Clinical characteristics and influencing factors of prognosis in patients with sepsis complicated with acute renal injury
-
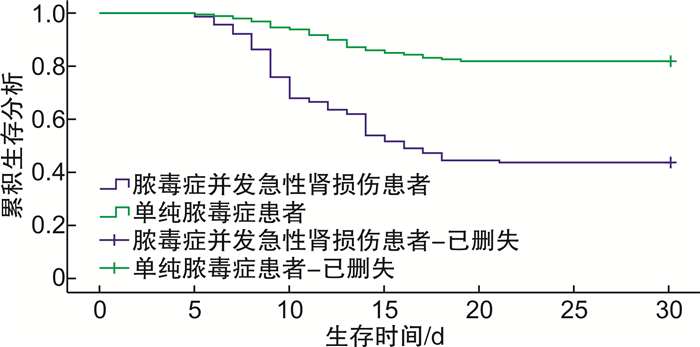
摘要: 目的 观察脓毒症并发急性肾损伤患者临床特征,并分析其预后的影响因素。方法 收集2019年1月-2021年12月我院急诊科312例脓毒症患者的临床资料,将其中发生急性肾损伤的136例患者纳入发生组,将未发生急性肾损伤的176例患者纳入未发生组。观察两组患者临床特征,并分析脓毒症并发急性肾损伤患者预后的影响因素。结果 发生组和未发生组序贯器官衰竭(SOFA)评分、入住ICU时间、总住院时间、机械通气支持率、糖尿病发生率之间进行比较,差异有统计学意义(P< 0.05)。随访1个月,136例脓毒症并发急性肾损伤患者中预后不良78例(57.35%),预后良好58例(42.65%);176例单纯脓毒症患者中预后不良33例(18.75%),预后良好143例(81.25%);预后不良组SOFA评分、Scr、连续性肾替代治疗、机械通气支持与预后良好组比较,差异有统计学意义(P< 0.05);经COX回归分析结果显示,SOFA评分、Scr、机械通气支持是脓毒症并发急性肾损伤患者预后的危险因素(HR> 1,P< 0.05);连续性肾替代治疗是脓毒症并发急性肾损伤患者预后的保护因素(HR< 1,P< 0.05)。结论 脓毒症并发急性肾损伤患者以高SOFA评分、机械通气支持率、糖尿病发生率以及入住ICU时间、总住院时间长为主要临床特征,SOFA评分、Scr、机械通气支持是脓毒症并发急性肾损伤患者预后的危险因素,连续性肾替代治疗是其保护因素。Abstract: Objective To observe the clinical characteristics of patients with sepsis complicated with acute renal injury, and to analyze the influencing factors of prognosis.Methods The clinical data of 312 patients with sepsis in the hospital from January 2019 to December 2021 were collected. One hundred and thirty-six patients with acute renal injury were included in the occurrence group, and 176 patients without acute renal injury were included in the non-occurrence group. The clinical characteristics of patients in the two groups were observed, and the influencing factors of prognosis in patients with sepsis complicated with acute renal injury were analyzed.Results Compared the score of sequential organ failure(SOFA), the time of intensive care unit(ICU), total hospitalization time, mechanical ventilation support and diabetes between the occurrence group and the non occurrence group, the difference was statistically significant(P< 0.05). Among 136 patients with sepsis complicated with acute renal injury, 78 cases(57.35%) had a poor prognosis and 58 cases(42.65%) had a good prognosis. Among 176 patients with simple sepsis, 33 cases(18.75%) had a poor prognosis and 143 cases(81.25%) had a good prognosis; compared SOFA score, Scr, continuous renal replacement therapy and mechanical ventilation support between the poor prognosis group and the good prognosis group, the difference was statistically significant(P< 0.05); through Cox regression analysis, the result showed that SOFA score, Scr and mechanical ventilation support were the risk factors of prognosis in patients with sepsis complicated with acute renal injury(HR> 1,P< 0.05); continuous renal replacement therapy was a protective factor for the prognosis of patients with sepsis complicated with acute renal injury(HR< 1,P< 0.05).Conclusion The main clinical features of patients with sepsis complicated with acute kidney injury are high SOFA score, mechanical ventilation support rate, diabetes incidence, and ICU duration and length of hospitalization time. SOFA score, Scr and mechanical ventilation support are the risk factors of prognosis in patients with sepsis complicated with acute renal injury, and continuous renal replacement therapy is its protective factor.
-
Key words:
- sepsis /
- acute renal injury /
- clinical features /
- prognosis
-

-
表 1 脓毒症并发与未并发急性肾损伤患者临床特征比较
例(%),X±S 临床特征 发生组(136例) 未发生组(176例) χ2/t P 性别 0.286 0.593 男 76(55.88) 93(52.84) 女 60(44.12) 83(47.16) 年龄/岁 70.28±4.76 69.78±4.53 0.947 0.344 SOFA评分/分 10.66±3.47 8.20±3.14 6.550 < 0.001 APACHE Ⅱ评分/分 24.18±4.15 24.58±4.29 0.834 0.405 住ICU时间/d 11.53±2.76 8.15±2.31 11.562 < 0.001 总住院时间/d 15.26±3.18 12.94±2.95 6.060 < 0.001 机械通气支持 10.180 0.001 使用 91(66.91) 86(48.86) 未使用 45(33.09) 90(51.14) 糖尿病 4.300 0.038 有 22(16.18) 15(10.80) 无 114(83.82) 161(89.20) 高血压 0.297 0.586 有 73(53.68) 89(50.57) 无 63(46.32) 87(49.43) 慢性心力衰竭 0.186 0.667 有 25(18.38) 22(11.93) 无 111(81.62) 154(88.07) 血管活性药物使用情况 0.045 0.833 使用 71(52.21) 94(53.41) 未使用 65(47.79) 82(46.59) 肾毒性药物使用 8.153 0.004 使用 33(24.26) 21(11.93) 未使用 103(75.74) 155(88.07) 创伤 6.840 0.009 有 42(30.88) 32(18.18) 无 94(69.12) 144(81.82) 乳酸/(mmol·L-1) 2.81±0.83 2.08±0.61 8.953 < 0.001 白蛋白/(g·dL-1) 2.68±0.91 3.06±1.02 3.419 0.001 降钙素原/(ng·L-1) 21.36±4.86 16.38±4.25 9.638 < 0.001 表 2 预后不良与预后良好组患者临床特征比较
例(%),X±S 临床特征 预后不良组(78例) 预后良好组(58例) χ2/t P 性别 0.021 0.886 男 44(56.41) 32(55.17) 女 34(43.59) 26(44.83) 年龄/岁 70.70±4.81 69.72±4.52 1.191 0.236 SOFA评分/分 11.87±3.47 9.03±3.19 4.893 < 0.001 APACHE Ⅱ评分/分 24.36±4.09 23.94±3.96 0.612 0.542 Scr/(μmol·L-1) 219.45±42.39 196.84±37.62 3.225 0.002 入住ICU时间/d 11.66±2.78 11.36±2.60 0.623 0.535 总住院时间/d 15.02±2.99 15.58±3.02 1.070 0.286 连续性肾替代治疗 13.218 < 0.001 使用 24(30.77) 36(62.07) 未使用 54(69.23) 22(37.93) 机械通气支持 4.582 0.032 使用 58(74.36) 33(56.90) 未使用 20(25.64) 25(43.10) 血管活性药物使用情况 0.197 0.657 使用 42(53.85) 29(50.00) 未使用 36(46.15) 29(50.00) 表 3 主要自变量说明
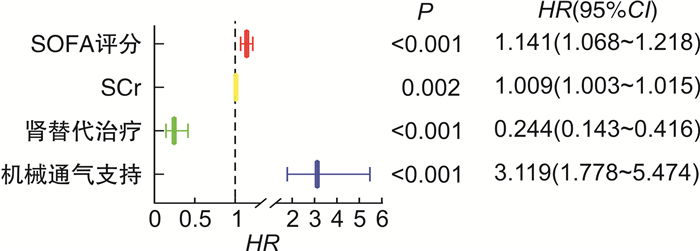
自变量 变量说明 赋值情况 SOFA评分 连续变量 原值输入 Scr 连续变量 原值输入 连续性肾替代治疗 分类变量 1=“使用”, 2=“未使用” 机械通气支持 分类变量 1=“使用”, 2=“未使用” 表 4 脓毒症并发急性肾损伤患者预后COX回归分析
项目 β SE Wald χ2 P HR 95%CI SOFA评分 0.131 0.034 15.208 < 0.001 1.141 1.068~1.218 Scr 0.009 0.003 9.964 0.002 1.009 1.003~1.015 连续性肾替代治疗 -1.412 0.272 26.878 < 0.001 0.244 0.143~0.416 机械通气支持 1.138 0.287 15.719 < 0.001 3.119 1.778~5.474 -
[1] Manrique-Caballero CL, Del Rio-Pertuz G, Gomez H. Sepsis-Associated Acute Kidney Injury[J]. Crit Care Clin, 2021, 37(2): 279-301. doi: 10.1016/j.ccc.2020.11.010
[2] Lelubre C, Vincent JL. Mechanisms and treatment of organ failure in sepsis[J]. Nat Rev Nephrol, 2018, 14(7): 417-427. doi: 10.1038/s41581-018-0005-7
[3] Skube SJ, Katz SA, Chipman JG, et al. Acute Kidney Injury and Sepsis[J]. Surg Infect, 2018, 19(2): 216-224. doi: 10.1089/sur.2017.261
[4] Chen Y, Qiu J L, Chen B, et al. Long non-coding RNA NEAT1 plays an important role in sepsis-induced acute kidney injury by targeting miR-204 and modulating the NF-B pathway[J]. Int Immunopharmacol, 2018, 59: 252-260. doi: 10.1016/j.intimp.2018.03.023
[5] Vijayan A. Tackling AKI: prevention, timing of dialysis and follow-up[J]. Nat Rev Nephrol, 2021, 17(2): 87-88. doi: 10.1038/s41581-020-00390-3
[6] 中国医师协会急诊医师分会, 中国研究型医院学会休克与脓毒症专业委员会, 中国人民解放军总医院第一附属医院创伤研究中心, 等. 中国脓毒症/脓毒性休克急诊治疗指南(2018)[J]. 临床急诊杂志, 2018, 19(9): 567-588. https://www.cnki.com.cn/Article/CJFDTOTAL-ZZLC201809001.htm
[7] 郭锦洲. 改善全球肾脏病预后组织(KDIGO)临床实践指南: 急性肾损伤[J]. 肾脏病与透析肾移植杂志, 2013, 22(1): 57-60. doi: 10.3969/j.issn.1006-298X.2013.01.014
[8] Kotani Y, Fujii T, Uchino S, et al. Modification of sequential organ failure assessment score using acute kidney injury classification[J]. J Crit Care, 2019, 51: 198-203. doi: 10.1016/j.jcrc.2019.02.026
[9] Rowan KM, Kerr JH, Major E, et al. Intensive Care Society's Acute Physiology and Chronic Health Evaluation(APACHE Ⅱ)study in Britain and Ireland: a prospective, multicenter, cohort study comparing two methods for predicting outcome for adult intensive care patients[J]. Crit Care Med, 1994, 22(9): 1392-401. doi: 10.1097/00003246-199409000-00007
[10] 中华医学会糖尿病学分会. 中国2型糖尿病防治指南(2017年版)[J]. 中华糖尿病杂志, 2018, 10(1): 4-67. doi: 10.3760/cma.j.issn.1674-5809.2018.01.003
[11] 中国高血压基层管理指南修订委员会. 中国高血压基层管理指南(2014年修订版)[J]. 中华高血压杂志, 2015, 23(1): 24-43. https://www.cnki.com.cn/Article/CJFDTOTAL-ZGGZ201501010.htm
[12] 中华医学会, 中华医学会杂志社, 中华医学会全科医学分会, 等. 慢性心力衰竭基层诊疗指南(实践版·2019)[J]. 中华全科医师杂志, 2019, 18(10): 948-956. doi: 10.3760/cma.j.issn.1671-7368.2019.10.009
[13] 金魁, 王玉兰, 汪跃国, 等. 不同感染部位脓毒症急性肾损伤发生率及相关死亡风险分析[J]. 临床急诊杂志, 2021, 22(7): 445-452. https://www.cnki.com.cn/Article/CJFDTOTAL-ZZLC202107002.htm
[14] 陈秀凯, 李文雄. 急性肾损伤的研究进展与回顾[J]. 中国急救医学, 2014, 34(2): 111-115. doi: 10.3969/j.issn.1002-1949.2014.02.005
[15] 盛松, 张艳虹, 马杭琨, 等. 查尔森合并症指数对合并急性肾损伤并接受连续肾脏替代治疗的脓毒症患者死亡风险的评估价值[J]. 临床急诊杂志, 2021, 22(11): 764-771. https://www.cnki.com.cn/Article/CJFDTOTAL-ZZLC202111012.htm
[16] Liu J, Xie H, Ye Z, et al. Rates, predictors, and mortality of sepsis-associated acute kidney injury: a systematic review and meta-analysis[J]. BMC Nephrol, 2020, 21(1): 318-334.
[17] Lambden S, Laterre PF, Levy MM, et al. The SOFA score-development, utility and challenges of accurate assessment in clinical trials[J]. Crit Care, 2019, 23(1): 374.
[18] 欧阳秀梅, 刘常青, 徐金艳. 连续性肾脏替代治疗脓毒症合并急性肾损伤的预后危险因素[J]. 吉林医学, 2022, 43(2): 488-490. doi: 10.3969/j.issn.1004-0412.2022.02.079
[19] Nakashima T, Miyamoto K, Shimokawa T, et al. The Association Between Sequential Organ Failure Assessment Scores and Mortality in Patients With Sepsis During the First Week: The JSEPTIC DIC Study[J]. J Intensive Care Med, 2020, 35(7): 656-662.
[20] 岳英丽, 陈珊珊, 韩斌. ALR、β2-MG联合Scr对重症急性胰腺炎合并急性肾损伤的早期预测价值[J]. 广西医科大学学报, 2019, 36(8): 1309-1313. https://www.cnki.com.cn/Article/CJFDTOTAL-GXYD201908022.htm
[21] 郭玉红, 戴浩然, 刘清泉. 脓毒症急性肾损伤相关因素分析[J]. 世界中医药, 2017, 12(4): 725-727. https://www.cnki.com.cn/Article/CJFDTOTAL-SJZA201704002.htm
[22] 刘莉, 刘名鑫, 牛世慧, 等. 脓毒症并发急性肾损伤患者肾功能衰竭的影响因素[J]. 中华医院感染学杂志, 2021, 31(20): 3078-3081. https://www.cnki.com.cn/Article/CJFDTOTAL-ZHYY202120009.htm
[23] 王敏佳, 龚仕金, 徐靓, 等. 持续肾脏替代治疗启动后液体平衡对脓毒症急性肾损伤患者预后的影响[J]. 浙江医学, 2020, 42(7): 726-729. https://www.cnki.com.cn/Article/CJFDTOTAL-ZJYE202007024.htm
[24] Lin J, Ji XJ, Wang AY, et al. Timing of continuous renal replacement therapy in severe acute kidney injury patients with fluid overload: A retrospective cohort study[J]. J Crit Care, 2021, 35(64): 226-236.
[25] Harvey AK, Burns K, Mcarthur E, et al. Short-and long-term outcomes of sustained low efficiency dialysis vs continuous renal replacement therapy in critically ill patients with acute kidney injury[J]. J Crit Care, 2021, 35(62): 76-81.
[26] Bento HA, Mayer KP. Active Mobilization for Patients Requiring Continuous Renal Replacement Therapy: Let Us Get Moving[J]. Crit Care Med, 2021, 49(1): e117-e118.
-




 下载:
下载: