The predictive value of oxygen index and alkaline excess in non-external membrane oxygenation treatment of neonatal acute respiratory distress syndrome prognosis
-
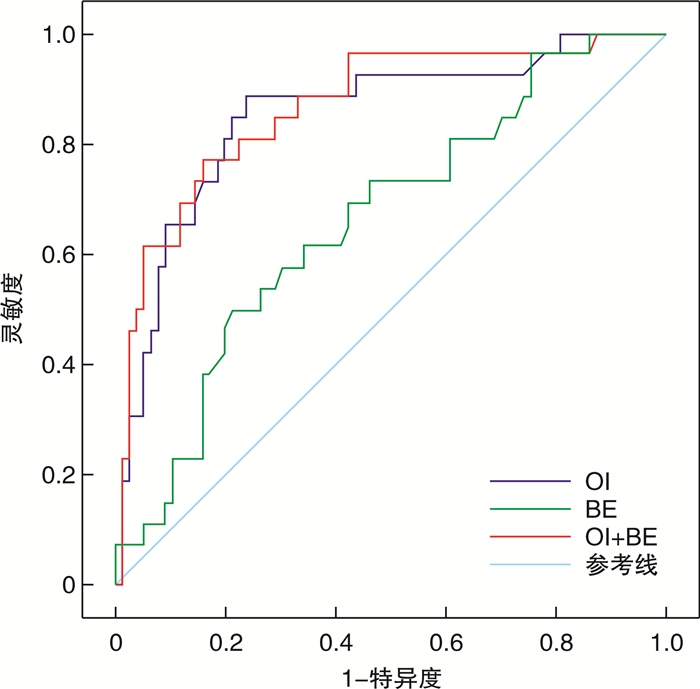
摘要: 目的 分析氧指数(OI)和碱剩余(BE)对非体外膜氧合(ECMO)治疗新生儿急性呼吸窘迫综合征(ARDS)预后的预测价值。方法 选取2016年7月—2021年7月收治的非ECMO治疗的ARDS新生儿为研究对象,记录患儿的人口学及临床检验指标,根据患儿出院前是否死亡分为存活组和死亡组。采用多因素logistic回归统计非ECMO治疗的ARDS患儿各指标与其病死率的相关性,分析各影响因素对病死率的预测价值。结果 共纳入103例患儿,存活组患儿77例,死亡组患儿26例,2组在性别、分娩方式、OI、血液酸碱度(PH)、BE方面比较差异有统计学意义(P<0.05)。受试者工作特征曲线(ROC)分析表明,OI和BE结合在预测患儿预后的能力上优于其他变量。OI和BE结合预测患儿预后的曲线下面积(AUC)为0.865。当OI>30 mmHg和BE<-7.40 mmol/L时,预测患儿死亡的灵敏度和特异度分别为77.0%和84.0%。结论 OI和BE相结合可作为非ECMO治疗的ARDS新生儿病死率的预测指标,OI>30 mmHg和BE<-7.40 mmol/L可作为选择ECMO治疗的重要依据之一。Abstract: Objective To analyze the predictive value of oxygen index(OI) and alkaline excess(BE) on the prognosis of non-external membrane oxygenation(ECMO) in the treatment of neonatal acute respiratory distress syndrome(ARDS).Methods The neonates with ARDS who were not treated with ECMO in our hospital from July 2016 to July 2021 were selected.The demographic and clinical test indicators of the neonates were recorded.The neonates were divided into two groups according to whether theywere survival at discharge. Multivariate logistic regression was used to analyze the correlation between the clinical indicators of non-ECMO-treated ARDS neonates and their mortality, and to analyze the predictive value of each influence factor on mortality.Results A total of 103 neonates were included, 77 neonates survived at discharge, and 26 children died. There were statistically significant differences between the two groups in terms of gender, delivery method, OI, PH, and BE(P < 0.05). Receiver operating characteristic curve(ROC) analysis shows that the combination of OI and BE is superior to other variables in predictive ability. The area under the combined curve of OI and BE(AUC) is 0.865. When OI>30 mmHg and BE < -7.40 mmol/L, the sensitivity and specificity of predicting death were 77.0% and 84.0%, respectively.Conclusion The combination of OI and BE can be used as a predictor of non-ECMO treatment of neonatal ARDSmortality. OI>30 mmHg and BE < -7.40 mmol/L can be considered as one of the important evidences for the selection of ECMO treatment.
-
Key words:
- acute respiratory distress syndrome /
- neonates /
- oxygen index /
- alkaline excess /
- predictive value
-

-
表 1 2组患儿临床资料比较
例,M(Q1, Q3),X±S 临床资料 存活组(n=77) 死亡组(n=26) Z/χ2 P 性别 男 54 11 6.462 0.011 女 23 15 分娩方式 阴道分娩 14 10 4.473 0.034 剖宫产 63 16 年龄/d 8.00(4.00,19.00) 6.00(4.75,11.25) -1.214 0.225 出生体重/g 3 269.61±533.32 3 165.77±572.91 0.843 0.401 OI/mmHg 22.25(18.00,29.78) 40.00(32.53,62.78) -5.306 <0.001 PH 7.31(7.24,7.37) 7.20(7.12,7.34) -2.184 0.029 PaCO2/mmHg 43.00(38.00,50.50) 39.00(35.00,54.50) -0.589 0.556 BE/(mmol·L-1) -4.40(-7.00,-1.20) -7.15(-9.78,-3.48) -2.437 0.015 Lac/(mmol·L-1) 4.15(2.80,5.10) 4.79(2.68,7.75) -1.207 0.228 表 2 ARDS患儿死亡的多因素分析
因素 β SE Wald χ2 P OR(95%CI) 性别 -0.026 0.014 3.591 0.058 0.974(0.949~1.001) 分娩方式 -1.657 1.029 2.592 0.107 0.191(0.025~1.434) OI 1.562 0.693 5.085 0.024 4.770(1.227~18.546) PH -0.087 0.025 12.146 <0.001 0.917(0.873~0.963) BE 1.943 0.493 15.556 <0.001 6.982(2.658~18.340) -
[1] 刘慧, 程伟, 伍莉, 等. 新生儿急性呼吸窘迫综合征的临床特征及预后相关性分析[J]. 医学研究杂志, 2020, 49(12): 79-82, 108-108. https://www.cnki.com.cn/Article/CJFDTOTAL-YXYZ202012023.htm
[2] 张永芳, 于新桥, 廖建华, 等. 鄂西南地区新生儿急性呼吸窘迫综合征临床流行病学调查[J]. 中国当代儿科杂志, 2020, 22(9): 942-947. https://www.cnki.com.cn/Article/CJFDTOTAL-DDKZ202009005.htm
[3] 马俊苓, 刘鸽, 王晓鹏, 等. 不同水平呼气末正压对新生儿急性呼吸窘迫综合征的疗效及血流动力学的影响[J]. 中国现代医学杂志, 2020, 30(16): 85-88. doi: 10.3969/j.issn.1005-8982.2020.16.017
[4] 邹远霞, 张家瑜, 周波, 等. 新生儿急性呼吸窘迫综合征诊疗研究进展[J]. 医学研究杂志, 2021, 50(3): 129-132. doi: 10.3877/cma.j.issn.1674-1366.2021.03.001
[5] Khalesi N, Choobdar FA, Khorasani M, et al. Accuracy of oxygen saturation index in determining the severity of respiratory failure among preterm infants with respiratory distress syndrome[J]. J Matern Fetal Neonatal Med, 2021, 34(14): 2334-2339. doi: 10.1080/14767058.2019.1666363
[6] 中国医师协会新生儿科医师分会. "新生儿急性呼吸窘迫综合征"蒙特勒标准(2017年版)[J]. 中华实用儿科临床杂志, 2017, 32(19): 1456-1458. doi: 10.3760/cma.j.issn.2095-428X.2017.19.004
[7] 刘慧, 伍莉, 吴芳, 等. 新生儿急性呼吸窘迫综合征的母孕期高危因素分析[J]. 重庆医学, 2021, 50(1): 54-57, 62-62. doi: 10.3969/j.issn.1671-8348.2021.01.012
[8] 谈林华, 杜立中. 儿童急性肺损伤与急性呼吸窘迫综合征的机械通气治疗进展[J]. 中华儿科杂志, 2011, 49(1): 34-37. https://www.cnki.com.cn/Article/CJFDTOTAL-ZJJY200804026.htm
[9] Maca J, Jor O, Holub M, et al. Past and Present ARDS Mortality Rates: A Systematic Review[J]. Respir Care, 2017, 62(1): 113-122. doi: 10.4187/respcare.04716
[10] Fletcher K, Chapman R, Keene S. An overview of medical ECMO for neonates[J]. Semin Perinatol, 2018, 42(2): 68-79. doi: 10.1053/j.semperi.2017.12.002
[11] 邱志磊, 张思泉, 周可幸, 等. 新型冠状病毒肺炎患者肺部CT征象与生化指标和氧合指数的相关性分析[J]. 江苏医药, 2020, 46(9): 908-912. https://www.cnki.com.cn/Article/CJFDTOTAL-YIYA202009013.htm
[12] Hammond BG, Garcia-Filion P, Kang P, et al. Identifying an Oxygenation Index Threshold for Increased Mortality in Acute Respiratory Failure[J]. Respir Care, 2017, 62(10): 1249-1254. doi: 10.4187/respcare.05092
[13] Trachsel D, McCrindle BW, Nakagawa S, et al. Oxygenation index predicts outcome in children with acute hypoxemic respiratory failure[J]. Am J Respir Crit Care Med, 2005, 172(2): 206-211. doi: 10.1164/rccm.200405-625OC
[14] 张立涛, 郝清卿, 赵静, 等. 乳酸碱剩余对早期重症社区获得性肺炎患者肾功能的评估[J]. 临床急诊杂志, 2020, 21(6): 470-473. http://zzlc.cbpt.cnki.net/WKC/WebPublication/paperDigest.aspx?paperID=939baced-f37b-4d84-9738-c86d447f82bc
[15] 黄四云, 丘文凤, 罗伟文. 乳酸清除率联合剩余碱评估失血性低血容量休克患者预后的价值分析[J]. 检验医学与临床, 2017, 14(9): 1280-1281, 1284-1284. https://www.cnki.com.cn/Article/CJFDTOTAL-JYYL201709029.htm
[16] Ghuman AK, Newth CJ, Khemani RG. The association between the end tidal alveolar dead space fraction and mortality in pediatric acute hypoxemic respiratory failure[J]. Pediatr Crit Care Med, 2012, 13(1): 11-15. doi: 10.1097/PCC.0b013e3182192c42
[17] Lee CU, Jo YH, Lee JH, et al. The index of oxygenation to respiratory rate as a prognostic factor for mortality in Sepsis[J]. Am J Emerg Med, 2021, 45: 426-432. doi: 10.1016/j.ajem.2020.09.052
[18] Rowan CM, Hege KM, Speicher RH, et al. Oxygenation index predicts mortality in pediatric stem cell transplant recipients requiring mechanical ventilation[J]. Pediatr Transplant, 2012, 16(6): 645-650. doi: 10.1111/j.1399-3046.2012.01745.x
-




 下载:
下载: