Correlation analysis between Padua score, serum vWF, IMA levels and the occurrence of venous thromboembolism in patients with septic shock
-
摘要: 目的 探究Padua评分、血清血管性假血友病因子(von willebrand factor,vWF)、缺血修饰白蛋白(ischemia modified albumin,IMA)水平与脓毒性休克患者发生静脉血栓栓塞症(venous thromboembolism,VTE)的关系。 方法 选取汉中市三二〇一医院2015年3月—2023年8月收治的脓毒性休克患者377例,根据住院期间VTE发生情况,将其分为VTE组(发生VTE者,68例)和非VTE组(未发生VTE者,309例)。收集患者临床资料并进行Padua评分,检测血清vWF、IMA水平,分析脓毒性休克患者Padua评分、血清vWF、IMA水平的相关性,分析Padua评分、血清vWF、IMA水平预测脓毒性休克患者发生VTE的价值及影响发生VTE的因素。 结果 VTE组患者急性生理学与慢性健康状况评分Ⅱ(acute physiology and chronic health evaluation,APACHE Ⅱ)评分、序贯器官衰竭评分、D-二聚体、Padua评分、血清vWF、IMA水平明显高于非VTE组,差异有统计学意义(P<0.05);脓毒性休克患者Padua评分与血清vWF、IMA水平均呈正相关(P<0.05),血清vWF与IMA水平呈正相关(P<0.05);Padua评分、血清vWF、IMA、三者联合预测脓毒性休克患者发生VTE的曲线下面积(AUC)分别为0.879、0.776、0.756、0.954,三者联合预测的AUC高于Padua评分、血清vWF、IMA各自单独预测的AUC(P<0.05);APACHE Ⅱ评分高、D-二聚体水平高、Padua评分高、vWF水平高、IMA水平高均是影响脓毒性休克患者发生VTE的独立危险因素(P<0.05)。 结论 脓毒性休克并发VTE患者Padua评分、血清vWF、IMA水平均呈高表达,三者联合对脓毒性休克患者发生VTE的预测效能较高,均是影响VTE发生的独立危险因素。Abstract: Objective To explore the relationship between Padua score, serum von willebrand factor(vWF), ischemia modified albumin(IMA) level and the occurrence of venous thromboembolism(VTE) in patients with septic shock. Methods A total of 377 patients with septic shock admitted to Hanzhong 3201 Hospital from March 2015 to August 2023 were selected, according to the occurrence of VTE during hospitalization, they were divided into VTE group(68 patients with VTE) and non-VTE group(309 patients with no VTE). Clinical data of patients were collected and Padua score was performed. Serum vWF and IMA levels were detected. Analyze the correlation of Padua score, serum vWF and IMA level in patients with septic shock, the value of Padua score, serum vWF and IMA level in predicting the occurrence of VTE in patients with septic shock and the factors affecting the occurrence of VTE. Results APACHEⅡ, SOFA score, D-dimer, Padua score, serum vWF and IMA levels in VTE group were significantly higher than those in non-VTE group(P < 0.05). In septic shock patients, Padua score was positively correlated with serum vWF and IMA levels(P < 0.05), and serum vWF was positively correlated with IMA levels(P < 0.05). The area under curve(AUC) of Padua score, serum vWF, IMA and the combined prediction of VTE in septic shock patients were 0.879, 0.776, 0.756 and 0.954, respectively, the AUC predicted by the combination of the three methods was higher than that predicted by Padua score, serum vWF and IMA alone(P < 0.05). High APACHEⅡ score, D-dimer level, Padua score, vWF level and IMA level were independent risk factors for the occurrence of VTE in septic shock patients(P < 0.05). Conclusion The Padua score, serum vWF and IMA levels of patients with septic shock complicated with VTE were highly expressed, and the combination of the three factors had a high predictive effect on the occurrence of VTE in patients with septic shock, which were independent risk factors affecting the occurrence of VTE.
-
Key words:
- septic shock /
- venous thromboembolism /
- Padua score /
- von willebrand factor /
- ischemia modified albumin
-

-
表 1 VTE组和非VTE组患者临床资料比较
X±S 指标 非VTE组(309例) VTE组(68例) χ2/t P 性别/例 1.538 0.215 男 171 32 女 138 36 年龄/岁 58.12±14.95 61.40±16.07 1.616 0.107 BMI(kg/m2) 21.83±3.16 22.09±3.04 0.618 0.537 吸烟史/例(%) 70(22.65) 19(27.94) 0.864 0.353 糖尿病史/例(%) 47(15.21) 16(23.53) 2.771 0.096 ICU住院时间/d 10.14±3.29 9.35±3.02 1.818 0.070 APACHE Ⅱ评分/分 18.86±4.94 23.19±5.87 6.315 <0.001 SOFA评分/分 9.72±2.55 14.38±3.69 12.478 <0.001 血小板计数/(×109/L) 237.01±74.28 254.93±80.87 1.772 0.077 D-二聚体/(mg/L) 5.13±1.39 6.42±1.85 6.495 <0.001 表 2 VTE组和非VTE组患者Padua评分及血清vWF、IMA水平比较
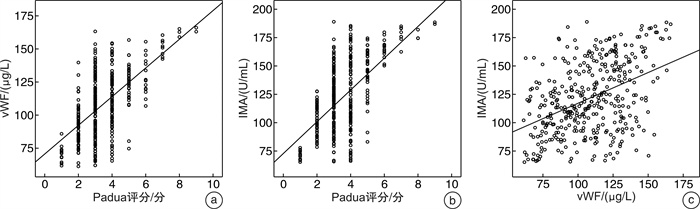
X±S 组别 例数 Padua评分/分 vWF/(μg/L) IMA/(U/mL) 非VTE组 309 3.10±0.98 92.34±26.92 97.55±30.94 VTE组 68 5.26±1.50 128.67±35.30 141.21±43.68 t 14.777 9.484 9.709 P <0.001 <0.001 <0.001 表 3 Padua评分、血清vWF、IMA水平对脓毒性休克患者发生VTE的预测价值
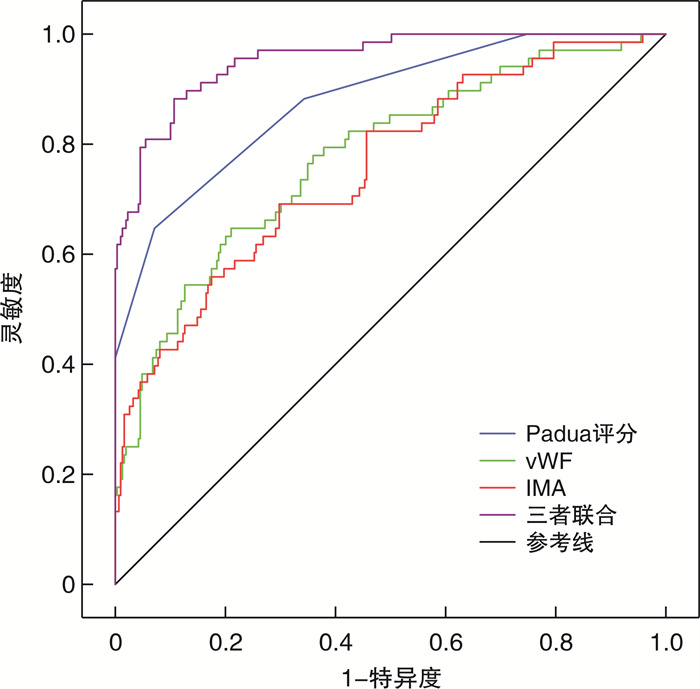
指标 AUC 95%CI 截断值 灵敏度/% 特异度/% Padua评分 0.879 0.832~0.925 4.52分 64.71 92.93 vWF 0.776 0.712~0.840 115.68 μg/L 61.58 81.86 IMA 0.756 0.691~0.822 109.84 U/mL 62.14 73.62 三者联合 0.954 0.930~0.979 - 97.25 72.38 表 4 影响脓毒性休克患者发生VTE的多因素分析
因素 β SE Wald P OR 95%CI APACHE Ⅱ评分 0.599 0.239 6.290 0.012 1.821 1.140~2.909 SOFA评分 0.305 0.172 3.135 0.077 1.356 0.968~1.900 D-二聚体 0.665 0.248 7.185 0.007 1.944 1.196~3.161 Padua评分 1.172 0.315 13.833 <0.001 3.227 1.740~5.983 vWF 1.061 0.263 16.283 <0.001 2.890 1.726~4.839 IMA 0.947 0.291 10.591 0.001 2.578 1.457~4.560 -
[1] Foster DM, Kellum JA. Endotoxic Septic Shock: Diagnosis and Treatment[J]. Int J Mol Sci, 2023, 24(22): 16185-16196. doi: 10.3390/ijms242216185
[2] Yamashita Y, Morimoto T, Kimura T. Venous thromboembolism: Recent advancement and future perspective[J]. J Cardiol, 2022, 79(1): 79-89. doi: 10.1016/j.jjcc.2021.08.026
[3] Tran A, Fernando SM, Rochwerg B, et al. Prognostic factors associated with development of venous thromboembolism in critically ill patients-a systematic review and meta-analysis[J]. Crit Care Med, 2022, 50(4): 370-381. doi: 10.1097/CCM.0000000000005382
[4] Arakaki D, Iwata M, Terasawa T. External Validation of the Padua and IMPROVE-VTE Risk Assessment Models for Predicting Venous Thromboembolism in Hospitalized Adult Medical Patients: A Retrospective Single-Center Study in Japan[J]. Ann Vasc Dis, 2023, 16(1): 60-68. doi: 10.3400/avd.oa.22-00108
[5] 李继萍, 乜庆荣, 韩雪峰, 等. Padua评分对呼吸科住院患者静脉血栓栓塞症的评估价值[J]. 心肺血管病杂志, 2022, 41(9): 979-983. https://www.cnki.com.cn/Article/CJFDTOTAL-XFXZ202209006.htm
[6] 吴畏, 张建涛, 吴海生. P选择素、溶血磷脂酸、血管性假血友病因子对腹部创伤患者下肢深静脉血栓形成的预测价值[J]. 华南国防医学杂志, 2021, 35(10): 725-727, 758.
[7] 王耀, 郭筱王. 脓毒症患者血清心肌肌钙蛋白Ⅰ及缺血修饰白蛋白的变化及临床意义[J]. 临床急诊杂志, 2021, 22(7): 478-481. https://lcjz.whuhzzs.com/article/doi/10.13201/j.issn.1009-5918.2021.07.008
[8] 高戈, 冯喆, 常志刚, 等. 2012国际严重脓毒症及脓毒性休克诊疗指南[J]. 中华危重病急救医学, 2013, 25(8): 501-505. https://cpfd.cnki.com.cn/Article/CPFDTOTAL-FJMZ201305005029.htm
[9] 张福先, 王深明. 静脉血栓栓塞症诊断与治疗[M]. 北京: 人民卫生出版社, 2013: 88-92.
[10] Lutsey PL, Zakai NA. Epidemiology and prevention of venous thromboembolism[J]. Nat Rev Cardiol, 2023, 20(4): 248-262. doi: 10.1038/s41569-022-00787-6
[11] Ghouse J, Tragante V, Ahlberg G, et al. Genome-wide meta-analysis identifies 93 risk loci and enables risk prediction equivalent to monogenic forms of venous thromboembolism[J]. Nat Genet, 2023, 55(3): 399-409. doi: 10.1038/s41588-022-01286-7
[12] Lavon O, Tamir T. Evaluation of the Padua Prediction Score ability to predict venous thromboembolism in Israeli non-surgical hospitalized patients using electronic medical records[J]. Sci Rep, 2022, 12(1): 6121-6127. doi: 10.1038/s41598-022-10209-9
[13] 彭清, 刘佳君, 尚华, 等. Padua量表在内科住院患者静脉血栓栓塞症中的应用研究进展[J]. 实用医院临床杂志, 2021, 18(2): 200-203.
[14] Klen J, Horvat G, Blinc A. Perioperative Prevention of Venous Thromboembolism in Abdominal Surgery Patients Based on the Caprini or the Padua Risk Score-A Single Centre Prospective Observational Study[J]. Life(Basel), 2022, 12(11): 1843-1853.
[15] Moss SR, Jenkins AM, Caldwell AK, et al. Risk Factors for the development of hospital-associated venous thromboembolism in adult patients admitted to a Children's Hospital[J]. Hosp Pediatr, 2020, 10(2): 166-172. doi: 10.1542/hpeds.2019-0052
[16] 高伟飞, 李鹏, 乔镇, 等. Padua评分对老年住院病人发生静脉血栓栓塞症的预测价值[J]. 实用老年医学, 2023, 37(8): 803-805, 810. https://www.cnki.com.cn/Article/CJFDTOTAL-SYLA202308012.htm
[17] Zhou C, Guang Y, Luo Y, et al. Superior Predictive Value of D-Dimer to the Padua Prediction Score for Venous Thromboembolism in Inpatients with AECOPD: A Multicenter Cohort Study[J]. Int J Chron Obstruct Pulmon Dis, 2022, 17(1): 2711-2722.
[18] 陈艳青, 黄潇, 孔桂青, 等. HMGB1和vWF等细胞因子对脓毒症患者病情严重程度及预后评估的意义[J]. 中华危重病急救医学, 2020, 32(8): 933-937.
[19] Shin H, Kim JG, Jang BH, et al. Diagnostic Accuracy of Ischemia-Modified Albumin for Acute Coronary Syndrome: A Systematic Review and Meta-Analysis[J]. Medicina(Kaunas), 2022, 58(5): 614.
[20] Choo SH, Lim YS, Cho JS, et al. Usefulness of ischemia-modified albumin in the diagnosis of sepsis/septic shock in the emergency department[J]. Clin Exp Emerg Med, 2020, 7(3): 161-169. doi: 10.15441/ceem.19.075
[21] 王兆娜, 安雪丽, 刘利叶, 等. 外周血血管紧张素Ⅱ、缺血修饰白蛋白及C反应蛋白对静脉血栓栓塞症的预测价值[J]. 中国动脉硬化杂志, 2022, 30(8): 705-708. https://www.cnki.com.cn/Article/CJFDTOTAL-KDYZ202208009.htm
-




 下载:
下载: