Value of combined detection of serum CST and Gal-3 in evaluating short-term prognosis of patients with acute decompensated heart failure after discharge
-
摘要: 目的 探讨血清儿茶酚抑素(CST)、半乳糖凝集素-3(Gal-3)联合检测对急性失代偿性心力衰竭(ADHF)患者出院后短期预后的评估价值。方法 采用前瞻性研究方法,选择2019年1月5日-2021年8月30日期间我院收治的ADHF患者为病例组,另选择同期在我院体检健康的志愿者98例为对照组,对比病例组患者入院时、对照组体检时血清CST、Gal-3水平。根据患者出院后30 d内是否出现不良事件将其分为预后不良组(因心力衰竭再入院或全因死亡)与预后良好组,对比预后不良组、预后良好组患者的临床资料、实验室指标和入院时血清CST、Gal-3水平,分析ADHF患者出院后短期内发生不良事件的危险因素,分析部分指标及联合检测对ADHF患者出院后短期内发生不良事件的预测价值。结果 病例组患者入院时血清CST、Gal-3水平显著高于对照组(P < 0.05);预后不良组患者的美国纽约心脏病学会(NYHA)心功能分级Ⅳ级比例及血清N末端B型利钠肽原(NT-proBNP)、CST、Gal-3水平均显著高于预后良好组(P < 0.05),左心室射血分数(LVEF)显著低于预后良好组(P < 0.05)。Logistic回归分析显示,LVEF降低、NT-proBNP升高、CST升高、Gal-3升高是患者出院后短期内不良事件发生的危险因素(P < 0.05)。受试者工作特征(ROC)曲线分析显示,联合检测患者出院后短期内发生不良事件的曲线下面积(AUC)为0.859、敏感度为0.833,特异度为0.883。结论 血清CST和Gal-3是ADHF患者出院后短期不良预后的危险因素,检测入院时血清CST、Gal-3水平有助于预测患者出院后短期不良预后,联合检测的预测价值更高。
-
关键词:
- 儿茶酚抑素 /
- 半乳糖凝集素-3 /
- 急性失代偿性心力衰竭 /
- 预后
Abstract: Objective To investigate the value of combined detection of serum catechinstatin(CST) and galectin-3(Gal-3) in evaluating short-term prognosis of patients with acute decompensated heart failure(ADHF) after discharge.Methods Using the prospective research method, patients with ADHF treated in the people's hospital of Inner Mongolia Autonomous Region from January 5, 2019 to August 30, 2021 were selected as the case group, and 98 healthy volunteers who underwent physical examination in our hospital in the same period were included in the control group. The levels of serum CST and Gal-3 in the case group at admission and in the control group at physical examination were compared. According to whether there were adverse events within 30 days after discharge, the patients were divided into poor prognosis group(readmission due to heart failure or all-cause death) and good prognosis group. The clinical data, laboratory indexes, serum CST and Gal-3 levels at admission of patients in poor prognosis group and good prognosis group were compared, the risk factors of adverse events in a short time after discharge of ADHF patients were analyzed, and the serum CST The predictive value of Gal-3 level for adverse events in the short term after discharge in patients with ADHF.Results The levels of serum CST and Gal-3 in the case group at admission were significantly higher than those in the control group(P < 0.05). The proportion of New York Heart Association(NYHA) cardiac function classification was grade IV and the levels of serum N-terminal pro-B-type natriuretic peptide(NT-proBNP), CST and Gal-3 in the poor prognosis group were significantly higher than those in the good prognosis group(P < 0.05), and the left ventricular ejection fraction(LVEF) was significantly lower than that in the good prognosis group(P < 0.05). logistic regression analysis showed that the decrease of LVEF, the increase of NT-proBNP, CST, Gal-3 were the risk factors of adverse events in the short term of patients(P < 0.05). The receiver operating characteristic(ROC) curve analysis showed that the area under curve(AUC) of combined prediction for short-term adverse events after discharge was 0.859, the sensitivity was 0.833, and the specificity was 0.883.Conclusion Serum CST and Gal-3 are risk factors for short-term poor prognosis in patients with ADHF after discharge. Detecting the levels of serum CST and Gal-3 at admission is helpful to predict the short-term poor prognosis after discharge, and the predictive value of combined detection is higher.-
Key words:
- catecholastatin /
- galectin-3 /
- acute decompensated heart failure /
- prognosis
-

-
表 1 两组临床资料、实验室指标和血清CST、Gal-3水平比较
例(%) 指标 预后良好组(77例) 预后不良组(48例) t(χ2) P 年龄/岁 61.09±5.03 61.86±5.28 1.110 0.268 BMI 22.56±3.19 22.79±3.24 0.531 0.596 性别 (0.016) 0.899 男 41(53.25) 25(52.08) 女 36(46.75) 23(29.87) 吸烟史 (0.780) 0.376 有 23(29.87) 18(37.50) 无 54(70.13) 30(62.50) 高脂血症史 (0.047) 0.827 有 32(41.56) 19(40.63) 无 45(58.44) 29(59.37) 高血压史 (0.485) 0.486 有 45(58.44) 25(52.08) 无 32(41.56) 23(29.87) 糖尿病史 (0.094) 0.758 有 31(40.26) 18(37.50) 无 46(59.74) 30(62.50) NYHA心功能分级 (7.323) 0.007 Ⅲ级 54(70.13) 22(45.83) Ⅳ级 23(29.87) 26(54.17) 应用β受体阻滞剂 (0.351) 0.553 是 49(63.64) 28(58.33) 否 28(36.36) 20(41.67) 应用ARB或ACEI (0.645) 0.422 是 55(71.43) 31(64.58) 否 22(28.57) 17(35.42) 应用利尿剂 (0.180) 0.671 是 51(66.23) 30(62.50) 否 26(33.77) 18(37.50) 应用醛固酮 (0.781) 0.377 是 54(70.13) 30(62.50) 否 23(29.87) 18(37.50) 住院时间/d 12.57±2.36 13.14±2.21 1.345 0.181 LVEF/% 52.79±6.24 40.82±4.03 11.831 < 0.001 白细胞/(×109·L-1) 8.09±1.14 8.42±1.23 1.527 0.129 血红蛋白/(g·L-1) 125.27±17.29 129.15±18.36 1.192 0.236 C反应蛋白/(mg·L-1) 61.28±6.07 61.59±5.82 0.282 0.778 NT-proBNP/(ng·L-1) 2 253.18±247.86 3 189.61±526.57 13.423 < 0.001 CST/(ng·mL-1) 4.93±1.19 8.45±1.62 13.968 < 0.001 Gal-3/(ng·mL-1) 12.42±2.39 26.51±3.68 25.969 < 0.001 注:ARB、ACEI为血管紧张素转换酶抑制剂。 表 2 ADHF患者出院后短期内发生不良事件的logistic回归分析
指标 赋值 β SE Wald χ2 P OR OR 95%CI 常数 -0.203 0.106 3.668 0.055 NYHA心功能分级 1:Ⅳ级,0:Ⅲ级 0.301 0.403 0.557 0.455 1.351 0.613~2.976 LVEF 1:≥50%,0:<50% -0.962 0.275 12.254 < 0.001 0.382 0.223~0.655 NT-proBNP 1:≥2700 ng/L,0:<2700 ng/L 1.065 0.286 13.842 < 0.001 2.901 1.655~5.084 CST 1:≥6 ng/mL,0:<6 ng/mL 0.723 0.259 7.784 0.005 2.061 1.240~3.426 Gal-3 1:≥20 ng/mL,0:<20 ng/mL 1.276 0.363 12.370 < 0.001 3.582 1.759~7.293 表 3 各指标预测ADHF患者出院后发生短期不良预后的ROC曲线分析
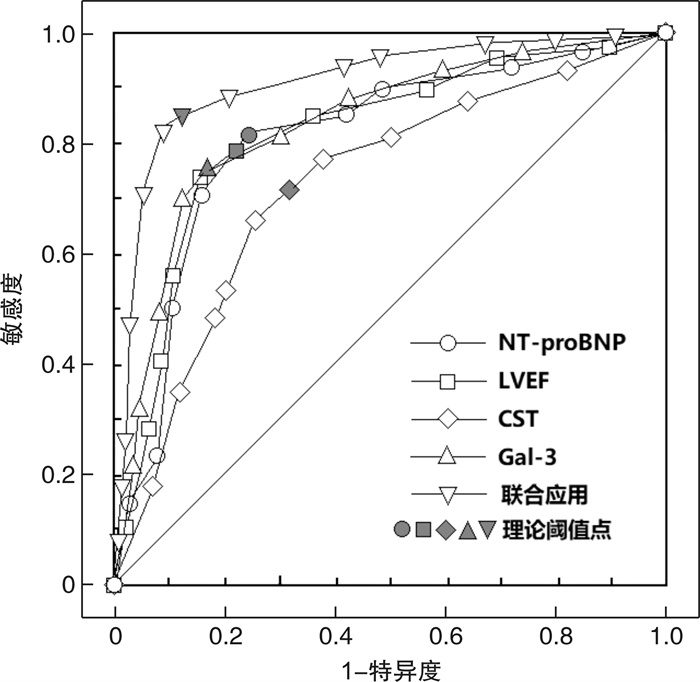
指标 AUC(95%CI) 阈值 敏感度 特异度 约登指数 准确度(n/N) NT-proBNP 0.778(0.631~0.929) 2600 ng/L 0.813 0.753 0.566 0.776(97/125) LVEF 0.790(0.613~0.960) 50% 0.792 0.780 0.572 0.784(98/125) CST 0.716(0.495~0.928) 6 ng/mL 0.708 0.688 0.396 0.695(87/125) Gal-3 0.799(0.654~0.942) 20 ng/mL 0.750 0.831 0.581 0.800(100/125) 联合检测 0.859(0.744~0.972) 0.833 0.883 0.716 0.864(108/125) -
[1] 张娜, 魏彤, 刘长凯. 血清钠和血尿素氮对急性失代偿性心力衰竭病人预后的影响[J]. 中西医结合心脑血管病杂志, 2020, 18(19): 3245-3249. doi: 10.12102/j.issn.1672-1349.2020.19.027
[2] 中华医学会心血管病学分会心力衰竭学组, 中国医师协会心力衰竭专业委员会, 中华心血管病杂志编辑委员会. 中国心力衰竭诊断和治疗指南2018[J]. 中华心力衰竭和心肌病杂志, 2018, 2(4): 196-225. https://www.cnki.com.cn/Article/CJFDTOTAL-ZLYS201904009.htm
[3] 彭智柯, 杨志明, 路申潞. Galectin-3对非瓣膜性持续性心房颤动患者射频消融术后临床疗效的预测价值[J]. 临床心血管病杂志, 2020, 36(8): 741-746. https://www.cnki.com.cn/Article/CJFDTOTAL-LCXB202008013.htm
[4] 刘银侠, 魏峰. 血浆CST水平对慢性心衰患者不良心血管事件的预测价值[J]. 医学临床研究, 2016, 5(33): 174-175.
[5] 马乔娟, 刘超, 张军, 等. 急性失代偿性心力衰竭患者血清钠离子和尿酸水平对短期预后的预测价值[J]. 中国心血管杂志, 2018, 23(6): 473-476. doi: 10.3969/j.issn.1007-5410.2018.06.009
[6] 潘辉军, 汪春艳. 急性失代偿性心力衰竭的治疗进展[J]. 医学综述, 2020, 26(17): 3461-3464, 3470. doi: 10.3969/j.issn.1006-2084.2020.17.026
[7] 张如意, 王宏, 秦晨, 等. 生物电阻抗分析测定液体状态在失代偿性心力衰竭诊治和预后评估中的作用[J]. 临床心血管病杂志, 2020, 36(7): 672-677. https://www.cnki.com.cn/Article/CJFDTOTAL-LCXB202007020.htm
[8] 包艳春, 关秀军, 王小娟, 等. 神经调节蛋白1表达水平与急性失代偿性心力衰竭患者短期预后的相关性[J]. 中华老年心脑血管病杂志, 2021, 23(6): 600-603. doi: 10.3969/j.issn.1009-0126.2021.06.012
[9] 曾永红. 血清Gal-3水平与脓毒症患者病情危重程度及预后关系的研究[J]. 临床急诊杂志, 2020, 21(5): 384-388. https://www.cnki.com.cn/Article/CJFDTOTAL-ZZLC202005011.htm
[10] Ji J, Cheng X, Wang W, et al. Vitamin D regulates cell viability, migration and proliferation by suppressing galectin-3(Gal-3) gene in ovarian cancer cells[J]. J Biosci, 2020, 45(1): 69. doi: 10.1007/s12038-020-00038-1
[11] Trippel TD, Mende M, Düngen HD, et al. The diagnostic and prognostic value of galectin-3 in patients at risk for heart failure with preserved ejection fraction: results from the DIAST-CHF study[J]. ESC Heart Fail, 2021, 8(2): 829-841. doi: 10.1002/ehf2.13174
[12] Wang N, Dang M, Zhang W, et al. Galectin-3 is associated with severe heart failure and death: A hospital-based study in Chinese patients[J]. Scand J Immunol, 2020, 91(5): e12826.
[13] 米传晓, 刘军妮, 邹承伟, 等. 血清可溶性肿瘤因子2抑制剂、半乳糖凝集素-3蛋白水平在慢性心衰分级及预后中的应用[J]. 山东大学学报(医学版), 2019, 57(1): 76-81. https://www.cnki.com.cn/Article/CJFDTOTAL-SDYB201901019.htm
[14] 洪莉丽, 张盛, 汪倩, 等. 基于RAAS/NF-κB/炎症因子级联反应探究真武汤对慢性心力衰竭大鼠治疗作用[J]. 中草药, 2020, 51(5): 1279-1286. https://www.cnki.com.cn/Article/CJFDTOTAL-ZCYO202005027.htm
[15] 高鸿敏, 高丽华. Galectin-3与心力衰竭关系的研究进展[J]. 中国循证心血管医学杂志, 2014, 10(3): 375-376. doi: 10.3969/j.1674-4055.2014.03.48
[16] 许涛, 王慧莹, 赵楚敏, 等. 原发性高血压及左室肥厚患者外周血儿茶酚抑素、脑钠肽及同型半胱氨酸检测的临床意义[J]. 宁夏医科大学学报, 2019, 5(8): 202-205. https://www.cnki.com.cn/Article/CJFDTOTAL-XNXY201904019.htm
[17] 周美欣, 楚天舒. 儿茶酚抑素在急性心肌梗死患者交感神经活性中的研究进展[J]. 心血管病学进展, 2020, 41(7): 695-697. https://www.cnki.com.cn/Article/CJFDTOTAL-XXGB202007006.htm
[18] 樊小容, 谭小青, 张旭升, 等. 儿茶酚抑素抑制血管钙化的作用及机制[J]. 海南医学, 2020, 5(5): 263-266. https://www.cnki.com.cn/Article/CJFDTOTAL-HAIN202005001.htm
[19] 朱小山, 张红申, 杨峰, 等. CHF病人血清儿茶酚抑素、和肽素水平与心力衰竭严重程度及短期心血管事件的关系分析[J]. 中西医结合心脑血管病杂志, 2019, 17(4): 90-93. https://www.cnki.com.cn/Article/CJFDTOTAL-ZYYY201904024.htm
[20] Peng F, Chu S, Ding W, et al. The predictive value of plasma catestatin for all-cause and cardiac deaths in chronic heart failure patients[J]. Peptides, 2016, 86: 112-117. doi: 10.1016/j.peptides.2016.10.007
[21] 甄根深, 张奇峰, 刘威, 等. hs-cTnI及NT-proBNP最佳截断值与慢性心衰患者生存期的相关性研究[J]. 中国循证心血管医学杂志, 2019, 11(4): 484-486, 490. doi: 10.3969/j.issn.1674-4055.2019.04.27
[22] 娄明, 郑玉丽, 邵博一, 等. 左心室射血分数对心力衰竭患者预后的影响[J]. 中国继续医学教育, 2018, 10(36): 49-52. doi: 10.3969/j.issn.1674-9308.2018.36.021
-




 下载:
下载: