Establishment and application of a novel assessment system for prognosis of elderly patients with upper gastrointestinal perforation
-
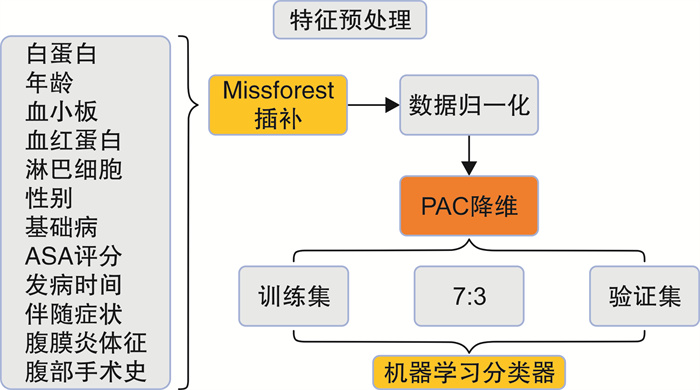
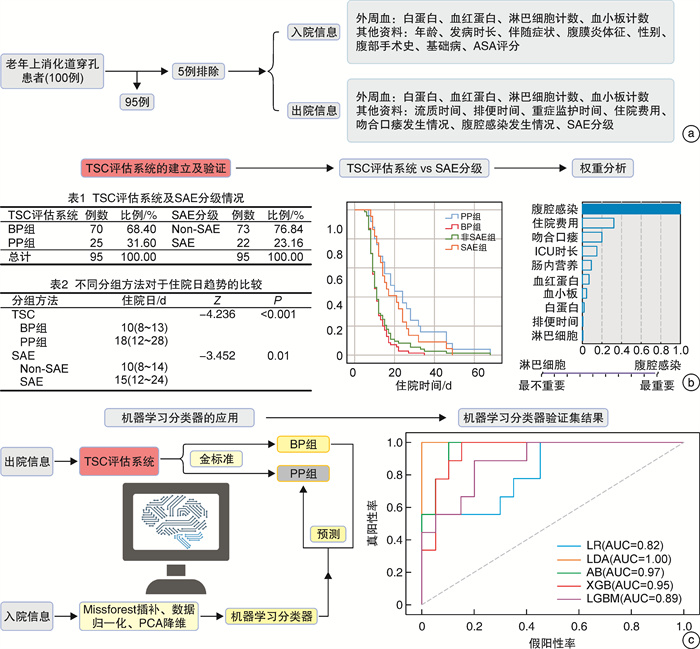
摘要: 目的 构建老年上消化道穿孔患者预后的新型评估系统及应用机器学习分类器,有助于入院快速预测老年上消化道穿孔患者的预后。 方法 回顾性收集在2017年6月—2023年7月收住福建医科大学附属协和医院急诊外科诊断为老年上消化道穿孔的95例患者。收集患者的临床资料和实验室检查资料,并对患者的术后严重并发症进行分级。采用二阶聚类分组(TWO-STEP cluster grouping,TSC)对其预后进行自动分组,分为预后良好组(GP组,70例)和预后不良组(PP组,25例)。利用机器学习分类器综合入院多因素对老年上消化道穿孔患者的预后进行预测,并采用受试者工作特征(ROC)曲线分析其预测效果。 结果 PP组患者术后胃肠道恢复时间、重症监护时间及住院费用均明显高于GP组;对比TSC评估系统和术后严重并发症(severe adverse events,SAE)分级对住院日的区分度,发现TSC评估系统相较于SAE分级有更好的区分度(TSC:P<0.001,SAE:P=0.01)。进一步对比两组患者的入院情况,发现PP组年龄明显高于GP组[77.00(71.50~82.50)岁vs 72.00(67.00~78.00)岁,P=0.043],其术前外周血白蛋白的水平明显低于GP组。对比不同机器学习分类器对TSC评估系统的预测效能,发现自适应增强分类器的预测效能最优,其曲线下面积(AUC)为0.97(95%CI:0.52~1.00,精确度为0.86)。 结论 TSC评估系统能有效针对老年上消化道穿孔患者的预后进行评估。超高龄和低白蛋白血症是上消化道穿孔患者预后不良的独立危险因素。自适应增强分类器有助于入院快速预测老年上消化道穿孔患者的预后,协助临床诊疗。Abstract: Objective To construct a novel assessment system for the prognosis of elderly patients with upper gastrointestinal perforation and the application of machine learning classifiers, for admission to quickly predict the prognosis of elderly patients with upper gastrointestinal perforation. Methods A total of 95 patients admitted to the Department of Emergency Surgery of Union Hospital of Fujian Medical University from June 2017 to July 2023 with a diagnosis of upper gastrointestinal perforation in the elderly were retrospectively collected. The clinical data and laboratory examination data of the patients were collected, and the postoperative serious complications of the patients were graded. Their prognosis was automatically grouped into good prognosis group(GP group, 70 cases) and poor prognosis group(PP group, 25 cases) using TWO-STEP cluster grouping(TSC). The prognosis of elderly patients with upper gastrointestinal perforation was predicted by integrating admission multifactors using machine learning classifiers, and the predictive effect was analysed by using the subject's work characteristics(ROC) curve. Results The postoperative gastrointestinal recovery time, intensive care time, and hospitalisation cost of the patients in the PP group were significantly higher than those in the GP group. Comparing the differentiation of hospitalisation days between the TSC assessment system and the severe adverse events(SAE) classification, it was found that: the TSC assessment system had a better differentiation compared with the SAE classification(TSC: P < 0.001, SAE: P=0.01). Further comparing the admission status of the two groups, it was found that: the PP group was significantly older than the GP group(77.00[71.50-82.50] vs 72.00[67.00-78.00], P=0.043), and its preoperative peripheral blood albumin level was significantly lower than that of the GP group. Comparing the predictive efficacy of different machine learning classifiers for the TSC assessment system, it was found that: the adaptive boosting classifier(AB) had the best predictive efficacy, with an area under the curve(AUC) of 0.97(95%CI: 0.52-1.00, precision 0.86). Conclusion The TSC assessment system is effective in targeting the prognosis of elderly patients with upper gastrointestinal perforation. Advanced age and hypoalbuminaemia were independent risk factors for poor prognosis in patients with upper gastrointestinal perforation. The AB helps to rapidly predict the prognosis of elderly patients with upper gastrointestinal perforation on admission and assists in clinical management.
-

-
表 1 不同分组方法对于住院日趋势的比较
分组 住院日/d Z P TSC BP组 10(8~13) -4.236 <0.001 PP组 18(12~28) SAE Non-SAE组 10(8~14) -3.452 0.01 SAE组 15(12~24) 表 2 TSC评估系统组成因素的组间对比及分组权重占比
组别 BP组(70例) PP组(25例) F/Z P 权重 血红蛋白/(g/L) 106.64±20.35 97.36±16.90 3.564 0.044 0.07 白蛋白/(g/L) 33.56±4.19 34.36±4.69 0.320 0.431 0.02 淋巴细胞计数/(×109/L) 1.16±0.40 1.20±0.63 1.447 0.746 0.01 血小板计数/(×109/L) 274.01±122.99 318.96±147.57 1.034 0.141 0.04 流质时间/d 6.16±2.23 7.68±3.63 7.987 0.016 0.09 排便时间/d 4.81±2.26 4.64±1.68 1.204 0.726 0.01 重症监护时长/h 24.50±59.20 114.90±204.25 30.503 0.001 0.15 住院费用/元 41 157.30±25 062.37 96 702.64±76 317.95 33.623 <0.001 0.32 吻合口瘘/例(%) -3.824 0 0.20 0 70(100.00) 20(80.00) 1 0 5(20.00) 腹腔感染/例(%) -9.169 0 1.00 0 70(100.00) 2(8.00) 1 0 23(92.00) 表 3 不同机器学习分类器对于TSC评估系统分组的预测效能比较
分类器 准确度 AUC(95%Cl) 精确度 召回率 F1值 LDA 1.00 1.00(0.50~1.00) 1.00 1.00 1.00 LR 0.76 0.82(0.48~0.83) 0.76 0.76 0.73 AB 0.86 0.97(0.52~1.00) 0.89 0.86 0.85 XGB 0.79 0.95(0.51~1.00) 0.84 0.79 0.75 LGBM 0.79 0.89(0.51~1.00) 0.79 0.79 0.77 注:以上各类项目的取值范围是0~1,越接近1则表示效果越强。 表 4 TSC评估系统的分组组间术前资料对比
组别 BP组(70例) PP组(25例) F P 白蛋白/(g/L) 36.43±6.21 33.33±4.77 1.442 0.026 年龄/岁 72.00(67.00~78.00) 77(71.50~82.50) -2.019 0.043 发病时间/h 20.50(10.00~24.00) 24.00(20.00~24.00) -1.480 0.139 血红蛋白/(g/L) 135.00(110.75-148.25) 130.00(112.50-139.50) -0.790 0.429 淋巴细胞计数/(×109/L) 0.57(0.40~0.76) 0.51(0.35~0.67) -0.774 0.439 血小板计数/(×109/L) 227.50(185.25~270.00) 254.00(181.50~366.00) -1.331 0.183 伴随症状/例(%) -0.321 0.748 无 20(28.57) 8(32.00) 有 50(71.43) 17(68.00) 腹膜炎体征/例(%) -0.318 0.751 无 22(31.43) 7(28.00) 有 48(68.57) 18(72.00) 性别/例(%) -0.318 0.751 男 48(68.57) 18(72.00) 女 22(31.43) 7(28.00) 腹部手术史/例(%) -1.801 0.072 无 55(78.57) 15(60.00) 有 15(21.43) 10(40.00) 基础病/例(%) -0.116 0.908 无 16(22.86) 6(24.00) 有 54(77.14) 19(76.00) ASA评分/例(%) -0.984 0.325 1分 1(1.43) 0 2分 28(40.00) 8(32.00) 3分 32(45.71) 12(48.00) 4分 5(7.14) 4(16.00) 5分 4(5.71) 1(4.00) -
[1] 吴乾龙, 龙志祥, 朱共元. 加速康复外科理念在老年患者急诊上消化道穿孔修补术中的应用[J]. 中国当代医药, 2021, 28(1): 72-74, 83. https://www.cnki.com.cn/Article/CJFDTOTAL-ZGUD202121019.htm
[2] 唐咸军, 范启腾, 辛恩平. 传统开腹修补术与腹腔镜修补术治疗老年上消化道穿孔的临床效果分析[J]. 临床医学工程, 2021, 28(6): 709-710. https://www.cnki.com.cn/Article/CJFDTOTAL-YBQJ202106003.htm
[3] 杨立民, 魁国菊. HALP与结肠癌临床病理特征的相关性及其对术后肝转移的预测价值[J]. 中国普外基础与临床杂志, 2023, 30(8): 958-963. https://www.cnki.com.cn/Article/CJFDTOTAL-ZPWL202308010.htm
[4] Xu H, Zheng X, Ai J, et al. Hemoglobin, albumin, lymphocyte, and platelet(HALP)score and cancer prognosis: A systematic review and meta-analysis of 13, 110 patients[J]. Int Immunopharmacol, 2023, 114: 109496. doi: 10.1016/j.intimp.2022.109496
[5] Farag CM, Antar R, Akosman S, et al. What is hemoglobin, albumin, lymphocyte, platelet(HALP)score? A comprehensive literature review of HALP's prognostic ability in different cancer types[J]. Oncotarget, 2023, 14: 153-172. doi: 10.18632/oncotarget.28367
[6] 袁梦依, 王培山, 孟瑞霞, 等. 术前HALP评分对老年非小细胞肺癌手术病人预后的预测价值[J]. 实用老年医学, 2022, 36(12): 1259-1263. https://www.cnki.com.cn/Article/CJFDTOTAL-SYLA202212018.htm
[7] 陈伟克, 肖荣耀, 蔡皎皓, 等. 胃癌根治术后吻合口瘘的危险因素及术前NRS2002评分的预测价值[J]. 浙江医学, 2019, 41(4): 345-347. https://www.cnki.com.cn/Article/CJFDTOTAL-ZJYE201904013.htm
[8] 吴秀文, 任建安. 中国腹腔感染诊治指南(2019版)[J]. 中国实用外科杂志, 2020, 40(1): 1-16. https://www.cnki.com.cn/Article/CJFDTOTAL-ZGWK202001001.htm
[9] Clavien PA, Barkun J, de Oliveira ML, et al. The Clavien-Dindo classification of surgical complications: five-year experience[J]. Ann Surg, 2009, 250(2): 187-196. doi: 10.1097/SLA.0b013e3181b13ca2
[10] Bhandoria G, Mane JD. Can Surgical Apgar Score(SAS)Predict Postoperative Complications in Patients Undergoing Gynecologic Oncological Surgery?[J]. Indian J Surg Oncol, 2020, 11(1): 60-65. doi: 10.1007/s13193-019-00995-6
[11] Wang H, Zhang JR, Chen S, et al. Who would avoid severe adverse events from nasointestinal tube in small bowel obstruction? A matched case-control study[J]. BMC Gastroenterol, 2022, 22(1): 332. doi: 10.1186/s12876-022-02405-8
[12] 李定云, 王婷, 张涛, 等. 上消化道穿孔患者死亡的危险因素分析[J]. 中国实用医药, 2020, 15(19): 34-36. https://www.cnki.com.cn/Article/CJFDTOTAL-ZSSA202019012.htm
[13] 姚正顺, 闫鸿, 甄博, 等. 老年上消化道穿孔患者行腹腔镜下修补术对血清炎性细胞因子、细胞免疫指标的影响[J]. 疑难病杂志, 2018, 17(4): 366-369, 373.
[14] 夏文岩. 探究微创腹腔镜与传统开腹修补术治疗老年上消化道穿孔术后的并发症及预后差异[J]. 中国医药指南, 2020, 18(1): 73-74. https://www.cnki.com.cn/Article/CJFDTOTAL-YYXK202020032.htm
[15] 骆平, 李军, 张翔, 等. 加速康复外科理念在老年患者上消化道穿孔修补术中的应用价值[J]. 安徽医学, 2018, 39(4): 480-482. https://www.cnki.com.cn/Article/CJFDTOTAL-AHYX201804031.htm
[16] 曹押宏. 老年胃穿孔患者手术治疗效果及影响因素分析[J]. 中国现代普通外科进展, 2017, 20(2): 124-125. https://www.cnki.com.cn/Article/CJFDTOTAL-PWJZ201702012.htm
[17] Voldby AW, Boolsen AW, Aaen AA, et al. Complications and Their Association with Mortality Following Emergency Gastrointestinal Surgery-an Observational Study[J]. J Gastrointest Surg, 2022, 26(9): 1930-1941. doi: 10.1007/s11605-021-05240-6
[18] 金卫, 张晓燕, 杜江, 等. 降钙素原和白介素-6在老年复杂性腹腔感染患者预后评估中的意义[J]. 老年医学与保健, 2017, 23(1): 9-11, 18.
[19] 梁树华. Logistic回归分析影响胃癌患者术后吻合口瘘发生的因素[J]. 中外医学研究, 2022, 20(3): 155-158.
[20] 王洪霞, 刘旭, 毕红英, 等. 不同部位急性胃肠道穿孔所致脓毒性休克的临床分析[J]. 中华危重病急救医学, 2020, 32(8): 943-946.
[21] 葛华, 何学彦, 黄永生. 老年上消化道穿孔术后早期肠内营养与肠外营养的临床效果比较[J]. 安徽医药, 2018, 22(12): 2379-2382. https://www.cnki.com.cn/Article/CJFDTOTAL-AHYY201812027.htm
[22] 李宝玲, 朱宏丽, 王统民, 等. 老年人贫血状况及病因分析[J]. 中华老年多器官疾病杂志, 2019, 18(3): 185-188. https://www.cnki.com.cn/Article/CJFDTOTAL-ZLQG201903005.htm
[23] Chen T, Zhang Y, Dou Q, et al. . Machine Learning-Assisted Preoperative Diagnosis of Infection Stones in Urolithiasis Patients[J]. J Endourol, 2022, 36(8): 1091-1098. doi: 10.1089/end.2021.0783
[24] Choudhury A. Predicting cancer using supervised machine learning: Mesothelioma[J]. Technol Health Care, 2021, 29(1): 45-58. doi: 10.3233/THC-202237
[25] Vlasák A, Gerla V, Skalicky P, et al. Boosting phase-contrast MRI performance in idiopathic normal pressure hydrocephalus diagnostics by means of machine learning approach[J]. Neurosurg Focus, 2022, 52(4): E6. doi: 10.3171/2022.1.FOCUS21733
[26] 朱小烽, 钟武, 姜启栋, 等. 不同年龄段成人消化道穿孔的临床特征研究[J]. 现代消化及介入诊疗, 2019, 24(12): 1423-1426. https://www.cnki.com.cn/Article/CJFDTOTAL-XDXH201912015.htm
[27] 戴盈, 秦少云, 潘华琴, 等. 急性生理评分与序贯器官衰竭评估评分预测高龄脓毒症患者预后的价值[J]. 实用临床医药杂志, 2019, 23(4): 37-40. https://www.cnki.com.cn/Article/CJFDTOTAL-XYZL201904011.htm
[28] 陈晟, 柴瑞, 屠世良, 等. 术前糖化血红蛋白水平与老年结直肠癌伴2型糖尿病患者术后吻合口瘘的相关性研究[J]. 中国卫生检验杂志, 2018, 28(21): 2632-2634, 2638.
[29] 孙天平. 高龄患者上消化道穿孔60例手术治疗分析[J]. 中外医疗, 2013, 32(8): 53-54.
[30] 刘启领, 陈建华. 124例老年胃、十二指肠急性穿孔临床分析[J]. 中国实用医药, 2007, 2(32): 75-76. https://www.cnki.com.cn/Article/CJFDTOTAL-ZSSA200728054.htm
[31] 芮云峰, 鲁攀攀, 李荥娟, 等. 老年股骨转子间骨折患者术后死亡危险因素分析[J]. 中国修复重建外科杂志, 2019, 33(12): 1538-1542. https://www.cnki.com.cn/Article/CJFDTOTAL-ZXCW201912014.htm
[32] 姜大同, 项和平, 李贺, 等. 老年肠梗阻患者急诊手术并发症的影响因素分析[J]. 安徽医学, 2017, 38(3): 306-308. https://www.cnki.com.cn/Article/CJFDTOTAL-AHYX201703013.htm
-




 下载:
下载: