Disinfection effects of 2% chlorhexidine alcohol spray on mice abdominal surgical incision: a randomized controlled trial
-
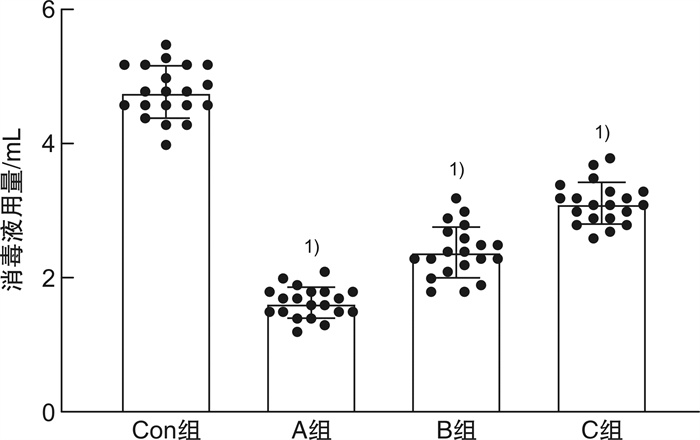
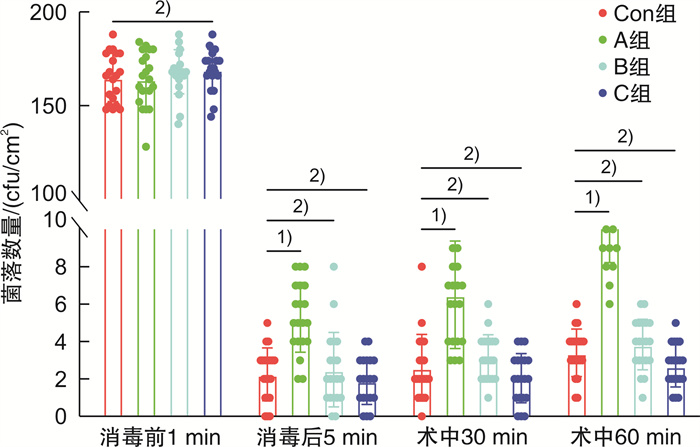
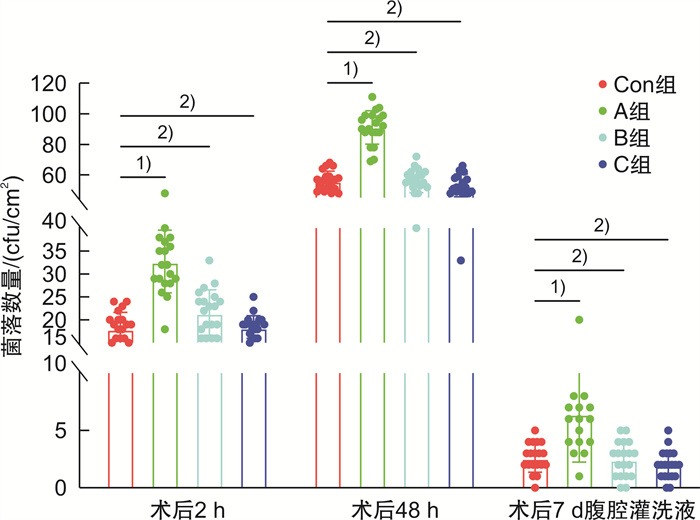
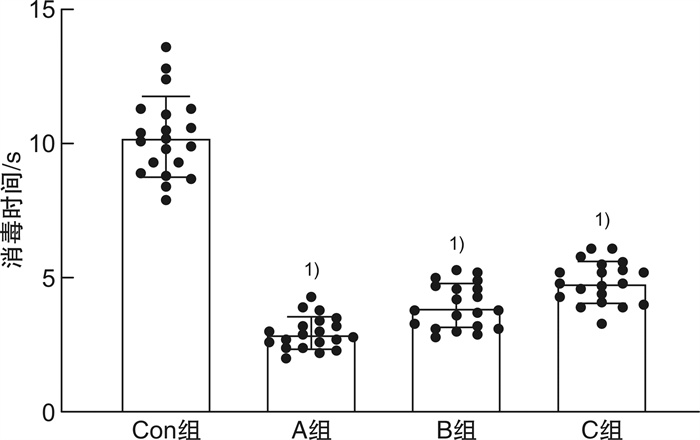
摘要: 目的 明确2%氯己定醇液喷雾消毒法在腹部手术切口中的消毒效果,以期为临床急腹症手术患者的腹部消毒方案提供新思路。方法 选用80只6~8周体重均一的健康C57BL/6雄性小鼠,随机分为4组:对照组、实验A组、实验B组、实验C组,每组20只。对照组采用2%氯己定醇液涂擦腹部3次消毒,实验A组用2%氯己定醇液喷洒2次,实验B组喷洒3次,实验C组喷洒4次,后行腹部正中切口模拟人体腹部手术过程。比较4组小鼠消毒时间、消毒液用量,消毒前后及手术前后切口边缘涂片和术后7 d腹腔灌洗液涂片培养的菌落数量,以及术后7 d内并发症发生情况。结果 实验A、B、C组均较对照组消毒时间短、消毒液用量少(P < 0.01);消毒前1 min,4组拟切口部位涂片培养菌落数比较差异无统计学意义(P>0.05);消毒后5 min,术中30 min、60 min,术后2 h、48 h切口涂片培养菌落数比较,实验A组较对照组明显增加(P < 0.01),实验B、C组与对照组比较差异无统计学意义(P>0.05);实验A组较对照组术后7 d内并发症总发生例数明显增加(P<0.05),实验B、C组与对照组比较差异无统计学意义(P>0.05)。结论 2%氯己定醇液在小鼠腹部手术部位的消毒,喷雾3次和4次的方式都能达到与涂擦3次同样的消毒效果,同时缩短了消毒用时和节约消毒液用量。因此,2%氯己定醇液喷雾消毒法在以腹部手术为主的急诊手术患者消毒中有较大应用前景。Abstract: Objective To clarify the disinfection effects of 2% chlorhexidine alcohol spray on mice abdominal surgical incisions, in order to provide a new disinfection choice for abdominal patients with acute abdomen surgery in clinical.Methods Eighty healthy C57BL/6 male mice(6-8 weeks old) were randomly divided into four groups: control group, experimental group A, experimental group B, and experimental group C, with 20 mice in each group. Mice in the control group were rubbed with 2% chlorhexidine solution on the abdomen for 3 times to disinfect, while mice in the experimental group A were sprayed with 2% chlorhexidine solution twice, mice in the experimental group B were sprayed for 3 times, and mice in the experimental group C were sprayed for 4 times. The median abdominal incision was applied to simulate the human abdominal surgical process. The time of disinfection, the volume of disinfectant, the amount of colonies cultured on the edge of the incision for pre-operation and post-operation, the amount of colonies cultured on the abdominal lavage fluid smear for the 7th day, and the postoperative complications within 7 days were compared among the four groups.Results Compared with the control group, experimental groups A, B and C showed shorter disinfection time and less volume of disinfectant(P < 0.01). As for the colony counts of bacteria cultured from the intended incision sites for one minute before disinfection, there was no significant difference within the four groups(P>0.05). The amounts of colonies in experimental group A was more than that in the control group at 5 minutes after disinfection, 30 and 60 minutes during operation, 2 and 48 hours after operation(P < 0.01), but there was no significant difference among experimental group B, C and control group(P>0.05). The total amount of post-operative complications within 7 days in experimental group A was more than that in the control group(P < 0.05), but there was no significant difference among experimental group B, C and the control group(P>0.05).Conclusion For the disinfection of 2% chlorhexidine alcohol solution in the abdominal surgical site of mice, three or four times of spraying can achieve the same disinfection effects as three times of rubbing. Furthermore, the spraying method shows shorter disinfection time and less volume of disinfectant. Therefore, 2% chlorhexidine alcohol spray disinfection has a great prospect in the disinfection of abdominal surgery especially for emergency surgery patients.
-

-
表 1 4组小鼠术后7 d内并发症发生情况比较
组别 并发症/例(%) 合计/例(%) χ2 P 死亡 切口红肿 Con组(n=20) 1(5.0) 0 1(5.0) A组(n=20) 3(15.0) 4(20.0) 7(35.0) 5.625 0.018 B组(n=20) 1(5.0) 0 1(5.0) 0 1.000 C组(n=20) 0 0 0 1.026 0.311 -
[1] Berríos-Torres SI, Umscheid CA, Bratzler DW, et al. Centers for Disease Control and Prevention Guideline for the Prevention of Surgical Site Infection, 2017[J]. JAMA Surg, 2017, 152(8): 784-791. doi: 10.1001/jamasurg.2017.0904
[2] Seidelman JL, Mantyh CR, Anderson DJ. Surgical Site Infection Prevention: A Review[J]. JAMA, 2023, 329(3): 244-252. doi: 10.1001/jama.2022.24075
[3] 卫生部发布《医疗机构消毒技术规范》等2项推荐性卫生行业标准[J]. 中国卫生标准管理, 2012, 3(4): 14-14.
[4] 欧鹏. 腹腔镜阑尾切除术与开腹阑尾切除术的临床对比研究[D]. 长沙: 中南大学, 2012.
[5] 刘洪斌. 腹腔镜胆囊切除术与传统开放手术治疗胆结石的效果比较[J]. 中国社区医师, 2019, 35(35): 78, 80. https://www.cnki.com.cn/Article/CJFDTOTAL-XCYS201935044.htm
[6] Yang J, Luo P, Wang Z, et al. Simulation training of laparoscopic pancreaticojejunostomy and stepwise training program on a 3D-printed model[J]. Int J Surg, 2022, 107: 106958. doi: 10.1016/j.ijsu.2022.106958
[7] Rouquette L, Traore O, Descamps S, et al. Bacterial skin recolonization in the operating room: comparison between various antisepsis protocols[J]. J Hosp Infect, 2020, 106(1): 57-64. doi: 10.1016/j.jhin.2020.06.014
[8] Li L, Wang Y, Wang S. Efficacy comparison of chlorhexidine and iodine preparation in reduction of surgical site infection: A systemic review and meta-analysis[J]. Int J Nurs Stud, 2022, 127: 104059. doi: 10.1016/j.ijnurstu.2021.104059
[9] Poppolo Deus F, Ouanounou A. Chlorhexidine in Dentistry: Pharmacology, Uses, and Adverse Effects[J]. Int Dent J, 2022, 72(3): 269-277. doi: 10.1016/j.identj.2022.01.005
[10] Reis MAO, de Almeida MCS, Escudero D, et al. Chlorhexidine gluconate bathing of adult patients in intensive care units in São Paulo, Brazil: Impact on the incidence of healthcare-associated infection[J]. Braz J Infect Dis, 2022, 26(1): 101666. doi: 10.1016/j.bjid.2021.101666
[11] Beausoleil C, Comstock SL, Werner D, et al. Antimicrobial persistence of two alcoholic preoperative skin preparation solutions[J]. J Hosp Infect, 2022, 129: 8-16. doi: 10.1016/j.jhin.2022.08.008
[12] Kanclerz P, Myers WG. Chlorhexidine and other alternatives for povidone-iodine in ophthalmic surgery: review of comparative studies[J]. J Cataract Refract Surg, 2022, 48(3): 363-369. doi: 10.1097/j.jcrs.0000000000000754
[13] Anderson J, Fulton RB, Li J, et al. Evaluation of chlorhexidine sensitization amongst healthcare workers[J]. Occup Med(Lond), 2022, 72(5): 343-346. doi: 10.1093/occmed/kqac038
[14] Wade RG, Burr NE, McCauley G, et al. The Comparative Efficacy of Chlorhexidine Gluconate and Povidone-iodine Antiseptics for the Prevention of Infection in Clean Surgery: A Systematic Review and Network Meta-analysis[J]. Ann Surg, 2021, 274(6): e481-e488.
[15] Chamsai B, Soodvilai S, Opanasopit P, et al. Topical Film-Forming Chlorhexidine Gluconate Sprays for Antiseptic Application[J]. Pharmaceutics, 2022, 14(6): 1124. doi: 10.3390/pharmaceutics14061124
[16] Daly BJ, Sharif MO, Jones K, et al. Local interventions for the management of alveolar osteitis(dry socket)[J]. Cochrane Database Syst Rev, 2022, 9(9): CD006968.
[17] Teschner D, Berisha M, Panse J, et al. Chlorhexidine gluconate-coated gel pad dressings for prevention of central venous catheter-related bloodstream infections in patients with hematologic diseases or autologous stem cell transplantation: A registry-based matched-pair analysis[J]. Eur J Haematol, 2023, 111(6): 914-921. doi: 10.1111/ejh.14098
[18] Simon AY, Ihejirika KA, Ogunkoya AB, et al. Comparison of the antimicrobial efficacy of topical antiseptic creams on canine wounds(preliminary communication)[J]. Bulg J Vet Med, 2007, 10: 273-281.
[19] Zhou HY, de Kraker MEA, Mimoz O, et al. Concentration of chlorhexidine gluconate-alcohol for skin antisepsis at the intravascular catheter insertion site[J]. J Hosp Infect, 2021, 115: 128-130. doi: 10.1016/j.jhin.2021.05.004
[20] de Morais Sampaio GA, de Meneses IHC, Vieira RA, et al. Influence of chlorhexidine digluconate on biocompatibility of cements: Morphological and immunohistochemistry analysis[J]. Microsc Res Tech, 2022, 85(7): 2438-2445. doi: 10.1002/jemt.24099
[21] Warren BG, Nelson A, Warren DK, et al. CDC Prevention Epicenters Program. Impact of preoperative chlorhexidine gluconate(CHG)application methods on preoperative CHG skin concentration[J]. Infect Control Hosp Epidemiol, 2021, 42(4): 464-466. doi: 10.1017/ice.2020.448
-

计量
- 文章访问数: 305
- 施引文献: 0



 下载:
下载: