Clinical study on the risk factors of mortality and the association of serum albumin and infection site with the prognosis in patients with bloodstream infection
-
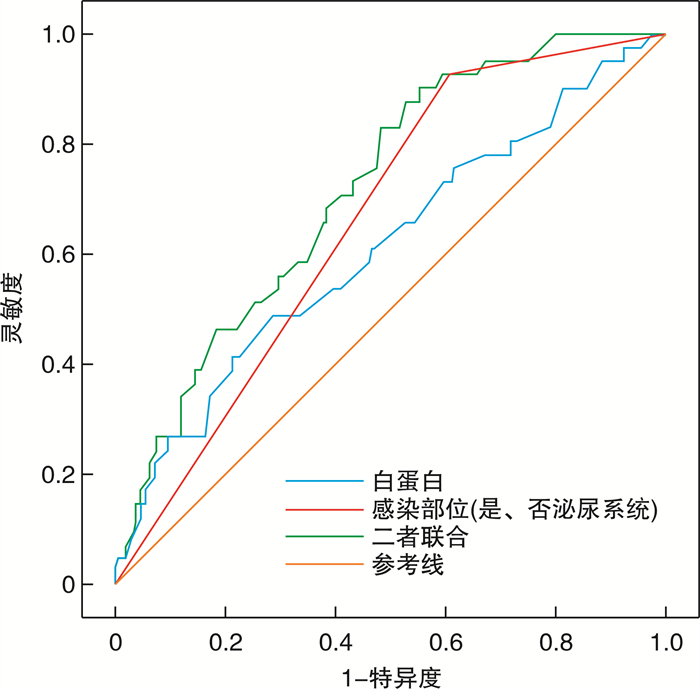
摘要: 目的 探讨血流感染患者28 d死亡危险因素和血清白蛋白及感染部位对预后的预测价值。方法 回顾分析南华大学附属长沙中心医院282例血培养阳性血流感染患者临床资料, 根据28 d生存情况分为生存组(241例)和死亡组(41例), 比较两组临床资料, 然后将差异有统计学意义的项目进行单因素和多因素logistic回归分析, 并以多因素分析有统计学意义的血清白蛋白、感染部位及二者联合构建预测模型, 绘制ROC曲线, 用ROC曲线评估血流感染28 d死亡风险的预测价值。结果 282例血培养阳性血流感染患者中, 革兰阴性菌为主, 占比为59.9%, 革兰阳性菌占比为39.0%;革兰阴性菌以大肠埃希菌(36.5%)和肺炎克雷伯氏菌(12.0%)为主, 革兰阳性菌以凝固酶阴性葡萄球菌(12.8%)和金黄色葡萄糖球菌(9.2%)为主; 28 d生存组和死亡组在性别、病原体分类、感染部位、血尿素氮、血肌酐和白蛋白方面比较, 差异有统计学意义(P < 0.05);年龄、糖尿病史、血糖、白细胞、中性粒细胞、淋巴细胞、血小板计数、红细胞压积、PCT分级、谷丙转氨酶、谷草转氨酶、总胆红素、直接胆红素和住院时间≥30 d比较, 差异无统计学意义(P>0.05);感染部位中泌尿系统、呼吸系统、消化管道、肝胆系统、导管相关、神经系统、骨关节及皮肤软组织分别为34.8%、34.4%、6.4%、9.6%、5.0%、2.8%和4.3%;多因素分析中感染部位和白蛋白与28 d死亡预后相关(P < 0.05);感染部位以泌尿系统为参照, 呼吸系统、消化管道、神经系统和骨关节及皮肤软组织28 d病死率分别为泌尿系统的9.5倍, 7.8倍, 21.8倍和9.0倍, 差异有统计学意义(P < 0.05);以血清白蛋白、感染部位及二者联合预测28 d死亡, 绘制ROC曲线, AUC分别为0.612(95%CI: 0.515~0.710)、0.661(95%CI: 0.583~0.738)和0.719(95%CI: 0.644~0.795)。结论 血清低白蛋白血症和感染部位是血流感染患者28 d死亡风险的独立危险因素, 相对于泌尿系统, 感染部位为呼吸系统、消化管道、神经系统和骨关节及皮肤软组织病死率风险高; 白蛋白及感染部位对血流感染患者28 d预后预测有一定的价值。Abstract: Objective To explore risk factors of 28-day mortality in patients with bloodstream infection, and the predictive value of serum albumin and infection site for prognosis.Methods A retrospective analysis was conducted on the clinical data of 282 patients with blood culture positive bloodstream infection in The Affiliated Changsha Central Hospital University South China. They were divided into a 28-day survival group(n=241) and a 28-day non-survival group(n=41). The clinical data of the two groups were compared, and statistically significances were analyzed by univariate and multivariate logistic regression analysis. A predictive model was constructed with serum albumin, infection site, and a combination of both. ROC curves were performed to evaluate the predictive value for 28-day mortality risk in patient with bloodstream infection.Results Among the 282 bloodstream infection patients with positive blood cultures.Gram-negative bacteria accounted for 59.9%, while Gram-positive bacteria accounted for 39.0%; Gram-negative bacteria were mainly Escherichia coli(36.5%) and Klebsiella pneumoniae(12.0%), while Gram-positive bacteria were mainly coagulase negative Staphylococcus(12.8%) and Staphylococcus aureus(9.2%). There were statistically significant differences (P < 0.05) between the survival group and the death group in terms of gender, pathogen classification, infection site, blood urea nitrogen, blood creatinine, albumin. There were no statistical significances (P>0.05) in age, history of diabetes, blood sugar, white blood cells, neutrophils, lymphocytes, platelet count, hematocrit, PCT grade, alanine transaminase, glutamic transaminase, total bilirubin direct bilirubin and hospitalization time≥30 days between 28-day survival group and 28-day non-survival group. The urinary system, respiratory system, gastrointestinal tract, hepatobiliary system, catheter-related, nervous system, and musculoskeletal and soft tissue accounted for 34.8%, 34.4%, 6.4%, 9.6%, 5.0%, 2.8%, and 4.3% respectively in terms of the site of infection.The infection site and albumin were associated with the 28-day mortality prognosis in the multivariate analysis (P < 0.05). Compared to the urinary system as a reference, the 28-day mortality rates for the respiratory system, digestive tract, nervous system, and musculoskeletal system and skin soft tissue were 9.5 times, 7.8 times, 21.8 times, and 9.0 times higher, respectively (P < 0.05). The ROC curves were plotted to predict 28-day mortality using serum albumin, infection site, and their combination. The AUC values were 0.612(95% CI: 0.515-0.710), 0.661(95% CI: 0.583-0.738), and 0.719(95% CI: 0.644-0.795) respectively.Conclusion Serum hypoalbuminemia and the site of infection were the independent risk factors for the 28-day mortality prognosis in patients with bloodstream infection. Those patients who had the infection sites including respiratory system, digestive tract, nervous system, bone joints, and skin soft tissue had a higher risk of mortality compared to the patients with urinary system infection. Hypoalbuminemia and the site of infection have some predictive value for the prognosis of patients with bloodstream infections at 28 days.
-
Key words:
- blood stream infection /
- sepsis /
- albumin /
- infection site /
- risk factors
-

-
表 1 282例血培养阳性生存组和死亡组临床资料比较
临床资料 生存组(241例) 死亡组(41例) χ2/t/Z P 性别/例(%) 5.669 0.017 男 116(48.1) 28(68.3) 女 125(51.9) 13(31.7) 年龄/(岁,X±S) 63.8±15.5 66.9±16.2 1.181 0.239 病原体分类/例(%) 19.774 < 0.001 革兰阴性菌 150(62.2) 19(46.3) 革兰阳性菌 91(37.8) 19(46.3) 真菌 0 3(7.4) 感染部位/例(%) 21.242 0.003 泌尿系统 95(39.4) 3(7.3) 呼吸系统 74(30.7) 23(56.1) 上、下消化管道 14(5.8) 4(9.8) 肝胆系统 25(10.4) 2(4.9) 导管相关 11(4.6) 3(7.3) 神经系统 6(2.5) 2(4.9) 骨关节及皮肤软组织 9(3.7) 3(7.3) 其他 7(2.9) 1(2.4) 糖尿病史/例(%) 65(27.0) 13(31.7) 0.393 0.531 血糖/[mmol/L,M(Q1,Q3)] 7.6(6.3,10.0) 7.8(5.8,13.0) -1.145 0.252 白细胞/[×109,M(Q1,Q3)] 10.02(6.10,14.83) 11.00(8.10,16.03) -1.190 0.234 中性粒细胞/[×109,M(Q1,Q3)] 8.78(5.22,13.60) 9.03(6.15,13.30) -0.359 0.719 淋巴细胞/[×109,M(Q1,Q3)] 0.60(0.32,1.00) 0.54(0.30,1.43) -0.197 0.844 血小板/[×109,M(Q1,Q3)] 151.0(109.5,214.5) 176.7(90.0,253.0) -0.678 0.497 红细胞压积/[M(Q1,Q3)] 0.36(0.31,0.41) 0.35(0.28,0.40) -0.898 0.369 PCT分级/例(%) 5.176 0.159 < 0.5 ng/mL 38(16.7) 1(2.7) 0.5~ < 2.0 ng/mL 41(18.1) 7(18.9) 2.0~ < 10.0 ng/mL 42(18.5) 9(24.3) ≥10.0 ng/mL 106(46.7) 20(54.1) 血尿素氮/[mmol/L,M(Q1,Q3)] 7.30(5.22,11.25) 13.80(5.77,20.74) -3.244 0.001 血肌酐/[μmol/L,M(Q1,Q3)] 95.0(72.5,155.0) 250.9(75.0,304.5) -2.033 0.042 谷丙转氨酶/[U/L,M(Q1,Q3)] 26.0(16.5,49.0) 57.2(15.5,42.5) -0.789 0.430 谷草转氨酶/[U/L,M(Q1,Q3)] 32.0(21.0,54.0) 35.0(22.0,95.0) -1.129 0.259 总胆红素/[μmol/L,M(Q1,Q3)] 15.00(9.35,24.85) 11.90(7.60,25.75) -0.949 0.343 直接胆红素/[μmol/L,M(Q1,Q3)] 5.90(3.40,11.40) 5.70(3.55,11.05) -0.164 0.870 白蛋白/[g/L,M(Q1,Q3)] 36.0(32.0,40.0) 34.0(26.3,38.0) -2.300 0.021 住院天数≥30 d/例(%) 23(10.8) 3(9.7) 0.036 0.850 表 2 28 d死亡预后单因素和多因素logistic回归分析
临床资料 单因素分析 多因素分析 OR(95%CI) P OR(95%CI) P 性别 男 - 女 0.431(0.213~0.872) 0.019 0.690(0.308~1.550) 0.369 病原体分类 0.362 0.639 革兰阴性菌 - 革兰阳性菌 1.648(0.829~3.277) 0.154 0.664(0.285~1.550) 0.344 真菌 1.275×1010(0.000-) 0.999 1.547×1010(0.000-) 0.999 感染部位 0.025 0.030 泌尿系统 - 呼吸系统 9.842(2.846~34.042) <0.001 9.501(2.516~35.880) 0.001 上、下消化管道 9.048(1.829~44.753) 0.007 7.841(1.386~44.344) 0.020 肝胆系统 2.533(0.401~15.993) 0.323 1.150(0.109~12.168) 0.908 导管相关 8.636(1.550~48.121) 0.014 4.875(0.693~34.283) 0.111 神经系统 10.556(1.472~75.710) 0.019 21.822(2.510~189.695) 0.005 骨关节及皮肤软组织 10.566(1.852~60.150) 0.008 9.073(1.316~62.535) 0.025 其他 4.524(0.415~49.361) 0.216 5.141(0.403~65.512) 0.207 白蛋白 0.936(0.891~0.983) 0.008 0.940(0.890~0.993) 0.027 血尿素氮 1.004(0.993~1.014) 0.503 1.001(0.979~1.024) 0.911 血肌酐 1.002(1.000~1.003) 0.008 1.002(1.000~1.003) 0.054 -
[1] 上海市微生物学会临床微生物学专业委员会, 上海市医学会检验医学专科分会, 上海市医学会危重病专科分会. 血流感染临床检验路径专家共识[J]. 中华传染病杂, 2022, 40(8): 457-475. doi: 10.3760/cma.j.cn311365-20220130-00033
[2] Vincent JL, Sakr Y, Singer M, et al. Prevalence and Outcomes of Infection Among Patients in Intensive Care Units in 2017[J]. JAMA, 2020, 323(15): 1478-1487. doi: 10.1001/jama.2020.2717
[3] Rhee C, Dantes R, Epstein L, et al. Incidence and Trends of Sepsis in US Hospitals Using Clinical vs Claims Data, 2009-2014[J]. JAMA, 2017, 318(13): 1241-1249. doi: 10.1001/jama.2017.13836
[4] 李永凯, 李丹丹, 袁新, 等. 早期乳酸/白蛋白比值对脓毒症预后的预测价值[J]. 中华危重病急救医学, 2023, 35(1): 61-65.
[5] 张静静, 金旭婷, 李若寒, 等. ICU住院期间平均血清白蛋白水平和患者预后的相关性分析——一项多中心回顾性队列研究[J]. 中国急救医学, 2022, 42(6): 476-480. doi: 10.3969/j.issn.1002-1949.2022.06.003
[6] 金魁, 王玉兰, 汪跃国, 等. 不同感染部位脓毒症急性肾损伤发生率及相关死亡风险分析[J]. 临床急诊杂志, 2021, 22(7): 445-452. https://lcjz.whuhzzs.com/article/doi/10.13201/j.issn.1009-5918.2021.07.002
[7] 黄飞, 祁玮, 何健, 等. 感染部位与发生脓毒症肝损伤的相关性研究[J]. 临床急诊杂志, 2021, 22(10): 653-656. https://lcjz.whuhzzs.com/article/doi/10.13201/j.issn.1009-5918.2021.10.003
[8] 中华人民共和国卫生部. 医院感染诊断标准(试行)[J]. 中华医学杂志, 2001, 81(5): 314-320. doi: 10.3760/j:issn:0376-2491.2001.05.027
[9] 杨祖耀, 詹思延, 王波, 等. 中国血流感染住院病死率的系统评价和meta分析[J]. 北京大学学报(医学版), 2010, 42(3): 304-307. https://www.cnki.com.cn/Article/CJFDTOTAL-BYDB201003016.htm
[10] 陈国芹, 刘丹, 吕水林, 等. 重症监护病房患者血流感染病原菌分布、临床特点及预后危险因素分析[J]. 新乡医学院学报, 2022, 39(1): 45-50. https://www.cnki.com.cn/Article/CJFDTOTAL-XXYX202201010.htm
[11] Parize P, Muth E, Richaud C, et al. Untargeted next-generation sequencing-based first-line diagnosis of infection in immunocompromised adults: a multicentre, blinded, prospective study[J]. Clin Microbiol Infect, 2017, 23(8): 574-574.
[12] 刘韶瑜, 李姝, 姚贝, 等. 急诊社区发病的血流感染病原学与临床特征[J]. 中国急救医学, 2020, 40(12): 1147-1152. https://www.cnki.com.cn/Article/CJFDTOTAL-ZJJY202012007.htm
[13] 韩涛, 邓秋明, 万献尧. 脓毒症患者低白蛋白血症研究进展[J]. 中华医学杂志, 2017, 97(3): 228-231.
[14] 李志华, 成慧昕, 王毅, 等. 白蛋白/纤维蛋白原比值对脓毒症患者28 d死亡风险的预测价值[J]. 中华急诊医学杂志, 2023, 32(2): 180-185. https://www.cnki.com.cn/Article/CJFDTOTAL-WXHX202303016.htm
[15] 杨萌, 李丽娟, 苏楠. 革兰氏阴性菌血流感染预后危险因素分析[J]. 中日友好医院学报, 2016, 30(3): 134-136. https://www.cnki.com.cn/Article/CJFDTOTAL-ZRYH201603002.htm
[16] 马立, 李丽娟, 林江涛, 等. 革兰阳性球菌血流感染预后危险因素分析[J]. 中国呼吸与危重监护杂志, 2016, 15(1): 7-11. https://www.cnki.com.cn/Article/CJFDTOTAL-ZGHW201601003.htm
[17] Martínez ML, Ferrer R, Torrents E, et al. Impact of Source Control in Patients With Severe Sepsis and Septic Shock[J]. Crit Care Med, 2017, 45(1): 11-19.
[18] Peters-Sengers H, Butler JM, Uhel F, et al. Source-specific host response and outcomes in critically ill patients with sepsis: a prospective cohort study[J]. Intensive Care Med, 2022, 48(1): 92-102.
[19] Raith EP, Udy AA, Bailey M, et al. Prognostic Accuracy of the SOFA Score, SIRS Criteria, and qSOFA Score for In-Hospital Mortality Among Adults With Suspected Infection Admitted to the Intensive Care Unit[J]. JAMA, 2017, 317(3): 290-300.
[20] 刘慧琳, 傅义程, 郝靖欣, 等. 血清降钙素原水平和APACHEⅡ评分对老年脓毒症患者预后的预测价值分析[J]. 中华危重病急救医学, 2023, 35(1): 56-60.
[21] 盛博, 陈炜, 甄洁, 等. 入院时APACHEⅡ评分、SOFA评分及ALB水平对严重脓毒症患者预后结局的影响[J]. 热带医学杂志, 2017, 17(12): 1648-1651, 1708. https://www.cnki.com.cn/Article/CJFDTOTAL-RDYZ201712021.htm
[22] Yin M, Si L, Qin WD, et al. Predictive Value of Serum Albumin Level for the Prognosis of Severe Sepsis Without Exogenous Human Albumin Administration: A Prospective Cohort Study[J]. J Intensive Care Med, 2018, 33(12): 687-694.
-




 下载:
下载: