Correlation study of soluble suppression of tumorigenicity 2 and NLR and MHR in severe heart failure
-
摘要: 目的 探讨可溶性生长刺激表达基因2蛋白(sST2)、单核细胞与高密度脂蛋白胆固醇比值(MHR)和中性粒细胞与淋巴细胞比值(NLR)在重症心力衰竭表达的相关性研究。方法 分析2017年12月-2020年12月期间我院心脏重症监护室(CCU)收治的重症心力衰竭患者85例。根据患者出院后6个月是否发生终点事件分为生存组67例和死亡组18例。分别检测白细胞(W)、中性粒细胞(N)、淋巴细胞(L)、单核细胞(M)和三酰甘油(TG)、总胆固醇(TC)、低密度脂蛋白(LDL)、高密度脂蛋白(HDL)、尿素氮(BUN)、肌酐(Cr)、N末端B型脑钠尿肽(NT-proBNP)、sST2、CRP以及内皮素-1(ET-1)、一氧化氮(NO)、丙二醛(MAD)、超氧化物歧化酶(SOD)水平;计算NLR以及MHR。测定左心室射血分数(LVEF)评估心功能。结果 死亡组心率、白细胞、中性粒细胞、淋巴细胞、单核细胞、BUN、Cr高于生存组,死亡组HDL低于生存组,差异有统计学意义(P< 0.05)。入院时,死亡组NLR、MHR、CRP、sST2、NT-proBNP高于生存组,差异有统计学意义(P< 0.05)。死亡组LVEF、ET-1、NO、SOD、MAD与生存组比较,差异无统计学意义(P>0.05);出院时,死亡组NLR、MHR、CRP、sST2、NT-proBNP、ET-1、MAD高于生存组,NO、SOD、LVEF低于生存组,差异有统计学意义(P< 0.05)。生存组,入院时NLR、MHR、CRP、sST2、NT-proBNP、ET-1、MAD高于出院时,NO、SOD、LVEF低于出院时,差异有统计学意义(P< 0.05)。死亡组患者入院时与出院时比较,差异无统计学意义(P>0.05)。相关分析显示:sST2、NLR、MHR与重症心力衰竭患者终点事件呈正相关。Logistic回归分析,sST2、NLR、MHR升高,重症心衰患者发生心血管死亡的危险性增加。采用接受者操作特性曲线显示,sST2、NLR、MHR联合检测曲线下面积为0.865,对重症心力衰竭患者预后预测价值最大。结论 sST2、NLR、MHR对重症心力衰竭患者早期病情及预后评估有重要的临床价值。Abstract: Objective To investigate the correlation of soluble growth-stimulating expression gene 2 protein(sST2), monocyte-high density lipoprotein cholesterol ratio(MHR), and neutrotrophil-to-lymphocyte-lymphocyte ratio(NLR) in severe heart failure.Methods Retrospective analysis of 85 severe heart failure patients admitted in CCU from December 2017 to December 2020. There were 67 survival and 18 deaths according to whether end events occurred 6 months after discharge. The levels of white blood cells, neutrophils, lymphocytes, monocytes, triglycerides, total cholesterol, low density lipoprotein, high density lipoprotein, urea nitrogen, creatinine, and N terminal B brain naturetic peptide were detected respectively; NLR and MHR were calculated. Left ventricular ejection fraction(LVEF) was determined to assess cardiac function.Results Heart rate, white blood leukocytes, neutrophils, lymphocytes, monocytes, urea nitrogen and creatinine were higher than the survival group, and HDL was lower than the survival group, which was statistically significant(P< 0.05). On admission, NLR, MHR, CRP, sST2, and NT-proBNP were higher than the survival group and were statistically significant(P< 0.05). LVEF, ET-1, NO, SOD, and MAD were not compared with the survival group(P>0.05), NLR, MHR, CRP, sST2, NT-proBNP, ET-1, MAD, NO, SOD, LVEF(P< 0.05). In the survival group, at admission, NLR, MHR, CRP, sST2, NT-proBNP, ET-1, and MAD were higher than at discharge, and at discharge, NO, SOD, and LVEF were lower than at discharge(P< 0.05). There was no difference between the hospital versus discharge(P>0.05). Related analysis showed that sST2, NLR, and MHR were positively correlated with the end-point events in patients with severe heart failure. In the logistic regression analysis, sST2, NLR, and MHR were increased, and the risk of cardiovascular death was increased in patients with severe heart failure. Then, the area under the sST2, NLR and MHR was 0.865, which was the greatest prognostic value for patients with severe heart failure.Conclusion sST2, NLR, MHR has an important clinical value for early condition and prognosis assessment in patients with severe heart failure.
-
Key words:
- severe heart failure /
- inflammation /
- oxidative stress /
- endothelial function
-

-
表 1 两组患者临床资料的比较
例(%), X±S 临床资料 生存组(67例) 死亡组(18例) 统计值 P 年龄/岁 68.11±3.62 69.61±4.73 1.462 0.226 女性 34(50.74) 10(55.56) 0.132 0.463 体质量/kg 67.56±2.34 66.72±3.41 0.794 0.458 心率/(次·min-1) 95.16±6.72 118.75±5.851) 5.386 0.002 收缩压/mmHga) 123.29±5.04 117.91±3.39 1.621 0.134 高血压 19(28.36) 3(16.67) 1.012 0.239 冠心病 37(55.22) 10(55.56) 0.002 0.592 扩心病 11(16.42) 5(27.78) 1.197 0.221 WBC/(×109·L-1) 9.69±1.26 13.94±1.571) 5.894 0.001 中性粒细胞/(×109·L-1) 5.34±0.38 7.42±0.751) 2.693 0.038 淋巴细胞/(×109·L-1) 0.95±0.02 0.87±0.031) 3.164 0.015 单核细胞/(×109·L-1) 0.82±0.02 0.89±0.021) 8.575 0.001 BUN/(mmol·L-1) 9.71±1.33 10.16±2.371) 4.745 0.003 Cr/(μmol·L-1) 116.29±5.63 126.12±6.671) 5.628 0.001 TC/(mmol·L-1) 5.48±1.87 5.37±1.55 1.434 0.217 TG/(mmol·L-1) 1.39±0.02 1.42±0.03 1.927 0.114 HDL/(mmol·L-1) 1.08±0.04 0.94±0.031) 4.479 0.005 LDL/(mmol·L-1) 3.34±0.07 3.42±0.08 1.743 0.138 注:a)1 mmHg=0.133 kPa; 与生存组比较,1)P < 0.05。 表 2 两组炎症指标和心功能的比较
X±S 项目 生存组(67例) 死亡组(18例) 统计值 P NLR 入院时 5.42±1.26 8.66±1.131) 3.204 0.018 出院时 4.15±0.642) 8.13±1.071) 5.695 0.001 MHR 10.026 0.001 入院时 0.77±0.02 0.95±0.041) 10.026 0.001 出院时 0.63±0.012) 0.88±0.031) 9.504 0.001 sST2/(μg·L-1) 入院时 62.68±6.92 68.41±8.461) 5.051 0.002 出院时 56.81±4.172) 66.74±7.161) 9.472 0.001 NT-proBNP/(μg·L-1) 入院时 9179.83±565.98 9819.01±854.541) 6.435 0.001 出院时 4988.26±327.442) 9527.35±364.951) 18.589 0.001 LVEF/% 入院时 35.12±4.12 33.53±3.73 1.137 0.299 出院时 37.59±1.742) 32.08±4.521) 6.025 0.001 CRP/(mg·L-1) 入院时 8.34±3.57 11.58±4.671) 3.394 0.015 出院时 5.56±1.382) 9.24±4.821) 5.618 0.001 与生存组比较,1)P < 0.05;与入院时比较,2)P < 0.05。 表 3 两组氧化应激指标和内皮功能的比较
X±S 项目 生存组(67例) 死亡组(18例) 统计值 P ET-1/(μg·L-1) 入院时 76.51±8.11 78.02±9.83 1.414 0.207 出院时 65.69±0.872) 77.12±1.461) 7.813 0.001 NO /(μmol·L-1) 入院时 45.65±4.92 44.17±5.17 1.606 0.159 出院时 57.13±6.312) 42.93±4.271) 9.331 0.001 MAD/(nmol·L-1) 入院时 6.13±1.92 7.45±2.63 1.077 0.323 出院时 3.52±1.042) 6.65±1.861) 9.943 0.001 SOD/(KU·L-1) 入院时 77.51±6.71 76.17±8.96 1.188 0.281 出院时 93.26±9.252) 75.35±6.881) 12.925 0.001 与生存组比较,1)P < 0.05;与入院时比较,2)P < 0.05。 表 4 重症心力衰竭患者死亡的logistic分析
因素 β SE(β) Wald P R=exp(β) sST2 0.972 0.662 2.159 0.031 2.643 NHR 3.771 1.419 1.922 0.028 1.967 MHR 0.845 0.509 2.761 0.019 2.328 表 5 sST2、NLR、MHR及联合检测对重症心力衰竭患者预后的预测
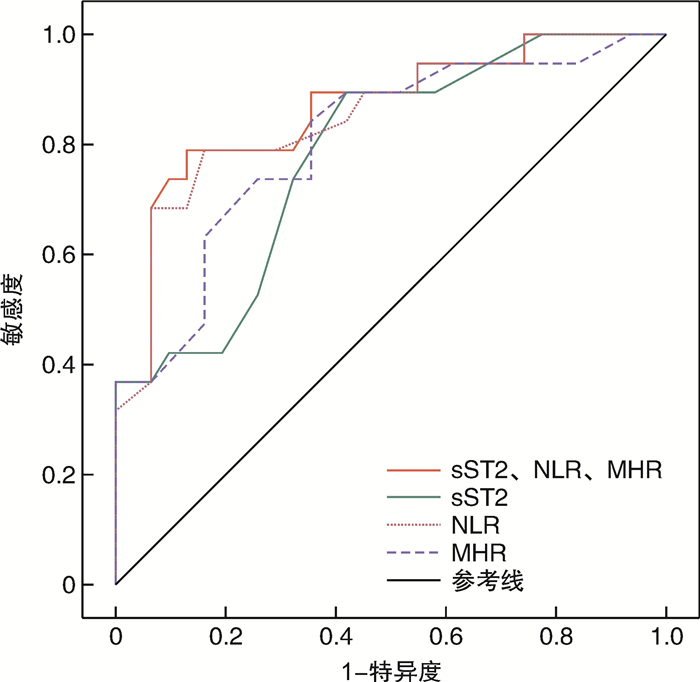
指标 曲线下面积 95%CI 敏感度 特异度 sST2 0.783 0.655~0.911 0.743 0.648 NLR 0.852 0.742~0.962 0.825 0.712 MHR 0.804 0.681~0.938 0.808 0.678 联合检测 0.865 0.757~0.974 0.846 0.739 -
[1] Taniguchi T, Shiomi H, Morimoto T, et al. Incidence and prognostic impact of heart failure hospitalization during follow-up after primary percutaneous coronary intervention in ST-segment elevation myocardial infarction[J]. Am J Cardiol, 2017, 119(11): 1729-1739. doi: 10.1016/j.amjcard.2017.03.013
[2] Komanduri S, Jadhao Y, Guduru SS, et al. Prevalence and risk factors of heart failure in the USA: NHANES 2013-2014 epidemiological follow-up study[J]. J Community Hosp Intern Med Perspect, 2017, 7(1): 15-20. doi: 10.1080/20009666.2016.1264696
[3] Ungprasert P, Srivali N, Thongprayoon C. Nonsteroidal anti-inflammatory drugs and risk of incident heart failure: a systematic review and metaanalysis of observational studies[J]. Clin Cardiol, 2016, 39(2): 111-118. doi: 10.1002/clc.22502
[4] Harjola VP, Mullens W, Banaszewski M, et al. Organ dysfunction, injury and failure in acute heart failure: from pathophysiology to diagnosis and management. A review on behalf of the Acute Heart Failure Committeeof the Heart Failure Association(HFA)of the European Society of Cardiology(ESC)[J]. Eur J Heart Fail, 2017, 19(7): 821-836. doi: 10.1002/ejhf.872
[5] Tokmachev RE, Budnevsky AV, Kravchenko AY. The role of inflammation in the pathogenesis of chronic heart failure[J]. Ter Arkh, 2016, 88(9): 106-110.
[6] 中华医学会心血管病学分会心力衰竭学组, 中国医师协会, 心力衰竭专业委员会, 等. 中国心力衰竭诊断和治疗指南2018[J]. 中华心血管病杂志, 2018, 46(10): 760-789. doi: 10.3760/cma.j.issn.0253-3758.2018.10.004
[7] Mansour IN, Bress AP, Groo V, et al. Circulating procollagen type ⅢN-terminal peptide and mortality risk in African Americans with heartfailure〔J〕. J Cardiac Failure, 2016, 22(9): 692-699. doi: 10.1016/j.cardfail.2015.12.016
[8] Bello NA, Lewis EF, Desai AS, et al. Increased risk of stroke with darbepoetin alfa in anaemic heart failure patients with diabetes and chronic kidney disease[J]. Eur J Heart Fail, 2015, 17(11): 1201-1207. doi: 10.1002/ejhf.412
[9] 赵荫涛, 裴小鑫, 胡铂, 等. Ghrelin对多柔比星诱导大鼠心力衰竭和心肌损伤的保护作用及机制[J]. 实用医学杂志, 2021, 37(1): 30-34. doi: 10.3969/j.issn.1006-5725.2021.01.007
[10] 禹海文, 董炎炎, 党瑜华. T细胞免疫球蛋白和黏蛋白结构域蛋白-3对慢性心力衰竭患者T细胞功能的调控作用[J]. 中华医学杂志, 2020, 100(17): 1315-1319. doi: 10.3760/cma.j.cn112137-20190823-01876
[11] 黄丽, 齐洁, 崔建国, 等. 中性粒细胞/淋巴细胞比值与慢性心力衰竭急性发作患者院内死亡的相关性研究[J]. 临床心血管病杂志, 2020, 36(2): 138-142. https://www.cnki.com.cn/Article/CJFDTOTAL-LCXB202002010.htm
[12] Pickering RJ, Booty LM. NLR in eXile: Emerging roles of NLRX1 in immunity and human disease[J]. Immunology, 2021, 162(3): 268-280. doi: 10.1111/imm.13291
[13] 宋莹, 姜琳, 陈艳, 等. 高密度脂蛋白胆固醇水平对冠状动脉病变严重程度及介入治疗预后的影响[J]. 中华心血管病杂志, 2020, 48(2): 123-129. doi: 10.3760/cma.j.issn.0253-3758.2020.02.007
[14] Eichin D, Pessia A, Takeda A, et al. CD73 contributes to anti-inflammatory properties of afferent lymphatic endothelial cells in humans and mice[J]. Eur J Immunol, 2021, 51(1): 231-246. doi: 10.1002/eji.201948432
[15] 陈洁霞, 李洁华, 唐海沁. 单核细胞、单核细胞/高密度脂蛋白比值与冠状动脉狭窄的相关性[J]. 中国老年学杂志, 2019, 39(5): 1028-1031. doi: 10.3969/j.issn.1005-9202.2019.05.002
[16] 王艳华, 刘泉源, 卢金凤, 等. 老年心衰合并肺部感染患者血清CHE、Cys C和氧化应激指标变化[J]. 中华医院感染学杂志, 2020, 30(16): 2452-2456. https://www.cnki.com.cn/Article/CJFDTOTAL-ZHYY202016014.htm
[17] Saito A, Amiya E, Soma K, et al. Fractional exhaled nitric oxide in adult congenital heart disease[J]. Nitric Oxide, 2020, 100-101(1): 45-49.
[18] Stark RJ, Koch SR, Choi H, et al. Endothelial nitric oxide synthase modulates Toll-like receptor 4-mediated IL-6 production and permeability via nitric oxide-independent signaling[J]. FASEB J, 2018, 32(2): 945-956. doi: 10.1096/fj.201700410R
[19] Pusceddu I, Dieplinger B, Mueller T. ST2 and the ST2/IL-33 signalling pathway biochemistry and pathophysiology in animal models and humans[J]. Clin Chim Acta, 2019, 495: 493-500. doi: 10.1016/j.cca.2019.05.023
[20] 何智余, 武锋超, 马兰虎, 等. H2S和sST2与射血分数降低的心力衰竭的相关性研究[J]. 临床心血管病杂志, 2020, 36(10): 930-935. https://www.cnki.com.cn/Article/CJFDTOTAL-LCXB202010011.htm
[21] Mohseni J, Kazemi T, Maleki MH, et al. A systematic review on theprevalence of acute myocardial infarction in iran[J]. Heart Views, 2017, 18(4): 125-132. doi: 10.4103/HEARTVIEWS.HEARTVIEWS_71_17
[22] Dernissei BG, Cotter G, Prescott MF, et al. A multimarker multi-time point-based risk stratification strategy in acute heart failure! results from the RELAX-AHF trial[J]. Eur J Heart Fail, 2017, 19(8): 1001-1010. doi: 10.1002/ejhf.749
[23] Weinberg EO, Shimpo M, De Keulenaer GW, et al. Expression and regulation of ST2, and interleukin-I J1 weptor family member, in cardiomyocytes and myocardial in farction[J]. Circulation, 2002, 106(23): 2961-2966. doi: 10.1161/01.CIR.0000038705.69871.D9
[24] 孙杰. 有创机械通气治疗ICU重症心力衰竭患者的疗效观察[J]. 心血管病防治知识, 2020, 10(2): 39-41. doi: 10.3969/j.issn.1672-3015(x).2020.02.014
-




 下载:
下载: