Experience of extracorporeal membrane oxygenation support for inter-hospital transport in 27 critically ill patients
-
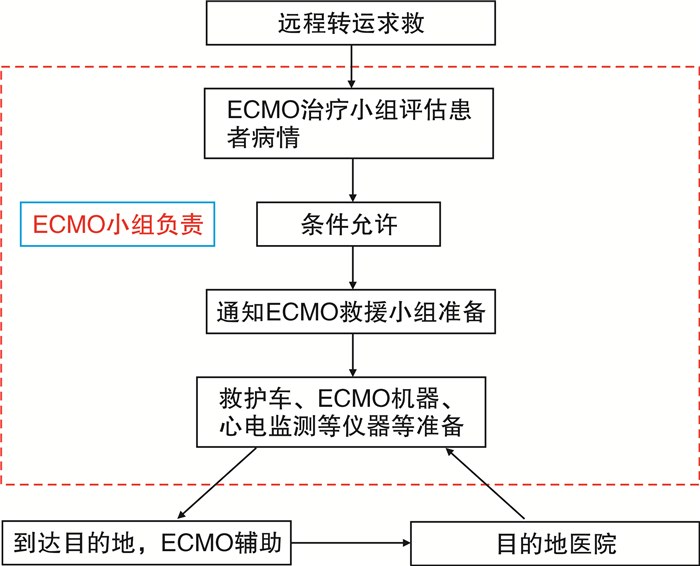
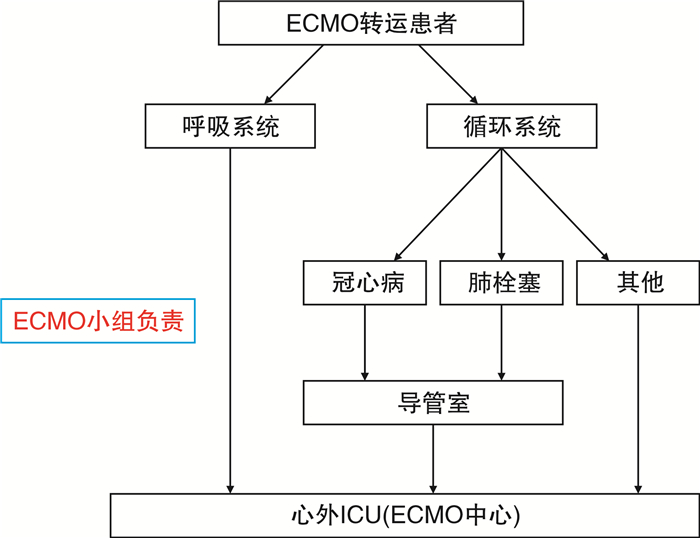
摘要: 目的 总结我院ECMO团队实施体外膜肺氧合(ECMO)辅助重症患者院际转运的临床经验。方法 回顾性分析2017年2月—2021年4月期间我院ECMO团队在ECMO支持下实现院际转运的27例危重患者的临床资料。记录患者疾病种类、插管地点、插管方法、院际转运距离、转运方式、患者转运期间不良事件发生情况以及临床转归。结果 27例患者均由我院心外科ECMO团队在外院置管后转至本单位。其中男24例,女3例;平均年龄52.5岁;转运距离4~300 km。1例患者采用直升机转运,26例患者采用地面救护车转运。转运过程中无死亡事件发生,但发生8例不良事件。ECMO顺利撤机18例,患者顺利出院14例。结论 ECMO辅助下危重患者的院际转运是安全而有效的,充分而周密的准备工作可有助于减少ECMO转运途中不良事件的发生。Abstract: Objective To summarize the clinical experiences of extracorporeal membrane oxygenation (ECMO) for inter-hospital transport in critically ill patients.Methods We collected the clinical data of 27 critically ill patients who were transferred by our ECMO team from February 2017 to April 2021 and retrospectively analyzed the disease types, intubation location, intubation methods, distance between hospitals, transportation mode, adverse events during transportation and prognosis.Results All of the 27 patients were transferred to our department by ECMO support, with 24 males and 3 females, average 52.5 years old, transportation distance 4 to 300 km. One patient was transferred by helicopter, and 26 patients were transferred by ground ambulance. There was no death but 8 adverse events occurred during ECMO transportation, with 18 patients successfully withdrawn ECMO and 14 were discharged.Conclusion The ECMO transportation is safe and effective for inter-hospital transport in critically ill patients. Adequate and careful preparations can be helpful to reduce the adverse events during ECMO transportation.
-

-
[1] 中国医师协会体外生命支持专业委员会. 成人体外膜氧合循环辅助专家共识[J]. 中华医学杂志, 2018, 98(12): 886-894. doi: 10.3760/cma.j.issn.0376-2491.2018.12.003
[2] Wilhelm MJ, Inderbitzin DT, Reser D, et al. Outcome of inter-hospital transfer of patients on extracorporeal membrane oxygenation in Switzerland[J]. Swiss Med Wkly, 2019, 149: w20054.
[3] Fouilloux V, Gran C, Ghez O, et al. Mobile extracorporeal membrane oxygenation for children: single-center 10 years' experience[J]. Perfusion, 2019, 34(5): 384-391. doi: 10.1177/0267659118824006
[4] 中国医药教育协会急诊专业委员会, 中华医学会急诊分会复苏学组, 中国急诊体外膜肺氧合联盟. 成人体外膜肺氧合患者院际转运专家共识[J]. 中华急诊医学杂志, 2020, 29(2): 165-170. doi: 10.3760/cma.j.issn.1671-0282.2020.02.007-1
[5] Heuer JF, Mirschel M, Bleckmann A, et al. Interhospital transport of ARDS patients on extracorporeal membrane oxygenation[J]. J Artif Organs, 2019, 22(1): 53-60. doi: 10.1007/s10047-018-1065-y
[6] Fletcher-Sandersjöö A, Frenckner B, Broman M. A Single-Center Experience of 900 Interhospital Transports on Extracorporeal Membrane Oxygenation[J]. Ann Thorac Surg, 2019, 107(1): 119-127. doi: 10.1016/j.athoracsur.2018.07.040
[7] 张世新, 夏梅, 吴蔚, 等. 危重患者在体外膜肺氧合支持下院间转运的病例系列报道[J]. 第三军医大学学报, 2019, 41(1): 13-18. https://www.cnki.com.cn/Article/CJFDTOTAL-DSDX201901004.htm
[8] 梅勇, 张劲松, 陈旭锋, 等. 急诊团队主导体外膜肺氧合支持下的院际转运经验[J]. 中华急诊医学杂志, 2020, 29(2): 227-230.
[9] 潘旗开, 刘延锦, 柴宇霞, 等. 重症体外膜肺氧合患者院际转运风险管理[J]. 中国急救复苏与灾害医学杂志, 2020, 15(1): 20-25. doi: 10.3969/j.issn.1673-6966.2020.01.007
[10] 徐磊, 王志勇, 李彤, 等. 体外膜肺氧合与机械通气用于严重急性呼吸窘迫综合征患者院间转运的对比研究[J]. 中华危重病急救医学, 2014, (11): 789-793. doi: 10.3760/cma.j.issn.2095-4352.2014.11.005
[11] Ann. ELSO Guidelines for ECMO Transport[DB/OL]. (2015-05)[2021-08]. http://www.elso.org/Resources/Guidelines.aspx
[12] Salna M, Chicotka S, Biscotti M 3rd, et al. Management of Surge in Extracorporeal Membrane Oxygenation Transport[J]. Ann Thorac Surg, 2018, 105(2): 528-534. doi: 10.1016/j.athoracsur.2017.07.019
[13] Morshuis M, Bruenger F, Becker T, et al. Inter-hospital transfer of extracorporeal membrane oxygenation-assisted patients: the hub and spoke network[J]. Ann Cardiothorac Surg, 2019, 8(1): 62-65. doi: 10.21037/acs.2018.12.03
[14] Ericsson A, Frenckner B, Broman LM. Adverse Events during Inter-Hospital Transports on Extracorporeal Membrane Oxygenation[J]. Prehosp Emerg Care, 2017, 21(4): 448-455. doi: 10.1080/10903127.2017.1282561
[15] Burgos CM, Frenckner B, Fletcher-Sandersjöö A, et al. Transport on extracorporeal membrane oxygenation for congenital diaphragmatic hernia: A unique center experience[J]. J Pediatr Surg, 2019, 54(10): 2048-2052. doi: 10.1016/j.jpedsurg.2018.11.022
-





 下载:
下载: