Application of musculoskeletal ultrasound and interventional diagnosis and treatment in acute traumatic lesions
-
摘要: 浅表软组织、肌肉、神经和骨骼的急性创伤性病变在急诊十分常见,肌骨超声能清晰显示这些病变的范围和程度,并能精准定位和引导介入操作,将诊断和治疗结合起来,对及时明确诊断和快速缓解症状发挥着重要作用。本文主要针对肌骨超声及超声引导下的介入诊疗在急性创伤性病变中的应用范围进行介绍。Abstract: Acute traumatic lesions of superficial soft tissue, muscle, nerve and bone are very common in emergency department. Musculoskeletal ultrasound can clearly show the scope and severity of these lesions, accurately locate and guide interventional operation. Musculoskeletal ultrasound combines diagnosis and treatment, which plays an important role in timely diagnosis and rapid relief of symptoms. This study mainly introduces the application of musculoskeletal ultrasound, ultrasound-guided interventional diagnosis and their treatment in acute traumatic lesions.
-
Key words:
- musculoskeletal /
- soft tissue /
- emergency /
- ultrasonic /
- intervention
-

-
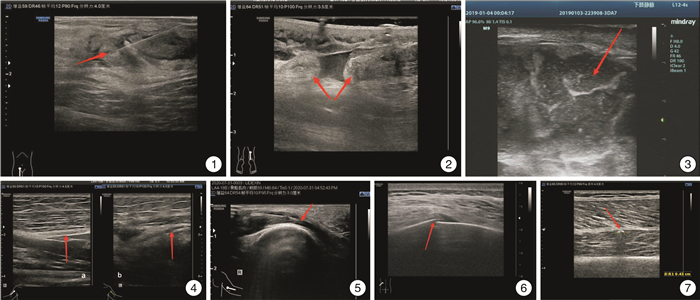
图 1 MSK US引导下右侧腹股沟区肿块下穿刺 抽出棕黄色液体约5 mL,细菌培养结果为金黄色葡萄球菌感染(红色箭头所指处为穿刺针抽吸位置); 图2 MSK US显示右侧跟腱完全断裂 断端之间可见无回声血肿,断端增厚、回缩,形成瘤样结节回声(红色箭头标记处为跟腱断端); 图3 骨筋膜室综合征 右侧小腿腘窝下方皮下层与肌肉之间可见一混合回声包块(范围约154 mm×68 mm×122 mm),形态欠规则,边界欠清,内以无回声为主,混杂光点及低回声、高回声,该处肌层显示不清、皮下软组织层明显水肿增厚(红色箭头标记处为混合回声包块); 图4 左侧桡神经创伤性损伤 左侧上臂肱骨中段处可见桡神经回声减低,结构模糊,长轴切面内径较对侧变窄,左图为右侧正常桡神经长轴切面,右图为左侧损伤桡神经长轴切面(红色箭头标记处为桡神经); 图5 MSK US引导下尺神经松解 对右侧受压的尺神经进行液压松解(红色箭头标记处为针尖位置); 图6 X线阴性骨折MSK US声像 1例肋骨骨折患者,X线显示阴性,MSK US可见患者疼痛处的肋骨高回声骨质线中断,周边软组织肿胀,呈低回声(红色箭头标记处为肋骨骨折处); 图7 异物识别 1例鸟枪中伤腿部的患者,MSK US检查显示左股肌层的异物——左股肌层内见圆弧形强回声(红色箭头标记处为残留子弹)。
-
[1] 顾鹏, 李峰, 刘颖, 等. 重复扩展创伤重点超声评估技术在急诊ICU的应用价值[J]. 临床急诊杂志, 2021, 22(6): 373-376. https://www.cnki.com.cn/Article/CJFDTOTAL-ZZLC202106003.htm
[2] Osterwalder J, Tamborrini G. CME sonography 100: emergency ultrasound of the soft tissues and the musculoskeletal system[J]. Praxis, 2021, 110(9): 488-507. doi: 10.1024/1661-8157/a003712
[3] 吕发勤, 黎檀实. 微型超声在肢体战伤"黄金1小时"救治中的应用前景[J]. 临床急诊杂志, 2017, 18(10): 726-728. https://www.cnki.com.cn/Article/CJFDTOTAL-ZZLC201710003.htm
[4] Yoo J, Kang SY, Jo IJ, et al. The use of point-of-care ultrasound in emergency medical centers in Korea: a national cross-sectional survey[J]. J Korean Med Sci, 2021, 36(21): e141. doi: 10.3346/jkms.2021.36.e141
[5] Acuña J, Rubin M, Hahn B, et al. Point-of-care ultrasound in United States pediatric emergency medicine fellowship programs: the current state of practice and training[J]. Pediatr Emerg Care, 2021, 37(12): e1181-e1185. doi: 10.1097/PEC.0000000000001955
[6] De Ranieri D, Lin S. Applications of musculoskeletal ultrasound in the pediatric emergency department[J]. Pediatr Ann, 2021, 50(10): e411-e418.
[7] Altmayer S, Verma N, Dicks EA, et al. Imaging musculoskeletal soft tissue infections[J]. Semin Ultrasound CT MRI, 2020, 41(1): 85-98. doi: 10.1053/j.sult.2019.09.005
[8] Kolinsky DC, Liang SY. Musculoskeletal Infections in the Emergency Department[J]. Emerg Med Clin North Am, 2018, 36(4): 751-766. doi: 10.1016/j.emc.2018.06.006
[9] Labied M, Salam S, Jabri S, et al. Morel-lavallee syndrome: a rare tumefactive lesion[J]. Eur J Case Rep Intern Med, 2020, 7(12): 001910.
[10] Annison DR, Smith M. Identification and triage of a Morel-Lavallée lesion using point of care ultrasound[J]. Ultrasound, 2022, 30(1): 85-89. doi: 10.1177/1742271X211001901
[11] Perone MV, Yablon CM. Musculoskeletal ultrasound in the emergency department: is there a role?[J]. Semin Roentgenol, 2021, 56(1): 115-123. doi: 10.1053/j.ro.2020.09.004
[12] Rosskopf AB, Taljanovic MS, Sconfienza LM, et al. Pulley, flexor, and extensor tendon injuries of the hand[J]. Semin Musculoskelet Radiol, 2021, 25(2): 203-215. doi: 10.1055/s-0041-1727196
[13] Chambers G, Kraft J, Kingston K. The role of ultrasound as a problem-solving tool in the assessment of paediatric musculoskeletal injuries[J]. Ultrasound, 2019, 27(1): 6-19. doi: 10.1177/1742271X18759807
[14] Chang KV, Wu WT, Özçakar L. Ultrasound imaging and rehabilitation of muscle disorders: Part 1. Traumatic injuries[J]. Am J Phys Med Rehabil, 2019, 98(12): 1133-1141. doi: 10.1097/PHM.0000000000001307
[15] Lawrence JE, Nasr P, Fountain DM, et al. Functional outcomes of conservatively managed acute ruptures of the Achilles tendon[J]. Bone Joint J, 2017, 99-B(1): 87-93. doi: 10.1302/0301-620X.99B1.BJJ-2016-0452.R1
[16] Mohammadrezaei N, Seyedhosseini J, Vahidi E. Validity of ultrasound in diagnosis of tendon injuries in penetrating extremity trauma[J]. Am J Emerg Med, 2017, 35(7): 945-948. doi: 10.1016/j.ajem.2017.01.059
[17] Park D, Kim YC, Cho SH, et al. Interrupted incision fasciotomy for acute compartment syndrome after extracorporeal membrane oxygenation: surgical technique with a report of two cases[J]. Orthop Surg, 2022, 14(1): 169-173. doi: 10.1111/os.13177
[18] Paoletta M, Moretti A, Liguori S, et al. Ultrasound imaging in sport-related muscle injuries: pitfalls and opportunities[J]. Medicina, 2021, 57(10): 1040. doi: 10.3390/medicina57101040
[19] Jara R, Castillo C, Valdés M, et al. Acute compartment syndrome as a complication of cutaneous loxoscelism mainly edematous[J]. Rev Chilena Infectol, 2020, 37(2): 175-178. doi: 10.4067/s0716-10182020000200175
[20] Wijntjes J, Borchert A, van Alfen N. Nerve ultrasound in traumatic and iatrogenic peripheral nerve injury[J]. Diagnostics(Basel), 2020, 11(1): 30.
[21] Forte AJ, Boczar D, Oliver JD, et al. Ultra-high-frequency ultrasound to assess nerve fascicles in Median nerve traumatic neuroma[J]. Cureus, 2019, 11(6): e4871.
[22] Strakowski JA, Chiou-Tan FY. Musculoskeletal ultrasound for traumatic and torsional alterations[J]. Muscle Nerve, 2020, 62(6): 654-663. doi: 10.1002/mus.27025
[23] Chianca V, Di Pietto F, Zappia M, et al. Musculoskeletal Ultrasound in the emergency department[J]. Semin Musculoskelet Radiol, 2020, 24(2): 167-174. doi: 10.1055/s-0039-3402050
[24] Champagne N, Eadie L, Regan LK, et al. The effectiveness of ultrasound in the detection of fractures in adults with suspected upper or lower limb injury: a systematic review and subgroup meta-analysis[J]. BMC Emerg Med, 2019, 19(1): 17. doi: 10.1186/s12873-019-0226-5
[25] Waterbrook AL, Adhikari S, Stolz U, et al. The accuracy of point-of-care ultrasound to diagnose long bone fractures in the ED[J]. Am J Emerg Med, 2013, 31(9): 1352-1356. doi: 10.1016/j.ajem.2013.06.006
[26] Lee SH, Yun SJ. Diagnostic performance of ultrasonography for detection of pediatric elbow fracture: a meta-analysis[J]. Ann Emerg Med, 2019, 74(4): 493-502. doi: 10.1016/j.annemergmed.2019.03.009
[27] 赵丽, 赵胜军, 徐洪. 高频超声在急诊创伤骨折中诊断价值研究[J]. 临床军医杂志, 2018, 46(7): 759-762, 766. https://www.cnki.com.cn/Article/CJFDTOTAL-JYGZ201807008.htm
[28] Simard R. Ultrasound imaging of orthopedic injuries[J]. Emerg Med Clin North Am, 2020, 38(1): 243-265. doi: 10.1016/j.emc.2019.09.009
[29] 江凌, 崔立刚. 肌骨超声在急危重症中的应用[J]. 中华诊断学电子杂志, 2018, 6(2): 73-76. https://www.cnki.com.cn/Article/CJFDTOTAL-ZDDZ201802001.htm
[30] Buonsenso D, Chiaretti A, Curatola A, et al. Pediatrician performed point-of-care ultrasound for the detection of ingested foreign bodies: case series and review of the literature[J]. J Ultrasound, 2021, 24(1): 107-114. doi: 10.1007/s40477-020-00452-z
[31] White RZ, Rezaian P, Parasuramar A, et al. Ultrasound-assisted foreign body extraction(U-SAFE): review of technique and technical pearls[J]. J Med Imaging Radiat Oncol, 2022, 66(3): 362-369. doi: 10.1111/1754-9485.13313
[32] Tesch C. Focused sonography in orthopedic emergencies[J]. Med Klin Intensivmed Notfmed, 2018, 113(8): 631-637. doi: 10.1007/s00063-018-0486-y
[33] PoSaw LL, Wubben BM, Bertucci N, et al. Teaching emergency ultrasound to emergency medicine residents: a scoping review of structured training methods[J]. J Am Coll Emerg Physicians Open, 2021, 2(3): e12439.
-




 下载:
下载: