Study on the relationship between oxygenation index and diffusion index and pulmonary restability and prognosis after positive end-expiratory pressure therapy in patients with severe acute respiratory distress syndrome
-
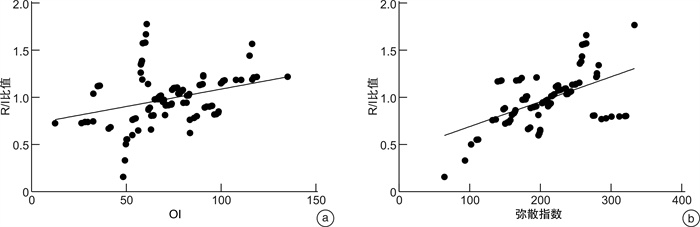
摘要: 目的 探讨氧合指数(OI)及弥散指数与重度急性呼吸窘迫综合征(ARDS)患者呼气末正压治疗后肺可复张性和预后的关系。方法 回顾性选择2020年1月-2021年12月期间我院收治的120例重症ARDS患者,所有患者均接受呼气末正压模式机械通气治疗,复张与充气比(R/I)评估肺复张潜力,并根据R/I比值将患者分为高可复张性组(R/I≥0.5,41例)和低可复张性组(R/I < 0.5,79例),根据住院28 d临床结果分为生存组(36例)和死亡组(84例)。多因素logistic回归分析影响重度ARDS患者临床结果的因素,受试者工作特征曲线(ROC)分析OI及弥散指数预测重度ARDS患者预后的价值。结果 高可复张性组OI、弥散指数高于低可复张性组(P < 0.01),OI及弥散指数与R/I比值均呈正相关(r=0.325、0.532,P < 0.01)。脏器衰竭个数≥2个是重度ARDS患者住院28 d死亡的危险因素(P < 0.05),OI、弥散指数、R/I比值是保护因素(P < 0.05)。弥散指数预测重度ARDS患者预后住院28 d死亡的曲线下面积为0.818,大于OI的0.679(Z=2.639,P < 0.05)。结论 重度ARDS患者OI和弥散指数偏低与肺可复张性低以及住院28 d死亡有关,相对于OI,弥散指数可为预后评估提供更准确信息。Abstract: Objective To investigate the relationship between oxygenation index(OI) and diffusion index and lung restability and prognosis in patients with severe acute respiratory distress syndrome(ARDS) after positive end-expiratory pressure therapy.Methods A total of 120 patients with severe ARDS admitted to our hospital from January 2020 to December 2021 were retrospectively selected. All patients received mechanical ventilation in positive end-expiratory pressure mode. The lung revascularization potential was assessed by R/I ratio, and patients were divided into the high extensibility group (R/I≥0.5, 41 cases) and the low extensibility group (R/I < 0.5, 79 cases) according to the R/I ratio, and the survival group (36 cases) and the death group(84 cases) according to the clinical results of 28 days in hospital. Multivariate logistic regression analyzed the factors affecting the clinical outcome of patients with severe ARDS, receiver operating characteristic curve(ROC) analyzed OI and dispersion index for predicting the prognosis of patients with severe ARDS.Results OI and diffusion index in the high extensibility group were higher than those in the low extensibility group(P < 0.01), OI and diffusion index were positively correlated with R/I ratio(r=0.325, 0.532, P < 0.01). The number of organ failure ≥2 was a risk factor for death of severe ARDS patients after 28 days in hospital(P < 0.05), while OI, dispersion index and R/I ratio were protective factors(P < 0.05). The area under the curve that dispersion index predicted the prognosis of severe ARDS patients and death on 28 days in hospital was 0.818, which was larger than 0.679 of OI(z=2.639, P < 0.05).Conclusion Lower OI and diffusion index in patients with severe ARDS are associated with lower lung extensibility and death after 28 days in hospital. Compared with OI, diffusion index can provide more accurate information for prognosis assessment.
-

-
表 1 高可复张性组和低可复张性组OI及弥散指数差异
x±S 组别 例数 OI 弥散指数 高可复张性组 41 82.35±13.06 246.35±35.09 低可复张性组 79 71.25±10.41 198.12±23.45 t 5.069 8.967 P < 0.01 < 0.01 表 2 影响重度ARDS患者预后的单因素分析结果
例(%) 组别 死亡组(84例) 生存组(36例) t/z/χ2 P 年龄/岁 53.39±3.05 48.79±2.19 8.182 < 0.01 性别 男 51(60.71) 20(55.56) 0.278 0.598 女 33(39.29) 16(44.44) 基础疾病 糖尿病 15(17.86) 5(13.89) 0.286 0.593 高血压 11(13.10) 4(11.11) 0.091 0.763 冠心病 6(7.14) 2(5.56) 0.102 0.749 高脂血症 7(8.33) 4(11.11) 0.234 0.629 ARDS病因 脓毒症 26(30.95) 9(25.00) 重症肺炎 28(33.33) 13(36.11) 肺挫伤 15(17.86) 6(16.67) 0.827 0.935 休克 8(9.52) 5(13.89) 其他 7(8.33) 3(8.33) 机械通气时间/d 15.13(11,17) 12.22(8,15) 5.176 < 0.01 ICU住院时间/d 19.24(15,25) 15.35(10,19) 6.919 < 0.01 脏器衰竭个数≥2个 35(41.67) 7(19.44) 5.470 0.019 合并休克 28(33.33) 5(13.89) 4.779 0.029 APACHEⅡ评分/分 18.15±5.24 14.02±3.74 4.280 < 0.01 SOFA评分/分 10.25±3.54 7.02±2.41 4.995 < 0.01 OI 68.24±8.23 90.91±6.53 14.656 < 0.01 弥散指数 189.32±10.52 273.58±6.09 44.875 < 0.01 R/I比值 0.68±0.20 1.02±0.31 7.172 < 0.01 表 3 影响重度ARDS患者预后的logistic回归方程
因素 β SE Wald χ2 OR(95%CI) P 常数项 5.223 1.083 23.259 < 0.01 脏器衰竭个数≥2个 1.229 0.295 17.356 3.418(1.917~6.093) < 0.01 OI -0.492 0.125 15.492 0.611(0.479~0.781) < 0.01 弥散指数 -0.632 0.167 14.322 0.532(0383~0.737) < 0.01 R/I比值 -0.705 0.196 12.938 0.494(0.336~0.726) < 0.01 表 4 OI及弥散指数预测重度ARDS患者预后的效能
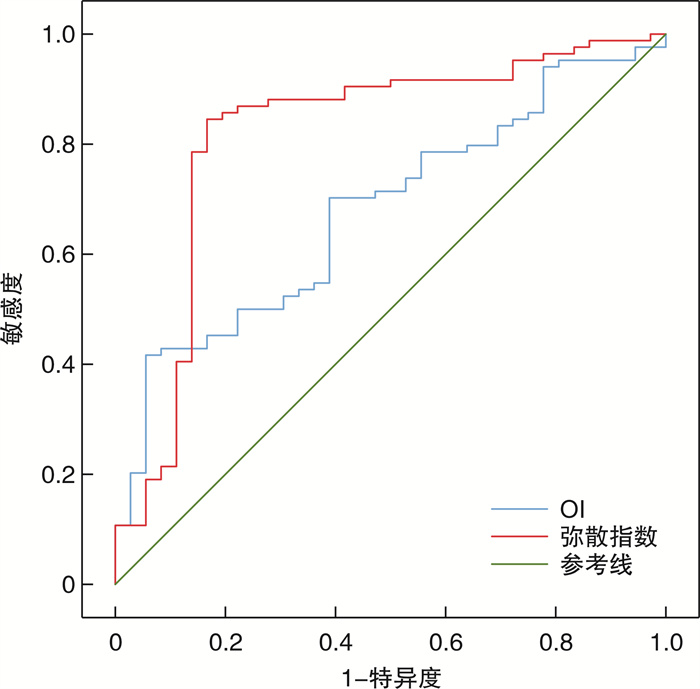
因素 曲线下面积(95%CI) P 临界值 敏感度/% 特异度/% 约登指数 OI 0.679(0.588~0.761) < 0.001 79.15 66.67 61.11 0.2779 弥散指数 0.818(0.738~0.883) < 0.001 221.35 84.52 83.33 0.6785 -
[1] Huppert LA, Matthay MA, Ware LB. Pathogenesis of Acute Respiratory Distress Syndrome[J]. Semin Respir Crit Care Med, 2019, 40(1): 31-39. doi: 10.1055/s-0039-1683996
[2] 何开源, 罗振吉, 王朝晖, 等. 重度急性呼吸窘迫综合征早期联合不同体位和呼气末正压模式对机械通气评价肺可复张性的临床研究[J]. 中国医师进修杂志, 2017, 40(6): 504-508. doi: 10.3760/cma.j.issn.1673-4904.2017.06.006
[3] Pereira SM, Tucci MR, Morais CCA, et al. Individual Positive End-expiratory Pressure Settings Optimize Intraoperative Mechanical Ventilation and Reduce Postoperative Atelectasis[J]. Anesthesiology, 2018, 129(6): 1070-1081. doi: 10.1097/ALN.0000000000002435
[4] Pan C, Chen L, Lu C, et al. Lung Recruitability in COVID-19-associated Acute Respiratory Distress Syndrome: A Single-Center Observational Study[J]. Am J Respir Crit Care Med, 2020, 201(10): 1294-1297. doi: 10.1164/rccm.202003-0527LE
[5] DesPrez K, McNeil JB, Wang C, et al. Oxygenation Saturation Index Predicts Clinical Outcomes in ARDS[J]. Chest, 2017, 152(6): 1151-1158. doi: 10.1016/j.chest.2017.08.002
[6] Vaz Fragoso CA, Cain HC, Casaburi R, et al. Spirometry, Static Lung Volumes, and Diffusing Capacity[J]. Respir Care, 2017, 62(9): 1137-1147. doi: 10.4187/respcare.05515
[7] 滕丽华. "弥散指数"对ARDS预后评估的研究[D]. 北京: 北京协和医学院, 2015.
[8] ARDS Definition Task Force, Ranieri VM, Rubenfeld GD, et al. Acute respiratory distress syndrome: the Berlin Definition[J]. JAMA, 2012, 307(23): 2526-2533.
[9] Chen L, Del Sorbo L, Grieco DL, et al. Potential for Lung Recruitment Estimated by the Recruitment-to-Inflation Ratio in Acute Respiratory Distress Syndrome. A Clinical Trial[J]. Am J Respir Crit Care Med, 2020, 201(2): 178-187. doi: 10.1164/rccm.201902-0334OC
[10] Knaus WA, Draper EA, Wagner DP, et al. APACHEⅡ: a severity of disease classification system[J]. Crit Care Med, 1985, 13(10): 818-829. doi: 10.1097/00003246-198510000-00009
[11] Ferreira FL, Bota DP, Bross A, et al. Serial evaluation of the SOFA score to predict outcome in critically ill patients[J]. JAMA, 2001, 286(14): 1754-1758. doi: 10.1001/jama.286.14.1754
[12] Sahetya SK, Hager DN, Stephens RS, et al. PEEP Titration to Minimize Driving Pressure in Subjects With ARDS: A Prospective Physiological Study[J]. Respir Care, 2020, 65(5): 583-589. doi: 10.4187/respcare.07102
[13] Banavasi H, Nguyen P, Osman H, et al. Management of ARDS-What Works and What Does Not[J]. Am J Med Sci, 2021, 362(1): 13-23. doi: 10.1016/j.amjms.2020.12.019
[14] 贾子毅, 刘晓伟, 刘志. 机械通气氧合指数对ARDS患者预后评估的价值: 附228例回顾性分析[J]. 中华危重病急救医学, 2017, 29(1): 45-50. https://www.cnki.com.cn/Article/CJFDTOTAL-XIBU201906027.htm
[15] 王俊, 姜淑庆. 氧合指数及弥散指数对新型冠状病毒肺炎合并急性呼吸窘迫综合征的机械通气患者预后的评估研究[J]. 中国全科医学, 2021, 24(35): 4481-4484, 4491. https://www.cnki.com.cn/Article/CJFDTOTAL-QKYX202135018.htm
-




 下载:
下载: