Correlation between serum LDH, D-LA levels and prognosis in patients with acute upper gastrointestinal bleeding
-
摘要: 目的 通过检测急性上消化道出血患者血清乳酸脱氢酶(lactate dehydrogenase, LDH)、D-乳酸(D-lactic acid, D-LA)水平, 探究二者与患者预后的关系。方法 选择2018年12月-2023年1月在邯郸市人民医院住院治疗的急性上消化道出血患者216例作为试验组, 体检健康人员132例作为对照组。收集急性上消化道出血患者临床资料、AIMS65评分和生化指标, 检测试验组和对照组血清LDH、D-LA水平。根据入院后30 d内存活情况, 将急性上消化道出血患者分为存活组194例, 死亡组22例。分析急性上消化道出血患者血清LDH与D-LA水平的相关性, 影响急性上消化道出血患者入院后30 d内死亡的因素, 血清LDH和D-LA水平对急性上消化道出血患者入院后30 d内死亡的预测价值。结果 与对照组比较, 试验组血清LDH、D-LA水平显著升高, 差异有统计学意义(P < 0.05);与存活组比较, 死亡组AIMS65评分、血清LDH、D-LA水平显著升高, 血红蛋白(Hb)水平显著降低, 差异有统计学意义(P < 0.05);急性上消化道出血患者血清LDH与D-LA水平呈正相关, 差异有统计学意义(P < 0.05);AIMS65评分高、高水平LDH、高水平D-LA均是影响急性上消化道出血患者入院后30 d内死亡的独立危险因素, 差异有统计学意义(P < 0.05);血清LDH、D-LA、二者联合预测急性上消化道出血患者入院后30 d内死亡的曲线下面积(AUC)分别为0.844、0.819、0.916, 二者联合预测的AUC高于血清LDH、D-LA各自单独预测的AUC(P < 0.05)。结论 急性上消化道出血患者血清LDH和D-LA水平升高, 二者水平与患者预后密切相关, 联合检测血清LDH和D-LA对患者预后有较高的预测价值。Abstract: Objective To investigate the relationship between serum lactate dehydrogenase(LDH) and D-lactic acid(D-LA) levels in patients with acute upper gastrointestinal bleeding and their prognosis.Methods A total of 216 patients with acute upper gastrointestinal bleeding hospitalized in Handan People's Hospital from December 2018 to January 2023 were selected as the experimental group, and 132 healthy persons were selected as the control group. Clinical data, AIMS65 score and biochemical indexes of patients with acute upper gastrointestinal bleeding were collected, and serum LDH and D-LA levels of the experimental group and control group were detected. According to the survival within 30 days after admission, patients with acute upper gastrointestinal bleeding were divided into survival group(194 cases) and death group(22 cases).Clinical data were analyzed, including the correlation between serum LDH and D-LA levels in patients with acute upper gastrointestinal bleeding, the factors affecting death within 30 days after admission in patients with acute upper gastrointestinal bleeding, and the predictive value of serum LDH and D-LA levels on death within 30 days after admission in patients with acute upper gastrointestinal bleeding.Results Compared with control group, serum LDH and D-LA levels in experimental group were significantly increased(P < 0.05). Compared with survival group, AIMS65 score, serum LDH and D-LA levels in death group were significantly increased, while hemoglobin(Hb) level was significantly decreased(P < 0.05). Serum LDH was positively correlated with D-LA level in patients with acute upper gastrointestinal bleeding(P < 0.05). High AIMS65 score, high LDH level and high D-LA level were independent risk factors for death within 30 days after admission in patients with acute upper gastrointestinal bleeding(P < 0.05). The area under curve(AUC) of serum LDH, D-LA, and their combined prediction of death within 30 days after admission in patients with acute upper gastrointestinal bleeding were 0.844, 0.819, and 0.916, respectively, and the AUC of combined prediction was higher than that of serum LDH and D-LA separately(P < 0.05).Conclusion Serum LDH and D-LA levels are elevated in patients with acute upper gastrointestinal hemorrhage, and the levels of both is closely related to patient prognosis, and the combined detection of serum LDH and D-LA has a high predictive value for patient prognosis.
-
Key words:
- acute upper gastrointestinal bleeding /
- lactate dehydrogenase /
- D-lactic acid /
- prognosis
-

-
表 1 AIMS65评分标准
指标 分数/分 ALB < 30 g/L 1 格拉斯哥昏迷量表评分 < 14分 1 收缩压 < 90 mmHga) 1 年龄>65岁 1 国际标准化比值>1.5 1 注:a)1 mmHg=0.133 kPa。 表 2 对照组和试验组血清LDH、D-LA水平比较
X±S 组别 例数 LDH/(U/L) D-LA/(mg/L) 对照组 132 197.42±29.44 9.17±2.05 试验组 216 489.03±52.71 21.06±4.13 t 58.233 30.825 P < 0.001 < 0.001 表 3 存活组和死亡组临床资料、AIMS65评分和生化指标比较
X±S 项目 存活组(194例) 死亡组(22例) χ2/t P 性别/例 0.008 0.927 男 99 11 女 95 11 年龄/岁 58.41±8.27 60.54±8.86 1.137 0.257 BMI/(kg/m2) 23.52±3.90 23.86±3.73 0.389 0.698 吸烟史/例(%) 68(35.05) 9(40.91) 0.296 0.587 饮酒史/例(%) 31(15.98) 5(22.73) 0.648 0.421 基础疾病史/例(%) 高脂血症 46(23.71) 7(31.82) 0.701 0.402 糖尿病 49(25.26) 6(27.27) 0.042 0.837 高血压 61(31.44) 8(36.36) 0.220 0.639 冠心病 20(10.31) 3(13.64) 0.230 0.632 肝硬化史 14(7.22) 2(9.09) 0.101 0.750 幽门螺杆菌感染 104(53.61) 13(59.09) 0.239 0.625 急性上消化道出血病因/例(%) 0.053 0.974 消化性溃疡 32(16.49) 4(18.18) 食管胃底静脉曲张破裂 119(61.34) 13(59.09) 急性胃黏膜损伤 43(22.17) 5(22.73) 抗血小板药物使用史/例(%) 22(11.34) 3(13.64) 0.102 0.750 AIMS65评分/分 2.26±0.43 3.58±0.49 13.450 < 0.001 TBIL/(μmol/L) 16.89±2.85 17.58±3.01 1.070 0.286 AST/(U/L) 37.59±4.18 38.04±4.77 0.472 0.638 ALT/(U/L) 33.76±4.50 35.06±5.12 1.266 0.207 BUN/(mmol/L) 6.01±0.61 6.23±0.73 1.570 0.118 Scr/(μmol/L) 77.08±9.13 79.52±10.35 1.172 0.243 ALB/(g/L) 30.01±4.17 29.04±3.96 1.039 0.300 Hb/(g/L) 106.33±11.68 97.84±10.15 3.271 0.001 PLT/(×109/L) 116.02±12.87 112.59±13.86 1.176 0.241 TT/s 15.03±2.18 15.24±2.09 0.430 0.668 PT/s 14.10±2.33 13.95±2.21 0.288 0.774 表 4 存活组和死亡组血清LDH、D-LA水平比较
X±S 组别 例数 LDH/(U/L) D-LA/(mg/L) 存活组 194 467.41±49.25 19.72±3.97 死亡组 22 679.68±83.22 32.88±5.54 t 17.622 14.094 P < 0.001 < 0.001 表 5 影响急性上消化道出血患者入院后30 d内死亡的因素分析
自变量 β SE Wald χ2 P OR 95%CI AIMS65评分 0.276 0.116 5.666 0.017 1.318 1.050~1.654 Hb -0.206 0.122 2.845 0.092 0.814 0.641~1.034 LDH 1.108 0.357 9.637 0.002 3.029 1.505~6.098 D-LA 0.922 0.269 11.745 0.001 2.514 1.484~4.259 表 6 血清LDH、D-LA水平对急性上消化道出血患者入院后30 d内死亡的预测价值
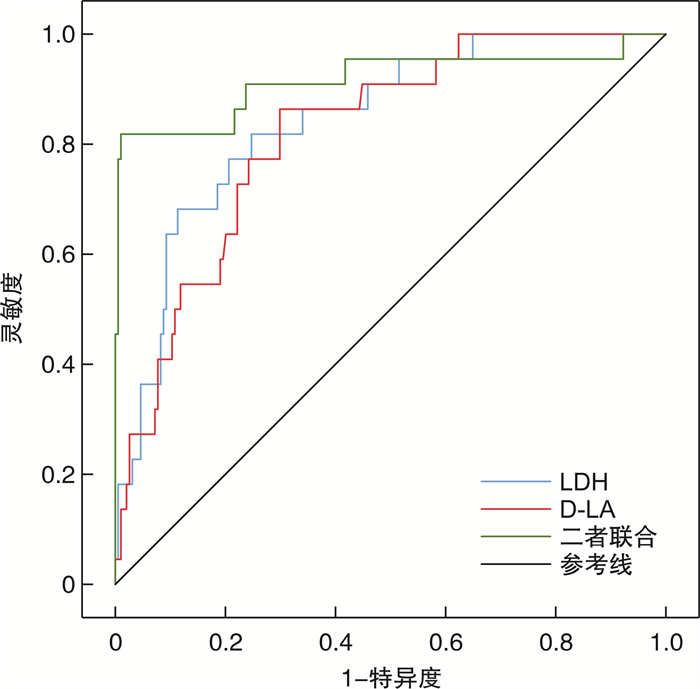
指标 AUC 95%CI 截断值 灵敏度/% 特异度/% 约登指数 LDH 0.844 0.764~0.924 522.91 U/L 81.82 75.26 0.571 D-LA 0.819 0.739~0.900 24.86 mg/L 86.36 70.10 0.565 二者联合 0.916 0.828~1.000 - 81.70 98.97 0.807 -
[1] Laursen SB, Oakland K, Laine L, et al. ABC score: a new risk score that accurately predicts mortality in acute upper and lower gastrointestinal bleeding: an international multicentre study[J]. Gut, 2021, 70(4): 707-716. doi: 10.1136/gutjnl-2019-320002
[2] 中国医师协会急诊医师分会, 中华医学会急诊医学分会, 全军急救医学专业委员会, 等. 急性上消化道出血急诊诊治流程专家共识(2020版)[J]. 中华急诊医学杂志, 2021, 30(1): 15-24. doi: 10.3760/cma.j.issn.1671-0282.2021.01.006
[3] Hreinsson JP, Jonsson A, Bjornsson ES. Acute upper gastrointestinal bleeding: a population-based, five-year follow-up study[J]. Scand J Gastroenterol, 2021, 56(1): 1-5. doi: 10.1080/00365521.2020.1849384
[4] Lau J. Management of acute upper gastrointestinal bleeding: Urgent versus early endoscopy[J]. Dig Endosc, 2022, 34(2): 260-264. . doi: 10.1111/den.14144
[5] Hicks KG, Cluntun AA, Schubert HL, et al. Protein-metabolite interactomics of carbohydrate metabolism reveal regulation of lactate dehydrogenase[J]. Science, 2023, 379(6636): 996-1003. doi: 10.1126/science.abm3452
[6] 徐玉龙, 管建国, 宗桂荣, 等. 急性胰腺炎患者血清二胺氧化酶及D-乳酸水平与肠道功能的关系[J]. 重庆医学, 2021, 50(15): 2583-2585, 2591. doi: 10.3969/j.issn.1671-8348.2021.15.014
[7] 王溪, 黄桔秀, 王颖, 等. 脓毒症患者肠道细菌紊乱与PCT、D-乳酸、内毒素水平的相关性[J]. 中国现代医生, 2022, 60(18): 141-144. https://www.cnki.com.cn/Article/CJFDTOTAL-ZDYS202218036.htm
[8] 中国医师协会急诊医师分会. 急性上消化道出血急诊诊治流程专家共识[J]. 中国急救医学, 2015, 35(10): 865-873. doi: 10.3969/j.issn.1002-1949.2015.10.001
[9] Robertson M, Ng J, Abu Shawish W, et al. Risk stratification in acute variceal bleeding: Comparison of the AIMS65 score to established upper gastrointestinal bleeding and liver disease severity risk stratification scoring systems in predicting mortality and rebleeding[J]. Dig Endosc, 2020, 32(5): 761-768. doi: 10.1111/den.13577
[10] 李会龙, 张晓哲. 三黄泻心汤在肝脾血瘀型肝硬化合并非静脉曲张性上消化道出血患者中的应用效果研究[J]. 中国中西医结合消化杂志, 2022, 30(11): 794-798. doi: 10.3969/j.issn.1671-038X.2022.11.08
[11] Sotiropoulos C, Papantoniou K, Tsounis E, et al. Acute Upper Gastrointestinal Bleeding: Less Severe Bleeding in More Frail and Older Patients, Comparison Between Two Time Periods Fifteen Years Apart[J]. Gastroenterology Res, 2022, 15(3): 127-135. doi: 10.14740/gr1534
[12] 董丽丽, 周荣斌. 急性上消化道出血救治研究现状[J]. 中国实用内科杂志, 2021, 41(3): 203-208. https://www.cnki.com.cn/Article/CJFDTOTAL-SYNK202103008.htm
[13] Lee HA, Jung HK, Kim TO, et al. Clinical outcomes of acute upper gastrointestinal bleeding according to the risk indicated by Glasgow-Blatchford risk score-computed tomography score in the emergency room[J]. Korean J Intern Med, 2022, 37(6): 1176-1185. doi: 10.3904/kjim.2022.099
[14] 李玥, 胡祥鹏, 章礼久. 三种内镜前评分系统对危险性急性上消化道出血预后评估的比较[J]. 蚌埠医学院学报, 2022, 47(8): 1026-1029. https://www.cnki.com.cn/Article/CJFDTOTAL-BANG202208009.htm
[15] Bockoven C, Benirschke RC, Lee HK. Elevated lactate dehydrogenase concentrations in plasma compared to serum[J]. Lab Med, 2022, 53(5): 479-482. doi: 10.1093/labmed/lmac026
[16] Conde Monroy DM, Girón Arango F, Rodríguez Moreno L, et al. Succoring the challenging acute mesenteric ischemia: Feasibility of lactate dehydrogenase for evaluation of intestinal necrosis extension and mortality[J]. Ann Med Surg(Lond), 2022, 84(1): 104922-104929.
[17] 张欢, 刘华柱, 黄小梅, 等. 肝硬化腹水患者血清与腹水中LDH、GLU、SAAG水平与肝功能分级及预后关系[J]. 西部医学, 2023, 35(2): 277-281. https://www.cnki.com.cn/Article/CJFDTOTAL-XIBU202302024.htm
[18] Nachmias-Peiser N, Soffer S, Horesh N, et al. Mortality in patients who underwent computed tomography angiography for a suspected acute mesenteric ischemia as a final alternative diagnosis[J]. Isr Med Assoc J, 2022, 25(12): 828-833.
[19] 肖田, 曹匡纬, 余运运, 等. 不同手术时机治疗小儿肠梗阻的临床效果及对患儿血清二胺氧化酶和D-乳酸水平的影响[J]. 中国妇幼保健, 2023, 38(4): 653-656. https://www.cnki.com.cn/Article/CJFDTOTAL-ZFYB202304020.htm
[20] Khrais A, Ali H, Choi S, et al. D-lactic acidosis in short bowel syndrome[J]. Cureus, 2022, 14(5): e25471.
[21] Li Q, Xu T, Zhong H, et al. Impaired intestinal barrier in patients with obstructive sleep apnea[J]. Sleep Breath, 2021, 25(2): 749-756.
[22] 王天鹏, 蒋成行, 胡升安, 等. 联合肠型脂肪酸结合蛋白、D-乳酸及D-二聚体在急性肠系膜上动脉闭塞患者中的临床意义[J]. 广东医学, 2020, 41(21): 2205-2208. https://www.cnki.com.cn/Article/CJFDTOTAL-GAYX202021013.htm
-




 下载:
下载: