Clinical effect of dexmedetomidine on cardiac function protection in patients with severe pneumonia on mechanical ventilation
-
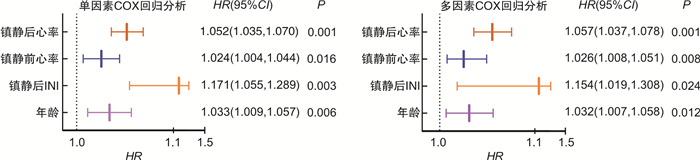
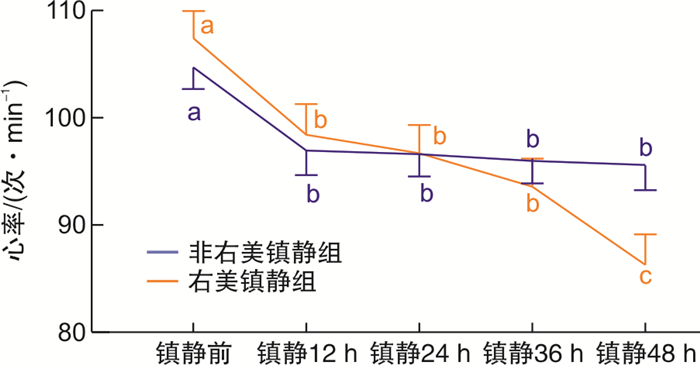
摘要: 目的 探讨右美托咪定对重症肺炎机械通气患者心功能保护的临床疗效。方法 回顾性分析南京医科大学附属常州第二人民医院急诊科2019年1月—2021年7月收治的112例重症肺炎机械通气伴休克患者的临床资料,根据镇静药物分为非右美托咪定镇静组60例和右美托咪定镇静组52例。观察两组患者镇静前后心肌损伤血液参数变化、心率变化以及血管活性药物剂量对比。结果 右美托咪定镇静后患者的肌钙蛋白I和脑钠肽显著下降,差异有统计学意义(P< 0.05); 非右美托咪定镇静后患者肌钙蛋白I和脑利钠肽显著升高,差异有统计学意义(P< 0.05)。重复测量方差分析显示右美托咪定镇静后患者心率显著下降,差异有统计学意义(P< 0.05)。校正混杂因素后多因素COX回归分析显示镇静前和镇静后48 h心率增快是患者死亡独立风险因素(HR:1.026,95%CI:1.008~1.051,P=0.008 vs.HR:1.057,95%CI:1.037~1.078,P< 0.001),且这一风险随着心率增快呈现趋势变化(P< 0.001)。两组患者总体血管活性药物用量差异无统计学意义(P>0.05)。结论 右美托咪定镇静显著降低重症肺炎伴机械通气及休克患者心率、肌钙蛋白I和脑利钠肽,保护心功能。Abstract: Objective To investigate the clinical effect of dexmedetomidine on cardiac function protection in patients with severe pneumonia on mechanical ventilation.Methods A retrospective analysis was performed on 112 patients with severe pneumonia with mechanical ventilation and shock in Changzhou NO.2 People's Hospital, the Affiliated Hospital of Nanjing Medical University from January 2019 to July 2021. According to sedative drugs, 60 patients were divided into non-dexmedetomidine sedation group and 52 patients were divided into dexmedetomidine sedation group. The changes of myocardial injury blood parameters, heart rate and the dose of vasoactive drugs were observed before and after sedation between the two groups.Results Troponin I and brain natriuretic peptide significantly decreased after dexmedetomidine sedation, and the difference was statistically significant(P< 0.05), while troponin I and brain natriuretic peptide were significantly increased after dexmedetomidine sedation, and the difference was statistically significant(P< 0.05). Repeated measures analysis of variance(ANOVA) showed a significant decrease in heart rate after dexmedetomidine sedation, and the difference was statistically significant(P< 0.05). Multivariate COX regression analysis after adjusting for confounding factors showed that increased heart rate before sedation and 48 hours after sedation was an independent risk factor for death(HR: 1.026, 95%CI: 1.008-1.051,P=0.008 vs.HR: 1.057, 95%CI: 1.037-1.078,P< 0.001). And there was a trend change(P for trend < 0.001). There was no significant difference in the total amount of vasoactive drugs between the two groups, and the difference was not statistically significant(P>0.05).Conclusion Dexmedetomidine sedation significantly reduced heart rate, troponin I and brain natriuretic peptide, and protected cardiac function in patients with severe pneumonia with mechanical ventilation and shock.
-
Key words:
- severe pneumonia /
- dexmedetomidine /
- shock /
- prognosis
-

-
表 1 两组患者一般基线资料比较
例 资料 非右美托咪定镇静组 右美托咪定镇静组 t/Z/χ2 P 性别 0.733 0.392 男 39 28 女 21 24 年龄/岁 76(68,86) 72(65,82) -1.149 0.250 高血压 27 23 2.170 0.141 糖尿病 14 15 2.820 0.093 吸烟 11 6 0.129 0.720 COPD 5 5 0.505a) 冠心病 9 7 0.174 0.677 APACHEⅡ评分/分 22.18±7.13 20.92±7.77 0.800 0.426 注:a)为Fisher精确检验。 表 2 两组患者镇静前后心肌损伤指标比较
M(P25,P75) 指标 镇静前 镇静后 Z P 非右美托咪定镇静组 TNI/(ng·mL-1) 0.044(0.012,0.139) 0.119(0.023,0.51) -2.529 0.011 BNP/(pg·mL-1) 2150(650,6455) 3480(1357,7665) -2.296 0.022 CPK/(mmol·L-1) 74.5(29.7,152.7) 97(34.8,264.0) -0.082 0.935 CKMB/(mmol·L-1) 8.7(4.4,13.8) 7(4.0,12.7) -0.710 0.478 AST/(U·L-1) 40.0(22.0,60.0) 39.5(24.3,77.3) -0.902 0.367 LDH/(U·L-1) 282.2(203.8,531.2) 318.7(217.5,520.3) -1.746 0.081 呼吸/(次·min-1) 26(23,28) 18(16,22) -4.519 < 0.001 右美托咪定镇静组 TNI/(ng·mL-1) 0.067(0.019,0.584) 0.047(0.019,0.134) -2.830 0.005 BNP/(pg·mL-1) 4326(2310,6350) 1660(996,3635) -2.529 0.011 CPK(mmol·L-1) 127(60,422) 155(39,396) -0.241 0.809 CKMB/(mmol·L-1) 12.75(6.03,26.70) 9.7(4.65,14.83) -1.310 0.190 AST/(U·L-1) 40(31,84) 51.5(35,204.5) -1.799 0.720 LDH/(U·L-1) 312.7(220.7,482.5) 408.6(242.8,609.2) -1.115 0.265 呼吸/(次·min-1) 26(24,30) 18(16,20) -5.165 < 0.001 表 3 镇静48h后心率分层COX回归分析
心率/(次·min-1) 单因素COX回归 多因素COX回归分析 HR(95%CI) P HR(95%CI) P ≤76 1 1 77~91 2.452(0.851~7.064) 0.097 1.905(0.616~5.896) 0.263 92~107 7.761(2.834~21.255) < 0.001 6.480(2.248~18.676) 0.001 ≥108 11.564(4.311~31.021) < 0.001 12.308(4.397~34.452) < 0.001 P < 0.001 < 0.001 注:多因素Cox回归分析校正了性别、年龄、高血压、糖尿病、冠心病、COPD和吸烟等因素。 表 4 两组患者血管活性药物使用剂量及并发心房颤动比较
项目 非右美托咪定镇静组 右美托咪定镇静组 Z/χ2 P 药物 去甲肾上腺素/支 24(0.5,86) 10(0,24) -1.724 0.085 间羟胺/支 45(10,103.75) 31.5(10,112.5) -0.545 0.586 心房颤动发生率/% 31.67(19/60) 19.23(10/52) 0.384 0.535 -
[1] Russell FM, Reyburn R, Chan J, et al. Impact of the change in WHO's severe pneumonia case definition on hospitalized pneumonia epidemiology: case studies from six countries[J]. Bull World Health Organ, 2019, 97(6): 386-393. doi: 10.2471/BLT.18.223271
[2] 中华医学会重症医学分会. 中国成人ICU镇痛和镇静治疗指南[J]. 中华危重病急救医学, 2018, 30(6): 497-514. doi: 10.3760/cma.j.issn.2095-4352.2018.06.001
[3] De Cassai A, Boscolo A, Geraldini F, et al. Effect of dexmedetomidine on hemodynamic responses to tracheal intubation: A meta-analysis with meta-regression and trial sequential analysis[J]. J Clin Anesth, 2021, 72: 110287. doi: 10.1016/j.jclinane.2021.110287
[4] Metlay JP, Waterer GW, Long AC, et al. Diagnosis and Treatment of Adults with Community-acquired Pneumonia. An Official Clinical Practice Guideline of the American Thoracic Society and Infectious Diseases Society of America[J]. Am J Respir Crit Care Med, 2019, 200(7): e45-e67. doi: 10.1164/rccm.201908-1581ST
[5] Nair GB, Niederman MS. Updates on community acquired pneumonia management in the ICU[J]. Pharmacol Ther, 2021, 217: 107663. doi: 10.1016/j.pharmthera.2020.107663
[6] Eleveld DJ, Colin P, Absalom AR, et al. Pharmacokinetic-pharmacodynamic model for propofol for broad application in anaesthesia and sedation[J]. Br J Anaesth, 2018, 120(5): 942-959. doi: 10.1016/j.bja.2018.01.018
[7] Pastis NJ, Yarmus LB, Schippers F, et al. Safety and Efficacy of Remimazolam Compared With Placebo and Midazolam for Moderate Sedation During Bronchoscopy[J]. Chest, 2019, 155(1): 137-146. doi: 10.1016/j.chest.2018.09.015
[8] Zhu CH, Yu J, Wang BQ, et al. Dexmedetomidine reduces ventilator-induced lung injury via ERK1/2 pathway activation[J]. Mol Med Rep, 2020, 22(6): 5378-5384. doi: 10.3892/mmr.2020.11612
[9] 赵珊珊, 金兆辰, 李勇. 应用右美托咪定及丙泊酚在重症肺炎使用有创机械通气患者中的镇静疗效研究[J]. 中华临床医师杂志(电子版), 2018, 12(11): 595-599. doi: 10.3877/cma.j.issn.1674-0785.2018.11.001
[10] 朱满意, 韦正祥, 李明新. 床旁超声评估右美托咪定镇静对机械通气患者胃肠功能的影响[J]. 临床急诊杂志, 2021, 22(5): 309-313. https://www.cnki.com.cn/Article/CJFDTOTAL-ZZLC202105004.htm
[11] Shen L, Jhund PS, Anand IS, et al. Incidence and Outcomes of Pneumonia in Patients With Heart Failure[J]. J Am Coll Cardiol, 2021, 77(16): 1961-1973. doi: 10.1016/j.jacc.2021.03.001
[12] Yu T, Liu D, Gao M, et al. Dexmedetomidine prevents septic myocardial dysfunction in rats via activation of α7nAChR and PI3K/Akt-mediated autophagy[J]. Biomed Pharmacother, 2019, 120: 109231. doi: 10.1016/j.biopha.2019.109231
[13] Aston SJ, Ho A, Jary H, et al. Etiology and Risk Factors for Mortality in an Adult Community-acquired Pneumonia Cohort in Malawi[J]. Am J Respir Crit Care Med, 2019, 200(3): 359-369. doi: 10.1164/rccm.201807-1333OC
[14] Zhang X, Wang R, Lu J, et al. Effects of different doses of dexmedetomidine on heart rate and blood pressure in intensive care unit patients[J]. Exp Ther Med, 2016, 11(1): 360-366. doi: 10.3892/etm.2015.2872
[15] Espinoza R, Silva J, Bergmann A, et al. Factors associated with mortality in severe community-acquired pneumonia: A multicenter cohort study[J]. J Crit Care, 2019, 50: 82-86. doi: 10.1016/j.jcrc.2018.11.024
[16] Jentzer JC, Vallabhajosyula S, Khanna AK, et al. Management of Refractory Vasodilatory Shock[J]. Chest, 2018, 154(2): 416-426. doi: 10.1016/j.chest.2017.12.021
[17] Lei Y, Peng X, Hu Y, et al. The Calcilytic Drug Calhex-231 Ameliorates Vascular Hyporesponsiveness in Traumatic Hemorrhagic Shock by Inhibiting Oxidative Stress and miR-208a-Mediated Mitochondrial Fission[J]. Oxid Med Cell Longev, 2020, 2020: 4132785.
[18] Ruder TL, Donahue KR, Colavecchia AC, et al. Hemodynamic Effects of Dexmedetomidine in Adults With Reduced Ejection Fraction Heart Failure[J]. J Intensive Care Med, 2021, 36(8): 893-899. doi: 10.1177/0885066620934416
[19] Morelli A, Sanfilippo F, Arnemann P, et al. The Effect of Propofol and Dexmedetomidine Sedation on Norepinephrine Requirements in Septic Shock Patients: A Crossover Trial[J]. Crit Care Med, 2019, 47(2): e89-e95. doi: 10.1097/CCM.0000000000003520
[20] Ferreira J. The Theory is Out There: The Use of ALPHA-2 Agonists in Treatment of Septic Shock[J]. Shock, 2018, 49(4): 358-363. doi: 10.1097/SHK.0000000000000979
-




 下载:
下载: