Establishment and evaluation of an early warning model for major cardiovascular adverse events in emergency patients with chest pain within 30 days
-
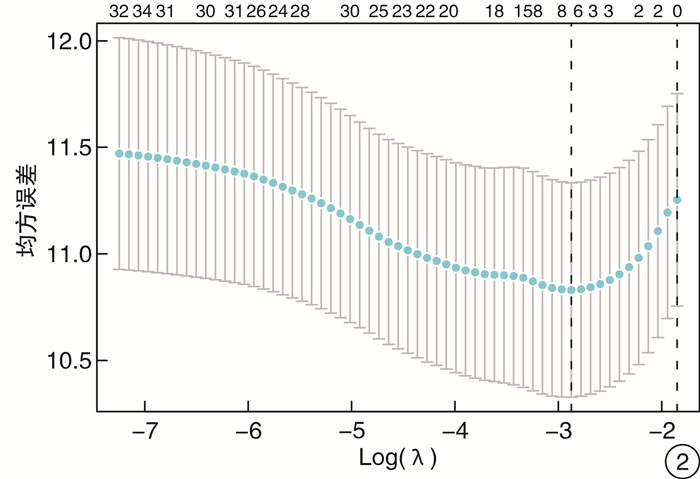
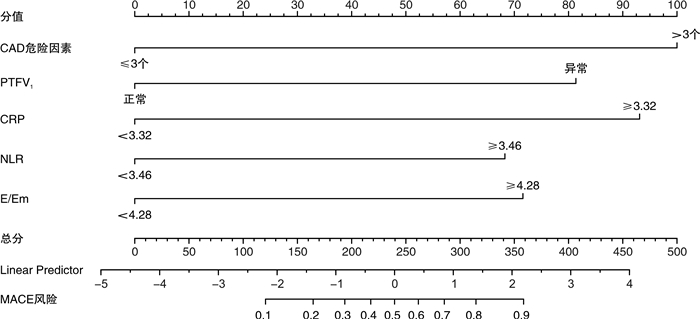
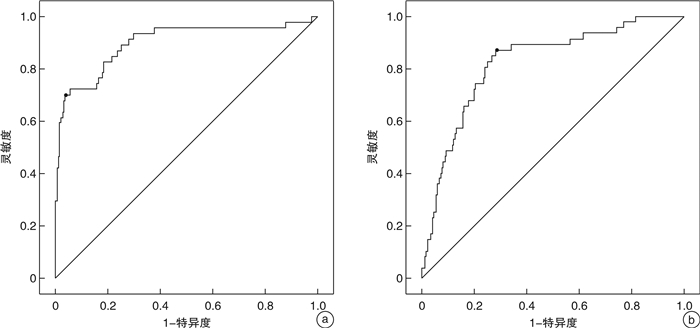
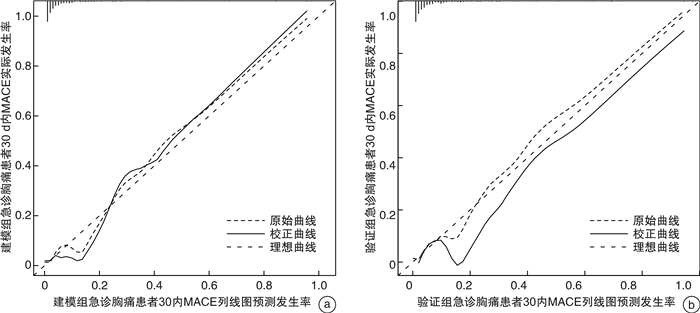
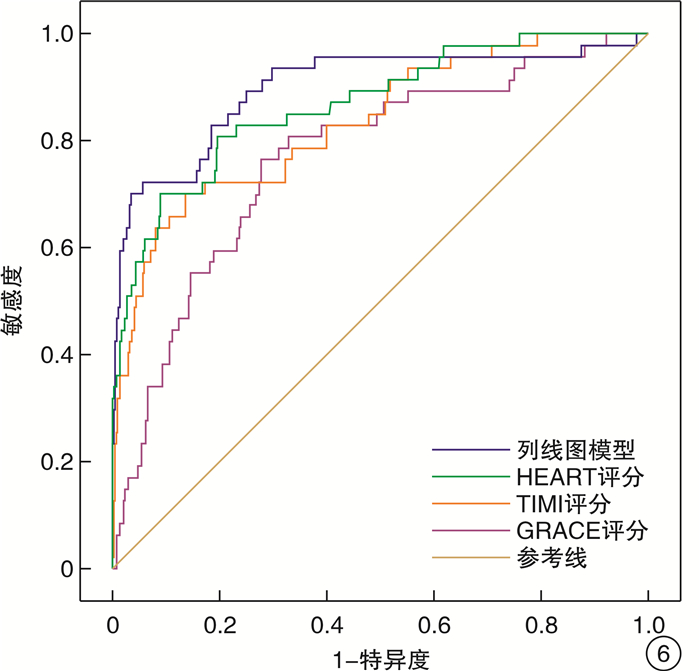
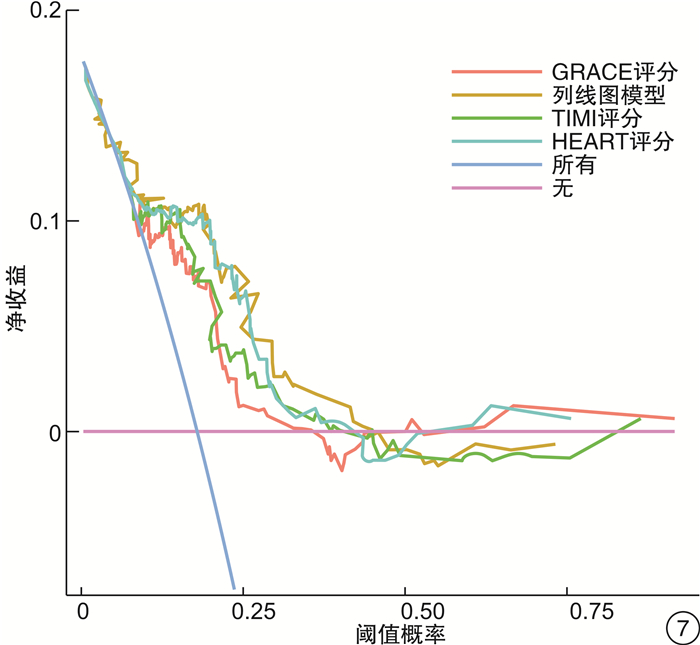
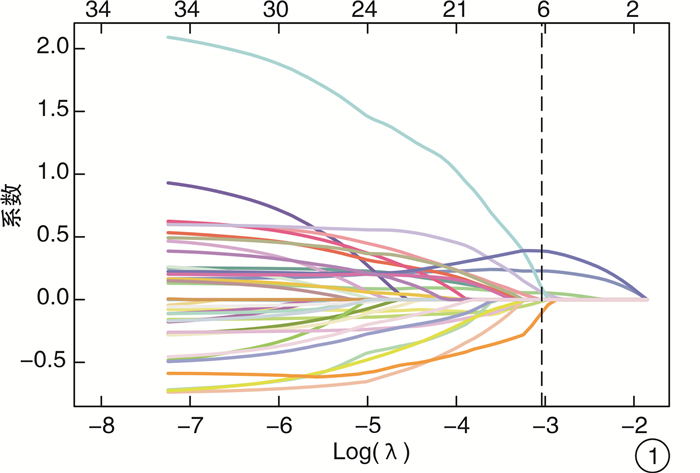
摘要: 目的 通过分析急诊胸痛患者一般资料、心电图指标、血清学指标及超声心动图指标筛选影响患者30 d内主要心血管不良事件(MACE)发生的危险因素,建立列线图预测模型并验证预测效果。方法 采用便利抽样法选取2017年1月-2020年10月我院收治的487例急诊胸痛患者作为建模组,另选取2020年11月-2021年12月我院收治的急诊胸痛患者185例作为验证组。收集患者的一般资料及临床检测指标,使用LASSO回归、多因素logistic回归分析筛选变量并绘制列线图预警模型。采用受试者工作特征(ROC)曲线、C-index、校准曲线评价模型的区分度和校准度;决策曲线分析(DCA)评估预测模型的临床有效性。结果 使用LASSO回归分析筛选出7个预测变量,采用多因素logistic回归进一步分析显示,冠状动脉疾病(CAD)危险因素 > 3个、心电图V1导联P波终末电势(PTFV1)异常、CRP≥3.32、NLR≥3.46、E/Em≥4.28是影响急诊胸痛患者30 d内MACE发生的独立危险因素(P < 0.05);基于预测变量绘制列线图预警模型,模型预测建模组与验证组患者发生MACE的C-index为0.896、0.802,AUC分别为0.900、0.823,且建模组与验证组的校准曲线显示预测发生风险与实际观察的发生风险基本一致;将本研究中列线图模型预测MACE的效果与HEART评分、GRACE评分、TIMI评分模型比较,结果显示列线图模型的AUC与DCA阈概率范围均大于3种评分模型,有更高的预测效能与临床应用价值。结论 基于5个预测变量建立的列线图预测模型在预测急诊胸痛患者30 d MACE发生率具有更准确地预测效果与更高的临床应用价值,有助于临床早期识别出MACE高危人群从而制定针对性的预防干预措施。Abstract: Objective By analyzing the general data, electrocardiographic indexes, serological indexes and echocardiographic indexes of patients with chest pain in emergency department, the risk factors affecting the occurrence of major adverse cardiovascular events(MACE) within 30 days were screened, and a nomogram prediction model was established to verify the prediction effect.Methods Convenience sampling method was used to select 487 emergency chest pain patients admitted to our hospital from January 2017 to October 2020 as the modeling group, and another 185 emergency chest pain patients admitted to our hospital from November 2020 to December 2021 were selected as validation Group. The general information and clinical test indicators of the patients were collected, and LASSO regression and multivariate logistic regression analysis were used to screen variables and draw a nomogram warning model. Receiver operating characteristic(ROC) curve, C-index, and calibration curve were used to evaluate the discrimination and calibration of the model; decision curve analysis(DCA) was used to evaluate the clinical validity of the prediction model.Results Screening out 7 predictors using LASSO regression analysis, further analysis by multivariate logistic regression showed that CAD risk factors > 3, abnormal PTFV1, CRP≥3.32, NLR≥3.46, E/Em≥4.28 were independent risk factors affecting the occurrence of MACE within 30 days of emergency chest pain patients(P < 0.05). Drawing a nomogram warning model based on the predictor variables, the C-index of the model predicting the occurrence of MACE in the modeling group and the validation group was 0.896 and 0.802, and the AUC was 0.900 and 0.823, respectively. And the calibration curves of the modeling group and the validation group show that the predicted occurrence risk was basically consistent with the actual observed occurrence risk. Comparing the effect of the nomogram model in predicting MACE with the HEART score, GRACE score, and TIMI score model in this study, the results showed that the AUC and DCA threshold probability ranges of the nomogram model were both greater than the three scores model, demonstrating higher predictive performance and clinical application value.Conclusion The nomogram prediction model based on five predictors has more accurate prediction effect and higher clinical application value in predicting the incidence of 30 d MACE in emergency chest pain patients, and is helpful to identify the high-risk groups of MACE in the early clinical stage so as to formulate targeted preventive interventions.
-
Key words:
- emergency chest pain /
- adverse cardiovascular events /
- prognosis /
- early warning model
-

-
表 1 建模组与验证组患者一般特征、心电图指标、血清学指标及心动图指标比较
例(%) 指标 建模组(487例) 验证组(185例) 统计值 P 年龄/岁 68.74±10.53 67.45±9.26 1.465 0.143 性别 0.947 0.331 男 256(52.57) 105(56.76) 女 231(47.43) 80(43.24) CAD危险因素 高血压 112(23.00) 32(17.30) 2.588 0.108 高脂血症 302(62.01) 110(59.46) 0.368 0.544 糖尿病 108(22.18) 35(18.92) 0.849 0.357 冠心病家族史 73(14.99) 33(17.84) 0.819 0.366 吸烟 79(16.22) 35(18.92) 0.692 0.405 大量饮酒史 210(43.12) 89(48.11) 1.350 0.245 肥胖 199(40.86) 83(44.86) 0.882 0.348 CAD危险因素/个 1.516 0.218 ≤3 345(70.84) 122(65.95) > 3 142(29.16) 63(34.05) 既往脑卒中史 0.539 0.463 无 456(93.63) 176(95.14) 有 31(6.37) 9(4.86) 既往心肌梗死史 1.754 0.185 无 379(77.82) 135(72.97) 有 108(22.18) 50(27.03) 收缩压/mmHg 138.72±27.65 135.57±29.40 1.296 0.195 舒张压/mmHg 77.56±12.33 78.24±14.86 0.602 0.547 心率/(次·min-1) 82.44±16.28 81.06±14.52 1.010 0.313 VPB 2.961 0.085 否 376(77.21) 131(70.81) 是 111(22.79) 54(29.19) PTFV1 1.376 0.241 正常 403(82.75) 160(86.49) 异常 84(17.25) 25(13.51) QTc 0.402 0.526 正常 415(85.22) 154(83.24) 延长 72(14.78) 31(16.76) CTnT/(ng·mL-1) 1.66±0.24 1.62±0.20 1.016 0.044 CK-MB/(U·L-1) 86.47±11.39 88.34±12.47 1.851 0.065 NT-proBNP/(ng·L-1) 94(73,122) 91(71,113) 1.925 0.054 白蛋白/(g·L-1) 41.84±7.35 42.03±8.61 0.285 0.776 血红蛋白/(g·L-1) 139.10±16.43 140.35±14.18 0.914 0.361 CRP/(mg·L-1) 2.26(1.75,3.67) 2.31(1.69,3.56) 1.324 0.103 NLR 2.58(1.88,3.39) 2.47(180,3.47) 1.106 0.144 Scr/(μmol·L-1) 80.68±15.38 78.49±16.73 1.609 0.108 空腹血糖/(mmol·L-1) 6.22±1.51 5.90±1.24 2.571 0.010 LAD/mm 34.76±3.89 33.92±4.10 2.463 0.014 LVESD/mm 34.07±3.72 33.86±4.38 0.622 0.534 LVEDD/mm 51.21±5.38 50.48±4.85 1.613 0.107 LVEF/% 60.74±4.28 61.35±3.69 1.712 0.087 LVH 0.253 0.615 否 344(70.64) 127(68.65) 是 143(29.36) 58(31.35) E/A 1.25(1.12,1.41) 1.20(1.09,1.37) 1.547 0.104 E/Em 4.32(3.55,5.37) 4.43(3.64,5.44) 1.143 0.096 注:1 mmHg=0.133 kPa。 表 2 变量赋值
变量 赋值 年龄 原值输入 CAD危险因素 ≤3个=0,>3个=1 PTFV1 正常=0,异常=1 cTnT 原值输入 CRP CRP < 3.32=0,CRP≥3.32=1 NLR NLR < 3.46=0,NLR≥3.46=1 E/Em E/Em < 4.28=0,E/Em≥4.28=1 表 3 影响急诊胸痛患者30d内MACE发生的多因素分析
因素 β SE Wald P OR 95%CI 下限 上限 年龄 0.029 0.020 2.209 0.137 1.030 0.991 1.070 CAD危险因素>3个 1.887 0.397 22.653 0.000 6.602 3.035 14.361 PTFV1 1.547 0.426 13.180 0.000 4.697 2.038 10.826 CTnT -0.128 0.847 0.023 0.880 0.880 0.167 4.632 CRP 1.675 0.516 10.553 0.001 5.340 1.943 14.671 NLR 1.235 0.388 10.102 0.001 3.438 1.605 7.361 E/Em 1.368 0.551 6.167 0.013 3.929 1.334 11.571 常量 -6.254 1.986 9.919 0.002 0.002 -
[1] 黄振华, 肖孝勇, 叶子, 等. 比较HEART、GRACE评分对急诊科急性胸痛患者30天MACE预测价值[J]. 中华急诊医学杂志, 2019, 28(2): 203-207.
[2] Boubaker H, Beltaief K, Grissa MH, et al. Inaccuracy of Thrombolysis in Myocardial Infarction and Global Registry in Acute Coronary Events scores in predicting outcome in ED patients with potential ischemic chest pain[J]. Am J Emerg Med, 2015, 33(9): 1209-1212. doi: 10.1016/j.ajem.2015.05.019
[3] Lin Z, Lim SH, Chua S, et al. High-sensitivity troponin T and long-term adverse cardiac events among patients presenting with suspected acute coronary syndrome in Singapore[J]. Singapore Med J, 2019, 60(8): 418-426. doi: 10.11622/smedj.2019013
[4] 俞尧, 陈东旭, 廖凤卿, 等. HEART、TIMI及GRACE评分对非ST段抬高型心肌梗死患者心血管不良事件的预测价值[J]. 中华急诊医学杂志, 2020, 29(7): 908-913. doi: 10.3760/cma.j.issn.1671-0282.2020.07.004
[5] 唐开放, 孔健华, 冯玉丽, 等. 改良HEART评分与GRACE评分在急诊高危胸痛患者分层治疗中的对比评价[J]. 临床急诊杂志, 2020, 21(4): 318-322. https://www.cnki.com.cn/Article/CJFDTOTAL-ZZLC202004013.htm
[6] 廖云海, 卢静, 王志民. HEART评分对急诊胸痛患者心血管不良事件的预测价值[J]. 中国现代医生, 2018, 56(24): 12-14. https://www.cnki.com.cn/Article/CJFDTOTAL-ZDYS201824004.htm
[7] Stopyra JP, Harper WS, Higgins TJ, et al. Prehospital Modified HEART Score Predictive of 30-Day Adverse Cardiac Events[J]. Prehosp Disaster Med, 2018, 33(1): 58-62. doi: 10.1017/S1049023X17007154
[8] 何路遥, 于文娟, 黄晶晶, 等. 第2代抗精神病药引起QTc间期延长的研究进展[J]. 中华精神科杂志, 2021, 54(1): 50-56. doi: 10.3760/cma.j.cn113661-20200322-00133
[9] 刘富湘, 莫介超, 陈注有, 等. 急性ST段抬高型心肌梗死患者急诊PCI术前中性粒细胞与淋巴细胞比率和TIMI风险评分的关系[J]. 广东医科大学学报, 2021, 39(3): 293-298. doi: 10.3969/j.issn.1005-4057.2021.03.013
[10] Bradshaw PJ, Ko DT, Newman AM, et al. Validity of the GRACE(Global Registry of Acute Coronary Events)acute coronary syndrome prediction model for six month post-discharge death in an independent data set[J]. Heart, 2006, 92(7): 905-909. doi: 10.1136/hrt.2005.073122
[11] Six AJ, Cullen L, Backus BE, et al. The HEART score for the assessment of patients with chest pain in the emergency department: a multinational validation study[J]. Crit Pathw Cardiol, 2013, 12(3): 121-126. doi: 10.1097/HPC.0b013e31828b327e
[12] 夏海云, 丁霞, 傅琳. 现场快速检测高敏肌钙蛋白在老年急性心肌梗死早期的临床诊断价值[J]. 临床急诊杂志, 2022, 23(1): 67-71. https://whxhyy.xml-journal.net/article/doi/10.13201/j.issn.1009-5918.2022.01.015
[13] Sanchis J, Bodí V, Núñez J, et al. New risk score for patients with acute chest pain, non-ST-segment deviation, and normal troponin concentrations: a comparison with the TIMI risk score[J]. J Am Coll Cardiol, 2005, 46(3): 443-449. doi: 10.1016/j.jacc.2005.04.037
[14] 刘文德, 胡华元. HEART评分与GRACE评分系统对高危急性胸痛患者30天心血管不良事件的预测价值比较[J]. 广东医学, 2018, 39(17): 2632-2634. doi: 10.3969/j.issn.1001-9448.2018.17.018
[15] 余洋, 李博, 刘聚伟, 等. 基于HEART评分预测心电图非ST段抬高的急性胸痛患者心脏不良事件的价值[J]. 实用医学杂志, 2019, 35(14): 2261-2265. doi: 10.3969/j.issn.1006-5725.2019.14.015
[16] Tereshchenko LG, Henrikson CA, Sotoodehnia N, et al. Electrocardiographic deep terminal negativity of the P wave in V(1) and risk of sudden cardiac death: the Atherosclerosis Risk in Communities(ARIC)study[J]. J Am Heart Assoc, 2014, 3(6): e001387. doi: 10.1161/JAHA.114.001387
[17] Huang Z, Zheng Z, Wu B, et al. Predictive value of P wave terminal force in lead V1 for atrial fibrillation: A meta-analysis[J]. Ann Noninvasive Electrocardiol, 2020, 25(4): e12739.
[18] Okin PM, Kamel H, Kjeldsen SE, et al. Electrocardiographic left atrial abnormalities and risk of incident stroke in hypertensive patients with electrocardiographic left ventricular hypertrophy[J]. J Hypertens, 2016, 34(9): 1831-1837.
[19] 陶依娆, 杨东辉. P波指数与缺血性脑卒中的研究进展[J]. 中华心律失常学杂志, 2020, 24(4): 425-428. doi: 10.3760/cma.j.cn.113859-20200722-00187
[20] Soeki T, Sata M. Inflammatory Biomarkers and Atherosclerosis[J]. Int Heart J, 2016, 57(2): 134-139. https://www.jstage.jst.go.jp/article/ihj/57/2/57_15-346/_article
[21] 曹建东, 马晓峰, 邓勇, 等. 同型半胱氨酸和C反应蛋白水平与冠状动脉粥样硬化性心脏病患者经皮冠状动脉介入治疗预后的关系研究[J]. 中国医药, 2018, 13(7): 973-976. doi: 10.3760/j.issn.1673-4777.2018.07.004
[22] Afari ME, Bhat T. Neutrophil to lymphocyte ratio(NLR)and cardiovascular diseases: an update[J]. Expert Rev Cardiovasc Ther, 2016, 14(5): 573-577.
[23] 郑佳彦, 杨志明, 王瑑, 等. 红细胞体积分布宽度、中性粒细胞淋巴细胞比值与冠状动脉病变程度及其预后的相关性研究[J]. 中西医结合心脑血管病杂志, 2019, 17(15): 2335-2341. doi: 10.12102/j.issn.1672-1349.2019.15.025
[24] Nam KW, Kwon HM, Jeong HY, et al. High neutrophil to lymphocyte ratios predict intracranial atherosclerosis in a healthy population[J]. Atherosclerosis, 2018, 269: 117-121. https://www.sciencedirect.com/science/article/pii/S0021915017314636
[25] Bressi E, Mangiacapra F, Ricottini E, et al. Impact of Neutrophil-to-Lymphocyte Ratio and Platelet-to-Lymphocyte Ratio on 5-Year Clinical Outcomes of Patients with Stable Coronary Artery Disease Undergoing Elective Percutaneous Coronary Intervention[J]. J Cardiovasc Transl Res, 2018, 11(6): 517-523.
[26] Gecmen C, Candan O, Kahyaoglu M, et al. Echocardiographic assessment of right ventricle free wall strain for prediction of right coronary artery proximal lesion in patients with inferior myocardial infarction[J]. Int J Cardiovasc Imaging, 2018, 34(7): 1109-1116.
[27] Gharacholou SM, Scott CG, Takahashi PY, et al. Left ventricular diastolic function and long-term outcomes in patients with normal exercise echocardiographic findings[J]. Am J Cardiol, 2013, 112(2): 200-207. http://www.pubmedcentral.nih.gov/picrender.fcgi?artid=PMC3706490&blobtype=pdf
[28] Cao ZN, Wang K, Zuo GX, et al. A nomogram to predict major adverse cardiovascular events of patients with acute chest pain, Non-ST-segment deviation, and normal troponin concentrations[J]. Eur Rev Med Pharmacol Sci, 2020, 24(19): 10096-10106.
[29] 余松林. 医学统计学[M]. 北京: 人民卫生出版社, 2004: 65.
-




 下载:
下载: