Value of bedside pulmonary ultrasound in real-time dynamic evaluation of the severity of the pneumonia in critically ill patients
-
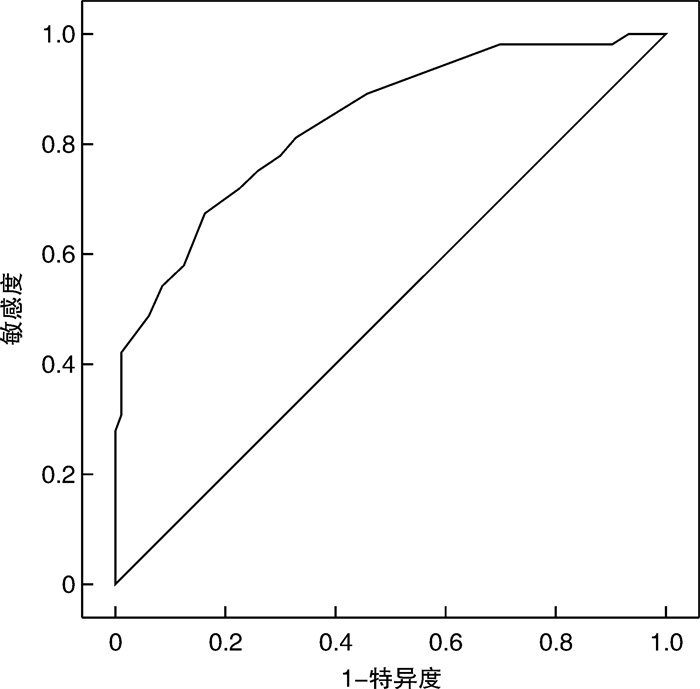
摘要: 目的 探讨床旁肺超声实时动态评估危重症患者肺炎病情严重程度的应用价值。方法 选取我院135例危重症肺炎患者,根据急性生理与慢性健康评分Ⅱ(APACHE Ⅱ)分为低危组(45例)、中危组(50例)、高危组(40例),比较3组间肺超声评分(LUS)、氧合指数(OI)、肺泡-动脉氧分压差(A-aDO2)、临床肺部感染评分(CPIS)、序贯器官衰竭评分(SOFA); 分析LUS与上述各指标间的相关性。根据临床结局分为死亡组(55例)和存活组(80例),比较两组间LUS的差异变化,采用ROC曲线评价LUS的临床诊断效能,并找出LUS预测危重症患者肺炎死亡的临床诊断分界值。结果 高危组LUS、A-aDO2、CPIS及SOFA均高于中危组和低危组,而中危组均高于低危组; 高危组OI则低于中危组和低危组,且中危组低于低危组,比较结果均差异有统计学意义(P< 0.05)。LUS与A-aDO2、CPIS及SOFA呈线性正相关(r=0.729,P< 0.01;r=0.641,P< 0.05;r=0.627,P< 0.05);与OI呈显著线性负相关(r=-0.756,P< 0.01)。死亡组LUS明显高于存活组,差异有显著统计学意义(P< 0.01)。LUS预测危重症肺炎患者死亡的曲线下面积(AUC)为0.839,预测敏感度为78.2%,特异度为84.8%,LUS为21.5作为预测危重症患者肺炎死亡的临床诊断分界值。结论 床旁LUS与危重症患者肺炎病情严重程度存在相关性,可用于实时动态评估患者的病情及预后判断。Abstract: Objective To explore the value of bedside pulmonary ultrasound in real-time dynamic evaluation of the severity of pneumonia in critically ill patients.Methods One hundred and thirty five patients with severe pneumonia in our hospital were divided into low-risk group(45 cases), medium-risk group(50 cases) and high-risk group(40 cases) according to acute physiology and chronic health score Ⅱ(APACHE Ⅱ). Lung ultrasound score(LUS), oxygenation index(OI), alveolar-arterial oxygen differential pressure(A-aDO2), clinical pulmonary infection score(CPIS) and sequential organ failure score(SOFA) were compared among the three groups; analyzing the correlation between LUS and the above indicators. According to the clinical outcome, patients were divided into death group (55 cases) and survival group (80 cases) with LUS compared the two groups were compared. The clinical diagnostic efficacy of LUS was evaluated by ROC curve, and the clinical diagnostic boundary value of LUS in predicting pneumonia death in critically ill patients was found.Results LUS, A-aDO2, CPIS and SOFA in high-risk group were higher than those in other two groups, while those in medium-risk group were higher than those in low-risk group; the OI of high-risk group was lower than that of other two groups, and the OI of medium-risk group was lower than that of low-risk group(P< 0.05). LUS was positively correlated with A-aDO2, CPISand SOFA(r=0.729,P< 0.01;r=0.641,P< 0.05;r=0.627,P< 0.05)and negatively correlated with OI(r=-0.756,P< 0.01). LUS in death group was significantly higher than that in survival group(P< 0.01). The area under the curve(AUC) of LUS for predicting the death of critically ill patients with pneumonia was 0.839, with the prediction sensitivity and specificity of 78.2% and 84.8% respectively; and the LUS value was 21.5 as the clinical diagnostic boundary value for predicting the death of critically ill patients with pneumonia.Conclusion Bedside LUS is correlated with the severity of pneumonia in critically ill patients, which can be used for real-time dynamic evaluation of patients' condition and prognosis.
-
Key words:
- lung ultrasound score /
- critically ill /
- pneumonia /
- severity
-

-
表 1 3组患者LUS及临床指标比较
X±S 参数 低危组(45例) 中危组(50例) 高危组(40例) F P LUS/分 15.93±2.59 20.00±3.87 25.33±4.78 9.258 0 OI/mmHg 112.00±18.68 98.26±13.55 77.00±17.20 16.532 0 A-aDO2/mmHg 304.73±44.20 348.58±56.61 366.28±75.48 12.527 0 CPIS/分 7.91±0.87 8.10±1.13 9.65±1.12 7.113 0.022 SOFA/分 5.69±1.02 6.28±0.88 7.25±0.93 6.564 0.026 注:1 mmHg=0.133 kPa。 -
[1] Ramsay KA, Sandhu H, Geake JB, et al. The changing prevalence of pulmonary infection in adults with cystic fibrosis: A longitudinal analysis[J]. J Cyst Fibros, 2017, 16(1): 70-77. doi: 10.1016/j.jcf.2016.07.010
[2] 陈炎, 陈亚蓓, 陶荣芳. 《NICE 2014成人肺炎指南》要点分析[J]. 中国实用内科杂志, 2016, 36(S1): 59-60. https://www.cnki.com.cn/Article/CJFDTOTAL-SYNK2016S1016.htm
[3] 张磊, 俞万钧, 马坚. 超声在肺部疾病中的临床应用[J]. 中国医学影像技术, 2017, 33(4): 608-611. https://www.cnki.com.cn/Article/CJFDTOTAL-ZYXX201704045.htm
[4] 中华医学会呼吸病学分会感染学组. 中国成人医院获得性肺炎与呼吸机相关性肺炎诊断和治疗指南(2018年版)[J]. 中华结核和呼吸杂志, 2018, 41(4): 255-280. doi: 10.3760/cma.j.issn.1001-0939.2018.04.006
[5] Monastesse A, Girard F, Massicotte N, et al. Lung Ultrasonography for the assessment of perioperative atelectasis: A pilot feasibility study[J]. Anesth Analg, 2017, 124(2): 494-504. doi: 10.1213/ANE.0000000000001603
[6] Alyami M, Passot G, Voiglio E, et al. Feasibility of catheter placement under ultrasound guidance for progressive preoperative pneumoperitoneum for large incisional hernia with loss of domain[J]. World J Surg, 2015, 39(12): 1-7.
[7] Dietrich CF, Mathis G, Blaivas M, et al. Lung B-line artefacts and their use[J]. J Thorac Dis, 2016, 8(6): 1356-1365. doi: 10.21037/jtd.2016.04.55
[8] 王敏佳, 龚仕金, 严静, 等. 肺部超声B线数目与血管外肺水的相关性分析[J]. 浙江医学, 2016, 38(2): 109-111. https://www.cnki.com.cn/Article/CJFDTOTAL-ZJYE201602014.htm
[9] Guerra M, Crichiutti G, Pecile P, et al. Ultrasound detection of pneumonia in febrile children with respiratory distress: a prospective study[J]. Eur J Pediatr, 2015, 175(2): 163-170.
[10] 李虹, 李一丹, 吕秀章, 等. 肺超声联合超声心动图评价左心衰患者的临床研究[J]. 中国超声医学杂志, 2016, 32(8): 696-699. doi: 10.3969/j.issn.1002-0101.2016.08.008
[11] Mongodi S, Via G, Girard M, et al. Lung ultrasound for early diagnosis of ventilator-associated pneumonia[J]. Chest, 2016, 149(4): 969-980. doi: 10.1016/j.chest.2015.12.012
[12] 郭凤梅, 邱海波, 杨毅. 重症超声在急性呼吸窘迫综合征检查中的应用[J]. 中华诊断学电子杂志, 2018, 6(2): 35-37. https://www.cnki.com.cn/Article/CJFDTOTAL-ZDDZ201802009.htm
[13] 张运玮, 曹春艳, 张进祥. 心肺联合超声结合临床评估在急诊科诊断急性心衰的研究[J]. 临床急诊杂志, 2021, 22(8): 553-557. http://zzlc.cbpt.cnki.net/WKC/WebPublication/paperDigest.aspx?paperID=067b7e30-958f-4ac2-8738-9ede55c01d8a
[14] 刘莹, 邓西龙, 潘越峻, 等. 肺部超声评估重症肺炎严重程度及预后的价值[J]. 实用医学杂志, 2018, 34(12): 2074-2078. doi: 10.3969/j.issn.1006-5725.2018.12.038
[15] 肖虹, 蒲婷婷, 刘宇, 等. 肺部超声和床旁胸部X线检查在诊断老年社区获得性肺炎的对比性研究[J]. 临床急诊杂志, 2021, 22(5): 319-324. http://zzlc.cbpt.cnki.net/WKC/WebPublication/paperDigest.aspx?paperID=aa5cd2e4-f06b-4ef2-a38c-7d01e72dc0dc
[16] Poitou C, Denis M, Chakhtoura Z, et al. Just the tip of the iceberg: difficulties in assessing and managing extreme obesity in routine clinical care[J]. Eur J Clin Nutri, 2018, 72(3): 452-454. doi: 10.1038/s41430-017-0056-z
[17] 李莲花, 杨倩, 李黎明, 等. 肺部超声评分评估急性呼吸窘迫综合征患者病情严重程度及预后的价值[J]. 中华危重病急救医学, 2015, 27(7): 579-584. doi: 10.3760/cma.j.issn.2095-4352.2015.07.008
[18] 张磊, 陶洋, 姚丽娜, 等. 肺超声评分在急性呼吸窘迫综合征患者早期病情评估中的应用[J]. 中国现代医生, 2019, 57(1): 28-32. https://www.cnki.com.cn/Article/CJFDTOTAL-ZDYS201901008.htm
[19] Siddiqui S, Chua M, Kumaresh V, et al. A comparison of pre ICU admission SIRS, EWS and q SOFA scores for predicting mortality and length of stay in ICU[J]. J Crit Care, 2017, 41(10): 191-193.
[20] 刘兴钊, 胡青茂, 胡永, 等. 床旁超声在机械通气重症肺炎患者中的应用价值[J]. 临床超声医学杂志, 2020, 22(12): 948-950. doi: 10.3969/j.issn.1008-6978.2020.12.026
[21] 邹健, 戴吉, 钱晴, 等. 肺部超声评分与重症肺炎患者病情进展的相关性[J]. 临床超声医学杂志, 2021, 23(3): 208-211. doi: 10.3969/j.issn.1008-6978.2021.03.017
[22] 王倩倩, 蔚文龙, 宋先斌, 等. 超声对危重症患者肺炎治疗效果的评估价值[J]. 中华急诊医学杂志, 2020, 29(2): 275-278. doi: 10.3760/cma.j.issn.1671-0282.2020.02.0032
-




 下载:
下载: