Early predictive value of serum lactate dehydrogenase level for the short-term prognosis in wasp stings
-
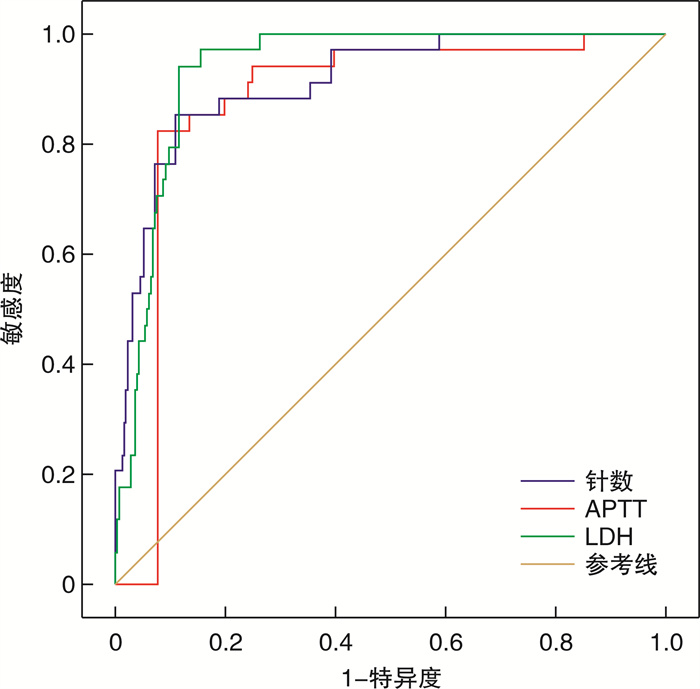
摘要: 目的 探讨乳酸脱氢酶(LDH)水平对胡蜂螫伤短期预后的早期预测价值。方法 回顾性分析2016年1月1日-2020年12月31日期间十堰市太和医院收治的312例胡蜂螫伤患者的临床资料。根据入院首次(24 h内)LDH水平分为LDH正常组(≤240 U/L)和LDH升高组(>240 U/L)。比较2组患者的各项临床指标及28 d存活情况。统计学分析采用独立样本t检验,Kruskal-Wallis非参数检验和χ2检验。采用logistic回归分析影响短期预后的因素,采用受试者操作特征曲线下面积(AUC)评价相关因素对28 d病死率的预测价值。结果 312例中轻型86例(27.6 %),中型92例(29.5%),重型134例(42.9%)。随访28 d存活278例,死亡34例,28 d病死率为10.9%。血清LDH正常141例(45.2%),LDH升高171例(54.8%)。LDH升高组进展为重症及死亡的比例分别为69.59%、19.88%,而LDH正常组仅为13.48%、0,差异具有统计学意义(P < 0.05)。除血小板计数外,两组年龄、针数、白细胞计数、红细胞、血红蛋白、肝肾功能及凝血功能和心肌酶谱均差异有统计学意义(P < 0.05)。同时两组患者性别、尿色、溶血发生例数、28 d死亡例数以及对血制品使用、血液净化、气管插管和机械通气使用例数上均差异有统计学意义(P < 0.05)。进行logistic单因素回归分析结果显示螫伤针数、T-bil、APTT、CK和LDH与患者预后有关。进一步进行多因素logistic回归分析结果显示针数、APTT和LDH仍然具有独立预测能力。针数预测胡蜂螫伤28 d死亡的AUC为0.912,最佳界值为0.738,敏感度为0.853,特异度为0.885,Cut-off为38针;LDH预测胡蜂螫伤28 d死亡的AUC为0.935,最佳界值为0.826,敏感度为0.941,特异度为0.885,Cut-off为1536 U/L;APTT预测胡蜂螫伤28 d死亡的AUC为0.875,最佳界值为0.716,敏感度为0.853,特异度为0.863,Cut-off为100 s。结论 LDH是早期评估胡蜂螫伤病情严重程度和短期预后的良好生物标志物,血清LDH升高可早期预测28 d死亡。Abstract: Objective To explore the early predictive value of lactate dehydrogenase(LDH) level on the prognosis of wasp stings.Methods The clinical data of 312 wasp stings in taihe hospital from January 1, 2016 to December 31, 2020 were analyzed retrospectively. Patients were divided into LDH normal group(≤240 U/L) and LDH elevated group(>240 U/L) according to lactate dehydrogenase level at the first admission(within 24 hours). The clinical indexes of the two groups were compared. Statistical analysis used independent sample t-test, Kruskal-Wallis nonparametric test and χ2 test. Logistic regression was used to analyze the prognostic factors, and AUC was used to evaluate the predictive value of related factors on 28-day mortality.Results Among 312 cases, 86 cases were mild(27.6%), 92 cases were moderate(29.5%) and 134 cases were severe(42.9%). 278 cases survived and 34 cases died after 28 days of follow-up, with a mortality rate of 10.9%. Serum LDH was normal in 141 cases(45.2%) and elevated in 171 cases(54.8%). The rates of severe and death in the elevated LDH group were 69.59% and 19.88% respectively, while those in the normal LDH group were only 13.48% and 0(P < 0.05). In addition to platelet count, there were significant differences in age, needle count, white blood cell count, red blood cell, hemoglobin, liver and kidney function, coagulation function and myocardial enzyme spectrum between the two groups(P < 0.05). At the same time, there were significant differences in gender, urine color, hemolysis cases, 28-day death cases, blood products use, blood purification, endotracheal intubation and mechanical ventilation between the two groups(P < 0.05). Logistic regression analysis showed that the number of stinging needles, T-bil, APTT, CK and LDH were related to the prognosis of patients. Further multivariate logistic regression analysis showed that needle number, APTT and LDH still had independent predictive ability. AUC, which predicted the death of wasp stinging for 28 days, was 0.912, with the best cut-off value of 0.738, sensitivity of 0.853, specificity of 0.885, and cut-off of 38 needles. AUC, the best limit value, sensitivity, specificity, and cut-off of 28 days after sting, was 0.935, 0.826, 0.941, 0.885, and 1536 u/l respectively. The AUC of APTT for predicting the death of wasps after stinging for 28 days is 0.875, the best cut-off value is 0.716, the sensitivity is 0.853, the specificity is 0.863, and the cut-off time is 100 seconds.Conclusion Elevated LDH is a sign of hemolysis and serious illness of wasp stings, and it is a good biomarker for early evaluation of the prognosis of wasp stings.
-
Key words:
- wasp stings /
- lactate dehydrogenase /
- prognosis
-

-
表 1 LDH正常组与LDH升高组患者的实验室检查指标比较
M(Q1,Q3) 临床指标 LDH正常组(141例) LDH升高组(171例) z P 年龄/岁 43.0(25.0,52.5) 50.0(23.0,60.0) -2.461 0.014 针数/针 7.0(3.0,15.0) 30.0(12.0,45.0) -9.434 <0.001 WBC/(×109·L-1) 10.5(8.3,14.7) 18.7(13.3,24.8) -9.168 <0.001 RBC/(×1012·L-1) 4.5(4.1,4.8) 4.1(3.6,4.6) -5.148 <0.001 Hb/(g·L-1) 132.0(123.0,146.0) 126.0(108.0,138.0) -4.232 <0.001 PLT/(×109·L-1) 213.0(170.5,256.5) 211.0(157.0,258.0) -0.841 0.400 T-bil/(μmol·L-1) 13.9(9.6,21.1) 50.4(20.1,95.2) -9.236 <0.001 U-bil/(μmol·L-1) 9.8(6.4,14.3) 38.8(14.0,70.4) -9.251 <0.001 ALT/(U·L-1) 17.0(12.0,25.0) 87.0(31.0,384.0) -11.505 <0.001 AST/(U·L-1) 25.0(19.5,32.0) 313.0(67.0,947.0) -13.721 <0.001 BUN/(mmol·L-1) 5.2(3.9,6.3) 8.2(5.2,13.2) -7.595 <0.001 Cr/(μmol·L-1) 78.9(67.8,90.8) 84.2(60.7,168.1) -2.170 0.030 PT/s 11.7(10.8,12.7) 13.1(11.5,15.3) -5.356 <0.001 APTT/s 33.4(28.9,50.0) 58.0(32.6,120.0) -5.281 <0.001 CK/(U·L-1) 122.0(82.5,216.0) 2060.0(567.0,7669.0) -12.752 <0.001 CK-MB/(U·L-1) 13.0(9.0,20.0) 106.0(39.0,273.0) -13.122 <0.001 LDH/(U·L-1) 185.000(162.0,210.0) 1086.000(425.0,2468.0) -15.202 <0.001 表 2 LDH正常组与LDH升高组患者的临床指标比较
例(%) 临床指标 LDH正常组 LDH升高组 总计 χ2 P 性别 男 94(66.67) 90(52.63) 184(58.97) 6.292 0.012 女 47(33.33) 81(47.37) 128(41.03) 尿色 黄色 138(97.87) 66(38.60) 204(65.38) 119.97 P<0.001 血色或酱油色 3(2.13) 105(61.40) 108(34.62) 溶血 是 19(13.48) 119(69.59) 138(44.23) 98.652 P<0.001 否 122(86.52) 52(30.41) 174(55.77) 转归 存活 141(100.00) 137(80.12) 278(89.10) 31.464 P<0.001 死亡 0(0) 34(19.88) 34(10.90) 血液制品 是 18(12.77) 62(36.26) 80(25.64) 22.367 P<0.001 否 123(87.23) 109(63.74) 232(74.36) 血液净化 是 8(5.67) 59(34.50) 67(21.47) 38.088 P<0.001 否 133(94.33) 112(65.50) 245(78.53) 气管插管 是 2(1.42) 36(21.05) 38(12.18) 27.852 P<0.001 否 139(98.58) 135(78.95) 274(87.82) 使用呼吸机 是 2(1.42) 34(19.88) 36(11.54) 25.813 P<0.001 否 139(98.58) 137(80.12) 276(88.46) 表 3 单因素及多因素logistic回归分析胡蜂螫伤28d病死率影响因素
因素 单因素 多因素 OR OR95%CI P OR OR95%CI P 性别 0.362 0.091~1.445 0.15 针数 0.941 0.904~0.979 0.003 0.936 0.903~0.971 P<0.001 尿色 0 0.000~null 1.000 溶血 0 0.000~null 0.986 血液制品 2.966 0.409~21.491 0.282 血液净化 0.662 0.151~2.905 0.585 气管插管 0.198 0.009~4.435 0.307 机械通气 0.077 0.005~1.170 0.065 WBC 0.965 0.882~1.056 0.436 RBC 5.439 0.885~33.428 0.068 Hb 0.966 0.925~1.008 0.111 PLT 0.994 0.984~1.004 0.218 Alb 1.16 0.982~1.371 0.081 T-bil 0.973 0.949~0.998 0.032 0.998 0.987~1.008 0.640 U-bil 1.027 0.992~1.063 0.128 ALT 1.001 0.999~1.002 0.34 AST 1 0.999~1.000 0.718 BUN 0.923 0.773~1.102 0.376 Cr 0.999 0.992~1.006 0.745 PT 0.968 0.872~1.074 0.538 APTT 0.93 0.892~0.970 0.001 0.948 0.924~0.972 P<0.001 CK 1.000~1.000 0.007 1.000 1.000~1.000 0.653 CK-MB 1.000~1.001 0.426 LDH 0.999 0.998~1.000 0.005 0.999 0.999~1.000 P<0.001 -
[1] Xie C, Xu S, Ding F, et al. Clinical features of severe wasp sting patients with dominantly toxic reaction: analysis of 1091 cases[J]. PLoS One, 2013, 8(12): e83164. doi: 10.1371/journal.pone.0083164
[2] 王文明, 朱贞祥, 程桐花, 等. 中性粒细胞比率联合乳酸脱氢酶对急性胰腺炎严重程度的早期预测价值[J]. 临床急诊杂志, 2022, 23(1): 11-14. https://www.cnki.com.cn/Article/CJFDTOTAL-ZZLC202201003.htm
[3] 李俊玉, 王雅慧, 刘慧珍, 等. 红细胞分布宽度与血小板计数比值对急诊脓毒症患者预后的预测价值[J]. 临床急诊杂志, 2022, 23(2): 132-137. https://www.cnki.com.cn/Article/CJFDTOTAL-ZZLC202202011.htm
[4] Feng Y, Xiong Y, Qiao T, et al. Lactate dehydrogenase A: A key player in carcinogenesis and potential target in cancer therapy[J]. Cancer Med, 2018, 7(12): 6124-6136. doi: 10.1002/cam4.1820
[5] Lu J, Wei Z, Jiang H, et al. Lactate dehydrogenase is associated with 28-day mortality in patients with sepsis: a retrospective observational study[J]. J Surg Res, 2018, 228: 314-321. doi: 10.1016/j.jss.2018.03.035
[6] You YH, In YN, Park JS, et al. Relationships between serum levels of lactate dehydrogenase and neurological outcomes of patients who underwent targeted temperature management after out-of-hospital cardiac arrest[J]. Medicine(Baltimore), 2021, 100(24): e26260.
[7] Szarpak L, Ruetzler K, Safiejko K, et al. Lactate dehydrogenase level as a COVID-19 severity marker[J]. Am J Emerg Med, 2021, 45: 638-639. doi: 10.1016/j.ajem.2020.11.025
[8] 中国毒理学会中毒与救治专业委员会, 中华医学会湖北省急诊医学分会, 湖北省中毒与职业病联盟. 胡蜂螫伤规范化诊治中国专家共识[J]. 中华危重病急学, 2018, 30(9): 819-823. https://cpfd.cnki.com.cn/Article/CPFDTOTAL-ZGDV201811001015.htm
[9] Wu Y, Lu C, Pan N, et al. Serum lactate dehydrogenase activities as systems biomarkers for 48 types of human diseases[J]. Sci Rep, 2021, 11(1): 12997. doi: 10.1038/s41598-021-92430-6
[10] Wang M, Prince S, Tang Y, et al. Macroscopic hematuria in wasp sting patients: a retrospective study[J]. Ren Fail, 2021, 43(1): 500-509. doi: 10.1080/0886022X.2021.1896547
[11] Tang X, Lin L, Yang YY, et al. Development and validation of a model to predict acute kidney injury following wasp stings: A multicentre study[J]. Toxicon, 2022, 209: 43-49. doi: 10.1016/j.toxicon.2022.02.003
[12] Zhang D, Shi L. Serum lactate dehydrogenase level is associated with in-hospital mortality in critically Ill patients with acute kidney injury[J]. Int Urol Nephrol, 2021, 53(11): 2341-2348. doi: 10.1007/s11255-021-02792-z
[13] Su D, Li J, Ren J, et al. The relationship between serum lactate dehydrogenase level and mortality in critically ill patients[J]. Biomark Med, 2021, 15(8): 551-559. doi: 10.2217/bmm-2020-0671
[14] 席秋萍, 陈宗英, 方文燕, 等. 蜂蛰伤中毒致急性肾损伤的相关危险因素调查[J]. 中华劳动卫生职业病杂志, 2018, 36(2): 106-109. https://cdmd.cnki.com.cn/Article/CDMD-10632-1017179871.htm
[15] 闫云云, 肖雪, 邹林林, 等. 贵州省遵义地区胡蜂蛰伤致凝血功能障碍的临床特点以及APTT水平与胡蜂蜇伤病情严重程度的相关性分析[J]. 中华急诊医学杂志, 2018, 27(8): 920-922.
-




 下载:
下载: