Relationship between the optic nerve sheath diameter measured by point-of-care ultrasonography and postoperative intracranial pressure in patients with severe craniocerebral injury
-
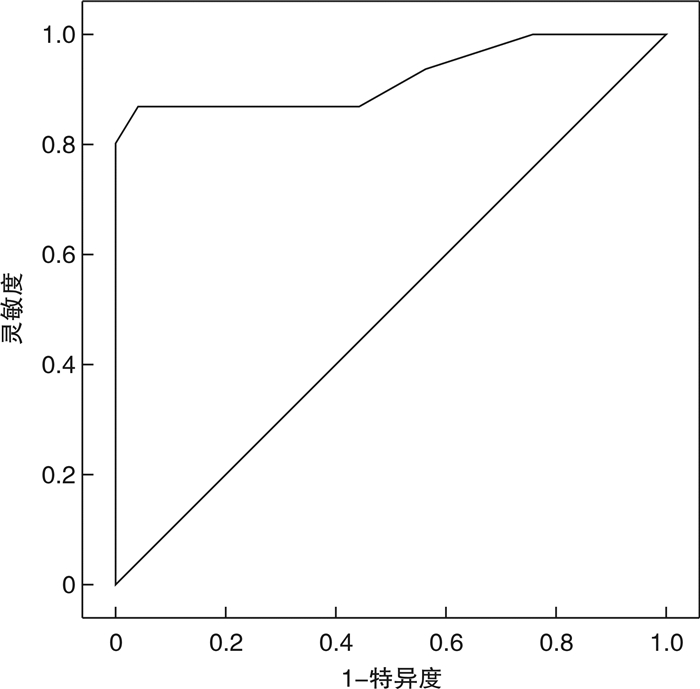
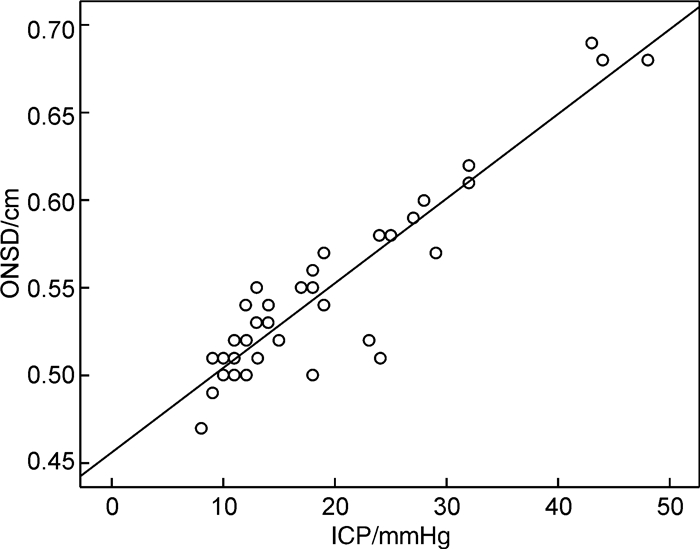
摘要: 目的 探讨床旁即时超声测量视神经鞘直径(ONSD)与重型颅脑损伤患者术后颅内压(ICP)增高的关系。方法 选取兰溪市人民医院急诊科2018年6月-2021年6月收治的重型颅脑损伤患者62例,均行手术治疗,将其按照患者术后ICP值分为3组。ICP值>25 mmHg组:13例,15~25 mmHg组:20例,<15 mmHg组:29例。应用床旁即时超声测量各组ONSD值,比较3组ONSD值的差异,使用Pearson分析ONSD和ICP间的关系,并通过ROC曲线分析ONSD评估术后ICP增高的准确性。结果 ICP值>25 mmHg组和15~25 mmHg组的ICP值、ONSD值均显著高于ICP值<15 mmHg组,差异均有统计学意义(P<0.05);ICP值>25 mmHg组ICP值、ONSD值显著高于15~25 mmHg组,差异均有统计学意义(P<0.05);且3组30°头高位ONSD值均低于平卧位,3组使用甘露醇后30 min ONSD值均低于使用甘露醇前,差异均有统计学意义(P<0.05)。通过Pearson分析相关性显示,床旁即时超声测量ONSD随着重型颅脑损伤患者术后ICP增高而增大,二者间呈正相关(r=0.875,P<0.01)。通过ROC曲线分析显示,ONSD评估重型颅脑损伤患者术后ICP增高(ICP值>20 mmHg)最佳临界值为5.45 mm,95%CI:0.870~0.992,AUC值为0.931,特异度为92.50%,灵敏度为81.82%。结论 ONSD可随着重型颅脑损伤患者术后ICP增高而增大,床旁即时超声测量ONSD作为无创、便捷的ICP监测方式,可良好地反映ICP增高水平,值得应用。Abstract: Objective To investigate the relationship between optic nerve sheath diameter(ONSD) measured by point-of-care ultrasound and postoperative intracranial pressure(ICP) in patients with severe traumatic brain injury.Methods A total of 62 patients with severe craniocerebral injury who were treated in our hospital from June 2018 to June 2021 were selected, all of them received surgical treatment, and they were divided into: ICP value>25 mmHg group(13 cases), In the 15 to 25 mmHg group(20 cases) and the < 15 mmHg group(29 cases). The ONSD value of each group was measured by point-of-care ultrasound, and the difference in ONSD value among the three groups was compared. The relationship between ONSD and ICP was analyzed by Pearson, and the accuracy of ONSD in assessing postoperative ICP increase was analyzed by ROC curve.Results In ICP value > 25 mmHg group and 15 to 25 mmHg group, ICP value and ONSD value were significantly higher than those in < 15 mmHg group; ICP value and ONSD value in ICP value > 25 mmHg group were significantly higher than those in 15 to 25 mmHg group, and the ONSD values of the three groups 30° head high were lower than those in the supine position, and the ONSD values 30 minutes after the use of mannitol in the three groups were lower than those before the use of mannitol, and the difference was significant (P < 0.05). The correlation analysis by Pearson showed that the ONSD measured by point-of-care ultrasound increased with the increase of postoperative ICP in patients with severe traumatic brain injury, and there was a positive correlation between the two (r=0.875, P < 0.01). The ROC curve analysis showed that the optimal critical value of ONSD to evaluate postoperative ICP increase in patients with severe craniocerebral injury (ICP value greater than 20 mmHg) was 5.45 mm, the 95%CI value was 0.870-0.992, and the AUC value was 0.931, with 92.50% specificity and 81.82% sensitivity respectively.Conclusion ONSD can increase with the increase of postoperative ICP in patients with severe craniocerebral injury. As a non-invasive and convenient ICP monitoring method, the bedside real-time ultrasound measurement of ONSD can well reflect the increased level of ICP and is worthy of application.
-

-
表 1 两组基本资料比较
例,X±S 组别 例数 性别 年龄/岁 损伤部位 男 女 额颞顶部 颞顶部 额颞部 >25 mmHg组 13 7 6 42.51±4.46 4 6 3 15~25 mmHg组 20 12 8 42.32±4.27 6 10 4 <15 mmHg组 29 16 13 42.09±4.52 8 15 6 P 0.800 0.549 0.719 表 2 3组患者ONSD值与ICP值比较
X±S 组别 ICP值>25 mmHg组 15~25 mmHg组 <15 mmHg组 例数 13例 20例 29例 ICP值/mmHg 42.32±4.78 19.31±2.45 10.07±2.05 ONSD值/cm 30°头高位 0.62±0.051) 0.54±0.041) 0.45±0.031) 平卧位 0.67±0.04 0.56±0.05 0.48±0.04 使用甘露醇前30 min 0.68±0.05 0.58±0.06 0.50±0.04 使用甘露醇后30 min 0.60±0.062) 0.52±0.052) 0.47±0.052) 与平卧位比较,1)P<0.05;与甘露醇使用前30 min比较,2)P<0.05。 -
[1] 黄先锋, 林小祥, 李剑侠. 重型颅脑损伤病人去骨瓣减压术后早期行颅骨修补的疗效及脑血流动力学变化[J]. 临床外科杂志, 2021, 29(10): 919-924. doi: 10.3969/j.issn.1005-6483.2021.10.007
[2] 王忠, 张瑞剑, 韩志桐, 等. 持续颅内压及脑组织氧分压监测在重度颅脑损伤患者治疗中的应用[J]. 中华危重症医学, 2021, 33(4): 449-454.
[3] 王思博, 邢英琦, 王翠翠, 等. 经颅多普勒超声及超声测量视神经鞘直径与脑炎患者颅内压增高的相关性[J]. 中国脑血管病杂志, 2020, 17(6): 315-319. doi: 10.3969/j.issn.1672-5921.2020.06.006
[4] 蔡俊红, 周建, 张铁耀, 等. 颅脑CT和床旁超声在重型颅脑损伤去骨瓣减压术后监测中的应用[J]. 中国临床神经外科杂志, 2020, 25(1): 7-9. https://www.cnki.com.cn/Article/CJFDTOTAL-ZGLC202001005.htm
[5] 徐万忠, 王晓麒. 床旁超声与颅脑CT在重型颅脑损伤去骨瓣减压的对比研究[J]. 重庆医学, 2018, 47(18): 2498-2500. doi: 10.3969/j.issn.1671-8348.2018.18.028
[6] 王蕾, 朱保锋, 张毅, 等. 急诊头痛患者视神经鞘直径与颅内压相关性研究[J]. 临床急诊杂志, 2020, 21(1): 25-28, 33. http://zzlc.cbpt.cnki.net/WKC/WebPublication/paperDigest.aspx?paperID=09d4f4db-d7c5-4766-ba94-122ac79977b6
[7] 杜雨森, 王文杰, 冯顺易, 等. 视神经鞘直径预测心搏骤停患者预后的meta分析[J]. 临床急诊杂志, 2020, 21(10): 826-831. http://zzlc.cbpt.cnki.net/WKC/WebPublication/paperDigest.aspx?paperID=1baeb65d-94c1-4f02-b8a8-d44d0a54abf1
[8] 张频捷, 曹利军, 陈虎, 等. 视神经鞘直径预测重症脑损伤患者死亡风险的价值[J]. 中华急诊医学杂志, 2021, 30(7) : 836-840.
[9] Wang J, Li K, Li H, et al. Ultrasonographic optic nerve sheath diameter correlation with ICP and accuracy as a tool for noninvasive surrogate ICP measurement in patients with decompressive craniotomy[J]. J Neuro Surg, 2020, 133(2): 514-520.
[10] Wang LJ, Chen HX, Chen Y, et al. Optic nerve sheath diameter ultrasonography for elevated intracranial pressure detection[J]. Ann Clin Transl Neurol, 2020, 7(5): 865-868. doi: 10.1002/acn3.51054
[11] 同济大学上海市第十人民医院神经外科第四版重型颅脑损伤救治指南翻译组. 重型颅脑损伤救治指南第四版[J]. 中华神经创伤外科电子杂志, 2016, 2(5): 1-96. https://www.cnki.com.cn/Article/CJFDTOTAL-SJCW201706001.htm
[12] Hawryluk G, Rubiano AM, Totten AM, et al. Guidelines for the Management of Severe Traumatic Brain Injury: 2020 Update of the Decompressive Craniectomy Recommendations[J]. Neurosurgery, 2020, 87(3): 427-434. doi: 10.1093/neuros/nyaa278
[13] 欧阳龙强, 夏文燕, 汪春晖, 等. 去骨瓣减压术后早期颅骨修补术对颅脑创伤患者神经功能和认知功能的影响[J]. 中国现代神经疾病杂志, 2020, 20(7): 620-624. doi: 10.3969/j.issn.1672-6731.2020.07.011
[14] 李永磊, 杨玉升, 黄建华, 等. 颅内压检测及脑脊液乳酸水平对重型颅脑损伤患者预后预测研究[J]. 创伤外科杂志, 2019, 21(5): 384-387. doi: 10.3969/j.issn.1009-4237.2019.05.014
[15] 陈常兴, 俞康龙, 刘毅. 视神经鞘直径早期评估颅脑损伤的价值[J]. 中华急诊医学杂志, 2018, 27(2): 208-211. doi: 10.3760/cma.j.issn.1671-0282.2018.02.020
[16] 吴志萍, 吴丹, 任江艳, 等. 侧俯卧位结合床头抬高对重型颅脑损伤患者颅内压的影响研究[J]. 中国药物与临床, 2020, 20(23): 3997-3999. https://www.cnki.com.cn/Article/CJFDTOTAL-YWLC202023055.htm
[17] 郭慧, 许宁, 申张顺, 等. 床旁超声视神经鞘宽度联合颅内血流测量评估心肺复苏术后患者颅内压增高的价值研究[J]. 中国临床医学影像杂志, 2021, 32(7): 461-465. https://www.cnki.com.cn/Article/CJFDTOTAL-LYYX202107002.htm
[18] 王忠, 张瑞剑, 韩志桐, 等. 持续颅内压监测在重度颅脑损伤及脑出血合并脑疝患者标准大骨瓣减压术及显微血肿清除术后的应用[J]. 中国医药导报, 2020, 17(5): 75-78+82. https://www.cnki.com.cn/Article/CJFDTOTAL-YYCY202005020.htm
[19] 杜洁, 邓岩军, 何晓昕, 等. 视神经鞘直径与眼球横径比值评估颅脑损伤患者颅内压的价值: 超声法确定[J]. 中华麻醉学杂志, 2018, 38(11): 1369-1387. https://www.cnki.com.cn/Article/CJFDTOTAL-DEJD200510023.htm
[20] 胡述立, 汤浩, 范学朋, 等. 超声测量视神经鞘直径评估俯卧位通气时颅内压的变化[J]. 实用医学杂志, 2018, 34(9): 1520-1523. https://www.cnki.com.cn/Article/CJFDTOTAL-SYYZ201809030.htm
-




 下载:
下载: