Predictive value of intracranial pressure combined with PCT and NSE monitoring in patients with severe craniocerebral injury
-
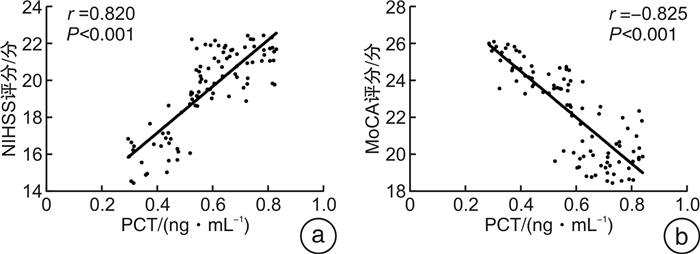
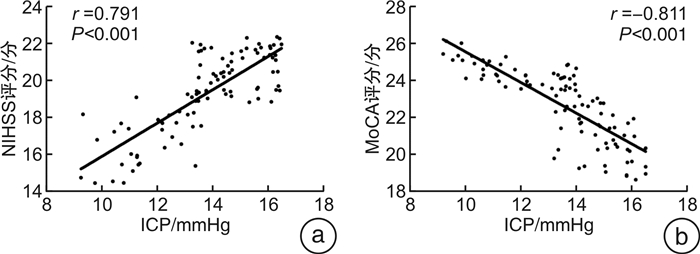
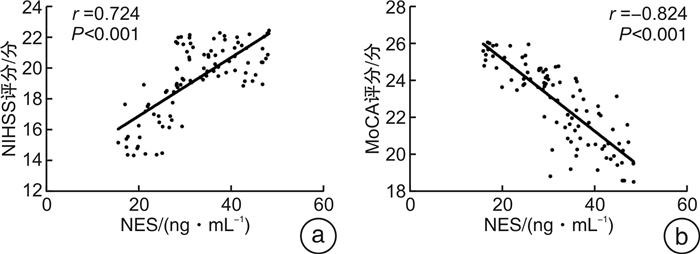
摘要: 目的 探讨颅内压(ICP)及降钙素原(PCT)、神经元特异性烯醇化酶(NSE)联合监测模式对重型颅脑损伤患者病情的预测价值及预后影响。方法 选取2020年3月—2021年3月入我院接受治疗的重型颅脑损伤患者96例作为研究对象并建立颅脑损伤组,将同期入院进行体检的37例健康受试者纳入健康对照组。观察各组ICP、PCT、NSE表达水平及神经功能缺损量表(NIHSS评分)、认知功能量表(MoCA)评分结果,对比6个月后不同预后表现患者的ICP、PCT、NSE表达水平及NIHSS评分、MoCA评分结果,ROC曲线分析ICP、PCT、NSE单项监测方式与联合监测方式对重型颅脑损伤患者病情的诊断价值,采用Pearson相关系数分析ICP、PCT、NSE指标水平与NIHSS评分、MoCA评分的相关性,采用Spearman相关系数分析颅脑损伤患者预后情况与ICP、PCT、NSE表达水平的相关性。结果 颅脑损伤轻型组、中型组、重型组患者的PCT、NSE表达水平较健康对照组均呈明显上升态势(均P < 0.05);NIHSS评分分值随着患者病情程度的加剧呈上升态势,MoCA评分分值呈下降态势(均P < 0.05);预后不良组患者ICP、PCT、NSE指标水平较预后良好组均明显升高,预后良好组NIHSS评分结果明显低于预后不良组,MoCA评分分值明显高于预后不良组(均P < 0.05);采用ROC曲线分析联合诊断曲线下面积较ICP、PCT、NSE单独检测的曲线下面积更高(AUC=0.917);Pearson相关系数分析示颅脑损伤患者ICP、PCT、NSE表达水平与NIHSS评分均呈明显正相关,与MoCA评分均呈明显负相关(均P < 0.05);Spearman相关系数分析发现颅脑损伤患者发生预后不良与ICP、PCT、NSE表达水平均呈正相关(均P < 0.05)。结论 ICP、PCT、NSE指标联合检测对临床准确鉴别重症颅脑损伤具备较高效用,且ICP、PCT、NSE表达水平变化与患者神经功能、认知功能明显相关,与颅脑损伤患者的预后呈显著相关,具有较高的临床应用价值。Abstract: Objective To investigate the predictive value and prognostic effect of ICP, PCT and NSE combined monitoring model for severe craniocerebral injury.Methods A total of 96 patients with severe craniocerebral injury admitted to our hospital from March 2020 to March 2021 were selected as the research objects and the craniocerebral injury group was established. And 37 healthy subjects admitted for physical examination during the same period were included in the healthy control group. The expression levels of ICP, PCT and NSE and the scores of National Institute of Health stroke scale(NIHSS) and Montreal cognitive assessment (MoCA) were observed. After 6 months, the expression levels of ICP, PCT and NSE and the scores of NIHSS and MoCA were compared in patients with different prognostic manifestations. ROC curve was used to analyze the diagnostic value of ICP, PCT and NSE in patients with severe craniocerebral injury by single monitoring and combined monitoring. Pearson correlation coefficient was used to analyze the correlation between ICP, PCT and NSE levels and NIHSS score and MoCA score. Spearman correlation coefficient was used to analyze the correlation between the prognosis of patients with craniocerebral injury and the expression levels of ICP, PCT and NSE.Results The expression levels of PCT and NSE in mild, moderate and severe craniocerebral injury group increased significantly than those in healthy control group(all P < 0.05); NIHSS score increased with the severity of the disease, while MoCA score decreased(all P < 0.05). ICP, PCT and NSE levels in the poor prognosis group increased significantly than those in the good prognosis group, NIHSS scores in the good prognosis group decreased significantly than those in the poor prognosis group, and MoCA scores increased significantly than those in the poor prognosis group(all P < 0.05). The area under the ROC curve was higher than that of ICP, PCT and NSE alone(AUC=0.917). The expression levels of ICP, PCT and NSE were positively correlated with NIHSS score and negatively correlated with MoCA score by Pearson correlation coefficient analysis(all P < 0.05). Spearman correlation coefficient analysis showed that the expression levels of ICP, PCT and NSE were positively correlated with poor prognosis in patients with head injury(all P < 0.05).Conclusion The combined detection of ICP, PCT and NSE has high clinical efficacy in the accurate identification of severe craniocerebral injury, and the diversity of ICP, PCT and NSE expression levels are significantly correlated with the neurological function and cognitive function of patients, and are significantly correlated with the prognostic effect of patients with craniocerebral injury, which has high clinical application value.
-
Key words:
- craniocerebral injury /
- intracranial pressure /
- procalcitonin /
- neuron-specific enolase /
- predictive value /
- prognosis
-

-
表 1 各组PCT、NSE指标表达水平对比
X±S 组别 ICP/mmHga) PCT/(ng·mL-1) NSE/(ng·mL-1) 健康对照组
(n=37)0.23± 0.06 13.46± 2.57 轻型组
(n=35)10.16± 1.03 0.77± 0.131) 58.33± 12.631) 中型组
(n=32)15.25± 1.722) 0.92± 0.171)2) 73.42± 18.611)2) 重型组
(n=29)19.32± 1.862)3) 1.83± 0.361)2)3) 109.27± 23.421)2)3) F 11.016 23.300 21.728 P < 0.001 < 0.001 < 0.001 注:a)1 mmHg=0.133 kPa。与健康对照组比较,1)P < 0.05;与轻型组比较,2)P < 0.05;与中型组比较,3)P < 0.05。 表 2 各组神经功能及认知功能缺损评分对比
分,X±S 组别 NIHSS评分 MoCA评分 轻型组(n=35) 14.17±1.53 23.82±1.46 中型组(n=32) 17.88±1.791) 19.17±1.241) 重型组(n=29) 21.03±1.951)2) 15.48±1.051)2) F 5.770 5.786 P < 0.001 < 0.001 与轻型组比较,1)P < 0.05;与中型组比较,2)P < 0.05。 表 3 颅脑损伤组内患者预后情况及各指标水平变化情况
X±S 组别 ICP/mmHg PCT/(ng·mL-1) NSE/(ng·mL-1) 预后良好组
(n=34)10.28±1.19 0.36±0.08 17.61±2.15 预后不良组
(n=62)14.82±1.67 0.68±0.16 43.16±5.29 t 14.007 10.919 26.918 P < 0.001 < 0.001 < 0.001 表 4 不同预后表现患者神经功能和认知功能缺损情况对比
分,X±S 组别 NIHSS评分 MoCA评分 预后良好组(n=34) 15.76±1.45 24.75±1.38 预后不良组(n=62) 20.63±1.81 18.68±1.26 t -13.485 21.823 P < 0.001 < 0.001 表 5 ICP、PCT、NSE及联合诊断重型颅脑损伤的价值分析
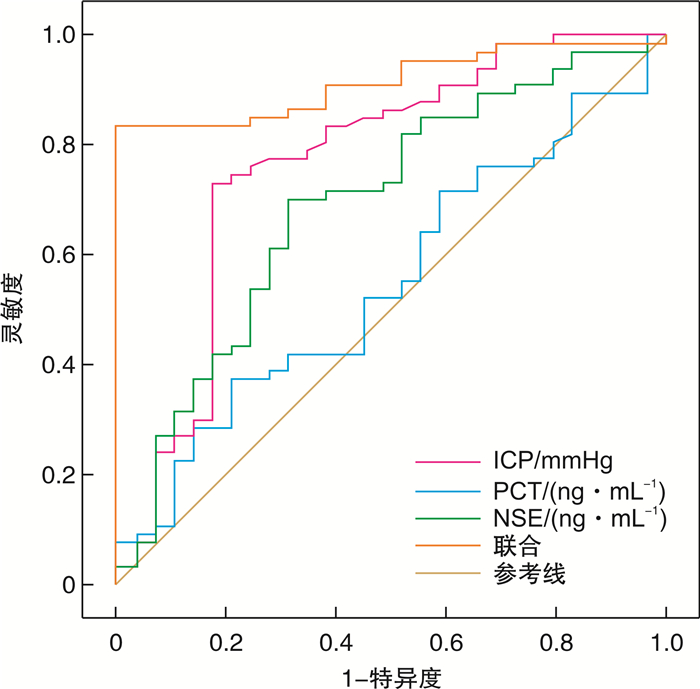
指标 AUC(95%CI) 灵敏度/% 特异度/% 约登指数 截断值 ICP 0.771(0.657~0.885) 78.500 81.000 0.595 12.621 mmHg PCT 0.551(0.429~0.674) 62.500 72.000 0.345 0.464 ng/mL NSE 0.694(0.577~0.861) 76.000 78.500 0.545 25.337 ng/mL 联合 0.917(0.862~0.971) 97.500 85.000 0.825 表 6 ICP、PCT、NSE与发生预后不良的相关性分析
指标 发生预后不良 r P ICP 0.755 < 0.001 PCT 0.715 < 0.001 NSE 0.750 < 0.001 -
[1] 叶永强, 何兰兰, 刘桂玲, 等. 重症颅脑损伤患者合并多重耐药菌肺部感染病原菌分布、影像学特征以及风险预测模型的建立与验证[J]. 中国医学科学院学报, 2022, 44(4): 636-642.
[2] 刘中平, 吴德模, 管义祥, 等. 血清ET-1、NFκB、PCT对重症颅脑外伤患者预后的预测价值[J]. 临床神经外科杂志, 2020, 17(5): 569-573.
[3] 谢晨阳, 陈秀侠. 重型颅脑损伤术中血压变异性对预后的影响[J]. 安徽医药, 2020, 24(1): 33-38.
[4] van Oers JAH, de Jong E, Kemperman H, et al. Diagnostic accuracy of procalcitonin and C-reactive protein is insufficient to predict proven infection: a retrospective cohort study in critically ill patients fulfilling the sepsis-3 criteria[J]. J Appl Lab Med, 2020, 5(1): 62-72. doi: 10.1373/jalm.2019.029777
[5] Kiiski H, Långsjö J, Tenhunen J, et al. S100B, NSE and MMP-9 fail to predict neurologic outcome while elevated S100B associates with milder initial clinical presentation after aneurysmal subarachnoid hemorrhage[J]. J Neurol Sci, 2018, 390: 129-134. doi: 10.1016/j.jns.2018.04.030
[6] 蒋颖, 毛可适, 岳春贤, 等. 长程脑电图和Glasgow昏迷量表评分对重症脑功能损伤患者预后的预测价值[J]. 临床神经病学杂志, 2018, 31(4): 257-259.
[7] Sharma D, Gandhi N. Role of platelet to lymphocyte ratio(PLR)and its correlation with NIHSS(national institute of health stroke scale)for prediction of severity in patients of acute ischemic stroke[J]. J Assoc Physicians India, 2021, 69(1): 56-60.
[8] Rose AF, Gilbertson AF, Cottrell C, et al. Cognitive screening for adult psychiatric outpatients: comparison of the Cognivue®to the Montreal Cognitive Assessment[J]. World J Psychiatry, 2021, 11(7): 265-270. doi: 10.5498/wjp.v11.i7.265
[9] 张彬, 毛小静, 冯杰. 影响颅脑创伤远期预后的因素分析[J]. 临床神经外科杂志, 2020, 17(1): 71-76.
[10] 庄汉亭, 曹维, 裘孝忠, 等. 重型颅脑损伤患者术后颅内感染病原菌及脑脊液单核细胞TLR4 mRNA与MyD88 mRNA水平[J]. 中华医院感染学杂志, 2023, 33(4): 537-541.
[11] 蒋鸿雁, 杨凤, 曹艳, 等. 2004~2013年昆明医科大学第一附属医院创伤性脑损伤流行病学特征调查[J]. 昆明医科大学学报, 2022, 43(4): 12-18.
[12] 孔庆飞, 高岭, 吕萌萌, 等. 颅脑损伤患者血清与脑脊液IL-1β及NSE水平的变化及临床意义[J]. 中国实用神经疾病杂志, 2017, 20(4): 63-65.
[13] Brennan PM, Murray GD, Teasdale GM. Simplifying the use of prognostic information in traumatic brain injury. Part 1: the GCS-Pupils score: an extended index of clinical severity[J]. J Neurosurg, 2018, 128(6): 1612-1620.
[14] 丁丽丽, 刘梦茹, 孙海军. 脑电双频指数、颅多普勒与颅内压联合监测在重度颅脑损伤预后评估中的价值[J]. 中国医药导报, 2023, 20(2): 69-71, 79.
[15] 王嘉楠. 血浆正五聚蛋白3、血清降钙素原水平对重度脑外伤病人呼吸机相关性肺炎的早期诊断价值[J]. 安徽医药, 2022, 26(9): 1831-1834, 1912.
[16] Thelin EP, Zeiler FA, Ercole A, et al. Serial sampling of serum protein biomarkers for monitoring human traumatic brain injury dynamics: a systematic review[J]. Front Neurol, 2017, 8: 300.
[17] 黄小龙, 胡齐, 黄浩. 一期双侧去骨瓣减压术对重型颅脑损伤颅内压及预后的影响[J]. 中国临床神经外科杂志, 2022, 27(3): 203-205.
[18] 高见, 张华, 刘国成, 等. 右美托咪定对重型颅脑损伤患者术后血清炎症因子和神经细胞因子水平及预后的影响[J]. 中国医药导报, 2021, 18(1): 111-114, 139.
[19] 卢毅, 聂智品, 祁向东, 等. 血清降钙素原对颅脑术后感染的诊断价值分析[J]. 中华医院感染学杂志, 2019, 29(17): 2656-2660.
[20] 孟云霞, 王小智, 康福新, 等. 重症感染患者的降钙素原与D-二聚体及病原体分析[J]. 中华医院感染学杂志, 2019, 29(16): 2414-2417, 2444.
[21] Mercier E, Tardif PA, Cameron PA, et al. Prognostic value of neuron-specific enolase(NSE)for prediction of post-concussion symptoms following a mild traumatic brain injury: a systematic review[J]. Brain Inj, 2018, 32(1): 29-40.
[22] 何金波, 毛峥嵘, 艾莘. 牛黄承气汤治疗重型颅脑损伤患者急性胃肠损伤的疗效及对血清MTL、DAO、NSE水平影响[J]. 中国实验方剂学杂志, 2022, 28(24): 131-137.
[23] 梁鑫, 李玉雄, 张凌, 等. 颅脑损伤后脑脊液NSE S100β水平动态变化与颅内压异常的关系研究[J]. 河北医学, 2017, 23(12): 2072-2076.
[24] 嵇雪莱, 李爱民, 周辉, 等. 血红蛋白水平、NLR比值与创伤性颅脑损伤早期病情判断和预后的相关性研究[J]. 徐州医科大学学报, 2022, 42(11): 812-816.
[25] 宋旭东, 罗波, 邓学云, 等. 颅脑损伤术后脑脊液HMGB1、sFas水平与交通性脑积水的关系[J]. 中国临床神经外科杂志, 2022, 27(11): 909-912, 916.
-




 下载:
下载: