.cnki.com.cn/Article/CJFDTOTAL-ZJSA202106021.htm
[4] 魏方明. 急性胰腺炎患者NLR、IL-8的表达及其与感染性胰腺坏死发生的关系分析[J]. 中国现代药物应用, 2023, 17(1): 43-46. https://www.cnki.com.cn/Article/CJFDTOTAL-ZWYY202317008.htm
[5] 王文梅, 张景丽, 张海蓉. 红细胞体积分布宽度与急性胰腺炎相关性研究新进展[J]. 中国全科医学, 2020, 23(8): 998-1002. https://www.cnki.com.cn/Article/CJFDTOTAL-QKYX202008022.htm
[6] 邓弘扬, 魏丰贤, 张宇浩, 等. 新型血清学指标早期预测急性胰腺炎严重程度及预后的研究进展[J]. 中国免疫学杂志, 2021, 37(10): 1274-1278. doi: 10.3969/j.issn.1000-484X.2021.10.025
[7] 李响. RDW/SC联合Apo-A1对急性胰腺炎发生感染性胰腺坏死的预测研究[D]. 西南医科大学, 2023.
[8] Wiese ML, Urban S, von Rheinbaben S, et al. Identification of early predictors for infected necrosis in acute pancreatitis[J]. BMC Gastroenterol, 2022, 22(1): 405. doi: 10.1186/s12876-022-02490-9
[9] Feng A, Ao X, Zhou N, et al. A Novel Risk-Prediction Scoring System for Sepsis among Patients with Acute Pancreatitis: A Retrospective Analysis of a Large Clinical Database[J]. Int J Clin Pract, 2022, 2022: 5435656.
[10] Hong W, Zheng L, Lu Y, et al. Non-linear correlation between amylase day 2 to day 1 ratio and incidence of severe acute pancreatitis[J]. Front Cell Infect Microbiol, 2022, 12: 910760. doi: 10.3389/fcimb.2022.910760
[11] 王锐, 韩秋菊, 敬慧丹. 重症急性胰腺炎合并腹腔感染的病原菌特点与治疗分析[J]. 临床急诊杂志, 2022, 23(1): 51-54. https://lcjz.whuhzzs.com/article/doi/10.13201/j.issn.1009-5918.2022.01.012
[12] Lv J, Li J, Ren X, et al. Differentiation between Thalassemia Trait and Iron Deficiency Anemia Based on Low Hemoglobin Density and Microcytic Anemia Factor[J]. Clin Lab, 2023, 69(10): 418.
[13] Masoumi M, Shadmanfar S, Davatchi F, et al. Correlation of clinical signs and symptoms of Behcet's disease with mean platelet volume(MPV)and red cell distribution width(RDW)[J]. Orphanet J Rare Dis, 2020, 15(1): 297. doi: 10.1186/s13023-020-01588-1
[14] Ainiwaer A, Kadier K, Abulizi A, et al. Association of red cell distribution width(RDW)and the RDW to platelet count ratio with cardiovascular disease among US adults: a cross-sectional study based on the National Health and Nutrition Examination Survey 1999-2020[J]. BMJ Open, 2023, 13(3): e68148.
[15] Liang L, Huang L, Zhao X, et al. Prognostic value of RDW alone and in combination with NT-proBNP in patients with heart failure[J]. Clin Cardiol, 2022, 45(7): 802-813. doi: 10.1002/clc.23850
[16] Han YQ, Yan L, Zhang L, et al. Red blood cell distribution width provides additional prognostic value beyond severity scores in adult critical illness[J]. Clin Chim Acta, 2019, 498: 62-67. doi: 10.1016/j.cca.2019.08.008
[17] Wu H, Liao B, Cao T, et al. Diagnostic value of RDW for the prediction of mortality in adult sepsis patients: A systematic review and meta-analysis[J]. Front Immunol, 2022, 13: 997853. doi: 10.3389/fimmu.2022.997853
[18] Wu J, Zhang X, Liu H, et al. RDW, NLR and RLR in predicting liver failure and prognosis in patients with hepatitis E virus infection[J]. Clin Biochem, 2019, 63: 24-31. doi: 10.1016/j.clinbiochem.2018.11.012
[19] Nan W, Li S, Wan J, et al. Association of mean RDW values and changes in RDW with in-hospital mortality in ventilator-associated pneumonia(VAP): Evidence from MIMIC-IV database[J]. Int J Lab Hematol, 2024, 46(1): 99-106. doi: 10.1111/ijlh.14192
[20] Deniz M, Ozgun P, Ozdemir E. Relationships between RDW, NLR, CAR, and APACHE Ⅱ scores in the context of predicting the prognosis and mortality in ICU patients[J]. Eur Rev Med Pharmacol Sci, 2022, 26(12): 4258-4267.
[21] Mahnashi MH, Jabbar Z, Alamgeer, et al. Venlafaxine demonstrated anti-arthritic activity possibly through down regulation of TNF-alpha, IL-6, IL-1beta, and COX-2[J]. Inflammopharmacology, 2021, 29(5): 1413-1425. doi: 10.1007/s10787-021-00849-0
[22] Li D, Yang A, Xia M, et al. Association between red blood cell distribution width-to-albumin ratio and the prognosis in patients with autoimmune encephalitis: a retrospective cohort study[J]. Front Neurol, 2023, 14: 1276026.
[23] Li F, Ye Z, Zhu J, et al. Early Lactate/Albumin and Procalcitonin/Albumin Ratios as Predictors of 28-Day Mortality in ICU-Admitted Sepsis Patients: A Retrospective Cohort Study[J]. Med Sci Monit, 2023, 29: e940654.
[24] Li B, Wu W, Liu A, et al. Establishment and Validation of a Nomogram Prediction Model for the Severe Acute Pancreatitis[J]. J Inflamm Res, 2023, 16: 2831-2843.
[25] Tenner S, Baillie J, DeWitt J, et al. American College of Gastroenterology guideline: management of acute pancreatitis[J]. Am J Gastroenterol, 2013, 108(9): 1400-1415, 1416.
[26] Kumaravel A, Stevens T, Papachristou G I, et al. A Model to Predict the Severity of Acute Pancreatitis Based on Serum Level of Amylase and Body Mass Index[J]. Clin Gastroenterol Hepatol, 2015, 13(8): 1496-1501.
[27] Zheng L, Hong W, Geng W, et al. A comparison of the BISAP score and Amylase and BMI(CAB)score versus for predicting severe acute pancreatitis[J]. Acta Gastroenterol Belg, 2019, 82(3): 397-400.
[28] 郭喆, 关键. 重症急性胰腺炎预防与阻断急诊专家共识[J]. 临床急诊杂志, 2022, 23(7): 451-462. https://lcjz.whuhzzs.com/article/doi/10.13201/j.issn.1009-5918.2022.07.001
-

计量
- 文章访问数: 39
- 施引文献: 0



 下载:
下载: