-
摘要: 目的 分析急性草甘膦中毒患者预后的影响因素,以期为急性草甘膦的预防和治疗提供参考依据。方法 本研究回顾性选取我院2009年9月—2021年2月期间收治的73例急性草甘膦中毒患者的临床资料,其中男32例,女41例;平均年龄(55.86±17.60)岁;所有患者均随访6个月。随访终点事件为全因死亡,全因死亡12例(16.4%)。按照临床结局分为存活组和死亡组,比较2组患者临床特征及实验室指标差异,将单因素分析中差异具有统计学意义的指标纳入多元logistic回归分析,得出独立预后影响因素,使用受试者工作特征(ROC)曲线检验独立危险因素在急性草甘膦中毒预后的预测价值。结果 73例患者单因素分析显示,死亡组年龄、首次医疗接触(FMC)、总胆红素(TBIL)、谷氨酰转移酶(GGT)、碱性磷酸酶(ALP)、谷草转氨酶(AST)、氯、白细胞、凝血时间均大于存活组,钾低于存活组(P< 0.05);多元logistic回归分析显示,GGT、白细胞、凝血时间、年龄及接触医疗时间为急性草甘膦中毒患者预后的影响因素(P< 0.05);创建新的预测模型:-21.559+0.054×GGT(U/L)+0.253×白细胞(×109/L)+0.593×凝血时间(s)+0.103×年龄(岁)(>70岁=1, < 70岁=0)+1.656×FMC(2 h以内=1、2~6 h=2、6 h以上=3);ROC曲线显示,预测模型的AUC为0.900,临界值为0.622,此时的敏感度为91.7%,特异度为70.5%,诊断价值优于单一指标。结论 GGT、白细胞、凝血时间、年龄及接触医疗时间是预测急性草甘膦中毒患者预后的独立危险因素,建立新的预测模型对急性草甘膦中毒患者预后具有较好的预测价值。Abstract: Objective To analyze the prognostic factors of patients with acute glyphosate poisoning, in order to provide reference basis for the prevention and treatment of acute glyphosate poisoning.Methods The clinical data of patients with acute glyphosate poisoning treated in Hefei Second People's Hospital from September 2009 to February 2021 were retrospectively selected. All patients were followed up for 6 months. The end point of follow-up was all-cause death. According to the clinical outcome, the patients were divided into survival group and death group. The differences of clinical characteristics and laboratory indexes between the two groups were compared. The statistically significant indexes in univariate analysis were included in multiple logistic regression analysis to obtain independent prognostic factors. The receiver operating characteristic(ROC) curve was used to test the predictive value of independent risk factors in the prognosis of acute glyphosate poisoning.Results A total of 73 patients were included, including 32 males and 41 females, aged(55.86±17.60) years, and 12 all-cause deaths(16.4%); Univariate analysis showed that age, first medical contact(FMC), TBIL, GGT, ALP, AST, chlorine, leukocyte and coagulation time in the death group were greater than those in the survival group, and potassium was lower than those in the survival group(P< 0.05); Multiple logistic regression analysis showed that GGT, leukocyte, coagulation time, age and medical contact time were the influencing factors of prognosis in patients with acute glyphosate poisoning(P< 0.05); Create a new prediction model: -21.559 + 0.054 × GGT(U/L) +0.253×Leukocyte(×109 /L)+ 0.593 × Coagulation time(s)+ 0.103×Age(years)(>70 years=1, < 70 years=0)+ 1.656 × FMC(within 2 hours=1, 2 to 6 hours=2, more than 6 hours=3); The ROC curve showed that the AUC of the prediction model was 0.900 and the critical value was 0.622. At this time, the sensitivity was 91.7% and the specificity was 70.5%. The diagnostic value was better than a single index.Conclusion GGT, leukocyte, coagulation time, age and medical exposure time are independent risk factors for predicting the prognosis of patients with acute glyphosate poisoning. The establishment of a new prediction model has good predictive value for the prognosis of patients with acute glyphosate poisoning.
-
Key words:
- glyphosate /
- poisoning /
- prognostic factors /
- prediction model /
- receiver operating characteristic curve
-

-
表 1 单因素分析急性草甘膦中毒预后的影响因素
例,X±S 项目 死亡组(n=12) 存活组(n=61) χ2/t/z P 年龄/岁 66.75±20.66 53.72±16.27 t=2.423 0.018 性别 χ2=0.027 0.868 男 5 27 女 7 34 合并疾病 高血压 8 10 χ2=13.642 < 0.001 糖尿病 4 3 χ2=9.339 0.002 恶性肿瘤 5 2 χ2=17.044 < 0.001 心脑血管疾病 7 9 χ2=4.686 0.03 消化道反应 恶心、呕吐 10 58 χ2=2.169 0.141 腹痛 6 15 χ2=3.159 0.075 呼吸系统损害 咳嗽、胸闷 7 52 χ2=4.686 0.03 呼吸困难、呼吸衰竭 1 7 χ2=6.75 0.009 心血管系统损害 心动过速 2 5 χ2=0.83 0.362 心动过缓 0 2 χ2=0.405 0.525 神经系统损害 头晕、乏力 5 23 χ2=0.067 0.796 出汗流涎 4 8 χ2=2.984 0.084 神志异常、抽搐和昏迷 1 3 χ2=0.226 0.635 肝功能损害 TBIL升高 2 6 χ2=0.479 0.489 GGT升高 6 9 χ2=7.63 0.006 ALT升高 1 5 χ2=1.358 0.244 AST升高 10 23 χ2=8.428 0.004 LDH升高 1 3 χ2=0.226 0.635 肾功能损害 尿酸升高 0 1 χ2=0.199 0.655 尿素升高 1 6 χ2=0.026 0.872 电解质紊乱 低钾血症 3 16 χ2=0.008 0.929 高钠血症 0 3 χ2=0.615 0.433 高氯血症 2 12 χ2=0.058 0.809 血常规异常 白细胞升高 5 41 χ2=2.808 0.094 凝血功能异常 凝血酶原时间延长 3 22 χ2=0.545 0.46 文化程度 χ2=0.826 0.251 小学及以下 5 23 初中 3 30 高中及以上 4 8 婚姻状态 χ2=0.139 0.709 已婚 7 32 未婚 5 29 子女状态 χ2=3.54 0.06 有 10 33 无 2 28 FMCa):1/2/3 3/7/2 37/22/2 χ2=6.726 0.029 洗胃 12 61 - - 血液灌流 11 48 χ2=2.861 0.091 TBIL/(μmol·L-1) 21.87±10.95 13.28±6.26 z=-2.895 0.004 GGT/(U·L-1) 64.50±49.31 31.75±22.52 z=-2.727 0.036 ALP/(U·L-1) 92.16±38.10 70.20±26.15 t=2.454 0.017 LDH/(U·L-1) 666.17±36.34 521.21±124.48 z=-0.298 0.766 AST/(U·L-1) 52.25±23.4 37.52±21.80 t=2.106 0.039 UA/(μmol·L-1) 298.52±47.44 271.00±42.97 t=1.231 0.222 Urea/(μmol·L-1) 5.57±1.89 5.31±2.55 t=0.649 0.518 K/(μmol·L-1) 3.34±0.17 3.67±0.34 z=-3.605 < 0.001 NA/(μmol·L-1) 142.17±4.71 139.99±3.39 t=1.523 0.132 CL/(μmol·L-1) 108.33±5.80 103.98±3.25 z=-2.095 0.036 WBC/(×109·L-1) 12.30±3.53 10.37±2.69 t=2.152 0.035 凝血时间/s 15.18±2.04 13.69±1.92 t=2.441 0.017 中毒剂量/mL 100(100,200) 200(30,200) z=0.067 0.939 注:a)FMC:2 h以内=1,2~6 h=2,6 h以上=3。 表 2 中毒预后多因素分析结果
变量 B Wald χ2 P OR 95%CI 常量 -21.559 10.644 0.307 0.000 0.000 GGT 0.054 6.090 0.014 1.055 1.011~1.102 白细胞 0.253 4.154 0.042 1.288 1.013~1.643 凝血时间 0.593 5.254 0.022 1.810 1.090~3.005 年龄 0.103 7.516 0.006 1.108 1.030~1.193 FMC 1.656 4.001 0.045 5.238 1.034~26.538 注:因变量:存活=0,死亡=1;年龄:>70岁=1,≤70岁=0;FMC:2 h以内=1,2~6 h=2,6 h以上=3。 -
[1] 赵倩, 洪广亮, 赵光举, 等. 我国综合性医院急性中毒流行病学现状分析[J]. 临床急诊杂志, 2016, 17(2): 131-136.
[2] 郭浩然, 蔡文妍, 刘炘, 等. 草甘膦生物毒性研究进展[J]. 职业卫生与应急救援, 2018, 36(3): 212-215, 219.
[3] Van Bruggen A, He MM, Shin K, et al. Environmental and health effects of the herbicide glyphosate[J]. Sci Total Environ, 2018, 616-617: 255-268. doi: 10.1016/j.scitotenv.2017.10.309
[4] 杨益军. 2018年中国(全球)草甘膦市场研究报告(一)[J]. 南方农药, 2018, 22(1): 28-31.
[5] 翟素平, 陆士奇, 闫彬, 等. 急性中毒患者血栓弹力图和常规凝血指标的相关性及应用[J]. 中国急救医学, 2021, 41(10): 856-861. doi: 10.3969/j.issn.1002-1949.2021.10.005
[6] 中国医师协会急诊医师分会, 中国毒理学会中毒与救治专业委员会. 急性中毒诊断与治疗中国专家共识[J]. 中华急诊医学杂志, 2016, 25(11): 1361-1375. doi: 10.3760/cma.j.issn.1671-0282.2016.11.004
[7] 于光彩, 菅向东, 高蓓钧, 等. 急性草甘膦中毒10例临床分析[J]. 中华劳动卫生职业病杂志, 2017, 35(5): 382-383. doi: 10.3760/cma.j.issn.1001-9391.2017.05.019
[8] 殷菲. APACHE Ⅱ评分和血清白蛋白联合分析在评估急性重症有机磷中毒患者预后中的价值研究[J]. 临床急诊杂志, 2021, 22(1): 21-26. https://www.cnki.com.cn/Article/CJFDTOTAL-ZZLC202101005.htm
[9] Moon JM, Chun BJ, Cho YS. The characteristics of emergency department presentations related to acute herbicide or insecticide poisoning in South Korea between 2011 and 2014[J]. J Toxicol Environ Health A, 2016, 79(11): 466-476. doi: 10.1080/15287394.2016.1172529
[10] 窦建瑞, 周信, 苗润丰, 等. 40例急性草甘膦中毒患者临床特点及预后影响因素分析[J]. 中华劳动卫生职业病杂志, 2021, 39(9): 676-681. doi: 10.3760/cma.j.cn121094-20201030-00601
[11] 王晶. 血清ALT、AST和GGT水平检测在肝脏疾病诊断中的应用分析[J]. 医药论坛杂志, 2018, 39(10): 176, 封3. https://www.cnki.com.cn/Article/CJFDTOTAL-HYYX201810067.htm
[12] 方悦, 滕晓晶. 不同类型肝病患者纤维蛋白/纤维蛋白原降解产物D二聚体与凝血四项联合检测的临床意义[J]. 中国药物与临床, 2019, 19(22): 3986-3987.
[13] 李军, 李恒. 血清胆碱酯酶和急性有机磷农药中毒患者预后相关性分析[J]. 毒理学杂志, 2017, 31(5): 378-381. https://www.cnki.com.cn/Article/CJFDTOTAL-WSDL201705013.htm
[14] 蒋臻, 陈金刚, 曹钰, 等. 白细胞计数早期评估急性百草枯中毒患者预后的价值[J]. 临床急诊杂志, 2017, 18(3): 166-169. https://www.cnki.com.cn/Article/CJFDTOTAL-ZZLC201703003.htm
[15] 李勇, 吴征臻, 李龙. 急诊床旁血液灌流治疗老年镇静催眠类药物中毒的疗效[J]. 临床急诊杂志, 2021, 22(1): 60-64. https://www.cnki.com.cn/Article/CJFDTOTAL-ZZLC202101014.htm
[16] 吴一旭, 王蕾, 吴章, 等. 老年急性中毒患者临床特点和死亡危险因素分析[J]. 中华劳动卫生职业病杂志, 2017, 35(5): 353-355. doi: 10.3760/cma.j.issn.1001-9391.2017.05.008
[17] 廖周勇, 杨千山, 伏利蓉, 等. 2012-2017年阆中市60岁及以上老年人伤害死亡分析[J]. 预防医学情报杂志, 2020, 36(1): 25-28, 33.
[18] 尹一帆, 蒲玟静, 蔡娅茜, 等. 农药中毒继发急性肾损伤的危险因素[J]. 中华劳动卫生职业病杂志, 2021, 39(5): 333-336. doi: 10.3760/cma.j.cn121094-20200909-00522
[19] Mishra A, Rustgi V. Prognostic Models in Acute Liver Failure[J]. Clin Liver Dis, 2018, 22(2): 375-388.
[20] 胡辉, 黄贝贝, 宁玲, 等. HBV相关慢加急性肝衰竭患者短期预后预测模型的建立与评价[J]. 临床肝胆病杂志, 2020, 36(1): 123-127.
-

| 引用本文: | 韩琴, 李四生, 姚莉. 急性草甘膦中毒的预后因素分析[J]. 临床急诊杂志, 2022, 23(1): 19-24. doi: 10.13201/j.issn.1009-5918.2022.01.005 |
| Citation: | HAN Qin, LI Sisheng, YAO Li. Analysis of prognostic factors of acute glyphosate poisoning[J]. J Clin Emerg, 2022, 23(1): 19-24. doi: 10.13201/j.issn.1009-5918.2022.01.005 |
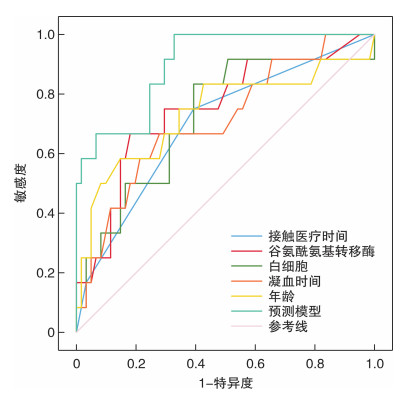
- Figure 1.



 下载:
下载: