Predictive study of changes in serum SIRT1 and Syndecan-1 levels in patients with severe acute pancreatitis complicated with acute kidney injury to condition and clinical outcome
-
摘要: 目的 研究重症急性胰腺炎(severe acute pancreatitis,SAP)合并急性肾损伤(acute kidney injury,AKI)患者血清沉默信息调节因子1(silent information regulator 1,SIRT1)、蛋白聚糖-1(Syndecan-1)水平变化对患者病情和临床转归的预测能力。方法 前瞻性选取2021年2月—2023年2月临沂市中心医院收治的130例SAP合并AKI患者,另选取同期于我院体检健康的70例健康志愿者。比较健康志愿者与不同AKI分期SAP患者血清SIRT1、Syndecan-1水平。SAP合并AKI患者均接受综合治疗,根据入院28 d临床转归结局将其分为死亡组和生存组,比较两组基线资料。多因素logistic回归模型分析影响SAP合并AKI患者死亡的危险因素。受试者工作特征(receiver operating characteristic curve,ROC)曲线分析血清SIRT1、Syndecan-1对SAP合并AKI患者死亡的预测价值。结果 SAP合并AKI患者血清Syndecan-1水平高于健康志愿者,血清SIRT1水平低于健康志愿者(P < 0.05),且随着AKI分期的增加,血清SIRT1水平降低(r=-0.624,P < 0.05)、Syndecan-1水平升高(r=0.498,P < 0.05)。SAP合并AKI患者入院28 d内死亡率约为24.62%(32/130);与生存组比较,死亡组急性生理与慢性健康(acute physiology and chronic health evaluation,APACHE Ⅱ)评分、连续肾脏替代疗法治疗比例、血肌酐、尿素氮、D-二聚体(D-Dimer,D-D)、肾损伤分子1(kidney injury molecule 1,KIM-1)、Syndecan-1水平升高,SIRT1水平降低,组间比较差异有统计学意义(P < 0.05)。多因素logistic回归分析结果显示:APACHE Ⅱ评分、血肌酐、D-D、KIM-1、Syndecan-1水平升高,SIRT1水平降低是影响SAP合并AKI患者死亡的危险因素(P < 0.05)。ROC曲线结果显示,血清SIRT1、Syndecan-1及其联合应用模型预测SAP合并AKI患者死亡的AUC(95%CI)分别为0.803(0.634~0.948)、0.827(0.702~0.929)、0.857(0.768~0.939)。结论 SAP患者AKI损伤越严重,其血清SIRT1水平越低、Syndecan-1水平越高,且血清SIRT1、Syndecan-1联合检测预测SAP合并AKI患者死亡的效能较高。Abstract: Objective To investigate the predictive ability of changes in serum silencing information regulator 1(SIRT1) and proteoglycan-1(Syndecan-1) levels in patients with severe acute pancreatitis(SAP) complicated with acute kidney injury(AKI) on the patients' condition and clinical regression.Methods A total of 130 patients with SAP combined with AKI admitted to Linyi Central Hospital from February 2021 to February 2023 were prospectively selected, and 70 healthy volunteers who underwent physical examination in our hospital during the same period were also selected. The serum SIRT1 and Syndecan-1 levels were compared between volunteers and patients with SAP with different AKI stages. All patients with SAP complicated with AKI received comprehensive treatment, and they were divided into death group and survival group according to the clinical outcome 28 d after admission, and the baseline data of the two groups were compared. Multivariate logistic regression model was used to analyze the risk factors of death in patients with SAP complicated with AKI. The predictive value of serum SIRT1 and Syndecan-1 for death in patients with SAP complicated with AKI was analyzed by receiver operating characteristic(ROC) curve.Results The serum Syndecan-1 level in patients with SAP complicated with AKI were higher than that of healthy volunteers, and the serum SIRT1 level were lower than that of healthy volunteers(P < 0.05), and with the increase of AKI stage, the serum SIRT1 levels were decreased(r=-0.624, P < 0.05) and the Syndecan-1 level were increased(r=0.498, P < 0.05). The mortality rate of patients with SAP complicated with AKI within 28 d after admission were 24.62%(32/130). Compared with survival group, acute physiology and chronic health evaluation(APACHE Ⅱ) score, proportion of continuous renal replacement therapy treatment, serum creatinine, urea nitrogen, D-dimer(D-D), kidney injury molecule 1(KIM-1) and Syndecan-1 levels in death group were increased, and SIRT1 levels were decreased, the differences between groups were statistically significant(P < 0.05). Multivariate logistic regression analysis showed that APACHE Ⅱ score, serum creatinine, D-D, KIM-1 and Syndecan-1 levels were increased, and SIRT1 level was decreased, which were risk factors for death in patients with SAP complicated with AKI(P < 0.05). The results of ROC curve showed that the AUC(95%CI) of serum SIRT1, Syndecan-1 and their combined application model to predict the death of patients with SAP complicated with AKI were 0.803(0.634-0.948), 0.827(0.702-0.929), 0.857(0.768-0.939).Conclusion The more severe AKI injury in patients with SAP, the lower the serum SIRT1 level, and the higher the Syndecan-1 level, and the combined detection of serum SIRT1 and Syndecan-1 is more effective in predicting the death of patients with SAP complicated with AKI.
-

-
表 1 健康志愿者和不同AKI分期SAP患者血清SIRT1、Syndecan-1水平比较
X±S 组别 例数 SIRT1/(pg/mL) Syndecan-1/(μg/mL) 健康志愿者 70 2 151.43±164.86 0.37±0.10 AKIⅠ期SAP患者 62 1 776.82±98.771) 0.94±0.221) AKIⅡ期SAP患者 48 1 285.50±85.931)2) 1.68±0.351)2) AKI Ⅲ期SAP患者 20 825.32±42.831)2)3) 2.24±0.581)2)3) Fa) 874.412 332.569 Pa) < 0.001 < 0.001 r -0.624 0.498 P < 0.05 < 0.05 注:a)整体比较为单因素方差分析, 多重比较为LSD-t检验。与健康志愿者比较,1)P < 0.05;与AKIⅠ期SAP患者比较,2)P < 0.05;与AKIⅡ期SAP患者比较,3)P < 0.05。 表 2 死亡组、生存组临床资料比较
X±S 临床资料 死亡组(32例) 生存组(98例) t/χ2 P 性别/例(%) 0.083 0.773 男 20(62.50) 64(65.31) 女 12(37.50) 34(34.69) 年龄/岁 46.36±6.18 46.21±6.20 0.119 0.906 BMI/(kg/m2) 21.25±1.02 21.07±1.05 0.848 0.398 吸烟史/例(%) 12(37.50) 32(32.65) 0.253 0.615 酗酒史/例(%) 18(56.25) 50(51.02) 0.264 0.607 高血压/例(%) 12(37.50) 32(32.65) 0.253 0.615 糖尿病/例(%) 8(25.00) 20(20.41) 0.301 0.583 APACHE Ⅱ评分/分 18.25±3.15 9.50±1.45 15.197 < 0.001 CRRT治疗/例(%) 22(68.75) 30(30.61) 14.619 < 0.001 血红蛋白/(g/L) 137.54±10.99 139.26±12.25 0.707 0.481 血白蛋白/(g/L) 33.80±5.25 34.20±5.20 0.377 0.707 白细胞计数/(×109/L) 15.50±2.54 14.76±2.44 1.475 0.143 血肌酐/(μmol/L) 114.26±9.40 96.22±7.16 9.954 < 0.001 尿酸/(μmol/L) 389.25±42.16 380.65±40.29 1.037 0.302 尿素氮/(mmol/L) 15.25±1.26 10.84±1.20 17.830 < 0.001 甘油三酯/(mmol/L) 3.10±0.65 2.98±0.24 1.022 0.314 总胆固醇/(mmol/L) 4.20±0.71 4.38±0.75 1.194 0.235 D-D/(mg/L) 31.05±3.74 20.47±2.16 15.196 < 0.001 CRP/(mg/L) 182.46±20.26 180.14±18.75 0.596 0.552 KIM-1/(ng/L) 5.50±0.78 2.08±0.34 34.654 < 0.001 SIRT1/(pg/mL) 1 028.63±74.42 1 587.60±89.64 31.849 < 0.001 Syndecan-1/(μg/mL) 2.18±0.52 1.16±0.29 10.572 < 0.001 表 3 logistic回归分析赋值
变量 代码 因素/指标 哑变量赋值设计 因变量 Y 临床转归 死亡=1,存活=0 自变量 X1 APACHE Ⅱ评分 ≥10=1,否=0 X2 CRRT治疗 是=1,否=0 X3 血肌酐 ≥100 μmol/L=1,否=0 X4 尿素氮 ≥11 mmol/L=1,否=0 X5 D-D ≥22 mg/L=1,否=0 X6 KIM-1 ≥2.5 ng/L=1,否=0 X7 SIRT1 ≥1 400 pg/mL=1,否=0 X8 Syndecan-1 ≥1.4 μg/mL=1,否=0 表 4 影响SAP合并AKI患者死亡的危险因素
自变量 β SE Wald χ2 P OR 95%CI 常数项 -0.146 0.061 5.692 0.017 APACHE Ⅱ评分 0.594 0.167 12.589 < 0.001 1.812 1.305~2.515 血肌酐 0.501 0.198 6.390 0.011 1.650 1.119~2.434 D-D 0.628 0.212 8.788 0.003 1.874 1.237~2.838 KIM-1 0.686 0.184 13.870 < 0.001 1.985 1.384~2.849 SIRT1 -0.533 0.147 13.065 < 0.001 0.587 0.440~0.784 Syndecan-1 0.817 0.225 13.234 < 0.001 2.264 1.458~3.515 表 5 血清SIRT1和Syndecan-1预测SAP合并AKI患者死亡的效能
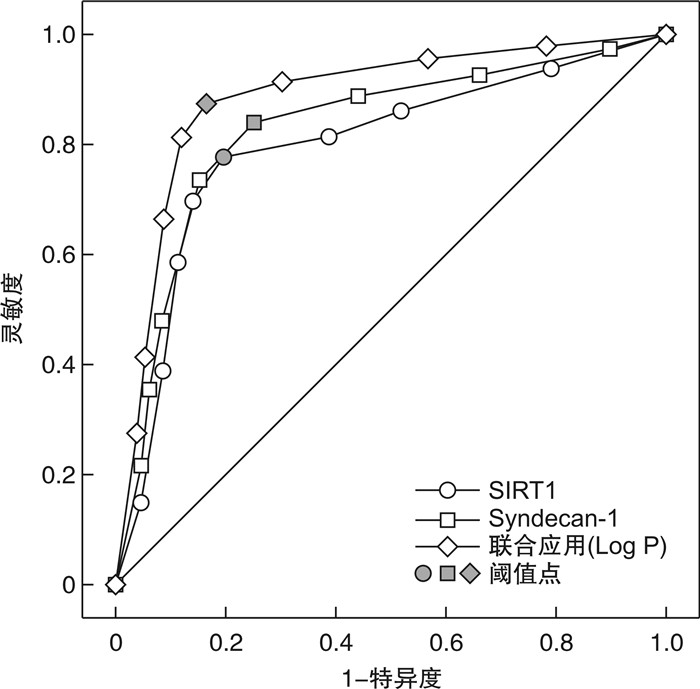
指标 AUC(95%CI) 阈值 灵敏度 特异度 约登指数 准确度(n/N) SIRT1 0.803(0.634~0.948) 0.5(1 400 pg/mL) 0.781 0.806 0.587 0.800 Syndecan-1 0.827(0.702~0.929) 0.5(1.4 μg/mL) 0.844 0.745 0.589 0.769 联合应用模型 0.857(0.768~0.939) 0.14a) 0.875 0.837 0.712 0.846 a)联合应用模型的阈值为Ln(P/1-P)模型的理论计算值。各样本对应指标的输入值为回归哑变量值。 -
[1] Gupta M, Liti B, Barrett C, et al. Prevention and management of hypertriglyceridemia-induced acute pancreatitis during pregnancy: a systematic review[J]. Am J Med, 2022, 135(6): 709-714. doi: 10.1016/j.amjmed.2021.12.006
[2] 高娜, 李静. 重症急性胰腺炎合并急性肾损伤的危险因素分析[J]. 临床消化病杂志, 2022, 34(3): 203-206.
[3] 李峰, 刘春生. 全身免疫炎症指数对重症胰腺炎并发急性肾损伤早期预测价值的研究[J]. 临床急诊杂志, 2022, 23(2): 100-105. https://lcjz.whuhzzs.com/article/doi/10.13201/j.issn.1009-5918.2022.02.005
[4] Wei S, Gao Y, Dai X, et al. SIRT1-mediated HMGB1 deacetylation suppresses sepsis-associated acute kidney injury[J]. Am J Physiol Renal Physiol, 2019, 316(1): F20-F31. doi: 10.1152/ajprenal.00119.2018
[5] Ay D, Engin M, Sünbül SA, et al. Syndecan-1 as a marker to predict acute kidney injury after isolated coronary artery bypass graft operations[J]. Rev Assoc Med Bras, 2023, 69(1): 107-111. doi: 10.1590/1806-9282.20220839
[6] 中华医学会消化病学分会胰腺疾病学组, 中华胰腺病杂志编辑委员会, 中华消化杂志编辑委员会. 中国急性胰腺炎诊治指南(2019年, 沈阳)[J]. 中华消化杂志, 2019, 39(11): 721-730.
[7] 郭锦洲. 改善全球肾脏病预后组织(KDIGO)临床实践指南: 急性肾损伤[J]. 肾脏病与透析肾移植杂志, 2013, 22(1): 57-60.
[8] Bahtouee M, Eghbali SS, Maleki N, et al. Acute Physiology and Chronic Health Evaluation Ⅱ score for the assessment of mortality prediction in the intensive care unit: a single-centre study from Iran[J]. Nurs Crit Care, 2019, 24(6): 375-380. doi: 10.1111/nicc.12401
[9] Vannier E, Dupont-Lucas C, Lagarde B, et al. Development of a score for predicting severe acute pancreatitis at admission[J]. Pancreas, 2022, 51(2): 128-134. doi: 10.1097/MPA.0000000000001984
[10] 黄铭凤, 叶博, 周晶, 等. 急性胰腺炎并发急性肾损伤患者的临床转归及死亡的危险因素分析[J]. 中华胰腺病杂志, 2022, 22(5): 335-340.
[11] 王艳, 王利利, 刘伟, 等. 血必净注射液对重症急性胰腺炎患者肾功能、炎性因子和外周血单核细胞TLR4/NF-κB信号通路的影响[J]. 现代生物医学进展, 2023, 23(4): 709-713.
[12] 郭喆, 关键. 重症急性胰腺炎预防与阻断急诊专家共识[J]. 临床急诊杂志, 2022, 23(7): 451-462. https://lcjz.whuhzzs.com/article/doi/10.13201/j.issn.1009-5918.2022.07.001
[13] 郑寿浩, 丁国明. 沉默交配型信息调节2同系物-1激活剂SRT1720对重度失血性休克/复苏大鼠急性肾损伤的治疗作用及机制[J]. 中国血液净化, 2022, 21(1): 42-47.
[14] Liu Y, Sun Y, Xue BH, et al. Negative regulation of SIRT1 by IRF9 involved in hyperlipidemia acute pancreatitis associated with kidney injury[J]. Dig Dis Sci, 2021, 66(4): 1063-1071. doi: 10.1007/s10620-020-06331-1
[15] Hahn RG, Zdolsek M, Zdolsek J. Plasma concentrations of syndecan-1 are dependent on kidney function[J]. Acta Anaesthesiol Scand, 2021, 65(6): 809-815. doi: 10.1111/aas.13801
[16] Nascimento de Moura AC, Mota S, Holanda F, et al. Syndecan-1 predicts hemodynamic instability in critically ill patients under intermittent hemodialysis[J]. Clin Kidney J, 2023, 16(7): 1132-1138. doi: 10.1093/ckj/sfad043
[17] 王旭东, 赵玉良, 史为涛, 等. 黄芪多糖对脓毒症急性肾损伤大鼠AMPK/SIRT1信号通路介导的肾上皮细胞能量代谢的影响[J]. 中国医院药学杂志, 2021, 41(21): 2181-2185.
[18] 孔超, 张艳, 孙静姝, 等. 血清syndecan-1在成人急性肾损伤诊断中价值探讨[J]. 中国中西医结合肾病杂志, 2022, 23(4): 339-342.
[19] 杨姗, 李红, 庄惠君, 等. 血清肌酐和肾小球滤过率与代谢综合征患病率相关性的横断面研究[J]. 重庆医学, 2022, 51(10): 1670-1674.
[20] 陈红, 李松, 宋春元, 等. D-D, Fib和血小板参数对急性胰腺炎严重程度的诊断价值[J]. 川北医学院学报, 2022, 37(5): 650-652.
[21] 易立勋, 刘辉亮. NGAL、KIM-1和IL-18对创伤性肾损伤的早期诊断价值[J]. 海南医学院学报, 2015, 21(2): 191-193.
-




 下载:
下载: