Predictive value of interleukin-10 to lymphocyte ratio combined with sequential organ failure assessment score for 28-day mortality risk in patients with septic shock
-
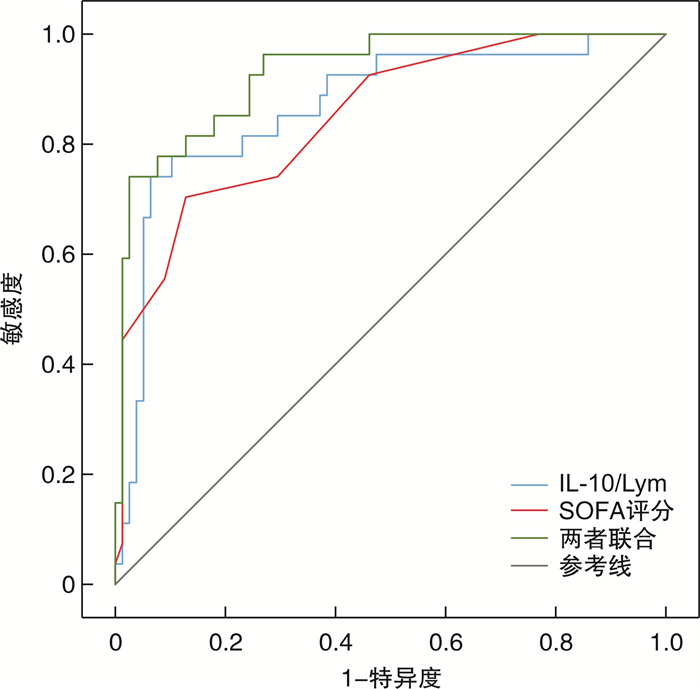
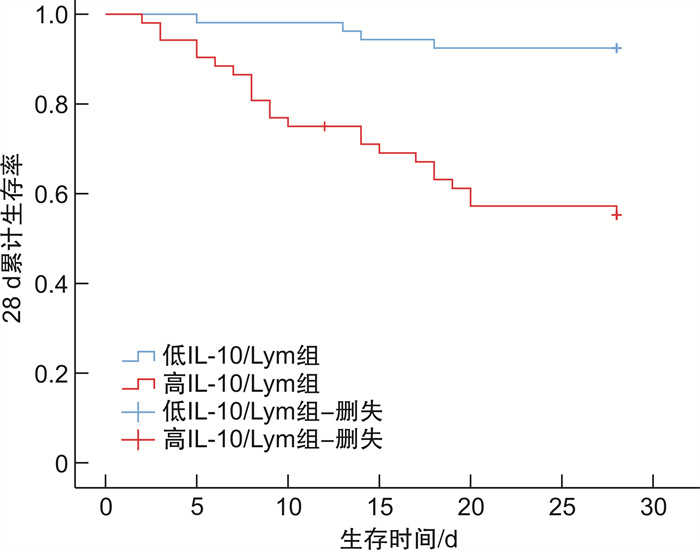
摘要: 目的 探讨白细胞介素-10与淋巴细胞比值(IL-10/Lym)联合序贯器官衰竭估计(SOFA)评分对脓毒性休克患者28 d死亡风险的预测价值,以期为临床医生对脓毒性休克患者不良预后的早期评估提供帮助。方法 纳入2020年1月—2021年9月期间海南医学院第二附属医院急诊重症监护室(EICU)收治的脓毒性休克患者105例,收集患者的临床资料及检测IL-10和Lym水平,并计算IL-10/Lym值。根据28 d预后情况,将患者分为死亡组(27例)和存活组(78例)。比较两组患者的临床资料以及IL-10、Lym和IL-10/Lym水平。采用多因素Cox比例风险回归模型探究脓毒性休克患者28 d死亡的影响因素。通过受试者工作特征曲线(ROC)评价各指标在预测脓毒性休克患者28 d死亡风险中的应用价值。结果 脓毒性休克患者在本研究中的28 d病死率为25.7%(27/105)。死亡组患者年龄、SOFA评分、急性生理学与慢性健康状况Ⅱ(APACHE Ⅱ)评分、IL-10、IL-10/Lym和血乳酸(Lac)与存活组相比明显升高,差异具有统计学意义(P< 0.05)。Kalpan-Meier分析显示,低IL-10/Lym组比高IL-10/Lym组具有较高的生存优势(χ2=14.491,P< 0.001)。多因素Cox比例风险回归模型分析结果显示,年龄>65岁(HR=3.599,95%CI:1.373~9.434,P=0.009)、IL-10/Lym(HR=1.041,95%CI:1.014~1.070,P=0.003)和SOFA评分(HR=1.474,95%CI:1.201~1.808,P< 0.001)是脓毒性休克患者28 d死亡独立影响因素。ROC曲线分析结果显示,IL-10/Lym联合SOFA评分预测脓毒性休克患者28 d死亡风险的AUC明显高于两个指标单独预测(0.931 vs.0.869,Z=2.129,P< 0.05;0.931 vs.0.850,Z=2.604,P< 0.05)。当IL-10/Lym最佳截断值为27.5 ng·10-9时,其诊断敏感度为74.13%,特异度为93.62%;当SOFA评分最佳截断值为10分时,其诊断敏感度为70.41%,特异度为87.24%。结论 IL-10/Lym和SOFA评分值升高是脓毒性休克患者28 d死亡的独立危险因素,两者联合检测在预测脓毒性休克患者的28 d死亡风险方面具有较好的临床价值。
-
关键词:
- 白细胞介素-10与淋巴细胞比值 /
- 序贯器官衰竭估计评分 /
- 脓毒性休克 /
- 预测价值 /
- 病死率
Abstract: Objective To investigate the predictive value of interleukin-10 to lymphocyte ratio(IL-10/Lym) combined with sequential organ failure assessment(SOFA) score for 28-day mortality risk in patients with septic shock, to provide help for clinical physicians to make the early assessment of poor prognosis of patients with septic shock.Methods One hundred and five patients with septic shock treated in the emergency intensive care unit(EICU) of the Second Affiliated Hospital of Hainan Medical College from January 2020 to September 2021 were enrolled. The clinical data of the patients were collected, the levels of IL-10 and Lym were detected, and the IL-10/Lym values were calculated. The patients were divided into the death group(n=27) and the survival group(n=78), according to the 28-day prognosis. The clinical data and the levels of IL-10, Lym and IL-10/Lym were compared between the two groups. Multivariate Cox proportional hazards regression model was performed to explore the influencing factors of 28-day mortality in patients with septic shock. Receiver operating characteristic curve(ROC) was applied to evaluate the application value of various indicators for predicting 28-day mortality risk in patients with septic shock.Results The 28-day mortalityof patients with septic shock in this study was 25.7%(27/105). The age, SOFA score, acute physiology and chronic health evaluation Ⅱ(APACHE Ⅱ) score, IL-10, IL-10/Lym and serum lactic acid(Lac) in the death group were significantly higher than those in the survival group, and the differences were statistically significant(P< 0.05). Kalpan-Meier analysis showed that the low IL-10/Lym group had a higher survival advantage than the high IL-10/Lym group(χ2=14.491,P< 0.001). Multivariate Cox proportional hazards regression model analysis showed that age over 65 years(HR=3.599, 95%CI: 1.373-9.434,P=0.009), IL-10/Lym(HR=1.041, 95%CI: 1.014-1.070,P=0.003) and SOFA score(HR=1.474, 95%CI: 1.201-1.808,P< 0.001) were independent influencing factors for 28-day mortality in patients with septic shock. ROC curve analysis showed that the area under the curve(AUC) of IL-10/Lym combined with SOFA score for predicting 28-day mortality risk in patients with septic shock was significantly larger than that of IL-10/Lym or SOFA score alonely(0.931 vs. 0.869,Z=2.129,P< 0.05; 0.931 vs. 0.850,Z=2.604,P< 0.05). The optimal cut-off value of IL-10/Lym was 27.5 ng·10-9, and the sensitivity and specificity were 74.13% and 93.62%, respectively. The optimal cut-off value of SOFA score was 10 points, and the sensitivity and specificity were 70.41% and 87.24%, respectively.Conclusion Elevated value of IL-10/Lym and SOFA score are independent risk factors for 28-day mortality in patients with septic shock, and IL-10/Lym combined with SOFA score had a good clinical value for predicting 28-day mortality risk in patients with septic shock. -

-
表 1 两组患者的临床资料比较
例(%),X±S,M(P25,P75) 指标 存活组(78例) 死亡组(27例) Z/t/χ2 P 性别/例 0.230 0.631 男 45 17 女 33 10 年龄/岁 60.36±12.08 68.70±8.69 -3.320 0.001 年龄>65岁 25(32.05) 20(74.07) 14.463 < 0.001 BMI 25.56±4.34 24.69±3.84 0.927 0.356 发病至入EICU时间/h 5.14±2.55 5.22±2.69 -0.152 0.880 SOFA评分/分 8.69±1.76 11.82±2.32 -7.293 < 0.001 APACHEⅡ评分/分 17.21±5.54 23.00±7.76 -4.203 < 0.001 基础疾病 慢性心衰 10(12.82) 4(14.81) 0.069 0.793 高血压 20(25.64) 9(33.33) 0.594 0.441 糖尿病 12(15.38) 6(22.22) 0.660 0.416 COPD 10(12.82) 5(18.52) 0.532 0.466 脑血管疾病 17(21.79) 8(29.63) 0.679 0.410 感染部位 1.514 0.679 肺部感染 32(41.03) 10(37.04) 泌尿系感染 18(23.08) 4(14.81) 腹腔感染 24(30.77) 11(40.74) 其他 4(5.13) 2(7.41) WBC/(×109·L-1) 15.03±8.40 15.51±8.88 0.252 0.851 Neu/(×109·L-1) 12.88±7.41 14.34±8.76 -0.840 0.403 Lym/(×109·L-1) 0.99±0.52 0.79±0.58 1.629 0.111 PCT/(μg·L-1) 4.76(1.67,13.91) 5.84(2.01,15.32) -0.851 0.395 CRP/(mg·L-1) 26.75(21.98,38.55) 27.70(23.80,57.75) -0.792 0.428 Lac/(mmol·L-1) 1.70(1.00,2.40) 2.30(1.70,3.80) -2.682 0.007 IL-10/(ng·L-1) 8.48(6.15,11.91) 15.62(9.25,33.84) -4.492 < 0.001 IL-10/Lym/(ng·10-9) 9.87(5.85,14.91) 32.67(23.45,45.10) -5.697 < 0.001 注:COPD为慢性阻塞性肺疾病。 表 2 脓毒性休克患者28 d死亡影响因素的多因素Cox比例风险回归模型分析
项目 β SE Wald χ2 HR 95%CI P 年龄>65岁 1.281 0.492 6.784 3.599 1.373~9.434 0.009 SOFA评分 0.388 0.104 13.803 1.474 1.201~1.808 < 0.001 APACHEⅡ评分 -0.501 0.042 1.500 0.950 0.875~1.031 0.221 Lac -0.198 0.121 2.673 0.820 0.646~1.050 0.102 IL-10 0.031 0.020 2.430 1.032 0.992~1.073 0.119 IL-10/Lym 0.041 0.014 8.626 1.041 1.014~1.070 0.003 表 3 SOFA评分、IL-10/Lym及两者联合对脓毒性休克患者28 d死亡风险的ROC曲线分析
指标 AUC 95%CI 临界值 敏感度/% 特异度/% 约登指数 IL-10/Lym 0.869 0.789~0.927 27.5 ng·10-9 74.13 93.62 0.677 SOFA评分 0.850 0.767~0.912 10分 70.41 87.24 0.576 联合检测 0.931 0.865~0.971 - 74.07 97.44 0.715 -
[1] Seymour CW, Liu VX, Iwashyna TJ, et al. Assessment of Clinical Criteria for Sepsis: For the Third International Consensus Definitions for Sepsis and Septic Shock(Sepsis-3)[J]. JAMA, 2016, 315(8): 762-774. doi: 10.1001/jama.2016.0288
[2] Scheer CS, Kuhn SO, Fuchs C, et al. Do Sepsis-3 Criteria Facilitate Earlier Recognition of Sepsis and Septic Shock? A Retrospective Cohort Study[J]. Shock, 2019, 51(3): 306-311. doi: 10.1097/SHK.0000000000001177
[3] 任娜, 刘名胜, 周森. 液体复苏前后外周灌注指数水平对脓毒性休克患者28 d死亡风险预测价值的研究[J]. 临床急诊杂志, 2021, 22(6): 377-382. http://zzlc.cbpt.cnki.net/WKC/WebPublication/paperDigest.aspx?paperID=4f02dc04-8a22-400a-853c-0dadff2131c7
[4] Cheng Z, Abrams S, Toh J, et al. The Critical Roles and Mechanisms of Immune Cell Death in Sepsis[J]. Front Immunol, 2020, 11(1): 1918.
[5] Maddux AB, Hiller TD, Overdier KH, et al. Innate Immune Function and Organ Failure Recovery in Adults With Sepsis[J]. J Intensive Care Med, 2019, 34(6): 486-494. doi: 10.1177/0885066617701903
[6] 苏明华, 杨鹏, 宋孟龙, 等. 脓毒性休克患者肿瘤坏死因子-α白细胞介素-10与血清降钙素原动态变化相关关系研究[J]. 中国急救医学, 2018, 38(9): 757-760. doi: 10.3969/j.issn.1002-1949.2018.09.002
[7] 杨建伟, 张玲, 龚微娜, 等. 脓毒性休克患者淋巴细胞计数的临床意义分析[J]. 临床急诊杂志, 2020, 21(1): 55-58. http://zzlc.cbpt.cnki.net/WKC/WebPublication/paperDigest.aspx?paperID=7bcc53d6-f7d5-4ef4-a98c-17c169fc2f4d
[8] 赵永祯, 梅雪, 贾育梅, 等. 序贯器官衰竭评分联合可溶性程序性死亡因子-1对脓毒症患者的预后评估价值[J]. 中国急救医学, 2020, 40(12): 1177-1181. doi: 10.3969/j.issn.1002-1949.2020.12.012
[9] Bauer M, Gerlach H, Vogelmann T, et al. Mortality in sepsis and septic shock in Europe, North America and Australia between 2009 and 2019-results from a systematic review and meta-analysis[J]. Crit Care, 2020, 24(1): 239. doi: 10.1186/s13054-020-02950-2
[10] Hernández G, Ospina-Tascón GA, Damiani LP, et al. Effect of a Resuscitation Strategy Targeting Peripheral Perfusion Status vs Serum Lactate Levels on 28-Day Mortality Among Patients With Septic Shock: The ANDROMEDA-SHOCK Randomized Clinical Trial[J]. JAMA, 2019, 321(7): 654-664. doi: 10.1001/jama.2019.0071
[11] 梁欢, 苗常青, 吴梦茹, 等. 中性粒细胞与淋巴细胞比值对脓毒性休克患者28 d死亡风险的预测价值评估[J]. 临床急诊杂志, 2019, 20(7): 503-508. http://zzlc.cbpt.cnki.net/WKC/WebPublication/paperDigest.aspx?paperID=55c41be6-8150-466e-978e-f47ba1f55340
[12] Lee GT, Hwang SY, Park JE, et al. Diagnostic accuracy of lactate levels after initial fluid resuscitation as a predictor for 28 day mortality in septic shock[J]. Am J Emerg Med, 2021, 46: 392-397. doi: 10.1016/j.ajem.2020.10.020
[13] 蒋政宇, 卞金俊, 邓小明. 免疫反应代谢调控: 脓毒症研究的新方向[J]. 中华危重病急救医学, 2019, 31(1): 122-125. doi: 10.3760/cma.j.issn.2095-4352.2019.01.025
[14] 郭伟, 李平, 陈翠, 等. 脓毒症诱导T细胞功能紊乱及免疫治疗进展[J]. 临床急诊杂志, 2020, 21(9): 758-762. http://zzlc.cbpt.cnki.net/WKC/WebPublication/paperDigest.aspx?paperID=5bed3f4b-7e39-4b82-803d-9e8589c4191f
[15] Wang G, Li X, Zhang L, et al. Crosstalk between Dendritic Cells and Immune Modulatory Agents against Sepsis[J]. Genes, 2020, 11(3): 1-6.
[16] Cao C, Yu M, Chai Y. Pathological alteration and therapeutic implications of sepsis-induced immune cell apoptosis[J]. Cell Death Dis, 2019, 10(10): 782. doi: 10.1038/s41419-019-2015-1
[17] Adrie C, Lugosi M, Sonneville R, et al. Persistent lymphopenia is a risk factor for ICU-acquired infections and for death in ICU patients with sustained hypotension at admission[J]. Ann Intensive Care, 2017, 7(1): 30. doi: 10.1186/s13613-017-0242-0
[18] 赵雪峰, 魏秀华. 脓毒血症患者血清IL-6以及IL-10的表达及对免疫功能的影响[J]. 中国实验诊断学, 2017, 21(2): 279-281. doi: 10.3969/j.issn.1007-4287.2017.02.032
[19] 王明禄, 刘名胜, 邢柏, 等. 血清冷诱导RNA结合蛋白与脓毒性休克患者病情严重程度及预后的相关性[J]. 中国急救医学, 2021, 41(2): 117-121. https://www.cnki.com.cn/Article/CJFDTOTAL-ZJJY202102005.htm
[20] 郝翠平, 胡庆河, 朱丽娜, 等. 血乳酸和降钙素原与病情严重程度评分对脓毒性休克患者短期预后的联合预测价值[J]. 中华危重病急救医学, 2021, 33(3): 281-285. doi: 10.3760/cma.j.cn121430-20201113-00715
[21] 李骥轩, 傅强. 不同序贯器官衰竭评分方式对重症监护病房感染患者预后评估的意义[J]. 中国中西医结合急救杂志, 2021, 28(1): 43-47. doi: 10.3969/j.issn.1008-9691.2021.01.011
[22] 杨亚南, 邵换璋, 史源, 等. 肝素结合蛋白联合SOFA评分对脓毒性休克的预测价值[J]. 中华危重病急救医学, 2019, 31(3): 336-340. doi: 10.3760/cma.j.issn.2095-4352.2019.03.015
[23] Khwannimit B, Bhurayanontachai R, Vattanavanit V. Comparison of the accuracy of three early warning scores with SOFA score for predicting mortality in adult sepsis and septic shock patients admitted to intensive care unit[J]. Heart Lung, 2019, 48(3): 240-244.
-




 下载:
下载: