Clinical value of early serum colloid osmotic pressure of ARDS secondary to hemorrhagic shock
-
摘要: 目的 探讨血浆胶体渗透压(COP)在创伤失血性休克合并ARDS患者中的早期变化以及对诊断及预后的预测价值。方法 回顾性选取2017年3月—2021年3月期间我院收治的216例创伤患者,其中无休克患者70例(A组),创伤失血性休克合并ARDS 67例(B组),未发生ARDS 79例(C组),收集入院时以及入院后24 h、48 h和72 h的白蛋白(ALB)、纤维蛋白原(FIB)水平,计算COP水平。并采用受试者工作特征(ROC)曲线进行创伤失血性休克并发ARDS诊断及预后效能评价。结果 B、C 2组COP水平在72 h中逐渐下降,B组较C组下降显著,A组变化不明显。入院时B组的ALB、FIB以及COP均显著低于A、C组。ROC曲线分析表明,入院时诊断创伤失血性休克并发ARDS的最大曲线下面积(AUC)为0.746(95%CI:0.665~0.828)(COP);预测死亡的最大AUC为0.842(95%CI:0.725,0.960)(COP)。结论 COP在创伤失血性休克合并ARDS的患者中显著下降,且可以作为创伤失血性休克并发ARDS的诊断及评估预后不良的评价指标。Abstract: Objective To discuss the changes of serum colloid osmotic pressure(COP) in ARDS secondary to hemorrhagic shock, and evaluate the clinical value in diagnosis and mortality predication of ARDS.Methods 216 cases of severely traumatic hemorrhage were divided into non-shock group(70 cases, A group), ARDS secondary to shock group(67 cases, B group) and non-ARDS secondary to shock group(79 cases, C group). Data of ALB, FIB and COP at admission and the 24, 48, 72 hours after admission were collected. Receiver operating characteristic(ROC) curve was used to evaluate the performance of these indexes in cases of hemorrhagic shock with ARDS diagnosis and mortality prediction.Results The levels of COP decreased significantly in group B and group C, and did not change obviously in group A at all time points. The levels of ALB, FIB and COP were significantly lower in group B compared with group A and group C. There were 45 patients died in group B plus group C, whose ALB, FIB and COP levels at admission were significantly lower than those of the survival ones. ROC curves suggested that the best predictive AUC of the early diagnosis in cases of hemorrhagic shock with ARDS at admission were 0.746(95%CI: 0.665-0.828)(COP). Meanwhile the best predictive AUC of mortality at admission was 0.842(95%CI: 0.725-0.960)(COP).Conclusion It is possible that COP should be as significant diagnostic indicators for ARDS secondary to severely traumatic hemorrhage and as predictive markers for poor prognosis of cases with ARDS.
-

-
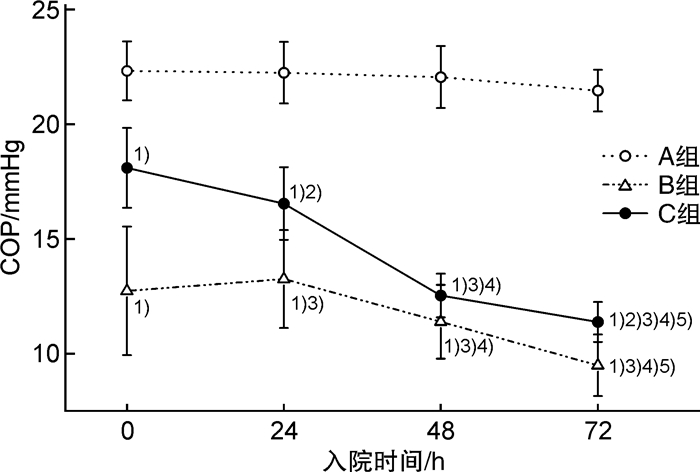
表 1 3组患者入院时ALB、FIB及COP指标的比较
组别 ALB/(g·L-1) FIB/(g·L-1) COP/mmHg A组 37.02±1.52 3.73±0.62 22.39±1.14 B组 25.53±3.031) 1.57±0.651) 12.99±2.071) C组 32.03±2.571)2) 2.42±0.661)2) 18.03±2.011)2) 与A组比较:1)P < 0.05;与B组比较:2)P < 0.05。 表 2 入院时ALB、FIB和COP诊断创伤失血性休克合并ARDS的ROC分析
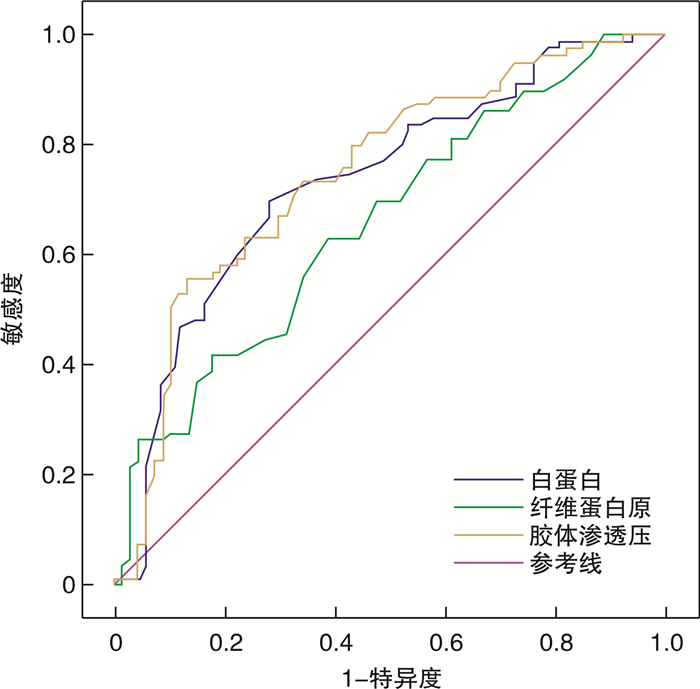
项目 AUC 95%CI Cut-off 敏感度 特异度 ALB 0.731 0.649~0.815 32.05 0.696 0.716 FIB 0.658 0.570~0.746 2.48 0.633 0.612 COP 0.746 0.665~0.828 17.97 0.734 0.657 表 3 创伤失血性休克患者死亡组与存活组3个指标的比较
组别 ALB/
(g·L-1)FIB/
(g·L-1)COP/
mmHg存活组(n=101) 26.57±1.99 1.89±0.59 13.93±1.31 死亡组(n=45) 23.51±2.84 1.44±0.56 11.51±1.95 t -5.075 -3.025 -5.964 P 0.000 0.004 0.000 表 4 入院时ALB、FIB和COP预测创伤失血性休克并发ARDS预后不良的ROC分析
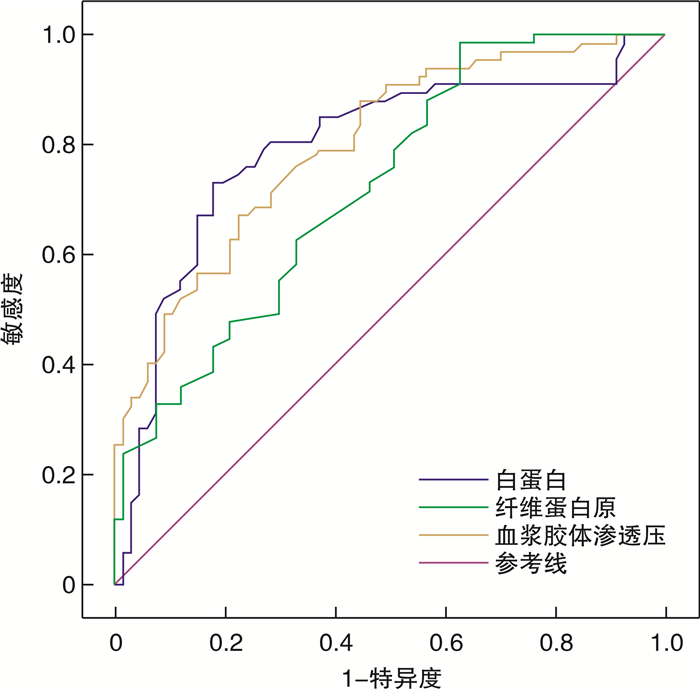
项目 AUC 95%CI Cut-off 敏感度 特异度 ALB 0.790 0.652~0.928 24.55 0.935 0.667 FIB 0.714 0.581~0.847 1.85 0.565 0.810 COP 0.842 0.725~0.960 12.48 0.935 0.714 -
[1] Bellani G. Epidemiology, patterns of care, and mortality for patients with acute respiratory distress syndrome in intensive care units in 50 countries[J]. JAMA, 2016, 315: 788-800. doi: 10.1001/jama.2016.0291
[2] 黄丽丽, 刘玲, 邱海波. 急性呼吸窘迫综合征诊断的进步与发展[J]. 中国实用内科杂志, 2018, 38(11): 7-10. https://www.cnki.com.cn/Article/CJFDTOTAL-SYNK201811001.htm
[3] Geranton F, Chantrel F, Bouiller M, et al. Prediction of colloid osmotic pressure in renal patients[J]. Clinical Nephrology, 2000, 53(4): 269-275.
[4] Moss M, Huang DT, Brower RG. Early neuromuscular blockade in the acute respiratory distress syndrome[J]. N Engl J Med, 2019, 380: 1997-2008. doi: 10.1056/NEJMoa1901686
[5] Meyer NJ, Gattinoni L, Calfee CS. Acute respiratory distress syndrome[J]. Lancet, 2021, S0140-6736(21)00439-6.
[6] Laffey JG, Madotto F, Bellani G. Geo-economic variations in epidemiology, patterns of care, and outcomes in patients with acute respiratory distress syndrome: insights from the LUNG SAFE prospective cohort study[J]. Lancet Respir Med, 2017, 5: 627-638. doi: 10.1016/S2213-2600(17)30213-8
[7] Mourad BM, Rose KM. Acute Respiratory Distress Syndrome[M]. John Wiley & Sons, Ltd, 2021.
[8] 张静, 思永玉. 创伤性凝血病的研究进展[J]. 麻醉安全与质控, 2018, 33(3): 174-180. https://www.cnki.com.cn/Article/CJFDTOTAL-MZAQ201803023.htm
[9] 万珍, 徐俊, 方强. 纤维蛋白原水平对创伤性凝血病预后影响的前瞻性观察研究[J]. 中国急救医学, 2020, 40(9): 6-9. https://www.cnki.com.cn/Article/CJFDTOTAL-ZJJY202009007.htm
[10] 陈鑫, 李亮, 杨志洲, 等. D-二聚体联合损伤严重度评分对创伤患者预后的预测价值[J]. 中华急诊医学杂志, 2018, 13(5): 486-491. doi: 10.3760/cma.j.issn.1671-0282.2018.05.006
[11] 梅程清, 叶正龙, 邹晖, 等. 多发伤患者创伤性凝血病影响因素分析[J]. 中国医刊, 2017, 22(12): 85-88. doi: 10.3969/j.issn.1008-1070.2017.12.025
[12] Geranton F. Prediction of colloid osmotic pressure in renal patients[J]. Clin Nepherol, 2000, 53(4): 269-275.
[12] Vincent JL, Dubois MJ, Navickis RJ, et al. Hypoalbuminemia in acute illness: is there a rationale for intervention? A meta-analysis of cohort studies and controlled trials[J]. Ann Surg, 2003, 237(3): 319-334.
[14] Weil MH, Henning RJ, Puri VK. Colloid oncotic pressure: clinical signifi cance[J]. Crit Care Med, 1979, 7(3): 113-116. doi: 10.1097/00003246-197903000-00006
[15] Martin GS. Fluid balance and colloid osmotic pressure in acute respiratory failure: emerging clinical evidence[J]. Crit Care, 2000, 4 Suppl2: S21-S25.
[16] Rahbar E, Baer LA, Cotton BA, et al. Plasma colloid osmotic pressure is an early indicator of injury and hemorrhagic shock[J]. Shock, 2014, 41(3): 181-187. doi: 10.1097/SHK.0000000000000101
[17] 黄鹂, 艾宇航. 重症患者全血胶体渗透压影响因素的研究[J]. 中南大学学报, 2014, 39(4): 401-407. https://www.cnki.com.cn/Article/CJFDTOTAL-HNYD201404016.htm
-




 下载:
下载: