Correlation between serum HBP and severity of organ injury and clinical outcome in patients with sepsis
-
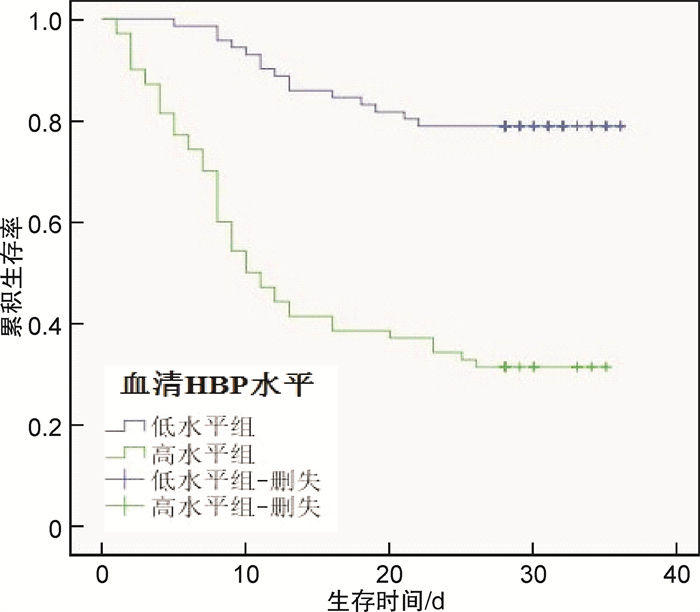
摘要: 目的 分析脓毒症患者血清肝素结合蛋白(HBP)与器官损伤和临床结局的关系。方法 选取2017年3月-2020年4月期间我院重症监护病房(ICU)招募了141例脓毒症患者。于诊断24 h内采集静脉血,采用酶联免疫吸附试验检测血清HBP水平。以为30 d院内死亡主要观察终点。结果 脓毒症患者血清HBP水平为281.46(161.99~409.60) ng/mL。谷丙转氨酶>40.00 U/L、序贯器官衰竭估计量表>11分及急性生理及慢性健康系统Ⅱ>24分的患者血清HBP水平更高(P < 0.05)。高水平组发生心功能障碍、急性肾损伤(AKI)的患者例数更多(P < 0.001)。24 h内外周灌注指数(PI) < 1.4脓毒症患者的血清HBP水平显著高于PI≥1.4(P < 0.001);同时24 h内毛细血管充盈试验(CRT)≥3 s的患者血清HBP水平也显著高于CRT < 3 s者(P < 0.001)。Kaplan-Meier分析(Log-rank检验)显示血清HBP低水平者30 d院内生存率(χ2=12.566,P < 0.001)更高。此外,单因素及多因素COX回归分析的结果显示,血清HBP水平仍然是影响脓毒症患者30 d内院内死亡的独立预后因子(P < 0.001)。结论 血清HBP水平升高与脓毒症患者心功能障碍及AKI发生相关,同时血清HBP对脓毒症患者的短期预后预测有良好价值,值得临床应用。Abstract: Objective To analyze the relationship between serum heparin-binding protein(HBP)and organ injury and clinical outcome in patients with sepsis.Methods A total of 141 patients with sepsis were recruited from the intensive care unit(ICU)of our hospital from March 2017 to April 2020.Venous blood was collected within 24 hours of diagnosis, and serum HBP level was detected by enzyme-linked immunosorbent assay.It was the main endpoint of in-hospital death in 30 days.Results The level of serum HBP in patients with sepsis was 281.46(161.99, 409.60) ng/mL.Patients with alanine aminotransferase>40.00 U/L, Sequential Organ Failure Assessment>11 points and acute physiology and chronic health evaluationⅡ>24 points had higher serum HBP levels(P>0.05).There were more cases of cardiac dysfunctionand acute kidney injury(AKI)in the high level group(P>0.001).Serum HBP level in sepsis patients with 24 h perfusion Index(PI) < 1.4 was significantly higher than PI≥1.4(P < 0.001);Meanwhile, the serum HBP level of patients with 24hcapillary filling test(CRT)≥3 s was significantly higher than that of patients with CRT≥3 s(P < 0.001).Kaplan-Meier analysis(log-rank test)showed the 30 d hospital survival rate of patients with low serum HBP level(χ2=12.566, P < 0.001) higher.In addition, univariate and multivariate COX regression analysis showed that serum HBP level was still an independent prognostic factor for in-hospital death within 30 days of sepsis(P < 0.001).Conclusion The increase of serum HBP level is related to cardiac dysfunction and AKI in patients with sepsis.Meanwhile, serum HBP has good value in predicting the short-term prognosis of patients with sepsis and is worthy of clinical application.
-
Key words:
- sepsis /
- heparin binding protein /
- organ injury /
- clinical outcome /
- acute kidney injury /
- cardiac dysfunction
-

-
表 1 脓毒症患者血清HBP水平与临床病理特征的相关性
例(%) 临床病理特征 例数 血清HBP水平 χ2 P 低水平组(71例) 高水平组(70例) 年龄/岁 ≤60 80 37(52.11) 43(61.43) 1.246 0.264 >60 61 34(47.89) 27(38.57) 性别 男 86 45(63.38) 41(58.57) 0.343 0.558 女 55 26(36.62) 29(41.43) 体重/kg ≤70 80 38(53.52) 42(60.00) 0.603 0.438 >70 61 33(46.48) 28(40.00) 从出现症状至入住ICU时间/h ≤3 78 41(57.75) 37(52.86) 0.341 0.559 >3 63 30(42.25) 33(47.14) 感染原因 肺炎 53 28(39.44) 25(35.71) 腹部感染 39 18(25.35) 21(30.00) 0.428 0.934 泌尿道感染 29 15(21.13) 14(20.00) 其他部位感染 20 10(14.08) 10(14.29) 糖尿病史 否 121 63(88.73) 58(82.86) 0.999 0.317 是 20 8(11.27) 12(17.14) 冠心病史 否 123 65(91.55) 58(82.86) 2.391 0.122 是 18 6(8.45) 12(17.14) 高脂血症史 否 109 53(74.65) 56(80.00) 0.576 0.448 是 32 18(25.35) 14(20.00) 慢性阻塞性肺疾病 否 111 57(80.28) 54(77.14) 0.207 0.649 是 30 14(19.72) 16(22.86) MAP/mmHg ≤82.33 70 37(52.11) 33(47.14) 0.348 0.555 >82.33 71 34(47.89) 37(52.86) PaO2/FiO2 ≤258.62 71 36(50.70) 35(50.00) 0.007 0.933 >258.62 70 35(49.30) 35(50.00) TBIL/(μmol·L-1) ≤17.10 77 36(50.70) 41(58.57) 0.880 0.348 >17.10 64 35(49.30) 29(41.43) ALB/(g·L-1) ≤35.00 120 60(84.51) 60(85.71) 0.041 0.841 >35.00 21 11(15.49) 10(14.29) ALT/(U·L-1) ≤40.00 80 47(66.20) 33(47.14) 5.214 0.022 >40.00 61 24(33.80) 37(52.86) BUN/(mg·dL-1) ≤1.20 64 33(46.48) 31(44.29) 0.117 0.733 >1.20 74 36(50.70) 38(54.29) SCr/(mg·dL-1) ≤71 71 38(53.52) 33(47.14) 0.574 0.449 >71 70 33(46.48) 37(52.86) 尿量/(mL·kg-1·h-1) ≤0.50 52 25(35.21) 27(38.57) 0.171 0.679 >0.50 89 46(64.79) 43(61.43) PLT ≤100×109/L 70 34(47.89) 36(51.43) 0.177 0.674 >100×109/L 71 37(52.11) 34(48.57) WBC ≤10.0×109/L 50 27(38.03) 23(32.86) 0.412 0.521 >10.0×109/L 91 44(61.97) 47(67.14) CRP/(mg·dL-1) ≤10 46 18(25.35) 28(40.00) 3.441 0.064 >10 95 53(74.65) 42(60.00) PCT/(ng·mL-1) ≤0.50 8 2(2.82) 6(8.57) 2.181 0.140 >0.50 133 69(97.18) 64(91.43) 血糖/(mmol·L-1) ≤6.10 39 23(32.39) 16(22.86) 1.602 0.206 >6.10 102 48(67.61) 54(77.14) 动脉血乳酸/(mmol·L-1) ≤2.00 74 43(60.56) 31(44.29) 3.433 0.064 >2.00 66 28(67.61) 38(54.29) APACHEⅡ/分 ≤24 78 48(67.61) 30(42.86) 8.734 0.003 >24 63 23(32.39) 40(57.14) SOFA评分/分 ≤11 84 53(74.65) 31(44.29) 13.491 < 0.001 >11 57 18(25.35) 39(55.71) 表 2 血清HBP水平与脓毒性休克及器官损伤的相关性
例(%) 组别 例数 脓毒性休克 器官功能障碍 无休克 休克 严重休克 心功能 呼吸功能 AKI 凝血功能 肝功能 低水平组 71 2(2.82) 68(95.77) 1(1.41) 10(14.08) 17(23.94) 4(5.63) 34(47.89) 14(19.71) 高水平组 70 3(4.29) 67(95.71) 0 26(37.14) 18(25.71) 27(38.57) 36(51.43) 11(15.71) t/χ2 1.200 9.857 0.059 22.291 0.177 0.387 P 0.549 0.002 0.808 < 0.001 0.674 0.534 表 3 单因素及多因素COX回归分析脓毒症患者30d内院内死亡的影响因素
影响因素 单因素 多因素 OR(95%CI) P OR(95%CI) P 年龄 1.013(0.998~1.028) 0.088 性别 1.029(0.621~1.705) 0.910 体重 0.991(0.976~1.005) 0.216 从出现症状至入住ICU时间 0.971(0.892~1.057) 0.499 感染原因 1.022(0.812~1.286) 0.855 糖尿病史 1.356(0.707~2.600) 0.359 冠心病史 1.228(0.606~2.488) 0.568 高脂血症史 1.290(0.732~2.276) 0.379 慢性阻塞性肺疾病 1.166(0.644~2.112) 0.612 MAP 1.010(0.999~1.023) 0.086 PaO2/FiO2 0.999(0.997~1.001) 0.434 TBIL 0.992(0.979~1.006) 0.254 ALB 1.023(0.978~1.069) 0.319 ALT 1.000(0.999~1.001) 0.911 BUN 1.033(1.002~1.065) 0.038 1.015(0.975~1.056) 0.476 SCr 1.006(1.002~1.010) 0.002 1.002(0.998~1.007) 0.372 尿量 0.852(0.595~1.220) 0.383 PLT 0.998(0.995~1.001) 0.150 WBC 1.015(0.990~1.040) 0.239 CRP 0.995(0.972~1.019) 0.701 PCT 1.001(0.995~1.007) 0.741 血糖 1.029(0.965~1.099) 0.382 动脉血乳酸 1.166(1.004~1.355) 0.044 1.014(0.844~1.218) 0.881 APACHEⅡ 1.095(1.058~1.133) < 0.001 1.085(1.029~1.144) 0.003 SOFA评分 1.130(1.057~1.207) < 0.001 0.912(0.819~1.015) 0.091 血清HBP水平 1.004(1.003~1.005) < 0.001 1.004(1.00~1.015) < 0.001 -
[1] 张晓慧, 郭娜, 宁海慧, 等. Nrf2及其信号通路在脓毒症相关脏器损伤中的研究进展[J]. 中国急救医学, 2022, 42(1): 81-86. https://www.cnki.com.cn/Article/CJFDTOTAL-ZJJY202201017.htm
[2] Wang C, Liang G, Shen J, et al. Long Non-Coding RNAs as Biomarkers and Therapeutic Targets in Sepsis[J]. Front Immunol, 2021, 12: 722004. doi: 10.3389/fimmu.2021.722004
[3] Pierrakos C, Velissaris D, Bisdorff M, et al. Biomarkers of sepsis: time for a reappraisal[J]. Crit Care, 2020, 24(1): 287. doi: 10.1186/s13054-020-02993-5
[4] 邓俊超, 赵芳丽, 乔莉娜. 肝素结合蛋白对儿童重症感染诊断价值的前瞻性研究[J]. 中国当代儿科杂志, 2022, 24(1): 85-89. https://www.cnki.com.cn/Article/CJFDTOTAL-DDKZ202201012.htm
[5] 张重威, 罗茜, 曹彦, 等. 有潜力的脓毒症生物标志物: 肝素结合蛋白[J]. 中国急救医学, 2021, 41(10): 916-921. doi: 10.3969/j.issn.1002-1949.2021.10.017
[6] Singer M, Deutschman CS, Seymour CW, et al. The Third International Consensus Definitions for Sepsis and Septic Shock(Sepsis-3)[J]. JAMA, 2016, 315(8): 801-810. doi: 10.1001/jama.2016.0287
[7] 张志忠, 王国兴, 杨立沛. 休克指数对急诊严重脓毒症和脓毒性休克预后评估的意义[J]. 中华急诊医学杂志, 2015, 24(2): 147-150. https://www.cnki.com.cn/Article/CJFDTOTAL-HAIN201717035.htm
[8] 黄伟. 《第三版脓毒症与感染性休克定义国际共识》解读[J]. 中国实用内科杂志, 2016, 36(11): 959-962. https://www.cnki.com.cn/Article/CJFDTOTAL-SYNK201611012.htm
[9] 感染诱发的老年多器官功能障碍综合征诊断与治疗中国指南2019[J]. 中华老年多器官疾病杂志, 2019, 18(11): 801-838.
[10] Hernández G, Ospina-Tascón GA, Damiani LP, et al. Effect of a Resuscitation Strategy Targeting Peripheral Perfusion Status vs Serum Lactate Levels on 28-Day Mortality Among Patients With Septic Shock: The ANDROMEDA-SHOCK Randomized Clinical Trial[J]. JAMA, 2019, 321(7): 654-664. doi: 10.1001/jama.2019.0071
[11] Ait-Oufella H, Bakker J. Understanding clinical signs of poor tissue perfusion during septic shock[J]. Intensive Care Med, 2016, 42(12): 2070-2072. doi: 10.1007/s00134-016-4250-6
[12] Lima AP, Beelen P, Bakker J. Use of a peripheral perfusion index derived from the pulse oximetry signal as a noninvasive indicator of perfusion[J]. Crit Care Med, 2002, 30(6): 1210-1213. doi: 10.1097/00003246-200206000-00006
[13] 谭扬扬, 杨旭凯, 蔡高平, 等. 血清淀粉样蛋白A对成人脓毒症诊断价值的Meta分析[J]. 中国急救医学, 2022, 42(1): 35-40. https://www.cnki.com.cn/Article/CJFDTOTAL-ZJJY202201008.htm
[14] Ludwig KR, Hummon AB. Mass spectrometry for the discovery of biomarkers of sepsis[J]. Mol Biosyst, 2017, 13(4): 648-664. doi: 10.1039/C6MB00656F
[15] Huang M, Cai S, Su J. The pathogenesis of sepsis and potential therapeutic targets[J]. Int J Mol Sci, 2019, 20(21): 5376.
[16] 刘俊, 湛允波, 刘献志. 肝素结合蛋白在开颅术后早期颅内感染的诊断价值[J]. 中国微侵袭神经外科杂志, 2021, 26(3): 114-117. https://www.cnki.com.cn/Article/CJFDTOTAL-ZWQX202103008.htm
[17] Yang Y, Liu G, He Q, et al. A Promising Candidate: Heparin-Binding Protein Steps onto the Stage of Sepsis Prediction[J]. J Immunol Res, 2019, 2019: 7515346.
[18] Caraballo C, Jaimes F. Organ Dysfunction in Sepsis: An Ominous Trajectory From Infection To Death[J]. Yale J Biol Med, 2019, 92(4): 629-640.
[19] Xue M, Zeng Y, Qu HQ, et al. Heparin-binding protein levels correlate with aggravation and multiorgan damage in severe COVID-19[J]. ERJ Open Res, 2021, 7(1): 00741-2020.
[20] Tverring J, Nielsen N, Dankiewicz J, et al. Repeated measures of Heparin-binding protein(HBP)and procalcitonin during septic shock: biomarker kinetics and association with cardiovascular organ dysfunction[J]. Intensive Care Med Exp, 2020, 8(1): 51.
[21] Poston JT, Koyner JL. Sepsis associated acute kidney injury[J]. BMJ, 2019, 364: k4891.
-




 下载:
下载: