The prognostic value of serum myostatin in elderly patients with severe decompensated acute heart failure
-
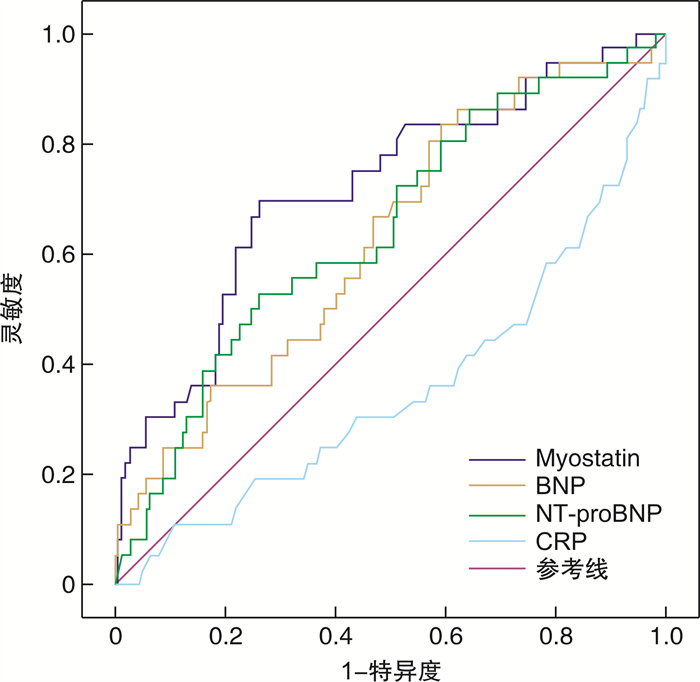
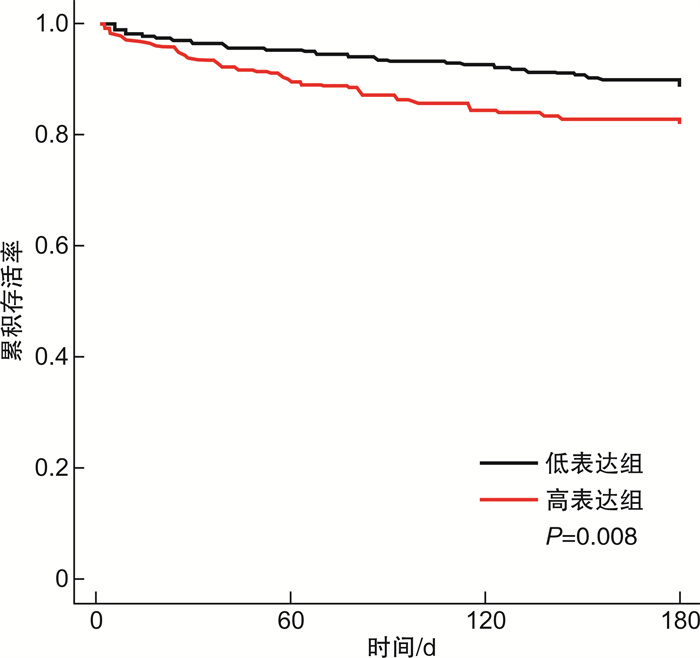
摘要: 目的 探讨血清肌肉生长抑制素(myostatin)在老年严重失代偿期急性心力衰竭(AHF)患者预后评估中的价值。方法 选取2015年6月—2019年1月期间收治的286例老年严重失代偿期AHF患者。入院24 h内采患者肘静脉血,用酶联免疫吸附试验检测myostatin水平,以中位数为截断值,将患者分为高表达组和低表达组。计算286例患者入院后180 d的存活率,进而将患者分为存活组和死亡组。绘制Kaplan-Meier曲线分析患者生存率,logistic回归分析影响患者死亡预后的因素;受试者工作特征曲线(ROC)分析myostatin预测患者死亡预后的价值。结果 286例患者入院后180 d时死亡54例,病死率为18.88%。286例患者的血清myostatin浓度为(12.18±4.08) ng/mL,中位数为10.27 ng/mL,高表达组患者的存活率明显低于低表达组,差异有统计学意义(P< 0.05)。死亡组C反应蛋白(CRP)、B型脑钠肽(BNP)、N末端B型利钠肽原(NT-proBNP)和myostatin表达水平均高于存活组,差异有统计学意义(P< 0.05)。Logistic多因素分析结果显示,CRP、BNP、NT-proBNP和myostatin是老年严重失代偿期AHF患者死亡的独立影响因素(P< 0.05)。血清myostatin预测患者死亡的ROC曲线下面积为0.736,明显高于CRP(0.379)、BNP(0.625)和NT-proBNP(0.643)。结论 Myostatin对早期预测老年严重失代偿期AHF患者的死亡预后有一定价值。Abstract: Objective To explore the value of serum myostatin in the prognosis of elderly patients with severe decompensated acute heart failure(AHF).Methods From June 2015 to January 2019, 286 elderly patients with severe decompensated AHF were selected. Within 24 hours after admission, the elbow vein blood was drawn and the myostatin level was detected by enzyme-linked immunosorbent assay. Patients were divided into high expression group and low expression group with median as cutoff value. The survival rate of 286 patients was calculated 180 days after admission, and then the patients were divided into survival group and death group. Kaplan-Meier curve was drawn to analyze the survival rate of patients; logistic regression was used to analyze the factors influencing the prognosis of patients; ROC curve was used to analyze the value of myostatin in predicting the prognosis of patients.Results Two hundred and eighty-six patients died 180 days after admission, the mortality rate was 18.88%. The serum concentration of myostatin was(12.18±4.08) ng/mL, the median was 10.27 ng/mL, the survival rate of patients in the high expression group was significantly lower than that in the low expression group(P< 0.05). The expression levels of CRP, BNP, NT-proBNP and myostatin in the dead group were higher than those in the living group(P< 0.05). The results of logistic multivariate analysis showed that CRP, BNP, NT-proBNP and myostatin were the independent factors for death in elderly patients with severe decompensated AHF(P< 0.05). The area under ROC curve(AUC) of serum myostatin was 0.736, which was significantly higher than CRP(AUC=0.379), BNP(AUC=0.625) and NT-proBNP(AUC=0.643).Conclusion Myostatin has a certain value in predicting the prognosis of elderly AHF patients in severe decompensation.
-
Key words:
- serum /
- myostatin /
- acute heart failure /
- prognosis
-

-
表 1 影响老年严重失代偿期AHF患者死亡的单因素分析
例(%),X±S 影响因素 存活组(n=232) 死亡组(n=54) t/χ2 P 年龄/岁 70.03±6.36 73.76±12.14 2.187 0.029 性别 男 150(64.66) 32(59.26) 0.551 0.458 女 82(35.34) 22(40.76) LVEF/% 37.26±8.36 35.36±6.28 1.872 0.062 CRP/(mg·dl-1) 0.74±0.15 1.15±0.63 4.745 < 0.001 BNP/(pg·mL-1) 676.39±116.32 796.35±210.34 4.046 < 0.001 NT-proBNP/(pg·mL-1) 3 005.24±981.37 6 125.36±1 263.02 16.990 < 0.001 myostatin/(ng·mL-1) 10.02±3.27 14.32±1.35 21.311 < 0.001 利尿剂 101(43.53) 20(37.04) 0.758 0.384 硝酸甘油 41(17.67) 10(18.52) 0.021 0.884 ACEI/ARB 99(42.67) 21(38.89) 0.257 0.612 β受体阻滞剂 64(27.59) 21(38.89) 2.679 0.102 钙通道阻滞剂 80(34.48) 17(31.48) 0.144 0.704 地高辛 17(7.33) 3(5.56) 0.211 0.646 他汀类 38(16.38) 13(24.07) 1.770 0.183 表 2 影响老年严重失代偿期AHF患者死亡的多因素分析
影响因素 OR 95%CI P CRP 1.123 0.998~1.285 0.041 BNP 1.213 1.032~1.416 0.023 NT-proBNP 1.921 1.302~2.862 < 0.001 myostatin 2.030 1.298~3.168 < 0.001 表 3 血清myostatin预测患者死亡的价值
指标 AUC(95%CI) 截断值 敏感度/% 特异度/% CRP/(mg·dl-1) 0.379(0.251~0.467) 1.04 25.54 46.82 BNP/(pg·mL-1) 0.625(0.525~0.727) 789.36 82.36 41.55 NT-proBNP/(pg·mL-1) 0.643(0.541~0.745) 5 864.82 53.26 72.69 myostatin/(ng·mL-1) 0.736(0.618~0.815) 13.58 70.36 74.50 -
[1] 张艳利, 于海侠, 郭金朋, 等. 新活素对心肺复苏后心力衰竭患者心功能及血清IL-6影响的研究[J]. 临床急诊杂志, 2020, 21(3): 209-211. http://zzlc.cbpt.cnki.net/WKC/WebPublication/paperDigest.aspx?paperID=77808ece-bcf1-4b57-8d33-f1dfc554c502
[2] 胡振, 温伟, 张新超. 红细胞分布宽度联合N末端B型利钠肽原评估老年急性心力衰竭预后的价值[J]. 临床急诊杂志, 2020, 21(1): 29-33. http://zzlc.cbpt.cnki.net/WKC/WebPublication/paperDigest.aspx?paperID=fc9885b6-9b64-44d9-91d4-9b83ee335126
[3] Kitzman DW, Whellan DJ, Duncan P, et al. Physical Rehabilitation for Older Patients Hospitalized for Heart Failure[J]. N Engl J Med, 2021, 385(3): 203-216. doi: 10.1056/NEJMoa2026141
[4] Lee SJ. Targeting the myostatin signaling pathway to treat muscle loss and metabolic dysfunction[J]. J Clin Invest, 2021, 131(9): e148372. doi: 10.1172/JCI148372
[5] Esposito P, Verzola D, Picciotto D, et al. Myostatin/Activin-A Signaling in the Vessel Wall and Vascular Calcification[J]. Cells, 2021, 10(8): 2070. doi: 10.3390/cells10082070
[6] Chen P, Liu Z, Luo Y, et al. Predictive value of serum myostatin for the severity and clinical outcome of heart failure[J]. Eur J Intern Med, 2019, 64(1): 33-40.
[7] 中华医学会心血管病学分会心力衰竭学组, 中国医师协会心力衰竭专业委员会中华心血管病杂志编辑委员会. 中国心力衰竭诊断和治疗指南2018[J]. 中华心血管病杂志, 2018, 46(10): 760-789. doi: 10.3760/cma.j.issn.0253-3758.2018.10.004
[8] 倪婳, 李从圣, 杨静, 等. 心力衰竭患者血清中内质网应激标志物GRP78的水平变化及其在评估近期预后中的价值[J]. 临床急诊杂志, 2020, 21(8): 638-642. http://zzlc.cbpt.cnki.net/WKC/WebPublication/paperDigest.aspx?paperID=80c5dd53-fee4-4365-942b-b525bafad2aa
[9] Kiuchi K, Shirakabe A, Kobayashi N, et al. Prognostic impact of new-onset atrial fibrillation associated with worsening heart failure in aging patients with severely decompensated acute heart failure[J]. Int J Cardiol, 2020, 302(1): 88-94.
[10] Park JJ, Lee HY, Kim KH, et al. Heart failure and atrial fibrillation: tachycardia-mediated acute decompensation[J]. ESC Heart Fail, 2021, 8(4): 2816-2825. doi: 10.1002/ehf2.13354
[11] McDonagh TA, Metra M, Adamo M, et al. 2021 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure[J]. Eur Heart J, 2021, 42(36): 3599-3726.
[12] Kumagai H, Coelho AR, Wan J, et al. MOTS-c reduces myostatin and muscle atrophy signaling[J]. Am J Physiol Endocrinol Metab, 2021, 320(4): E680-E690. doi: 10.1152/ajpendo.00275.2020
[13] Baczek J, Silkiewicz M, Wojszel ZB. Myostatin as a Biomarker of Muscle Wasting and other Pathologies-State of the Art and Knowledge Gaps[J]. Nutrients, 2020, 12(8): 2401. doi: 10.3390/nu12082401
[14] Lim S, McMahon CD, Matthews KG, et al. Absence of myostatin improves cardiac function following myocardial infarction[J]. Heart Lung Circ, 2018, 27(6): 693-701. doi: 10.1016/j.hlc.2017.05.138
[15] Meloux A, Rochette L, Maza M, et al. Growth Differentiation Factor-8(GDF8)/Myostatin is a Predictor of Troponin I Peak and a Marker of Clinical Severity after Acute Myocardial Infarction[J]. J Clin Med, 2019, 9(1): 116. doi: 10.3390/jcm9010116
[16] Omosule CL, Phillips CL. Deciphering Myostatin's Regulatory, Metabolic, and Developmental Influence in Skeletal Diseases[J]. Front Genet, 2021, 12: 662908. doi: 10.3389/fgene.2021.662908
[17] Qi H, Ren J, Ba L, et al. MSTN Attenuates Cardiac Hypertrophy through Inhibition of Excessive Cardiac Autophagy by Blocking AMPK/mTOR and miR-128/PPARγ/NF-κB[J]. Mol Ther Nucleic Acids, 2020, 19: 507-522. doi: 10.1016/j.omtn.2019.12.003
[18] Ishida J, Konishi M, Saitoh M, et al. Myostatin signaling is up-regulated in female patients with advanced heart failure[J]. Int J Cardiol, 2017, 238(1): 37-42.
[19] Furihata T, Kinugawa S, Fukushima A, et al. Serum myostatin levels are independently associated with skeletal muscle wasting in patients with heart failure[J]. Int J Cardiol, 2016, 220(1): 483-487.
[20] Chen P, Liu Z, Luo Y, et al. Predictive value of serum myostatin for the severity and clinical outcome of heart failure[J]. Eur J Intern Med, 2019, 64: 33-40. doi: 10.1016/j.ejim.2019.04.017
[21] Aravena J, Abrigo J, Gonzalez F, et al. Angiotensin(1-7) Decreases myostatin-induced nf-kappab signaling and skeletal muscle atrophy[J]. Int J Mol Sci, 2020, 21(3): 1-10.
[22] 汤勇才, 廖军, 黄小媛, 等. 急性心衰患者NTpro-BNP, cTnI, hs-CRP的变化及其临床意义[J]. 广州医药, 2017, 48(2): 46-50. doi: 10.3969/j.issn.1000-8535.2017.02.013
[23] Okazaki H, Shirakabe A, Kobayashi N, et al. The prognostic impact of uric acid in patients with severely decompensated acute heart failure[J]. J Cardiol, 2016, 68(5): 384-391. doi: 10.1016/j.jjcc.2016.04.013
[24] Konev AA, Kharitonov AV, Rozov FN, et al. CT-IGFBP-4 as a novel prognostic biomarker in acute heart failure[J]. ESC Heart Fail, 2020, 7(2): 434-444. doi: 10.1002/ehf2.12590
[25] Nishimoto Y, Kato T, Morimoto T, et al. C-reactive protein at discharge and 1-year mortality in hospitalised patients with acute decompensated heart failure: an observational study[J]. BMJ Open, 2020, 10(12): e041068. doi: 10.1136/bmjopen-2020-041068
-




 下载:
下载: