The predictive value of granulocyte combined with platelet detection in the severity and prognosis of snake bites
-
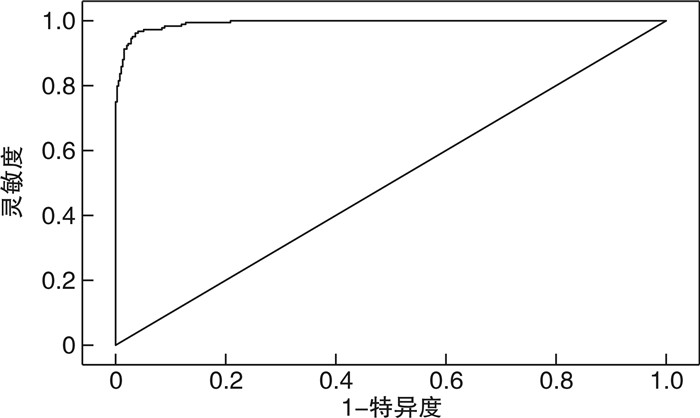
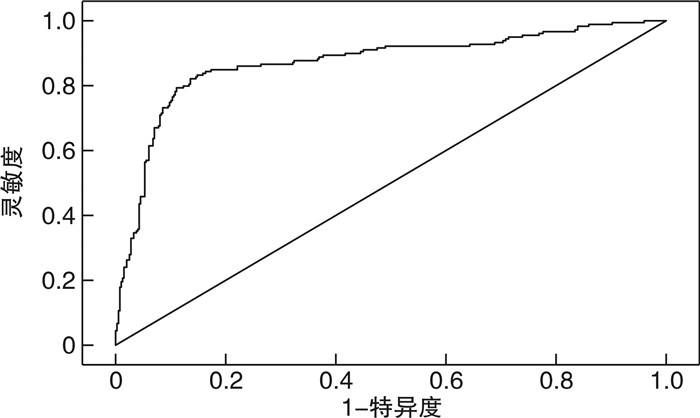
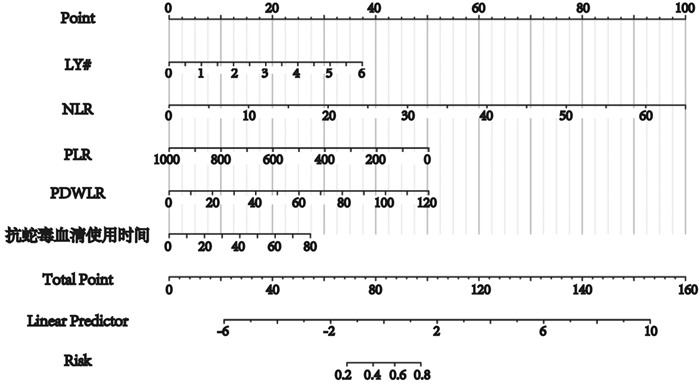
摘要: 目的 探讨蛇咬伤患者粒细胞联合血小板与蛇咬伤严重程度及发生并发症的相关性,并构建模型预测蛇咬伤患者发生严重并发症的概率。方法 回顾性分析2013年1月1日—2023年10月30日由恩施土家族苗族自治州中心医院西医部急诊中心收治的577例蛇咬伤患者,收集患者的一般资料、白细胞(white blood cell,WBC)、血小板(platelet, PLT)、血小板分布宽度(platelet distribution width, PDW)、平均血小板体积(mean platelet volume,MPV)、中性粒细胞绝对值(NE#)、淋巴细胞绝对值(LY#)、NLR(NE#/LY#)、PLR(PLT/LY#)、系统免疫炎症指数(systemic immune-inflammation index,SII)、PDWLR(PDW/LY#)、首次就诊时间、住院时间、住院费用、抗蛇毒血清使用时间等资料。根据是否发生严重并发症分成发生并发症组和未发生并发症组,根据蛇咬伤分度分成轻度和中重度蛇咬伤组。比较各组患者的一般资料及实验室数据,然后进行多因素logistic回归分析,构建ROC曲线评价指标的特异度和灵敏度,最后构建多因素的预测模型。结果 不同程度、不同预后的两组患者的年龄及性别等一般资料差异无统计学意义(P>0.05),轻度蛇咬伤的WBC、NE#、NLR、SII、PDWLR、住院时间、住院费用较中重度蛇咬伤患者更低,发生感染、组织坏死及需要输血和手术的患者更少,肿胀程度轻,PLT、LY#、PLR高,差异有统计学意义(P < 0.05);预后良好组的患者较发生并发症组WBC、NE#、NLR、SII和PDWLR更低,首次就诊时间和住院时间更短,抗蛇毒血清使用时间更早,住院费用更低,而PLT、LY#、PLR则更高,且两组间比较差异有统计学意义(P < 0.05)。结论 WBC、PLT、NLR、PLR、SII、PDWLR和抗蛇毒血清使用时间是蛇咬伤患者分度的影响因素。LY#、NLR、PLR、PDWLR及抗蛇毒血清使用时间是蛇咬伤患者预后的影响因素,其中LY#、NLR、PDWLR是预后的危险因素,而PLR和早期使用抗蛇毒血清是预后的保护因素,且综合分析上述因素能辅助蛇伤分度诊断和预测患者预后。Abstract: Objective To investigate the correlation between granulocyte combined with platelets and the severity and complications of snakebite patients, and to build a model to predict the probability of severe complications in snakebite patients.Methods The snakebite patients admitted to our hospital from January 1, 2013 to October 30, 2023 were retrospectively analyzed, and the general data, white blood cell(WBC), platelet(PLT), platelet distribution width(PDW), mean platelet volume(MPV), NE#, LY#, NLR(NE#/LY#), PLR(PLT/LY#), systemic immune-inflammation index(SII), PDWLR(PDW/LY#), time of first visit, length of stay, hospitalization cost, and duration of antivenom use of patients were collected. According to the occurrence of serious complications, the patients were divided into two groups: the group with complications and the group without complications, and the group with mild and moderate to severe snake bites were divided into two groups according to the snakebite scale. General data and laboratory data of each group of patients were compared, and then multivariate logistic regression analysis was performed to construct the specificity and sensitivity of ROC curve evaluation indicators, and finally a multivariate prediction model was constructed.Results There was no statistical significance in age, gender and other general data of the two groups with different degrees and different prognoses(P>0.05). The WBC, NE#, NLR, SII, PDWLR, length of hospital stay and hospitalization cost of mild snakebite were lower than those of moderate and severe snakebite.Fewer patients suffered from infection, tissue necrosis and needed blood transfusion and surgery, and the degree of swelling was mild. PLT, LY# and PLR were high, and the results were statistically significant(P < 0.05). Compared with the complication group, the patients in the good prognosis group had lower WBC, NE#, NLR, SII and PDWLR, shorter first visit time and hospital stay, earlier use of antivenin and lower hospital cost, while the PLT, LY# and PLR were higher, and there was statistical significance between the two groups(P < 0.05).Conclusion WBC, PLT, NLR, PLR, SII, PDWLR and duration of antivenom use were the factors influencing the classification of snakebite patients. LY#, NLR, PLR, PDWLR and duration of antivenom use were the influencing factors for prognosis of snakebite patients, among which LY#, NLR and PDWLR were the risk factors of prognosis, while PLR and early use of antivenom were the protective factors of prognosis (P < 0.05). And the comprehensive analysis of the above factors can assist in the classification diagnosis of snakebite and predict the prognosis of patients.
-
Key words:
- snake bite /
- granulocyte /
- platelet /
- prognosis /
- predictive value
-

-
表 1 患者一般资料比较
M(P25,P75) 临床资料 轻度蛇咬伤组 中重度蛇咬伤组 P 无并发症 有并发症 P 总例数 393 184 398 179 年龄/岁 60.00(50.00,67.00) 57.50(47.00,67.00) 0.394 60.00(50.50,67.00) 57.00(46.00,66.00) 0.132 性别/例 0.62 0.911 男 205 100 211 94 女 188 84 187 85 五步蛇(63例)/例 4 59 8 55 蝮蛇(179例)/例 146 33 133 46 竹叶青(44例)/例 23 21 21 23 烙铁头(59例)/例 49 10 49 10 不详(232例)/例 171 61 187 45 表 2 不同程度蛇咬伤患者一般资料及化验指标比较
M(P25,P75) 指标 轻度蛇咬伤组(393例) 中重度蛇咬伤组(184例) t/χ2 P 血清时间/h 5.50(4.50,7.50) 7.00(5.50,10.50) -5.560 < 0.001 WBC/(×109/L) 7.72(5.95,10.19) 11.64(8.09,14.98) -9.560 < 0.001 PLT/(×109/L) 199.50(170.00,242.75) 128.00(59.00,177.00) -12.100 < 0.001 PDW 16.30(16.10,16.60) 16.3(16.00,16.60) -0.640 0.522 MPV/FL 10.20(9.33,11.18) 10.20(9.20,11.30) -0.172 0.863 NE#/(×109/L) 7.08(4.39,9.72) 10.83(7.76,13.72) -8.536 < 0.001 LY#/(×109/L) 1.17(0.80,1.63) 0.76(0.52,1.03) -8.879 < 0.001 NLR 6.59(4.52,9.52) 18.70(14.50,25.23) -18.180 < 0.001 PLR 327.30(231.13,437.57) 157.72(112.67,218.42) -13.276 < 0.001 SII 1 099.95(562.83,1 940.07) 1 468.37(862.49,2 795.56) -4.231 < 0.001 PDWLR 14.22(10.02,20.44) 26.72(18.70,35.00) -11.800 < 0.001 首次就诊时间/h 4.00(3.00,6.00) 5.00(3.00,8.00) -1.670 0.095 住院时间/d 4.00(3.00,5.00) 7.00(4.00,11.00) -10.730 < 0.001 住院费用/元 3 186.87(2 088.67,5 569.59) 6 700.00(3 719.27,12 005.44) -9.770 < 0.001 合并感染/例 5 57 115.312 < 0.001 严重肿胀/例 22 91 153.073 < 0.001 输血/例 3 42 84.836 < 0.001 组织坏死/例 0 6 12.950 < 0.001 手术/例 0 34 77.167 < 0.001 表 3 不同预后患者一般资料及化验指标比较
M(P25,P75) 指标 未发生严重并发症组 严重并发症组 t/χ2 P 血清时间/h 5.50(4.50,7.50) 6.50(5.50,11.50) -4.95 < 0.001 WBC/(×109/L) 8.14(6.02,10.62) 10.83(7.68,14.48) -6.95 < 0.001 PLT/(×109/L) 197.00(162.00,236.00) 148.50(70.75,191.00) -8.92 < 0.001 PDW 16.30(16.00,16.60) 16.30(16.00,16.60) -0.19 0.860 MPV/FL 10.10(9.30,11.15) 10.20(9.40,11.30) -0.66 0.510 NE#/(×109/L) 7.30(4.53,10.07) 10.43(7.00,13.66) -7.06 < 0.001 LY#/(×109/L) 1.13(0.75,1.58) 0.80(0.56,1.15) -6.31 < 0.001 NLR 7.25(4.72,10.29) 16.69(11.42,23.77) -13.37 < 0.001 PLR 307.35(214.22,424.55) 165.56(116.93,244.07) -10.09 < 0.001 SII 1 195.59(576.73,1 978.27) 1 276.12(776.35,2 678.80) -2.32 0.020 PDWLR 14.78(10.36,21.72) 24.66(16.71,34.28) -9.03 < 0.001 首次就诊时间/h 4.00(3.00,6.00) 5.00(3.00,9.00) -2.17 0.030 住院时间/d 4.00(4.00,5.00) 6.00(4.00,11.00) -9.38 < 0.001 住院费用/元 3 423.23(2 151.56,5 876,58) 5 417.08(2 975.00,10 229.78) -6.18 < 0.001 表 4 蛇咬伤分度的多因素logistic回归分析
因素 B SE Wald χ2 df P Exp(B) 95%CI WBC 0.168 0.082 4.208 1 0.040 1.183 1.008~1.389 PLT -0.013 0.005 7.599 1 0.006 0.988 0.979~0.996 NLR 0.748 0.117 41.168 1 0 2.112 1.681~2.654 PLR -0.024 0.005 19.771 1 0 0.976 0.966~0.987 SII 0.001 0 4.759 1 0.029 1.001 1.000~1.002 PDWLR 0.095 0.049 3.849 1 0.050 1.100 1.000~1.210 血清使用时间 0.065 0.029 4.992 1 0.025 1.067 1.008~1.130 常量 -8.209 2.791 8.650 1 0.003 0 表 5 不良预后的多因素logistic回归分析
因素 B SE Wald χ2 df P Exp(B) 95%CI LY# 0.583 0.286 4.150 1 0.042 1.791 1.022~3.137 NLR 0.118 0.024 24.600 1 0 1.125 1.074~1.179 PLR -0.004 0.001 18.066 1 0 0.996 0.994~0.998 PDWLR 0.040 0.015 7.384 1 0.007 1.041 1.011~1.072 血清使用时间 0.036 0.015 5.816 1 0.016 1.037 1.007~1.068 常量 -3.201 0.808 15.698 1 0 0.041 -
[1] Knudsen C, Jürgensen JA, Føns S, et al. Snakebite Envenoming Diagnosis and Diagnostics[J]. Front Immunol, 2021, 12: 661457. doi: 10.3389/fimmu.2021.661457
[2] Habib AG, Kuznik A, Hamza M, et al. Snakebite is Under Appreciated: Appraisal of Burden from West Africa[J]. PLoS Negl Trop Dis, 2015, 9(9): e0004088. doi: 10.1371/journal.pntd.0004088
[3] Kumar A, Dungdung A, Kumar A, et al. A cross-sectional study of various clinical and laboratory parameters in snakebite and their association with mortality at a tertiary care centre in Jharkhand[J]. J Family Med Prim Care, 2022, 11: 7089-7094. doi: 10.4103/jfmpc.jfmpc_588_22
[4] Zychar BC, Clissa PB, Carvalho E, et al. Leukocyte recruitment induced by snake venom metalloproteinases: Role of the catalytic domain[J]. Biochem Biophys Res Commun, 2020, 521: 402-407. doi: 10.1016/j.bbrc.2019.10.144
[5] Liew PX, Kubes P. The Neutrophil's Role During Health and Disease[J]. Physiol Rev, 2019, 99(2): 1223-1248. doi: 10.1152/physrev.00012.2018
[6] Castanheira F, Kubes P. Neutrophils and NETs in modulating acute and chronic inflammation[J]. Blood, 2019, 133(20): 2178-2185. doi: 10.1182/blood-2018-11-844530
[7] Rane D, Patil T, More V, et al. Neutrophils: Interplay between host defense, cellular metabolism and intracellular infection[J]. Cytokine, 2018, 112: 44-51. doi: 10.1016/j.cyto.2018.07.009
[8] Zhou H, Mei X, He X, et al. Severity stratification and prognostic prediction of patients with acute pancreatitis at early phase: A retrospective study[J]. Medicine(Baltimore), 2019, 98: e15275.
[9] Gutta LMS, Ahmed T. NLR and PLR Ratios-Accessible and Affordable Predictors of Disease Severity in COPD[J]. J Assoc Physicians India, 2022, 70: 11-12. doi: 10.5005/japi-11001-0110
[10] Elbey B, Baykal B, Yazgan ÜC, et al. The prognostic value of the neutrophil/lymphocyte ratio in patients with snake bites for clinical outcomes and complications[J]. Saudi J Biol Sci, 2017, 24(2): 362-366. doi: 10.1016/j.sjbs.2015.10.002
[11] Aktar F, Tekin R. Mean platelet volume, neutrophil to lymphocyte ratio and platelet to lymphocyte ratio in determining the diagnosis or outcome in children with snakebite[J]. Arch Argent Pediatr, 2017, 115: 576-580.
[12] Ghobadi H, Mohammadshahi J, Javaheri N, et al. Role of leukocytes and systemic inflammation indexes(NLR, PLR, MLP, dNLR, NLPR, AISI, SIR-I, and SII)on admission predicts in-hospital mortality in non-elderly and elderly COVID-19 patients[J]. Front Med(Lausanne), 2022, 9: 916453.
[13] Luo F, Li Y, Zhao Y, et al. Systemic immune-inflammation index predicts the outcome after aneurysmal subarachnoid hemorrhage[J]. Neurosurg Rev, 2022, 45: 1607-1615. doi: 10.1007/s10143-021-01681-4
[14] Wang RH, Wen WX, Jiang ZP, et al. The clinical value of neutrophil-to-lymphocyte ratio(NLR), systemic immune-inflammation index(SII), platelet-to-lymphocyte ratio(PLR)and systemic inflammation response index(SIRI)for predicting the occurrence and severity of pneumonia in patients with intracerebral hemorrhage[J]. Front Immunol, 2023, 14: 1115031. doi: 10.3389/fimmu.2023.1115031
[15] Hrubaru I, Motoc A, Moise ML, et al. The Predictive Role of Maternal Biological Markers and Inflammatory Scores NLR, PLR, MLR, SII, and SIRI for the Risk of Preterm Delivery[J]. J Clin Med, 2022, 11(23): 6982. doi: 10.3390/jcm11236982
[16] van der Meijden P, Heemskerk J. Platelet biology and functions: new concepts and clinical perspectives[J]. Nat Rev Cardiol, 2019, 16(3): 166-179. doi: 10.1038/s41569-018-0110-0
[17] Xie RH, Ye XL, Tang CY, et al. Associated Clinical Factors for Coagulation Dysfunction due to Trimeresurus stejnegeri: A Retrospective Observational Study[J]. J Toxicol, 2023, 2023: 8832355.
[18] Abd El-Azim MM, Mousa MK, Abdelmaaboud RM, et al. Evaluation of the role of neutrophil to lymphocyte ratio(NLR), platelet to lymphocyte ratio(PLR)and mean platelet volume(MPV)time series as predictors of diagnosis and prognosis of hemotoxic snakebite[J]. Biomarkers, 2023, 28(7): 652-662. doi: 10.1080/1354750X.2023.2277668
[19] Köse A, Akdeniz A, Babus SB, et al. The Usefulness of Platelet Distribution Width and Platelet Distribution Width to Lymphocyte Ratio in Predicting Severity and Outcomes in Patients with Snakebite[J]. Wilderness Environ Med, 2021, 32(3): 284-292. doi: 10.1016/j.wem.2021.03.006
[20] Samaga S, Bhandary NM, Shetty N, et al. Prognostic Value of Neutrophil/Lymphocyte Ratio and Platelet Lymphocyte Ratio in Patients with Snake Bites in India[J]. J Assoc Physicians India, 2020, 68(1): 103.
[21] 罗杰, 熊丽, 何杨俊, 等. 烙铁头蛇咬伤患者不同时间段行切开引流的临床效果比较[J]. 创伤外科杂志, 2021, 23(9): 701-704. https://www.cnki.com.cn/Article/CJFDTOTAL-CXWK202109019.htm
[22] 刘彦伶, 陈莉, 周维, 等. 影响蝮蛇咬伤后肢体肿胀的相关因素[J]. 护理实践与研究, 2023, 20(21): 3218-3223. https://www.cnki.com.cn/Article/CJFDTOTAL-HLSJ202321009.htm
-

计量
- 文章访问数: 523
- 施引文献: 0



 下载:
下载: