Diagnostic value of HIF-1α in acute ST segment elevation myocardial infarction and its relationship with ventricular remodeling
-
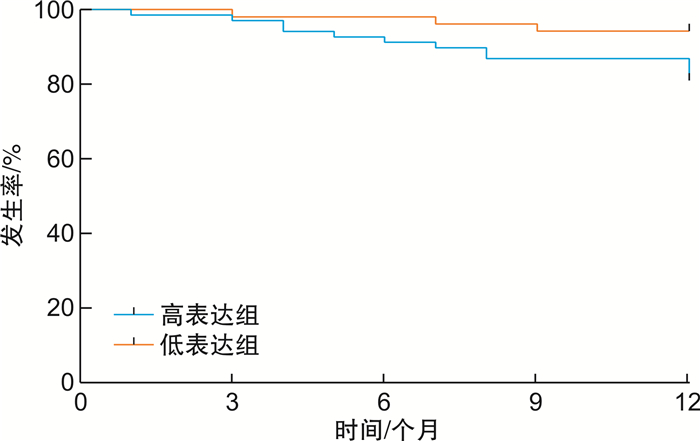
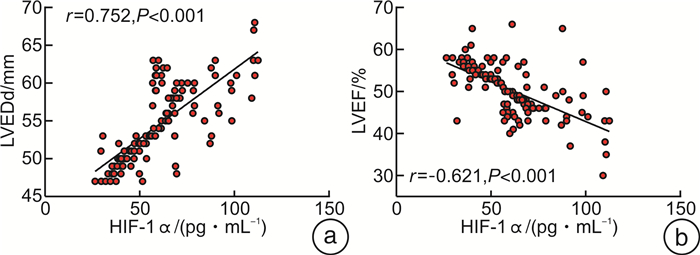
摘要: 目的 分析急性ST段抬高型心肌梗死(STEMI)患者体内低氧诱导因子-1α(HIF-1α)表达水平对左心室重构(VR)及远期预后的影响,以及两者间的相关性。方法 选取我院就诊的STEMI患者100例,其中男76例,女24例;检测入院时HIF-1α、CK-MB、Myo、cTNI及NT-proBNP水平。所有患者均行急诊血管再通治疗。根据术后3 d、3个月、6个月及12个月的心脏彩超的水平判断心梗后VR的发生率。以HIF-1α的中位数值(59.23 pg/mL)为界,将100例患者分为HIF-1α高表达组(50例)和低表达组(50例),分析患者不同HIF-1α表达水平与VR的关系。对不同表达组患者进行出院后随访,并用Kaplan-Meier生存曲线分析不同表达组的3个月、6个月及12个月主要心血管不良事件(MACE)的发生情况。结果 HIF-1α高表达组入院时CK-MB、Myo、cTNI水平较低表达组明显升高,差异有统计学意义(P< 0.05);两组患者入院时NT-proBNP比较,差异无统计学意义(P>0.05)。两组患者术后3 d左心室舒张末期内径(LVEDd)比较,差异无统计学意义(P>0.05);但高表达组术后3 d左心室射血分数(LVEF)较低表达组明显降低,差异有统计学意义(P< 0.05)。与低表达组相比,高表达组术后3个月、6个月及12个月LVEDd明显增大,伴随LVEF明显降低(P< 0.05)。高表达组术后3个月累计发生VR患者3例(6%),显著高于低表达组(1例,2%);术后6个月累计发生VR 6例(12%),显著高于低表达组(3例,6%);随访至术后12个月,高表达组累计发生VR 10例(20%),显著高于低表达组(5例,10%),两组比较差异有统计学意义(P< 0.01)。外周血HIF-1α水平与术后12个月LVEDd呈正相关(r=0.75,P< 0.001),与LVEF呈负相关(r=-0.621,P< 0.001)。高表达组随访12个月累计发生MACE 7例,显著高于低表达组(3例),差异有统计学意义(P< 0.05)。结论 HIF-1α表达水平与心肌损伤程度、VR及MACE存在一定相关性。Abstract: Objective To analyze the correlation of peripheral blood hypoxiainducible factor-1α(HIF-1α) level in patients with acute ST segment elevation myocardial infarction (STEMI) with ventricular remodeling (VR) and major adverse cardiovascular effects (MACE).Methods A total of 100 STEMI patients (76 males and 24 females) admitted to our hospital were selected to detect the levels of HIF-1α, CK-MB, Myo, cTNI and NT-proBNP on admission.All patients were treated with emergency recanalization.The incidence of VR after acute myocardial infarction was evaluated according to the level of color doppler echocardiography at 3, 6 and 12 months after discharge.Based on the median value of HIF-1α(59.23 pg/mL), 100 patients were divided into HIF-1α high expression group and HIF-1α low expression group, and the relationship between different HIF-1α expression levels and VR was analyzed.Patients in different expression groups were followed up after discharge, and Kaplan-Meier survival curve was used to analyze the occurrence of MACE at 3, 6 and 12 months in different expression groups.Results The levels of CK-MB, Myo and cTNI in the high expression group were significantly higher than those in the low expression group at admission, and the difference was statistically significant (P< 0.05).There was no significant difference in NT-proBNP between the two groups at admission.There was no significant difference in 3 d left ventricular end-diastolic diameter (LVEDd) between 2 groups after surgery, but 3 d left ventricular ejection fraction (LVEF) in the high expression group was significantly lower than that in the low expression group, the difference was statistically significant (P< 0.05).Compared with the low expression group, the LVEDd in the high expression group was significantly increased at 3 months, 6 months and 12 months after surgery, accompanied by a significant decrease in LVEF (P< 0.05).In the high expression group, 3 patients had accumulated VR 3 months after surgery, which was significantly higher than that in the low expression group (1 case).6 months after operation, 6 cases had VR, which was significantly higher than 3 cases in the low expression group.Up to 12 months after operation, 10 cases of high expression group developed VR, which was significantly higher than 5 cases of low expression group (P< 0.01).Peripheral blood HIF-1α level was positively correlated with LVEDd 12 months after discharge (r=0.75,P< 0.001) and negatively correlated with LVEF (r=-0.621,P< 0.001).During 12 months of follow-up, 7 cases of MACE occurred in the high expression group, which was significantly higher than 3 cases in the low expression group (P< 0.05).Conclusion The expression level of HIF-1α was correlated with the degree of myocardial injury, VR and MACE.
-

-
表 1 两组患者入院时CK-MB、Myo、cTNI及NT-proBNP水平比较
X±S 组别 例数 CK-MB/(ng·mL-1) Myo/(ng·mL-1) cTNI/(ng·mL-1) NT-proBNP/(pg·mL-1) 高表达组 50 23.3±5.71) 137.1±38.21) 2.8±0.71) 287.0±103.2 低表达组 50 17.9±4.5 98.6±29.3 1.7±0.5 291.7±98.4 与低表达组相比,1)P < 0.01。 表 2 两组患者术后3 d、3个月、6个月和12个月LVEDd及LVEF比较
X±S 组别 例数 术后3 d 术后3个月 术后6个月 术后12个月 LVEDd
/mmLVEF
/%LVEDd
/mmLVEF
/%LVEDd
/mmLVEF
/%LVEDd
/mmLVEF
(%)高表达组 50 49±4 53±51) 52±31) 52±31) 54±41) 50±41) 58±51) 47±41) 低表达组 50 48±5 56±4 49±4 56±3 49±5 57±5 50±3 55±3 与低表达组相比,1)P < 0.01。 表 3 两组患者术后3个月、6个月、12个月累计VR情况对比
例 组别 例数 术后3个
月术后6个
月术后12个
月高表达组 50 31) 61) 101) 低表达组 50 1 3 5 与低表达组比较,1)P < 0.01。 -
[1] 胡盛寿, 高润霖, 刘力生, 等. 《中国心血管病报告2018》概要[J]. 中国循环杂志, 2019, 34(3): 209-219. doi: 10.3969/j.issn.1000-3614.2019.03.001
[2] 张芹, 邹利群, 张伟, 等. 胸痛中心成立对急性心肌梗死患者诊疗效率和效果的影响[J]. 中华危重病急救医学, 2016, 28(7): 640-642. doi: 10.3760/cma.j.issn.2095-4352.2016.07.014
[3] Shukla SD, Walters EH, Simpson JL, et al. Hypoxia-inducible factor and bacterial infections in chronic obstructive pulmonary disease[J]. Respirology, 2020, 25(1): 53-63. doi: 10.1111/resp.13722
[4] Fitzpatrick SF. Immunometabolism and sepsis: a role for HIF?[J]. Front Mol Biosci, 2019, 6: 85. doi: 10.3389/fmolb.2019.00085
[5] Archid R, Solass W, Tempfer C, et al. Cachexia anorexia syndrome and associated metabolic dysfunction in peritoneal metastasis[J]. . Int J Mol Sci, 2019, 20(21): 5444. doi: 10.3390/ijms20215444
[6] 高敏雁, 吴红艳, 丁雪茹, 等. 血清缺氧诱导因子1α和心型脂肪酸结合蛋白水平与急性心肌梗死患者发生心力衰竭的相关性[J]. 中华实用诊断与治疗杂志, 2021, 35(2): 147-150. https://www.cnki.com.cn/Article/CJFDTOTAL-HNZD202102010.htm
[7] Luo Y, Teng X, Zhang L, et al. CD146-HIF-1α hypoxic reprogramming drives vascular remodeling and pulmonary arterial hypertension[J]. Nat Commun, 2019, 10(1): 3551. doi: 10.1038/s41467-019-11500-6
[8] Warbrick I, Rabkin SW. Hypoxia-inducible factor 1-alpha(HIF-1α)as a factor mediating the relationship between obesity and heart failure with preserved ejection fraction[J]. Obes Rev, 2019, 20(5): 701-712. doi: 10.1111/obr.12828
[9] Morariu M, Hodas R, Benedek T, et al. Impact of inflammation-mediated response on pan-coronary plaque vulnerability, myocardial viability and ventricular remodeling in the postinfarction period-the VIABILITY study: Protocol for a non-randomized prospective clinical study[J]. Medicine(Baltimore), 2019, 98(17): e15194.
[10] Bolognese L, Neskovic AN, Parodi G, et al. Left ventricular remodeling after primary coronary angioplasty: patterns of left ventricular dilation and long-term prognostic implications[J]. Circulation, 2002, 106(18): 2351-2357. doi: 10.1161/01.CIR.0000036014.90197.FA
[11] Heger LA, Kerber M, Hortmann M, et al. Expression of the oxygen-sensitive transcription factor subunit HIF-1α in patients suffering from secondary Raynaud syndrome[J]. Acta Pharmacol Sin, 2019, 40(4): 500-506. doi: 10.1038/s41401-018-0055-1
[12] Su F, Zhang W, Chen Y, et al. Significance of hypoxia-inducible factor-1α expression with atrial fibrosis in rats induced with isoproterenol[J]. Exp Ther Med, 2014, 8(6): 1677-1682. doi: 10.3892/etm.2014.1989
[13] Shyu KG, Liou JY, Wang BW, et al. Carvedilol prevents cardiac hypertrophy and overexpression of hypoxia-inducible factor-1alpha and vascular endothelial growth factor in pressure-overloaded rat heart[J]. J Biomed Sci, 2005, 12(2): 409-420. doi: 10.1007/s11373-005-3008-x
[14] Kumar S, Wang G, Liu W, et al. Hypoxia-Induced Mitogenic Factor Promotes Cardiac Hypertrophy via Calcium-Dependent and Hypoxia-Inducible Factor-1α Mechanisms[J]. Hypertension, 2018, 72(2): 331-342. doi: 10.1161/HYPERTENSIONAHA.118.10845
[15] Abe H, Semba H, Takeda N. The Roles of Hypoxia Signaling in the Pathogenesis of Cardiovascular Diseases[J]. J Atheroscler Thromb, 2017, 24(9): 884-894. doi: 10.5551/jat.RV17009
-




 下载:
下载: